permanently cured
Blog / 29 results found
PROSTATITIS TREATMENT BY PHYTOTHERAPY
DEFINITION
The prostatitis is an inflammation caused by a bacterial infection of the prostate.
This organ is an endocrine gland in the male genital system which has the function of producing the seminal fluid necessary for the development and mobility of sperm.
Conventional care for prostatitis requires the use of a cytobacteriological examination of the urine to identify the pathogen responsible for the disease.
As for herbal treatments, they help relieve the painful symptoms of prostatitis and speed up healing. Here is the natural treatment from the experts at Dawasanté herbal medicine to cure prostatitis. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
In this context, an effective mutual or insurance allows benefiting from high reimbursements of the expenses of consultations of urologists, ultrasounds and biological analyzes as well as herbal remedies prescribed by the doctors.
PLANTS TO RELIEVE PROSTATITIS
Saw palmetto to relieve benign prostatic hyperplasia
The saw palmetto (Serenoa repens) is a shrub whose berries contain sterols, substances which have the property of relieving the symptoms of BPH. Several cross-analyzes of clinical trials of good methodological quality have confirmed the interest of saw palmetto extracts in the treatment of BPH.
Commission E and WHO recognize the use of saw palmetto in "the treatment of urinary difficulties associated with BPH".
The EMA grants the status of “well-established medical use in the symptomatic treatment of BPH” only to saw palmetto extracts obtained with hexane as an extraction solvent. In addition, it only grants the status of "traditional use to relieve symptoms of the lower urinary tract associated with BPH" to saw palmetto extracts obtained with ethanol as an extraction solvent.
In France, drugs based on saw palmetto extracts are available for this use, only one of which uses hexane to extract the active ingredients and none uses ethanol.
African plum to relieve benign prostatic hyperplasia
The African plum (Pygeum africanum) is a tree whose bark is used to produce standardized extracts containing sterols and docosanol. A cross-analysis of eighteen clinical trials points to some efficacy of African plum extracts in the treatment of BPH, but less than that of saw palmetto extracts.
The EMA grants “traditional use to relieve symptoms of the lower urinary tract associated with BPH” status only to African plum extracts obtained with chloroform as an extraction solvent.
In France, drugs based on saw palmetto extracts are available for this use, none of which uses chloroform for the extraction of the active ingredients.
Pumpkin seeds to relieve benign prostatic hyperplasia
Pumpkin seed extracts (Cucurbita pepo) are recognized by Commission E to “facilitate the emission of urine in men suffering from BPH”. These seeds contain many substances (phytosterols, essential fatty acids, etc.) whose action on the prostate is poorly understood. There are few studies of pumpkin seeds used on their own (they are often combined with other herbs offered in the treatment of BPH). Their use in this indication is based on tradition.
The root of stinging nettle to relieve prostate benign
The roots of stinging nettle (Urtica dioica) contain lignans, with properties similar to those of female hormones and which could explain their effects on the prostate. However, clinical trials evaluating the effects of nettle root on prostate adenoma are of poor methodological quality. They point to the effectiveness of nettle root without providing scientific proof.
Unlike other official sources (WHO, Commission E and ESCOP), the European Medicines Agency (EMA) considers that these studies are inconclusive and that BPH being a disease that must be treated medically, the root nettle can not be considered a traditional treatment for this pathology.
Against prostate cancer: coffee and tomatoes
No plant to date can accompany or cure prostate cancer. On the other hand, in prevention, a large study carried out on 48,000 people by the National Cancer Institute was able to establish that consumption of 6 cups of coffee per day reduced the risk of 60% of suffering from cancer of the prostate. Unfortunately, consuming so much coffee daily is not reasonable: in addition to a phenomenon of dependence, excess caffeine causes many side effects, such as nervousness, restlessness, anxiety, palpitations, insomnia, stomach irritation. , diarrhea ...
The good news, decaffeinated offers the same virtues. It is indeed the polyphenols in coffee, and not caffeine, which gives it these preventive properties. A similar study published by the same institute also showed that consuming cooked tomatoes two to three times a week reduces the risk of developing prostate cancer by a third (compared to occasional consumption). Finally, healthy living remains effective prevention: avoiding exposure to toxic products, including pesticides (farmworkers are more exposed to this cancer), being active and limiting the consumption of red meat, cold meats and cheeses. fatty, while favoring large rations of fruits, vegetables and fish.
Treatment of prostatitis: treatment of inflammation and contributions of phytotherapy in case of prostatic hypertrophy
Prostatitis requires drug therapy with antibiotics and anti-inflammatories. This cure lasts from 3 to 8 weeks depending on the germ causing the infection.
Besides antibiotic therapy, the patient may resort to herbal remedies to relieve the symptoms of an enlarged prostate such as:
- bearberry: anti-inflammatory and soothing pain in urination, this plant is prescribed in cases of acute prostatitis and cystitis. Also called bear grape, it is an antiseptic and powerful antibacterial against pathogenic bacteria of the urinary tract.
- giant sequoia: antidepressant and hormonal regulator, giant sequoia buds help to treat inflammation in cases of prostatic hypertrophy. They are also effective in stimulating appetite and reducing the fatigue that accompanies prostatitis.
- pumpkin seeds: they are used in herbal tea against urinary disorders associated with an enlarged prostate. These seeds are also effective in relieving pain, facilitating mixing, etc.
- serenoa repens: the berries of this saw palmetto are used to treat inflammation of the prostate and prevent a recurrence
Massages of the genitourinary area of the prostate with essential oils (Scots pine, cypress, peppermint, etc.) are also recommended to relieve symptoms and prevent prostatitis.
Oral antibiotic intake and herbal medicine find their limits in severe prostatitis. Hospitalization for 2 to 4 days is then required in order to put the patient on intravenous antibiotic therapy.
Prostatitis: symptoms, types and risk factors of prostatic hypertrophy
Prostatitis causes enlargement of the gland and compression of the urethra and bladder. The first clinical signs of this prostatic hypertrophy are pain and discomfort when urinating, which results in the accumulation of urine residues at the origin of the aggravation and complication of the urological disease.
Inflammation of the prostate can be either:
- acute prostatitis: usually of bacterial origin, it is characterized by high fever, severe pain in the lower abdomen and general fatigue. The patient also experiences frequent urges to urinate despite the small amounts of urination expelled
- chronic prostatitis: of bacterial or non-bacterial origin, it is the consequence of a poorly healed urinary tract infection. This recurring pathology manifests itself by twitching in the lower abdomen, aggravated by retention of urine
The enlarged prostate is favored by:
- the stress
- sexually transmitted infections
- urogenital malformation
- prolonged sitting (office, car, plane)
- the practice of certain sports such as horse riding or cycling
Prostatitis affects young men. It is often associated with psychological impacts and a deterioration in the quality of life due to painful symptoms, incontinence and difficulty in sexual relations.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
VARICOCELE THROMBOSIS: Natural treatment
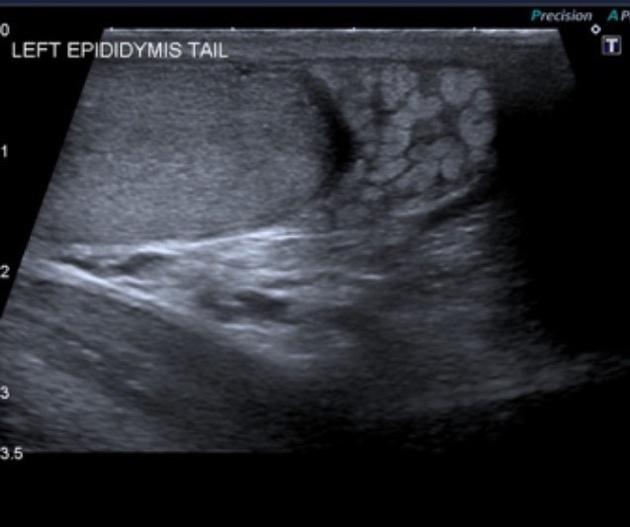
THROMBOSED VARICOCELE
Acute scrotal pain has various causes. Testicular torsion, twisting of the appendages, and epididymal-orchitis are common causes, while varicocele thrombosis is a rare cause. Read till the end to uncover the secret of natural herbal treatment for varicocele.
HOW DOES THIS COME ABOUT?
The thrombosis varicocele can occur after the operation or spontaneously. Five cases of postoperative thrombosis and five cases of spontaneous thrombosis have been described to date. The traditional advice in the management of thrombosed varicocele has been managed by the pharmacist and the patient. Here we present an unusual case of spontaneous varicocele thrombosis, as well as its presentation and surgical treatment. We would like to highlight the points of differentiation between spontaneous thrombosis and postoperative in vitro clot formation in varicoceles, these two entities being often confused.
But before that, Dawasanté experts provide you with a natural herbal treatment to treat spontaneous varicocele thrombosis. Click on the image below to discover this natural treatment.
How to cure varicocele with plants?
First, varicocele is not a fatality whose only way out is an operation. The use of natural plants makes it possible to permanently cure varicocele by avoiding surgical operation. The natural remedy for curing varicocele that we offer is completely herbal treatment. It is a natural remedy that cures varicocele successfully by strengthening the valves or valves located in the veins of the spermatic cords. So the veins become tonic and tenacious to facilitate the dynamic rise of blood along the veins. This to join the most important veins like the left renal vein and the inferior vena cava. So, it has proven its effectiveness with dozens of resolved cases. Associated with a suitable diet, it can treat varicocele quite easily.
Take advantage of this opportunity to discover our natural remedy for varicocele
To contact our experts please call or write to us on the following number, tel / WhatsApp: +22990431727
WE DELIVER ALL OVER THE WORLD
Presentation of the case
A 68-year-old man was presented with excruciating scrotal pain lasting a week. Doppler study of the scrotum revealed a left varicocele without a sign of epididymal-orchitis. He was treated with intravenous antibiotics, pain relievers, and an elevated scrotum. He had no relief and continued to have severe pain. The clinical examination was normal. The patient underwent semi-emergent exploratory surgery. Exploration revealed a normal testis with thrombosed varicoceles. The patient underwent a varicocelectomy. The postoperative patient had immediate pain relief. Histopathology revealed a varicocele significant thrombosis. A varicocelectomy sample (performed for primary infertility) was used for comparison. The points of differentiation between the two entities were noted.
Conclusion
Spontaneous varicocele thrombosis is a rare cause of acute scrotal pain. Pain out of proportion to clinical features is characteristic. Patients unresponsive to medical treatment may require varicocelectomy. Varicocelectomy can provide immediate relief. Histopathology is helpful in this disorder.
Acute scrotal pain has multiple etiologies. Torsion of the testis or its appendages and epididymal-orchitis are common, while varicocele thrombosis is a rare cause. Varicocele thrombosis can occur after the operation (5 cases) or spontaneously (5 cases). Spontaneous thrombosis can occur as a result of trauma or in patients with coagulation abnormalities. Kayes had reported that strenuous sexual or sports activities, infections, trauma, long hours theft, and medication could be the cause of the condition. There was no major predisposing mechanism to spontaneous thrombosis in our patient, but it is possible that vigorous sexual activity was the cause, because the patient developed pain after intercourse. Varicocele thrombosis (both spontaneous and postoperative) has been managed conservatively in all patients to date with medication (antibiotics and anti-inflammatory drugs) and scrotal support without a description of surgical treatment. There are conflicting reports regarding the timing and requirement of surgery in patients with thrombosed varicocele. Recommend non-operative conservative management, despite having submitted their patients to surgery. Therefore, the timing and necessity of surgery in patients with thrombosed varicocele become an extremely moot point. We present here a case of spontaneous thrombosis due to Varicocele, with particular emphasis on its presentation and surgical treatment. Spontaneous in vivo thrombi have always been confused with in vitro post varicocelectomy clot formation in the veins. We would like to highlight the histopathological differentiation between these two distinct entities.
OTHER NATURAL METHODS TO TRY
Perform Cooling Showers
Cooling is a method of reducing the body’s temperature. Testicular overheating is a major cause of concern for men with varicoceles, and can also cause infertility.[8]
It is shown to reduce inflammation markers.
Of note for varicocele, cooling can improve vein contractility and reduce the swelling of the veins.
How to Perform
- While taking a shower, run cold water over your testicles for 15–30 seconds.
- It helps to wash the whole scrotum, including the pubic area with cold water, because the veins run throughout the entire region.
- Perform cooling treatments as many times as needed per day to reduce testicular temperature but avoid overcooling.
Ginger for varicocele

Take a cup of ginger tea every day for 1 month.
Garlic for varicocele

Take 2 to 3 garlic pods and mash them.
Leave it for 15 mins.
Have it with a glass of water after 15mins.
Take it for 2 weeks.
Take advantage of this opportunity to discover our natural herbal treatment for varicocele
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022990431727
WE DELIVER ALL OVER THE WORLD
ASTHENOSPERMIA: NATURAL TREATMENT
What is asthenospermia?
The asthenospermia or asthenozoospermia is a sperm abnormality characterized by insufficient mobility of spermatozoa. It can alter a man's fertility and reduce the couple's chances of pregnancy because if they are not sufficiently mobile, the sperm cannot migrate from the vagina to the tube to fertilize the oocyte. However, Dawasanté experts provide you with a natural plant-based treatment to permanently cure asthenospermia.
Click here or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Asthenospermia can be isolated or associated with other sperm abnormalities. In the case of OATS, or oligo-astheno-teratozoospermia, it is associated with oligospermia (sperm concentration below normal values) and teratozoospermia (too high a proportion of abnormally shaped sperm). The impact on human fertility will be even greater.
Treatment
Here we are going to offer you a mixture of African plants, roots and barks that will help you heal your asthenospermia. Our blend of plants and roots has already enabled many men around the world to recover from their asthenospermia and experience the joy of being a father. What allows us to have excellent results is that we produce all these plants and roots ourselves and that we select only the best plants so that they retain all their therapeutic and medicinal virtues. They are the best roots and plants against asthenospermia.
Here are five plants and roots that will help you cure asthenospermia:
1. ROOTS MALE INFERTILITY
The effects of herbal remedies for treating asthenospermia problems have been proven by studies and hundreds of years of use. Here we are going to offer you a mixture of African plants, roots and bark that will help you heal your infertility. Our blend of plants and roots has already enabled many men around the world to heal from infertility and experience the joy of being a father. What allows us to have excellent results is that we produce all these plants and roots ourselves and that we select only the best plants so that they retain all their therapeutic and medicinal virtues.
2.The fruit of the Tribulus (Tribulus Terrestris)

Tribulus is expected to be very effective in improving sperm count, motility, and morphology when combined with changes in diet and exercise.
The main part of Tribulus that contributes to fertility in men is a constituent called protodioscin. This constituent improves the levels of DHEA in the male body. In men with erectile dysfunction, their DHEA levels have been found to below. Some studies have shown that protodioscin, extracted from Tribulus, increases the natural levels of DHEA necessary for a proper erection. Protodioscin is also the main constituent responsible for the aphrodisiac qualities of Tribulus. The increase in sexual desire while using this herb has been reported by both men and women.
A study by dawabio experts showed a 61% increase in conception in couples with anti-sperm antibodies (the immune system attacking sperm) taking Tribulus. The average duration of conception for a couple after treatment was 5 months. Tribulus is one of the best herbs for improving male fertility. Tribulus supports the production of LH and testosterone in men.
It also helps increase sperm count, motility, and health. It reduces the effects of anti-sperm antibodies.
3. Ginseng
Ginseng is often referred to as the king of all herbs and is proven to be the panacea for improving overall well-being. Ginseng is also an aphrodisiac and is used to treat sexual dysfunction and to improve sexual behavior in traditional Chinese medical practices. Data from animal studies have shown a positive correlation between ginseng's performance, libido and copulation, and these effects have been confirmed in case-control studies in humans. In addition, ginseng improves the quality of sperm and their number. We highly recommend it.
4. Maca

Maca has the ability to improve female fertility, which is why it is getting a lot of attention. It balances female hormones to improve fertility. However, this herb also has the ability to boost male fertility. This plant effectively improves the quality of sperm (the poor quality of sperm is a cause of male infertility). According to a study, men who consume maca regularly have more mobile sperm, more semen and more semen per ejaculation.
5. Ashwagandha

Ashwagandha is traditionally used to improve sexual health. It supports the endocrine system and promotes its better functioning. It also strengthens the hormonal balance in the body. It stimulates libido and improves sperm count in men. It improves stamina and also improves sexual performance.
The natural treatment that we offer to cure asthenospermia consists essentially of natural herbal teas. The herbal tea is composed of plants and roots whose active ingredients can restore the male hormonal balance, by increasing the level of testosterone, the number and the mobility of your sperm. It is the miracle solution to cure asthenospermia.
To discover our natural remedy to cure asthenospermia, click here
Causes of asthenospermia
As with all semen abnormalities, the causes of asthenospermia can be numerous:
- a morphological anomaly of the male gametes,
- an infection,
- presence of anti-sperm antibodies
- medication,
- a varicocele,
- a dietary deficiency,
- a renal failure,
- liver failure
- chemotherapy,
- exposure to radiation,
- excessive alcohol consumption,
- a deficiency in calcium, vitamin D or trace element ...
Symptoms
Asthenospermia does not show any symptoms other than difficulty conceiving.
Diagnostic
A semen analysis, or spermogram, is used to assess the mobility of the sperm. It should be remembered that only mobile gametes can fertilize the egg. Many medical analysis laboratories rely on the classification issued by the World Health Organization to classify spermatozoa:
- Level A (or I): progressive rapid sperm advance quickly and in a straight line,
- Level B (or II): the slow progressive spermatozoa advance slowly or in a curved line,
- Level C (or III): non-progressive spermatozoa move but do not progress,
- Level D (or IV): the sperm are immobile.
To be qualified as normal, the spermogram must show a minimum of 40% of motile sperm and 32% of sperm showing progressive mobility.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
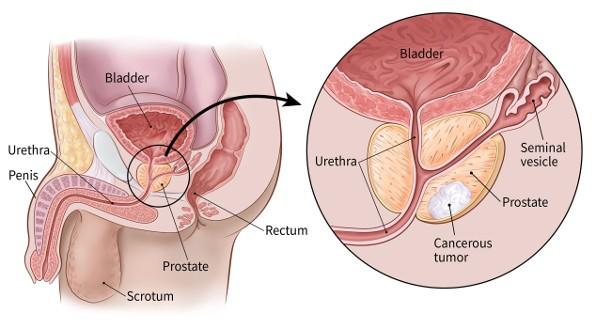
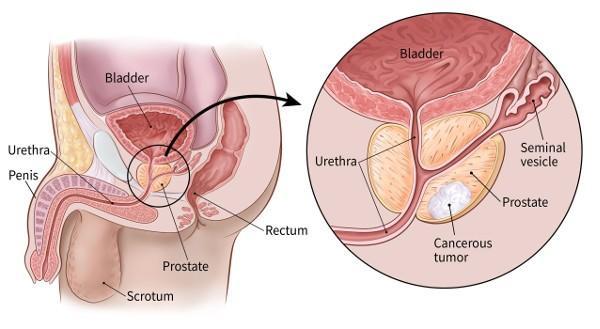
PROSTATE CANCER AND IMPOTENCE: Natural Treatment
Prostate Cancer and Impotence: Natural Treatment
Prostate cancer is the most common cancer, both in men and in the general population.
The prostate is a gland in the male reproductive system that plays a hormonal role and in the production of sperm. The appearance of cancer prostate is the transformation of prostate cells. Initially healthy, they multiply in an anarchic manner until they form a malignant tumor. In 95% of cases, cancers are in the histologic form of adenocarcinoma which develops from the cells making up the lining tissue of the prostate. If cancer starts out in the prostate, the tumor can then grow and invade other parts of the body. The course of this patient is often slow. As with all cancers, there are several stages of development. The evolution of cancer can be local or distant depending on the time of diagnosis. Prostate cancer can range from stage 1 to 4 depending on how widespread it is. To avoid having to suffer from this ailment which could have an impact on your whole life, we suggest that you approach Dawabio experts who are specialized in traditional treatments; as soon as you feel even a little pain or have doubts about your state of health. Here is the natural herbal treatment to permanently cure prostate cancer. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
What are the symptoms of prostate cancer?
This cancer is sometimes never discovered during the patient's lifetime. It is therefore only at a more advanced stage of development that the first symptoms appear. In the majority of cases, these are mainly urinary symptoms that affect urination (the action of urinating):
<> urge to urinate, excessive frequency of urination, painful urination, hematuria, acute retention of urine, dysuria. Difficulty urinating: difficulty starting to urinate or holding urine, inability to urinate, need to urinate frequently (especially at night), poor urine output, a burning sensation or pain when passing urine 'urinate. Blood in urine or semen. Frequent pain or stiffness in the lower back, hips, or upper thighs. Changes in urinary function: frequent urge, urge to urinate, urge to push, retention of urine, burning while urinating. Genital changes: painful ejaculations, or difficulty getting an erection. Predisposed people. benign prostatic hyperplasia. This enlarges, causing abnormalities in the functioning of the bladder and the sexual system. Thus, we can observe both urinary disorders (frequent urges to urinate, decrease in the force of the jet ...) and, often, more or less severe erection difficulties.
Prostate cancer does not cause sexual difficulties at the time. Rather, it is the treatment (intervention, certain medications, etc.) that can have repercussions on sexuality.
Treatment
It is possible to treat the prostate by a gentler method than surgery: ultrasound. This method called "ablatherm" or High-Intensity Focused Ultrasound consists of high-intensity ultrasound focused on the tumor. However, it remains less frequent and around fifty clinics or hospitals offer it in France.
Promising treatments
Certain molecules hold hope in the treatment of advanced forms, such as olaparib. The immunotherapy is also tested to boost the patient's immune system during chemotherapy.
Doctors also have other weapons at their disposal, such as hormone therapy which blocks the development of cancer by reducing the level of male hormones, or radiation therapy.
Several options are available to the doctor for treating prostate cancer, depending on its stage and speed of progression: resection surgery, external or internal radiotherapy (brachytherapy) or even simple monitoring. All these treatments should be discussed with the patient according to their risks and benefits. Thus, the risk of erectile dysfunction, more or less important depending on the treatment chosen, often comes into play in the decision.
Consequences of the operation
The operation often leaves after-effects. During the prostatectomy, the nerves of the erection can be damaged. This results in impotence in 60-90% of patients. But sometimes the erection can be recovered. It depends on the age and the damage to the erectile nerves. When this is not the case, there are treatments to cure impotence.
Another negative consequence of the operation: its impact on the urinary tract. The sphincters which allow the evacuation of urine are very close to the prostate. And when the prostate is removed, they are often damaged. Of urinary leakage appear mostly to the effort.
What are the risks of becoming impotent after prostate cancer surgery?
"It all depends on the treatments but there is a risk of impotence with the surgery. Now when the diagnosis is early enough, the surgery is a minimum. There are minimally invasive surgeries that allow preserving the shameful nerves. It is absolutely necessary to do so. talk with the doctor. There is less risk with irradiation or hormonal treatments but it all depends on the clinical case. If there is a loss of erection after the operation, there are still ways to 'intervene. If the shameful nerves have been preserved, one can act on the libido. Medicines can also help erection. Intra-cavernous injections and possibly penile prostheses can also be considered. But we must talk about it and we must especially not treat ourselves because we fear this kind of problem.
"Prostate cancer is very treatable if caught on time. However, impotence can be a complication of prostate cancer treatments and have an impact on the daily life of the cancer patient.
Several factors can increase the risk of impotence after the operation of prostate cancer, age, but also the frequency of sexual intercourse and erections: if they were low before the operation, this will increase the risk of impotence.
However, in some cases, impotence can be long-lasting. Treatments are then offered to bypass it such as injections and tablets.
The sooner the prostate cancer is treated, the lower the risk of impotence after the procedure.
Typically, impotence decreases and resolves within 18 months after the operation.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
MEDICAL TREATMENT OF THE EPIDIDYMAL CYST
MEDICAL TREATMENT OF THE EPIDIDYMAL CYST
A cyst is a lesion that develops within a tissue or organ. Testicular cysts are benign pathologies that can develop sometimes on the right testicle, sometimes on the left. They particularly affect children and young adults. There are two types of testicular cysts:
Cysts of the epididymis,
Dermoid cysts of the testis.
Cysts of the epididymis are benign tumors of unknown origin. They appear in the form of regular and painless swellings (single or multiple), located at the head of the epididymis.
To permanently cure this disease, Dawasanté experts provide you with a natural treatment based on medicinal plants. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
The cyst of the epididymis grows at the expense of the swollen part of the upper part or head of the epididymis. There may be one or more cysts within the same epididymis.
The intervention is proposed because of the discomfort or local pain that this cyst can cause. It aims to remove the lesion by the surgical opening of the bursa.
The absence of treatment has no consequence in itself, apart from the fact of a possible increase in the size of the cyst, discomfort, or local pain, which it can cause.
Symptoms and Pains
Concerning the cysts of the epididymis, the manifestations are mainly an increase in the volume of the bursa giving the sensation of having "a ball of fat" at this level, most often accompanied by local discomfort. As for dermoid cysts, the most evocative symptom is the increase in the volume of the bursa. Cysts "rarely cause pain, except in cases of large volume," said Dr. Antoine Faix, surgeon urologist and head of Andrology and Sexual Medicine of the French Urology Association Committee.
The spermatocele kystesdu often contain pools of dead sperm. Doctors don't know what is the cause. Often, epididymal cysts or spermatocele cysts develop for no particular reason.
There are no specific causes for the appearance of a cyst.
Most of the time, cysts in the epididymis don't hurt, so you may not have symptoms. You may only feel a lump when you examine your testicles. Your doctor might find it during an exam. As the cyst gets bigger, you may feel a heaviness in your testicle. You might also notice a lump or swelling behind or above your testicle.
Diagnosis: Who to conduct and what tests to do
If you experience the slightest discomfort and in any doubt, consult your doctor or herbalist quickly, as the symptoms suggesting the presence of testicular cysts are very similar to those suggesting the presence of malignant testicular tumors.
To make a diagnosis on the cysts of the epididymis, it is necessary to do an ultrasound, and possibly a histological examination (sample and tissue analysis) which will reveal the cystic nature of the tumor, and rule out the hypothesis of a cancerous tumor.
The diagnosis of cysts of the epididymis also involves a scrotal ultrasound. This may reveal rounded nodular and cystic formations of varying sizes in the testicular parenchyma (tissue). However, the definitive diagnosis is only established after the histological examination (tissue analysis) which makes it possible to rule out the cancerous hypothesis.
Treatments: What to do if a testicular cyst gets bigger?
Most of the time, this is not the case. Your doctor may prescribe pain relievers to make you more comfortable.
Aspiration is a procedure that can help relieve some of the pain and pressure from the spermatoceles. Your doctor will insert a needle into the cyst to remove some of the fluid.
If the cyst fills up and comes back, your doctor may perform a procedure called sclerotherapy. It will drain some of the fluid from the spermatocele. Then he will use a substance that causes the sac to fill with scar tissue. This tissue could reduce the risk of the spermatocele returning. But it can damage the epididymis. Your doctor can suggest this option only if you are not interested in having children.
In rare cases (if the spermatocele is interfering with your daily life) your doctor may remove it with surgery. It will numb the area, make a small incision (cut) in your scrotum or groin, and remove the growth.
Treatment of epididymal cysts relies on clinical and ultrasound monitoring when the benign cystic nature is evident.
Treatment of an epididymal cyst
The intervention takes place under general or locoregional anesthesia. A short incision is made at the level of the bursa. After checking the underlying testis, the cyst is completely removed by opening the envelope of the epididymis and dissecting as close as possible to the wall of the cyst. Sometimes the surgeon may need to remove part or all of the epididymis.
The intervention is carried out within the framework of an outpatient surgery hospitalization. It may, in some cases, require 1 or 2 days of hospitalization.
Pain at the incision is usually minimal and temporary.
For a few weeks, the bursa remains enlarged and small swelling around the testicle can sometimes persist.
Removal of the epididymal cyst is suggested in the event of an increase in the volume of the bursa and/or any local discomfort or pain associated with its presence. "A short incision is made at the level of the bursa. After checking the underlying testis, the cyst is completely removed by opening the envelope of the epididymis and dissecting as close as possible to the wall of the cyst. The surgeon can sometimes be having to remove part or all of the epididymis ", develops the site of the French Association of Urology. Surgery is also considered in the case of certain dermoid cysts, in the presence of small lesions.
Complicated cases of epididymal cyst
In the majority of cases, the operation takes place without complications. However, any surgical procedure carries a number of risks and complications, which are described below:
Hematoma: bleeding after the operation can lead to the constitution of a hematoma of the bursa, possibly extended to the external genitalia, a reoperation to drain the hematoma may be necessary.
Delayed healing: it may require prolonged local care.
Infection: the existence of discharge through the incision, general signs of infection such as fever, or local signs such as inflammation of the bursa can lead to the initiation of appropriate antibiotic treatment and the treatment of a possible abscess by your surgeon.
Testicular atrophy: it occurs exceptionally after surgery of the epididymis
Recurrence: his risk is extremely low.
Impact on fertility: partial or total removal of the epididymis will permanently prevent the passage of spermatozoa on this side. This risk is rarer in the event of simple removal of the cyst.
Persistence of local discomfort or pain: Removal of the cyst does not guarantee the total disappearance of discomfort or pain.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.

ANEJACULATION AND ASPERMIA: Natural treatment
Anejaculation and aspermia: how to fight this disorder of ejaculation and the absence of sperm by plants?
For a happy and fulfilling life, many couples wish to have a baby and start their own family. However, there are many sterile men and women who cannot fulfill this dream.
Male infertility is the inability to induce pregnancy. In rare cases, its cause will be aspermia.
What is aspermia, this ejaculation disorder
Aspermia is a condition related to the male reproductive organ. It is however found quite rarely in men, who if they suffer from this disease, will not ejaculate even a drop of semen at the time of orgasm. This happens when a person runs out of semen cells or when they ejaculate in their bladder (this is called retrograde ejaculation). However, there is a natural herbal treatment from Dawasanté experts to treat aspermia.
Click here or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Aspermia is not characterized by painful signs or symptoms. And it will only manifest itself during your sex or when you masturbate. In general, symptoms will vary from man to man, but the main ones are as follows:
· Infertility, that is, the inability to induce pregnancy;
·No or very little semen discharge at the time of orgasm;
A jet of urine after intercourse;
Traces of blood in semen or urine;
Mild to moderate pain in the scrotum or genitals when urinating.
What are the main causes of aspermia?
Aspermia can have many physiological and psychological causes. Here are the main reasons that can explain a lack of sperm during orgasm, and therefore male infertility.
Retrograde ejaculation
In this case, the semen is pushed back instead of coming out through the urethra during ejaculation. This condition can develop for a variety of reasons, including:
A failure of the bladder or closure of the glans which pushes the semen back;
- surgery of the testicles or prostate;
· But also a disease that damaged the nerves.
In many cases, diseases such as diabetes, spinal cord injury or multiple sclerosis can be responsible. Just like certain medical treatments, in particular for the prostate, antidepressants, antihypertensives, or antipsychotics.
Obstruction of the ejaculatory duct
This is the main cause of aspermia. This is called complete obstruction of the ejaculatory ducts, which may be total or partial. This condition can occur due to several factors such as:
The presence of congenital cysts in the ejaculatory ducts causing obstruction;
Inflammation of the prostate.
Tuberculosis of the prostate.
· But also a sexually transmitted disease, such as chlamydia.
A hormonal imbalance
An imbalance in hormonal levels can cause impaired spermatogenesis, which, but not always, causes aspermia. In a study of 126 men with aspermia who underwent geography and testicular biopsy, a correlation was found between the level of follitropin in the blood and the degree of inhibition of testicular aspermia spermatogenesis.
Testosterone (the male hormone par excellence) excreted in the urine and circulating in the blood plasma will be three times less important in the event of testicular aspermia. On the contrary, the plasma estradiol level will increase 1.5 times.
An infection
Aspermia can be associated with a urinogenital infection such as tuberculosis. But also sexually transmitted infections like chlamydia or herpes. Plasma infections are also very common causes of this ejaculation disorder. In all cases, the infection will most often be caused by mechanical obstruction of the ejaculatory ducts or by the secretion of an anti-sperm antibody.
Spinal cord injury
Aspermia can be associated with an injury to the spinal cord. A large number of senescent sperm in the seminal vesicles appears to be the main cause of poor sperm quality in men with spinal cord injury
Diabetes
Diabetes, especially juvenile, can also explain why you suffer from retrograde ejaculation or having sex without ejaculation.
Medical treatments
Aspermia may be associated with certain antihypertensive drugs with sympatholytic activity, such as guanethidine. Study results show that this is probably not due to retro sperm, but rather to an interruption in the transport of the sperm when it is released. Azoospermia can also be caused by;
Progesterone antagonists, such as mifepristone
Anabolic steroids,
Alpha-adrenergic receptor blockers (for the treatment of chronic prostatitis and benign prostatic hyperplasia);
· Excessive use of anticoagulants;
· Exposure to certain chemicals such as ethylene (especially among agricultural workers).
Alcohol consumption
Drinking alcohol excessively can lead to aspermia. One study showed that in alcoholics, the seminiferous tubules were mostly filled with degenerated sperm, which is thought to cause aspermia. Impotence decreased libido and a dysfunctional nervous system are commonly associated with alcoholism, which also can contribute to the development of this ejaculatory disorder.
Anti-carcinogenic treatments
Aspermia can be associated with radiation following cancer treatment. Irradiation doses are greater than 0.35 Gy cause aspermia which may be reversible. But the recovery time increases with higher doses. Chemotherapy can also contribute to aspermia, including causing anejaculation or retrograde ejaculation.
Therefore, it is recommended to combine chemo and radiation for children who have not yet reached their full growth potential in order to improve cure rates by reducing morbidity.
Congenital and developmental disorders
About 13.7% of infertile men with aspermia and 4.6% of those with oligospermia have a coexisting chromosomal abnormality. It could be a deletion of the Y chromosome or Klinefelter syndrome.
The latter has a prevalence of 3% in sterile patients, and 11% in men suffering from aspermia. In a recent study analyzing the seminal fluid, chromosomal formula, and testicular tissue in men with Klinefelter syndrome, aspermia was detected in over a third of cases.
Aspermia treatments: natural methods inspired by Ayurveda
Ayurveda has had natural solutions for treating aspermia for several millennia. Here are the most effective plants.
Asparagus Adscendens
This plant, also known as Safed Musli, is a natural remedy for ejaculation disorders. These roots increase the fertility, durability of the sperm. But also help boost your libido and maintain your erections.
It is therefore an effective remedy for erectile dysfunction and hormonal imbalances. It is found in France in the form of capsules, to be consumed twice a day for best results.
Tribulus Terrestris
This plant is also known to boost sperm production and therefore treat male infertility. It is also used in cases of low sexual desire and to treat erectile dysfunction. Component of many aphrodisiac food supplements like Go Viril, it improves sexual health in general but also lowers your bad cholesterol level and blood pressure.
Massages with essential oils
Massaging your body with essential oils is another natural way to treat aspermia. Essential oils such as chamomile, lavender, olive, or even rosemary have been used since Antiquity to promote the proper functioning of the body, and more particularly of the reproductive system.
For example, they have the effect of dilating the blood vessels and relaxing the nerves.
The Mucuna Pruriens
It is an excellent herbal product with amazing aphrodisiac properties. It is used to treat an obstruction of the testicles, low libido, premature ejaculation, low sperm count, and other sexual problems.
Mucuna Pruriens supplements work by increasing the production of gametes in the testes, which naturally increases sperm production. You can get it very easily in a capsule, to take it again twice a day.
How to medically treat aspermia?
Medical treatments have also been developed to overcome this ejaculatory disorder. In some cases, and if they are not enough to solve the problem, your doctor may recommend that you have the operation.
Oral treatments
Certain medications are prescribed to treat aspermia. They allow the neck of the bladder to be contracted during ejaculation, so that semen can flow directly through the urethra. Some also restore the function of the damaged nerve following disease.
Assisted reproduction
Some men with aspermia use this method to have a baby, including:
· Intrauterine insemination;
· In vitro fertilization;
The collection of sperm in the bladder.
The surgical intervention
The surgical procedure is performed if, and only if, aspermia cannot be treated with drugs or other complementary therapies. There are two main operations:
· Transurethral resection of the ejaculatory duct: This invasive procedure is used to correct obstruction of the ejaculatory duct if this is the cause of aspermia. This procedure leads to normal pregnancies but causes several complications (in particular at the level of the valves of the ejaculatory ducts);
· Ejaculatory duct recanalization: This is another procedure done to correct aspermia caused by obstruction of the ejaculatory ducts. A balloon catheter will dilate the blocked ejaculatory duct to allow sperm to flow freely.
We deliver all over the world.
For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number

ADENOMYOSIS AND INFERTILITY: Natural treatment
The adenomyosis uterus is often defined as the internal endometriosis in the uterus. It corresponds to the infiltration of the cells of the endometrium (uterine lining) into the muscle of the uterine wall (myometrium), which results in the thickening of the myometrium. However, Dawasanté experts provide you with a natural treatment based on medicinal plants to permanently cure adenomyosis.

Adenomyosis can be diffuse or focal (one or a few foci within the myometrium), superficial or deep. Diffuse adenomyosis is the most common. Namely: there is a link between endometriosis and adenomyosis but a woman can have endometriosis without adenomyosis or have adenomyosis without endometriosis.
This uterine pathology can affect fertility.
To discover our natural remedy for adenomyosis, click here
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
HOW ADENOMYOSIS RELATES TO INFERTILE
Adenomyosis is the presence of ectopic endometrial mucosa in the uterine muscle. The clinical symptomatology of adenomyosis is dominated by menometrorrhagia with pelvic pain and infertility. The diagnosis of adenomyosis is accessible on ultrasound, it will be confirmed or confirmed by MRI. Adenomyosis can be isolated or associated with endometriosis. The role of adenomyosis in female infertility is starting to be well-defined (chronic inflammation with ovulation disorder, contractility abnormalities and difficulty of implantation). The therapeutic modalities are medical, surgical and may involve embolization of the uterine arteries.
Always for in-depth the relationship between adenomyosis and infertility :
- Ballester et al. evaluated the cumulative rate of pregnancy after surgical treatment of colorectal endometriosis (68.6%) and found, in women with adenomyosis a rate of 19% against 82.4% in women without adenomyosis (OR: 0.34 with a 95% CI % (0.12-0.99)).
- -Kunz et al. conducted in 2005 a study in 227 infertile women, 160 with endometriosis and 67 without. The prevalence of adenomyosis is 79% in women with endometriosis, rising to 90% in those with a fertile partner (mobility of type “a” sperm greater than 20%), a significant difference (p <0.01). This can be explained by an alteration in the uterine transport of sperm due to changes in the junction area.
- -Kissler et al. studied these disturbances in uterotubal transport in hysterosalpingography. There was a correlation with the increase in the junction area and a difference between focused and diffuse adenomyosis. In the group of women with diffuse adenomyosis, 10% bilateral and 15% contralateral transport was observed. In focused adenomyosis, the rates were 40% and 35%, respectively.
These results are therefore arguments for IVF management of women with adenomyosis. Adenomyosis is responsible for a 30% decrease in the chances of pregnancy in AMP as well as an increase in the rate of spontaneous miscarriages. In infertile women with adenomyosis, there is a decrease in the implantation rate. In the case of gastrointestinal endometriosis surgery, the impact of adenomyosis is even greater, as mentioned above. Indeed, a review of the literature evaluating pregnancy rates after surgery for digestive endometriosis, reports a 68% reduction in the chances of pregnancy in adenomyosis. However, it seems that adenomyosis has an impact on embryo implantation rather than fertilization. However, these data should be qualified with the prospective study by Benaglia, published in 2014, which showed that asymptomatic adenomyosis did not affect the rates of implantation and pregnancy in IVF.
One of the most important parameters for implantation is the junction zone, the thickness of which increases between 20 and 50 years and decreases under treatment with GnRH agonists.
Protocols using a GnRH antagonist have a negative effect on the pregnancy rate. On the other hand, there is no significant difference in IVF / ICSI, between patients with or without adenomyosis, in the event of long protocols (more than 3 months) using a GnRH agonist. Preliminary series argues for a beneficial effect of GnRH analogues, prescribed for a period of 2 to 6 months, on the chances of pregnancy
The adenomyosis is responsible for pathophysiological disturbances decreasing the chances of pregnancy ; however, its effect during IVF / ICSI management is attenuated by the prescription of long protocols with GnRH agonists. There is also an increase in spontaneous miscarriages, probably related to a particular myometrial activity, according to some authors. From a therapeutic point of view, the medical treatment is disappointing (except the agonists ) and the surgical treatment must be reserved for the localized forms ( adenomyosis ). Therefore, the support in AMP should be preferred in cases of adenomyosis but remains complex. In the coming years, the SPRMs (currently under study) could provide satisfaction.
However, the high suspicion of its relation to endometriosis, a much more well-known pathology and having a close relation to infertility, has caused us to think for a long time in possible relation with the difficulty to get pregnant, and also suggested a link with worse outcomes after assisted reproduction treatment.
Currently, in view of the effects that adenomyosis produces on the uterus, it has been verified that there is a high discrepancy between what we observe and what the patient feels. That is to say that it is possible that we are in the presence of a uterus very affected or even deformed by adenomyosis and that this does not cause any symptoms in the patient or, on the contrary, that we observe slight clues and that we were dealing with a patient with severe symptoms. A uterus that is capable of producing very severe symptomatology could equally present difficulty in permitting embryonic implantation and therefore cause infertility which is difficult to resolve via infertility treatment.
Its relationship to repeated embryonic implantation defects has been suggested in much research, but cannot be confirmed due to inconsistency in diagnosing adenomyosis. What is clear is that in a patient with an implantation defect (more than 4 embryos transferred of good quality without obtaining pregnancy) the diagnosis of adenomyosis is of particular interest since a targeted and specific treatment of this pathology could improve the results of reproductive treatment.
To discover our natural remedy for adenomyosis, click here
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Uterine adenomyosis: symptoms and natural treatment
If you suffer from a very heavy and painful period, you could suffer from adenomyosis: find out what are the causes and symptoms of this pathology.
Uterine adenomyosis is a disease that occurs with swelling inside the walls of the uterus. The woman, therefore, experiences severe pain, bleeding and colic, in addition to other symptoms that we will see later.
This disease occurs when the tissue that usually lines the uterus (endometrial tissue) grows into the muscle wall of the uterus. The excess tissue continues to function normally, swells, deteriorates and causes bleeding during the menstrual cycle.
Adenomyosis is a mild disease, common in women who give birth between the ages of 35 and 50. This disease can present in two ways, depending on the amount of damaged tissue:
- Diffuse adenomyosis: in this case, the uterus is partially or totally involved.
- Focal adenomyosis: also known as an adenomyoma. It is an isolated mass, placed inside the myometrial.
How to get pregnant despite adenomyosis?
If you have adenomyosis and want to get pregnant and skip the operation, you've come to the right place. Here is a very effective natural remedy to cure adenomyosis permanently. It is specially designed for patients who do not feel like having surgery, who want to get pregnant and have a normal pregnancy. This natural herbal treatment for adenomyosis will remove the pain you feel during your period and allow you to have normal cycles. It outperforms conventional treatments that relieve pain, but don't get to the root of the pain. How does it work?
Our herbal tea contains plants that reduce estrogen levels in the blood. This helps block the proliferation and bleeding of adenomyosis lesions. These herbal remedies are rich in antioxidants that inhibit enzymes that lead to pro-inflammatory prostaglandins. These are nutrients in high doses anti-inflammatory. This will definitely put an end to the pain you feel during your period. We know that many of you have had adenomyosis treatment or surgery, but the pain returned years later. No panic ladies! With us, no recurrence, no side effects. You will be permanently cured of adenomyosis.
To discover our remedy for adenomyosis, CLICK HERE
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
NABOTH CYST AND INFERTILITY: Natural treatment
NABOTH'S CYSTS FOR INFERTILITY
The Naboth cysts are tiny cysts that form on the surface of your cervix. Your cervix connects your vagina to your uterus. It is sometimes called the cervical canal. Naboth's cysts are filled with mucus which is secreted by the cervical glands. Sometimes the small bumps are called cervical cysts, mucinous retention cysts, or epithelial cysts. Naboth's cysts are quite common. They do not pose a threat to your health and are not a sign of cervical cancer.
If you are looking for a natural treatment to fight Naboth cysts, the experts at Dawasanté have the solution for you. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
NATURAL TREATMENT
The natural treatment that we offer to cure Naboth cysts is essentially made from natural herbal teas. Herbal tea is made up of plants whose active ingredients are able to suppress the symptoms that you feel and allow you to have a total recovery. This is the solution to find a normal life.
To discover our natural remedy to cure Naboth cysts, click here
The causes
The cervix is the tissue that connects the uterus to the vagina. The cervix has two distinct parts lined up in two different types of cells:
- Glandular cells, which line the area of the cervix closest to the uterus
- · Squamous cells, which line the part of the cervix closest to the vagina
Glandular and squamous cells meet to form an area called the transformation zone. This area undergoes many changes over the course of a woman's life, especially during pregnancy and childbirth.
Cells in the transformation zone are constantly changing, making this zone very susceptible to abnormal cell growth.
A number of conditions can cause a lump on the cervix and are described in the following sections.
Cervical polyps
A cervical polyp is a bulb-shaped, non-cancerous growth that develops on the cervix. The appearance, size and color of polyps can vary widely. It is not known why cervical polyps develop, but some of the possible causes of these polyps can include:
- High estrogen levels
- Inflammation of the cervix
- Blocked blood vessels
In most cases, cervical polyps are benign, with only 1 in 1,000 being cancerous. The doctor can remove the cervical polyps in a simple procedure.
Pregnant women can develop small white bumps called Naboth's cysts. They can form when excess skin cells block the mucous glands lining the cervix. Women may not know they have a Nabothian cyst until their doctor finds one during a routine pregnancy check-up. Although Naboth's cysts usually don't cause symptoms, they can rupture and release a foul-smelling discharge or blood.
Cervical fibroids
Fibroids, or myomas, are non-cancerous tumors that usually grow in muscle tissue in the uterus. Although rare, fibroids can also grow in the cervix.
Fibroids can vary in size and some can grow large enough to cause weight gain and swelling of the lower abdomen. Fibroids are almost always benign. Cancerous fibroids are rare and occur in less than 1 in 1,000 cases.
Cervical cancer
A lump on the cervix may indicate cervical cancer. Early Stage Cervical Cancer May Not Cause Symptoms Reliable Source. Cervical cancer can affect one or both types of cells that line the cervix.
Symptoms
Naboth cysts can cause a variety of symptoms if any. They can cause the following symptoms:
- Heavy or painful periods
- Bleeding between periods
- Foul-smelling vaginal discharge
- Pressure or swelling of the lower abdomen
- Frequent need to urinate
- Pain in the lower back, pelvis or legs
- Pain during intercourse
To diagnose the underlying cause of a lump on the cervix, the doctor will collect the following information:
- Family history
- · medical background
- Current drugs
They may also perform a physical exam and other diagnostic tests:
· Ultrasound tests use sound waves to create images of structures inside the abdomen and pelvis.
· MRI scans use a strong magnetic field and radio waves to create detailed images of the tissues inside the body.
· Hysteroscopy can help diagnose conditions affecting the uterus. During the procedure, a healthcare professional will guide a thin tubular device called a hysteroscope through the vagina and uterus. The hysteroscope captures images inside the uterus and transmits them to a computer.
· Laparoscopy uses a camera attached to the end of a thin tube to examine female reproductive organs.
· Biopsies are small samples of tissue from the lining of the cervix. After removal, the doctor will send the sample to a laboratory for analysis. Biopsies can detect the presence of precancerous or cancerous cells.
Complications
Usually, fibroids do not cause serious complications. However, untreated fibroids can increase the risk of infertility and cause problems during pregnancy, such as:
- Placental ablation
- · premature delivery
- · miscarriage
Having fibroids does not increase the risk of developing cancerous fibroids. Naboth's cysts rarely cause serious complications and often go away without treatment.
However, large Naboth cysts can distort the shape of the cervix. These cysts may require excision or surgical removal.
Medical treatments
Benign growths, such as cervical polyps and Naboth's cysts, often do not require treatment.
However, even benign growths can cause problems. Cysts and polyps can grow large enough to distort the shape of the cervix and may require surgical removal or drainage.
Treatment options for bumps on the cervix may include:
Surgery
Here are examples of surgical treatments for bumps on the cervix:
· Polypectomy: this method is to remove a polyp of the cervix with forceps or a string. This procedure usually takes place in an outpatient clinic.
· Electro-coagulation ablation: This method uses the heat of an electric current to remove a cervical cyst.
· Myomectomy: During this procedure, a surgeon will remove the fibroids through a small incision in the lower abdomen.
Medication
Gonadotropin-releasing drugs (GnRH) agonists and antagonists can treat symptomatic cervical fibroids.
GnRH drugs cause the body to make less estrogen and progesterone, which effectively reduces the size of fibroids without harming fertility.
Taking over-the-counter pain relievers, such as ibuprofen and acetaminophen, may help reduce cramps and lower back pain associated with the cervical lump.
Risk factors
It is not known exactly what causes the bumps on the cervix. However, there are certain factors that can increase the risk of developing a lump on the cervix.
Risk factors for cervical lumps include:
- Taking birth control pills containing estrogen
- Having a family history of fibroids, polyps, cysts or cervical cancer
- Inflammation of the cervix due to infections such as HPV, herpes, or yeast infections
- Be overweight or obese
- Having a weakened immune system
Prevention
Maintaining a healthy weight and controlling hormone levels can help reduce the risk of developing a lump on the cervix.
However, leading a healthy lifestyle does not guarantee complete protection against conditions that can cause a lump on the cervix. Participating in routine pelvic exams and Pap smears can help detect cervical abnormalities at an early stage.
The widespread use of regular Pap smears over the past decades has resulted in a significant reduction in the rates of cervical cancer deaths and diagnoses.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.










