spermogram
the whole website / 4 results found
Blog 4 results found
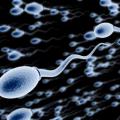
ALL ABOUT SPERMATOZOIDS: Bark, Roots, Herbal Teas, Plants
ALL ABOUT SPERMATOZOIDS: Bark, Roots, Herbal Teas, Plants A spermatozoon is a mobile male reproductive cell (or gamete) involved in sexual reproduction. During fertilization, the sperm unites with an egg or an oocyte (female gamete) to form an egg cell, which will then develop into an embryo to give a new individual. This is how the Dawasanté experts provide you with a natural treatment to treat your problems with sperm abnormalities (oligospermia, necrospermia, asthenospermia, teratospermia, azoospermia, etc.). Click on the image below to discover this natural treatment We deliver all over the world. For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number. The possible link between male infertility and chromosomal abnormalities in spermatozoa has been explored in several studies, since the advent of the technique of fluorescence in situ hybridization (FISH). INTRODUCTION Chromosomal abnormalities in humans may be responsible for infertility. In fact, the prevalence of abnormalities detected in the blood karyotype is ten times higher in infertile men than in the general population, ie around 5.3%, versus 0.6%. Numerical and structural abnormalities of the sex chromosomes are found with a high frequency, especially in men with severe azoospermia or oligo-astheno-teratospermia (OAT). The treatment of choice to remedy male infertility with OAT is Medically Assisted Reproduction (PMA) by Intra Cytoplasmic Sperm Injection (ICSI). However, it has been reported in recent years that the rate of aneuploidy (abnormal number of chromosomes) of the sex chromosomes and de novo structural chromosomal abnormalities of paternal origin is higher in the offspring of these men. The risk of transmission of a chromosomal abnormality to offspring as the natural process of sperm selection is bypassed by the ICSI procedure should therefore be carefully considered and evaluated. SPERMATOZOID CARYOTYPE AND FISH Karyotypic analysis of spermatozoa makes it possible to determine in what proportion the gametes themselves are carriers of chromosomal abnormalities, in particular in infertile men. In 1978, Rudak et al. described a technique for the karyotypic analysis of spermatozoa, based on the in vitro penetration of the latter into hamster oocytes. This technically heavy and delicate technique was only successfully practiced by a dozen laboratories around the world. The technique of FISH (Fluorescence In Situ Hybridization) and its developments now make it possible to perform the chromosomal study of spermatozoa and analyze a large number of cells, using chromosome-specific probes that hybridize to particular regions of the DNA and can then be detected visually using a fluorescence microscope. For the FISH study, sperm from an ejaculate is spread on slides and undergo a chemical treatment resulting in the decondensation of their heads, while maintaining the structure that distinguishes them from other cells that may be in the ejaculate. Spermatozoa are also distinguished by the fact that they present signals corresponding to haploid and non-diploid cells. intact with clear hybridization signals are counted MORPHOLOGICALLY NORMAL SPERMATOZOIDS Morphology and motility are currently the parameters used to identify the sperm that will be microinjected as part of an ICSI procedure. Spermatozoa with an abnormal morphology are also more likely to present aneuploidy, but this risk has not been clearly quantified. Ryu et al. studied the frequency of aneuploidy in sperm of normal morphology in infertile patients who are candidates for ICSI and all carriers of a normal blood karyotype compared to fertile patients. The morphology criterion used was that of Kruger. FISH analysis of chromosomes 18, X and Y were performed. In the group of infertile patients, and aneuploidy rate was found varying from 1.8% to 5.5% compared to 0% to 2.6% in the control patients. This result shows that the morphology of the spermatozoa is not an absolute criterion for the selection of a genetically normal spermatozoon. Note that the different reported figures of sperm aneuploidy in men without fertility problems vary between 0 and 5% depending on the studies, differences which may be due to the use of probes with variable hybridization efficiency or to the visual interpretation of signals. CHROMOSOMIC ANOMALIES, SPERMOGRAM AND LIFESTYLE In a recent review, the sperm karyotypes of men without spermogram abnormalities were analyzed, with the aim of looking for possible correlations with age and lifestyle. The results of some fifty studies combining data from sperm analysis by FISH from 500 men (more than 5 million spermatozoa) were compiled. The results are an average reported rate of abnormality of 0.15% for each chromosome and 0.26% for sex chromosomes. The majority of chromosomes had an even distribution of abnormalities, with the exception of chromosomes 21, 22 and sex in which the frequencies of abnormalities were significantly higher. Trisomies 21 and 22 are also the most frequently found in the products of spontaneous miscarriages, showing the link between chromosomal abnormalities in spermatozoa and abnormalities found in the embryo. This work also demonstrated a slight increase in the frequency of disomies with paternal age, mainly for the sex chromosomes, but no effect of smoking, alcohol and caffeine consumption. INFERTILITY AND KYOTYPES OF SPERMATOZOIDS It is reported that 23% of men with azoospermia and 5-10% of men with OAT have an abnormal blood karyotype, resulting in a high likelihood of producing aneuploid gametes. It is known, for example, that the proportion of gametes with a chromosomal imbalance can be as high as 50% in men carrying a reciprocal translocation. However, a normal blood karyotype does not exclude the production of aneuploid gametes. An abnormal intra-testicular environment can affect spermatogenesis, in particular by disrupting the mechanisms controlling chromosome segregation during cell division. A defect in spermatogenesis can have many origins such as systemic disease, malnutrition, endocrine disorders, obstructive pathologies and genetic defects. Indeed, a large number of severe OATs and azoospermia have genetic etiologies, including microdeletions at the level of the Y chromosome, abnormalities of meiosis, and mutations in the cystic fibrosis gene. However, “idiopathic” OAT remains the diagnosis most often retained in male infertility, despite extensive investigations to try to determine its origin. The main interest in identifying an etiology with OAT lies in the evaluation of the prognosis and the risk of producing embryos with chromosomal abnormalities. A large study is now the source of much controversy over the relationship between spermogram abnormalities and potential risks of chromosomal abnormalities in ICSI. Fertilization and pregnancy rates obtained in relation to parameters of sperm number, mobility and morphology of infertile men were retrospectively analyzed in 966 cycles of ART with ICSI. The results showed comparable ICSI successes independent of the magnitude of OAT parameters. They concluded that in the extreme, only a living sperm in ejaculate can be sufficient for ICSI to be successful. While this study was therefore very reassuring, it does not In order to study the etiology of “unlabelled” OATs, Calogero et al. used the FISH technique to explore the rate of aneuploidy in sperm chromosomes 8, 12, 18, X and Y in one group of patients with teratospermia, another with OAT and a control group. They observed similarly increased rates of aneuploidy in the first two groups, which suggested that teratospermia may be the critical endpoint associated with aneuploidy. The authors, therefore, recommended that a FISH analysis be performed in cases of teratospermia, before any attempt at ICSI. These same authors performed another study to try to relate the rate of sperm aneuploidy in eighteen men with OAT and the results of ICSI in affected couples. For these cases of OAT, and overall fertilization rate of 95% and a pregnancy of 39% was obtained. Very curiously, this pregnancy rate was significantly higher than reported by multiple centers practicing the ICSI technique (the generally accepted average rate is around 25%), which the authors of the article do not discuss. The rate of oocyte fertilization by ICSI was independent of the rate of aneuploidy. On the other hand, the patients who had not had a pregnancy (91%) had significantly higher aneuploidy rates than those of the controls. Bernardini et al. also analyzed by FISH the rate of aneuploidy of the spermatozoa for chromosomes 1, 17, X, and Y, on a series of twenty-two cases of infertile men compared to fertile controls. A significantly higher rate of aneuploidy was found in men with OAT (18%) compared to controls (2.28%). In the case of azoospermia patients, it is now sometimes possible to perform ICSI after a testicular biopsy in which sperm is found. The reported numbers of chromosomal abnormalities are impressive: indeed, one study estimated the proportion of chromosomal abnormalities at 19.6% in a group of patients with non-obstructive azoospermia and 8.2% in those with obstructive azoospermia. Here again, the link between gonadal insufficiency and the presence of chromosomal aneuploidies is well demonstrated. It can be concluded from these data that a high rate of aneuploidy in spermatozoa is associated with a low rate of pregnancy and therefore less success through assisted reproduction by ICSI. However, the rate of fertilization of the oocytes does not seem to depend on the rate of aneuploidy, which means that the transferred embryos are more often carriers of aneuploidies and that on the other hand, their implantation would be disadvantaged. In this context, genetic counseling following a FISH analysis of the sperm would be highly desirable, before a couple begins a long and difficult procedure of assisted reproduction by ICSI. SPERMATOZOID ANEUPLOIDS AND GENE FACTORS A particularly important point of these studies is that they make it possible to explain certain male infertilities so far called “idiopathic”. In fact, disturbances of meiosis or premeiotic mitosis during spermatogenesis could predispose to the non-chromosomal disjunctions that are observed. The next step would consist in identifying which are the genetic factors at the origin of these disorders of meiosis and mitosis and to characterize them to have one more diagnostic means available in idiopathic male infertility. If gene abnormalities predisposing to non-disjunctions were detected, this diagnostic tool would be available and the possible transmission in the offspring of this pathology would be evaluable. And then supported by numerous studies. We now know that at least thirty genes are involved in the control of meiotic and mitotic divisions. For example, the role of HspA2, a “chaperone” protein with a specific testicular expression that is thought to be involved in the synaptonemal complex has recently been demonstrated. The role of genes of the MAD (Mitotic Arrest Deficiency) family involved in premeiotic mitotic control is also discussed. There is a case, recently reported in the literature, where FISH analysis of spermatozoa made it possible to pose a contraindication to ART. In the study in question patients with different types of absolute teratospermia (100%) were studied. One of them had a sperm morphological abnormality consisting of macrocephaly and multiple flagella. In this patient, 90% of the sperm analyzed by FISH presented aneuploidy. This result was considered to be a contraindication to ICSI. FEASIBILITY In these various studies, between 3000 and 10,000 sperm per patient are analyzed. This represents a significant investment of time, considering that for FISH analysis on amniocytes, there are routinely between 50 and 100 cells. It is estimated that to detect significant levels of aneuploidy in sperm, an analysis of around 1000 cells may be sufficient. The method of collection is no different from that for a spermogram, and only a small fraction of ejaculate is used to smear onto slides for chemical treatment of the sample prior to FISH. CONCLUSION While the use of FISH on spermatozoa in male infertility appears undoubtedly valuable and contributory in the context of a pre-ART workup, or after repeated ART failures, the formal indications for this analysis have not yet been clearly established. established. One of the first uses of this approach could be to give couples undergoing a pre-ICSI procedure for OAT or azoospermia a more detailed indication of the chances of success and risks of miscarriages due to chromosomal abnormalities potentially present in the sperm. This information should then be communicated to patients within the framework of genetic counseling, taking into account the psychological repercussions of a possible poor prognosis of success. Some authors also consider that this technique can be used in the event of miscarriages with repetitions of undetermined etiology beyond the framework of male infertility. Indeed, if 60% of the miscarriages of the first trimester are due to chromosomal abnormalities and a majority are of maternal origin, the FISH technique on the spermatozoa has shown a paternal origin in 8 to 12% of cases, corresponding to a greater incidence of chromosomal abnormalities in their gametes. We deliver all over the world. For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
OLIGO-ASTHENO-TERATOSPERMIE
OLIGO-ASTHENO-TERATOSPERMIA You have been trying to have a baby for several months, but it is late. After tests, your doctor told you that your loved one has oligoasthenoteratospermia (OATS). What are OATS and what are the consequences? However, the experts at Dawasanté provide you with a natural treatment to permanently cure oligo- asthenoteratospermia. Click HERE or on the image below to discover this natural treatment We deliver all over the world. For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number. What is Oligoasthenoteratospermia or OATS? OATS designates a set of abnormalities found during the spermogram during a male infertility assessment. The OATS groups together a low concentration of sperm (oligo) with therefore too few spermatozoa to naturally fertilize an oocyte, too low mobility of these spermatozoa (astheno) which does not allow them to join the oocyte and too large a proportion abnormal sperm (terato). However, OATS can present varying degrees. It can be severe, with very low mobility and concentration indices while the malformation index is very high. It can be moderate with indices closer to normal. Intermediate forms exist with indices of the same degree or which may be of different degrees: severe for one or two types of indices (eg: mobility and concentration) and moderate for the third. What happens after diagnosis of the OATS? Once the OATS is discovered, the doctor will look to determine if there are any causes for these abnormalities. Indeed, OATS can be reduced, at least in part, depending on its origin. He will look first for signs of infections, old or recent. Some infections, such as chlamydia, can cause a decrease in male fertility. Their treatment can help regain better fertility. Likewise, the treatment of a varicocele (varicose veins in one or both testicles) or stopping smoking may improve the results of a spermogram. Further research will be carried out to find out if there is a malformation in the testes or seminal tract. In all cases, a second spermogram will be done because it is possible that significant variations appear and allow to hope for other opportunities for natural fertilization. What to do to have a child in the event of OATS? If the diagnosis of OATS is confirmed, the possibility of natural fertilization is reduced. However, it does exist, especially if it is a moderate form. However, certain factors, such as the woman's age or the length of time contraception has been stopped must be taken into account and assisted reproduction (ART) may be considered. Depending on the case, it will be an in utero insemination (IUI) where the sperm is introduced directly into the uterus, and in vitro fertilization (IVF) where the sperm is brought into contact with one or more oocytes in the laboratory or an intracytoplasmic sperm injection (ICSI) where sperm is introduced directly into an oocyte in the laboratory. These different techniques will be offered depending on the degree of OATS. The success of IVF or ICSI is of the order of 25 to 30% which leaves hope to those who are concerned by this difficulty. Asthenospermia is an abnormality of the sperm that is characterized by insufficient mobility while their number remains normal. Also called asthenozoospermia, this sperm fatigue is one of the possible causes of male fertility problems. What are the main causes? How is asthenospermia diagnosed? What treatment is there to promote procreation? What is asthenospermia due to? The main causes that can explain unsatisfactory sperm mobility are: a morphological anomaly of the male gametes, an infection, presence of anti-sperm antibodies medication, a varicocele, a dietary deficiency, a renal failure, liver failure chemotherapy, exposure to radiation, excessive alcohol consumption, a deficiency in calcium, vitamin D, or trace element ... How is asthenospermia diagnosed? A semen analysis, or spermogram, is used to assess the mobility of the sperm. It should be remembered that only mobile gametes can fertilize the egg. Many medical analysis laboratories rely on the classification decreed by the World Health Organization to classify spermatozoa: Level A (or I): progressive rapid sperm advance quickly and in a straight line, Level B (or II): the slow progressive spermatozoa advance slowly or in a curved line, Level C (or III): non-progressive spermatozoa move but do not progress, Level D (or IV): the sperm are immobile. To be qualified as normal, the spermogram must show a minimum of 40% of motile spermatozoa and 32% of spermatozoa showing progressive mobility. What solutions to have a child? The management of asthenospermia varies mainly according to its origin. Thus, an infection will have to be treated according to its nature with appropriate antibiotic drugs while certain testicular abnormalities may, in some cases, be the subject of surgery. While there is no curative treatment for asthenospermia, certain drugs help improve the quality of sperm: vitamins, hormones, alternative medicine (herbal medicine, homeopathy, aromatherapy, etc.). When the treatments do not give satisfactory results, in vitro fertilization with donor sperm or an intracytoplasmic injection of sperm may be considered in the context of Medically Assisted Reproduction ( MAP).) when the couple wants a child. We deliver all over the world. For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
MALE INFERTILITY TERATOSPERMIA
The teratospermia (or teratospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. However, the experts at Dawasanté provide you with a natural treatment to permanently cure teratospermia and allow you to conceive quickly. Click here or on the image below to find out what treatment We deliver all over the world. For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number. Teratospermia is a sperm abnormality characterized by sperm with morphologic defects. These abnormalities can affect different parts of the sperm: the head, which contains the nucleus carrying the 23 paternal chromosomes; the acrosome, a small membrane at the front of the head that, at the time of fertilization, will release enzymes that will allow the sperm to cross the pellucid area of the oocyte; the flagellum, this "tail" which allows it to be mobile and therefore to move up from the vagina to the uterus and then the tubes, for a possible encounter with the oocyte; the intermediate part between the flagellum and the head. Often, the anomalies are polymorphic: they can be multiple, in size or shape, affect both the head and the flagellum, vary from one sperm to another. It may be globozoospermia (absence of acrosome), double flagellum or double head, coiled flagellum, etc. All these abnormalities have an impact on the fertilizing power of the sperm, and therefore on the fertility of the man. The impact will be more or less important depending on the percentage of normal sperm remaining. Teratospermia can decrease the chances of conception and even lead to male infertility if it is severe. Often, teratospermia is associated with other spermatic abnormalities: oligospermia (insufficient number of spermatozoa-, asthenospermia (defect in sperm mobility. We then speak of oligo-asthenic-teratozoospermia (OATS). Like all sperm abnormalities, the causes can be hormonal, infectious, toxic, drug-related. The morphology of spermatozoa is in fact the first parameter to be altered by an external factor (exposure to toxicants, infection, etc.). More and more specialists also consider that atmospheric and food pollution (via pesticides in particular) has a direct impact on the morphology of spermatozoa. But sometimes, no cause is found. The main symptom of teratospermia is difficulty conceiving. The fact that the shape of the sperm is abnormal does not affect the occurrence of malformations in the unborn child, but only the chances of pregnancy. Teratospermia is diagnosed using a spermogram, one of the first examinations systematically performed in men during an infertility assessment. It allows a qualitative and quantitative study of sperm thanks to the analysis of different biological parameters: the volume of the ejaculate; pH; sperm concentration; the mobility of sperm; sperm morphology; the vitality of sperm. The part about sperm morphology is the longest and most difficult part of the spermogram. In a test called a spermocytogram, 200 sperm are fixed and stained on smear slides. Then the biologist will study the different parts of the sperm under a microscope in order to assess the percentage of morphologically normal sperm. The type of morphological abnormalities is also taken into account to estimate the impact of teratospermia on fertility. Several classifications exist: the David classification modified by Auger and Eustache, still used by certain French laboratories; the Kruger classification, the WHO international classification, is the most widely used in the world. Carried out using an automatic machine, this more “severe” classification classifies as atypical spermatozoa any spermatozoon which deviates, even very little, from the form considered as normal. If the proportion of correctly formed sperm is less than 4% according to the WHO classification, or 15% according to the modified David classification, teratospermia is suspected. But as for any spermatic abnormality, a second or even a third spermogram will be carried out 3 months apart (the duration of a spermatogenesis cycle being 74 days) in order to make a firm diagnosis, especially as various factors can influence on sperm morphology (long abstinence time, regular cannabis intake, feverish episode, etc.). A migration-survival test (TMS) usually completes the diagnosis. It makes it possible to have an evaluation of the number of spermatozoa able to end up in the uterus and able to fertilize the oocyte. A sperm culture is often coupled with the spermogram in order to detect an infection which could alter spermatogenesis and lead to morphological defects of the sperm. Teratospermia occurs when less than 4% of the sperm present in the male ejaculate is said to be “typical” or normal. The remaining 96% are carriers of abnormalities or have an alteration in their morphology. A normal sperm consists of an oval head, an intermediate body one and a half times longer than the head, and a long, thin tail (the flagellum) which promotes its mobility. The abnormalities detected can affect the head of the spermatozoon as well as its intermediate part or even its flagellum. There are also combined forms of anomalies. Teratospermia is usually the cause of male infertility. Indeed, alterations in the morphology of spermatozoa can affect their mobility and prevent them from reaching the egg. There are different degrees of severity of teratospermia which can be classified as mild, moderate, or severe. The higher the degree of severity, the more difficult natural procreation will be. Little is known about the causes of this anomaly. The origin can be infectious, medicinal, genetic, anatomical (varicocele or varicose veins of the testes), environmental or related to the hygiene of life. Finally, there are reversible forms of teratospermia. This is why the patient is generally asked to perform a second examination, 3 months apart from the first, in order to detect the persistence of the anomaly. We deliver all over the world. For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number.
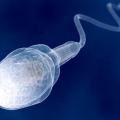
UNDERSTANDING THE SPERMOGRAM: Natural treatment
UNDERSTANDING THE SPERMOGRAM The semen is the result of the laboratory examination of the semen. Regardless of the poor quality and quantity of your sperm, Dawasanté experts provide you with a natural herbal treatment to improve the quality and quantity of your sperm. This will allow you to conceive quickly and be more fertile. Click on the image below to discover this natural treatment We deliver all over the world. For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number. Topic: AKINETOSPERMIA, ASPERMIA, ASTHENOSPERMIA, AZOOSPERMIA, Cryptozoospermia, DYSKINESIA, FLAGELLAR, HYPERSPERMIA, HYPOSPERMIA, AGGREGATES, LEUCOSPERMIA, NECROSPERMIA, Oligo-Asthenoospermia, TOSPEROPERMIA, POLYPERSPATERMIA, TERATOSPERSPATERMIA, TOSPEROPERMIA I - WHAT IS A SPERMOGRAM? The spermogram is an analysis that will study the quantity and quality of sperm. The spermogram is carried out after having collected the sperm in the laboratory and by masturbation. The spermogram includes: 1 - An analysis of the volume of the ejaculate 2 - A determination of the pH 3 - The study of the mobility of the spermatozoa at the emission of the sperm and after 1 hour and 3 hours 4 - The calculation of the number of spermatozoa 5 - Their vitality 6 - Viscosity 7 - The percentage of abnormal forms observed under the microscope… In addition, we also evaluate: 8 - The level of isolated flagella and / or lysed spermatozoa 9 - The level of white line cells 10 - The level of other cells (cells of the urogenital tract) 11 - The level of cell fragments 12 - The presence of red blood cells or blood residue II - REFERENCE VALUES 1 - Quantity 2 to 6 ml 2 - Color Normally viscous and opalescent white 3 - viscosity On ejaculation, the sperm coagulates and liquefies in less than 30 minutes at 37 ° C 4 - Number - From 40 million to 200 million per ml. - Greater than 15 million per ml and must be greater than 39 million for the entire ejaculate 5 - Mobility This is the most important parameter The mobility standard accepted after 30 minutes of the emission must not be below 80% of motile spermatozoa - After 1 hour - We must find more than 50% of motile spermatozoa that is to say in progressive displacement - After 3 hours - We must find at least 30% of motile spermatozoa Observation The mobility of sperm is classified into four categories or grades (see below). 6 - Vitality At ejaculation, the percentage of living spermatozoa must be equal to or greater than 60% of all spermatozoa 7 - Leukocytes The number of leukocytes must be less than 1 million / ml 8 - Abnormal forms - According to the classification of Cohen Bacri Abnormal forms should not exceed 15 to 20% of the total sperm - According to the classification of “David” Abnormal forms must not exceed 30%, of the total sperm - According to the classification of “Kruger” Abnormal forms must not exceed 4%, of the total spermatozoa 9 - The pH It must be between 7.2 to 8 Good to know The pH is a direct indicator of secretions from the annex glands (acid prostatic secretions and secretions from the seminal vesicles). 10 - Germ cells Their percentage must not exceed 10% Germ cells are the basic cells that evolve into the sperm after a complex transformation; a higher level may suggest a disorder in sperm production. III - INTERPRETATION OF THE RESULTS Male infertility can be caused: 1 - By poor quality sperm production 2 - By insufficient sperm production 3 - By an anomaly in the transport of these spermatozoa Spermatozoon and its various abnormalities IV - THE MAIN ANOMALIES 1 - HYPOSPERMIA The total volume of the ejaculate less than 2 ml The causes of hypospermia are varied: - Technical problem in collecting sperm - Abstinence - Secretion deficit - Retrograde ejaculation… Good to know The volume of semen gradually decreases with age without altering the other parameters. 2 - HYPERSPERMIA The volume of the ejaculate much greater than normal Hyperspermia and sometimes in connection with an inflammatory or infectious syndrome of the annex glands and more particularly the seminal vesicles. Important It can also be due to excessive sexual abstinence. 3 - OLIGOSPERMIA (OLIGOZOOSPERMIA) It corresponds to an insufficient quantity of spermatozoa in the semen Very important to know 1 - If the number of spermatozoa is less than 10 million / ml, there is infertility 2 - If the number of sperm is less than 5 million per ml, we speak of severe oligospermia. 4 - POLYSPERMIA The concentration of spermatozoa greater than 200 million per ml 5 - AZOOSPERMIA Absence of spermatozoa in the ejaculate Two types of azoospermia are encountered: 1 - Secretory azoospermia - Corresponds either to a primary, congenital or acquired testicular disease, or to an acquired congenital hypothalamic-pituitary insufficiency. 2 - Excretory azoospermia - Corresponds to the presence of an obstacle in the excretory tract (epididymis, vas deferens, ejaculatory ducts). These lesions can be acquired or congenital. 6 - ASTHENOSPERMIA Sperm mobility defect We speak of asthenospermia if at least 40% of the spermatozoa encountered are not mobile. Sperm mobility is classified into four categories or classes - 1 - Class A - Fast and progressive spermatozoa (speed> 25 µm / s) 2 - Class B - Slow or weakly progressive spermatozoa (speed 5 - 25 µm / s) 3 - Class C - Mobile spermatozoa but without any progressivity (mobility in place) 4 - Class D - Immobile spermatozoa 7 - NECROSPERMIA (NECROZOOSPERMIA) It is characterized by a very high percentage of dead spermatozoa Necrospermia is often due to microbial infections. There are two types of necrospermia: 1 - Partial necrospermia - Corresponds to 42% of the spermatozoa found are dead 2 - Total necrospermia - Corresponds to all the sperm found in the ejaculate are dead 8 - TERATOSPERMY OR TERATOZOOSPERMIA It corresponds to an excessive quantity of abnormal spermatozoa and can reach up to 30% (see above, abnormal forms). The main abnormal forms encountered are - 1 - Head abnormalities (less than 35%) - Microcephaly, macrocephalic, elongated head, irregular head ... 2 - Anomalies of the intermediate part (less than 20%) - The result from the presence of cytoplasmic remains 3 -Flagellum abnormalities (less than 20%) - Angulated, coiled flagellum ... 4 - Double forms (less than 10%) - 5 - The globozocephalic form - Characterized by the absence of the acrosome. The presence of this form is a sign that there is no possibility of fertilization. 9 - ASPERMIA A total absence of ejaculate 10 - OAT (Oligo-Astheno-Teratozoospermia) It is the association of three pathologies and which are: Oligospermia, Astheno-spermia and Teratozoospermia. 11 - AGGLUTINATES Agglutinates (or adjoining) correspond to a gathering of several spermatozoa living together. The agglutinates are explained by the presence of living sperm and carriers of anti-sperm antibodies. The presence of agglutinated spermatozoa should cause the presence of anti-sperm antibodies to be tested. 12 - AGGREGATES They are to be distinguished from agglutinates because they correspond to the joining of several spermatozoa which have died together. 13 - FLAGELLAR DYSKINESIA Abnormalities in the movements, speed and trajectory of spermatozoa 14 - LEUCOSPERMIA Leukocytosis at more than 1 million / ml This leukospermia suggests an infection 15 - AKINETOSPERMIA All spermatozoa are immobile 16 - CRYPTOZOOSPERMY * Absence of spermatozoa observed in a drop of sperm under the microscope A thorough search in the whole of the sperm allows one to find some spermatozoa (less than 100,000 spermatozoa in the whole of the ejaculate). There are two main cryptozoospermia - 1 - Severe cryptozoospermia The number of spermatozoa found is less than 10,000 2 - Moderate cryptozoospermia, The number of spermatozoa is greater than 10,000 * Important - Cryptozoospermia is a new entity which has only gained interest since the appearance of the ICSI technique (Intra Cytoplasmic Sperm Injection) because with this technique, just a few spermatozoa ejaculated or taken from epididymis or testis, and regardless of sperm concentration and mobility, to achieve fertilization and pregnancy. The appearance of the new technique of IMSI (Intra Cytoplasmic Morphologic Sperm Injection) which makes it possible to make a very thorough selection of the best spermatozoa in the ejaculate and to significantly increase the chances of obtaining fertilization and pregnancy from cryptozoospermic sperm. 17 - HEMOSPERMIA It is the presence of blood in the sperm V - APPENDIX Seminal biochemistry - It makes it possible to pose different types of pathology either having an origin of an obstacle being on the seminal tract, or of origin by malformation of the ways of excretion of the spermatozoa and more particularly at the level of the epididymis, duct vas deferens, seminal vesicles, prostate. The main substances of dosed are carnitine, alpha-glucosidase, citrate, acid phosphatases, zinc, fructose, etc. We deliver all over the world. For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
