fertility loss
Blog / 72 results found
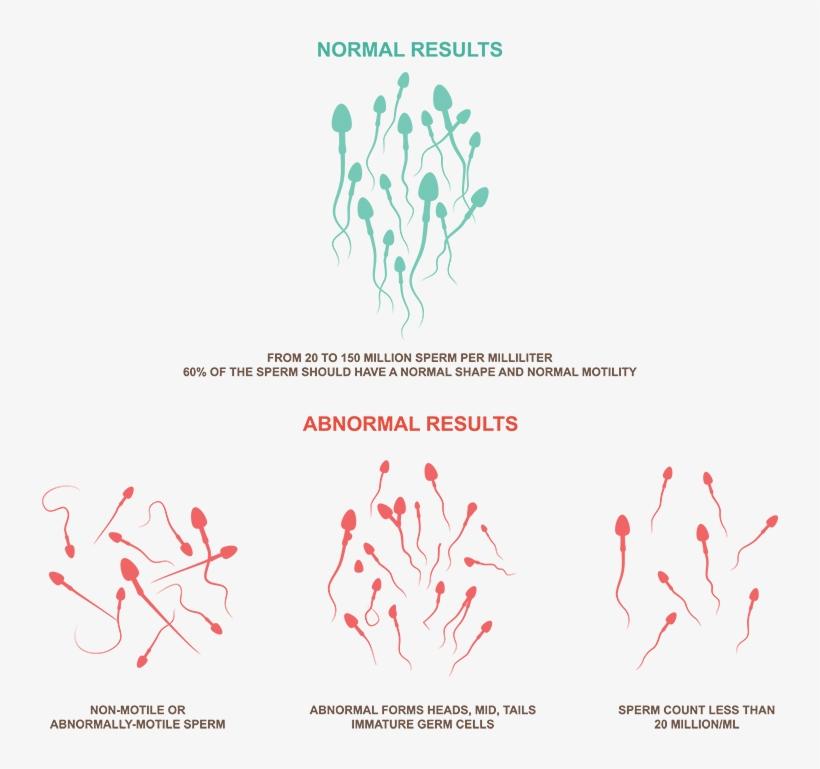
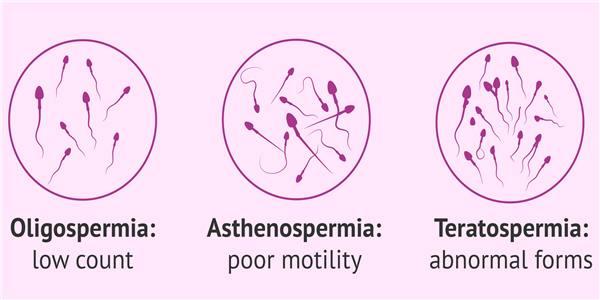
TYPES OF TERATOSPERMIA: mild, moderate, and severe
The teratospermia (or teratozoospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. This is how the Dawasanté experts provide you with a natural treatment to treat all your fertility problems related to the quality and quantity of your sperm.
Click HERE or on the image below to discover this natural treatment
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Teratozoospermia or teratospermia is a seminal alteration that involves a high percentage of abnormally shaped sperm.
It is a cause of male infertility, the severity of which will depend on the greater or lesser number of amorphous sperm cells in the semen.
According to the different criteria used to assess the degree of teratozoospermia, we can distinguish 3 types: mild, moderate, or severe.
1-Classification of teratozoospermia
When a man performs a spermogram to assess the quality of his sperm, in the results report, he will obtain the values of all seminal parameters, including sperm morphology.
A man is considered to have teratozoospermia when the percentage of sperm with normal morphology in his seminogram is less than 4%, according to criteria established by the World Health Organization (WHO) in 2010.
On the other hand, some labs also use Kruger's strict criteria to diagnose teratozoospermia. According to Kruger, a man suffers from teratozoospermia when less than 15% of his sperm has a normal form.
Percentage of normal sperm
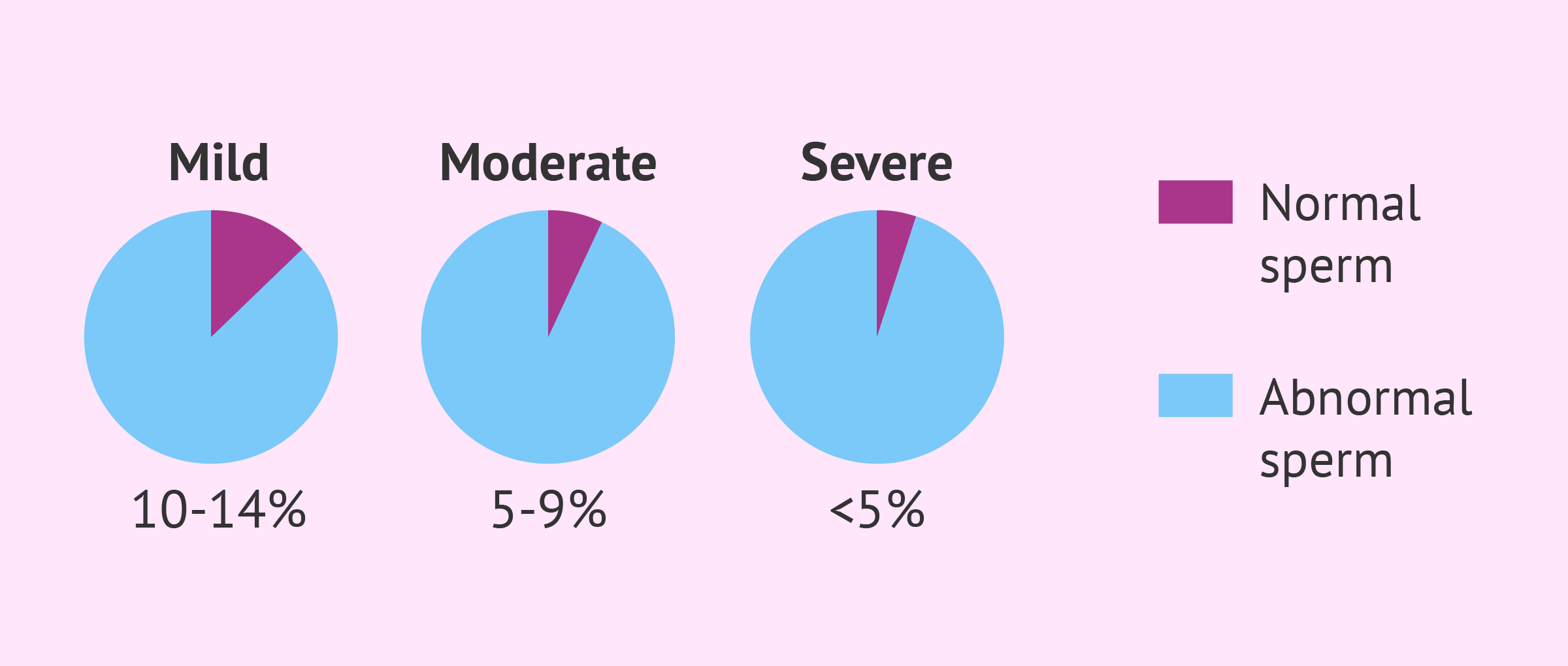
Since the WHO benchmark is so low, there is no point in talking about types of teratozoospermia based on the number of normal sperm. Therefore, for the classification of spermatozoa in this sense, it is better to use Kruger's criterion, which is stricter than the previous one.
1-1 Mild teratozoospermia
A man suffers from mild teratozoospermia when the number of normal sperm in his spermogram ranges from 14% to 10%.
The rest of the sperm will have an abnormality in their head, neck or tail. Despite this, men with mild teratospermia do not have a bad prognosis for having children.
If assisted reproduction techniques are necessary to achieve pregnancy, artificial insemination (AI) and in vitro fertilization ( IVF ) may be performed, depending on the concentration and mobility of the sperm.
The shape of the sperm is important for the fertilization of the egg. However, men with mild teratozoospermia can achieve a natural pregnancy.
In addition, there are various dietary supplements that contain vitamins and antioxidants that help in the maturation of sperm and can improve their morphology.
If you are interested in this topic, you can read the following article: Treatment of teratozoospermia.
1-2 Moderate teratozoospermia
Moderate or severe teratozoospermia is diagnosed when sperm results show that only 9-5% of sperm have a normal shape.
With this diagnosis, it is quite complicated to have children naturally. To achieve a pregnancy with moderate teratozoospermia, an in vitro fertilization technique such as ICSI will most likely be necessary.
The ICSI (Intracytoplasmic Sperm Injection) is based on the selection of spermatozoa under a microscope and their direct injection into each egg and fertilization.
PMA, like any medical treatment, requires that you trust the professionalism of the doctors and clinic you have chosen. Obviously, not all are the same. The Fertility Report selects the most advantageous clinics for you based on our rigorous quality criteria. In addition, the system performs a comparison of prices and conditions offered by different clinics to facilitate your decision making.
1-3 Severe teratozoospermia
When the spermogram morphology test shows a normal sperm value of less than 5%, the man has severe or severe teratozoospermia.
Sperm with good morphology is therefore very few in number and, therefore, the possibility of achieving natural pregnancy is very low.
Spermatozoa with alterations in their morphology have problems progressing gradually, they have more difficulty reaching the egg, penetrating its thick pellucid layer and also fusing its male nucleus with the female one. The consequence of all this is that they can lead to fertilization failures.
Teratozoospermia and fertilization failure

The most suitable assisted reproduction technique for extreme teratozoospermia is ICSI or its improved variant: IMSI.
The IMSI is the same as intracytoplasmic sperm injection, but with the use of a microscope magnification of 6300, so it is possible to get very close to the sperm morphology and make a better selection.
2-Your frequently asked questions
2-1 Can we cure severe teratozoospermia?
If a man has less than 5% of sperm with normal morphology, it is very difficult to regain a normal value with natural or pharmacological treatment. Improvement can be seen over time, especially if the man maintains a healthy lifestyle.
On the other hand, if the teratozoospermia appears associated with another pathology such as, for example, varicocele, it is possible that the spermogram improves its parameters during a surgical intervention to eliminate the varicocele.
2-2 What is isolated teratozoospermia?
Discrete teratozoospermia means that the affected parameter, in this case, the morphology of the sperm, does not have a value much lower than the reference value. Therefore, it would be a mild teratozoospermia.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
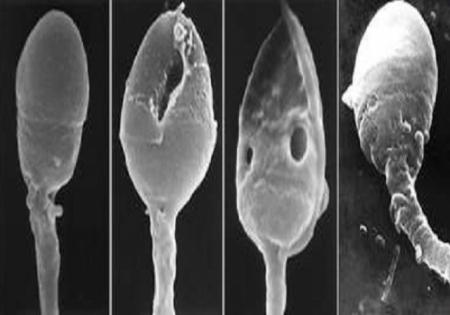
THE CAUSES OF TERATOSPERMIA: Natural treatment
The teratospermia (or teratozoospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. Dawasanté experts advise you to opt for a natural treatment without operation, against teratospermia.
Click HERE or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Teratozoospermia refers to the poor morphology of the sperm in a man's ejaculated semen.
These men have lower seminal quality and sometimes suffer from infertility and difficulty achieving pregnancy.
The causes of teratozoospermia are mostly unknown. However, we are going to address the possible alterations caused by these abnormal sperms in semen.
1-Defects in spermatogenesis
Most experts agree that the morphological changes in sperm occur during the last phase of their formation.
The spermatogenesis is the process by which sperm are formed in the testicles, which lasts about 3 months.
More precisely, spermiogenesis is the last phase of spermatogenesis, during which the spermatozoa, which already have their genetic content formed, undergo a process of maturation and acquire their characteristic morphology.
Once the sperm have their oval head and tail formed, they are released into the seminiferous tubules to follow their path.
Therefore, it is not surprising that any abnormality or alteration in spermiogenesis results in abnormalities in the head, neck or tail.
2-Reversible teratospermia
Teratozoospermia can be reversible or irreversible depending on the specific cause.
With reversible teratospermia, men can regain their seminal quality after a few months if they have received the appropriate treatment.
To check this, it is necessary to do another spermogram and compare it with the previous one.
We will now discuss the possible causes of reversible teratozoospermia:
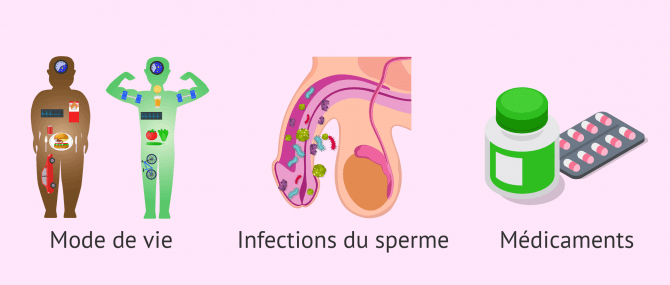
2-1 Way of life
Although it may seem surprising, the lifestyle of men greatly affects the quality of their semen.
During times of stress and anxiety, sperm morphology may deteriorate, as many other parameters such as concentration and mobility.
The abuse of alcohol, tobacco, or other drugs are also factors linked to alterations in sperm.
Prolonged exposure to testicular heat affects spermatogenesis. Therefore, the bad habit of placing the computer on your legs, wearing tight clothes, or driving for a long time can cause teratozoospermia.
Testicular heat causes teratozoospermia

Finally, diet and sport also contribute to male fertility.
Men who are planning to become pregnant with their partner are recommended to maintain a good lifestyle, eat a balanced diet, exercise regularly and not consume substances that are harmful to the body.
2-2 Seminal infections
Semen infections refer to the invasion of microorganisms, bacteria, and viruses, into the male reproductive system.
Its presence is found in urine and semen, causing alterations in the sperm, as well as inflammation and obstruction of the seminal ducts.
The most common bacterial infections in the testes are chlamydia and gonorrhea. These infections can be fought with antibiotics and male fertility can be restored. If you would like more information on this, you can access the following article: Types of infections in seminal fluid.
The episodes of fever caused by flu or another disease may also occasionally affect sperm quality.
2-3 Pharmaceuticals
Sex hormones like testosterone, LH, FSH and inhibin have a very important role in the regulation of spermatogenesis.
Therefore, any drug that changes the appropriate levels of these hormones or affects their secretion by the brain has negative consequences for sperm production.
As we have already said, the alteration of the phase of spermiogenesis prevents the correct maturation of sperm and causes teratozoospermia.
Reversible causes of teratozoospermia
3-Irreversible teratospermia
If a man with teratozoospermia fails to improve his second spermogram after receiving treatment, one may begin to suspect that the teratozoospermia is irreversible.
In these cases, the couple will have to resort to assisted reproduction if they want to become a parent because it will naturally be very difficult to obtain a pregnancy.
In addition, there are other pathologies or situations that cause irreversible or prolonged teratozoospermia. The most relevant cases are examined below:
3-1 Cancer treatment
Chemotherapy and radiation therapy alters both sperm stem cells and sperm production, causing severe teratozoospermia and other more serious changes.
For these reasons, all men with cancer are advised to save a semen sample if they wish to have children in the future after they have overcome the disease.
3-2 Genetic diseases
It is one of the most difficult causes of diagnosis. Normally, when it has not been possible to determine the pathology that causes teratozoospermia, it is attributed to a genetic factor.
Defects in the genes or chromosomes of the sperm are a serious problem because they cannot be corrected.
3-3 Associated pathologies
Teratozoospermia can also result from other diseases that mainly affect the testes, for example:
- Trauma or blows to the testicles, especially in childhood
- Testicular varicocele
- Meningitis
- Diabetic sugar
In addition to all this, the age of males can also affect the morphology of the sperm. In particular, it has been observed that men over 45 have a higher rate of abnormal sperm in their semen.
Irreversible causes of teratozoospermia

4-Your frequently asked questions
4-1 Can live sperm have poor morphology?
By Zaira Salvador (embryologist).
Yes, teratozoospermia can be present in both living and dead sperm.
Dead sperm do not always have a bad morphology. Sometimes they are confused with immobile sperm and it is necessary to make a tincture to find out whether they are viable or not.
4-2 Can leukospermia cause teratospermia and male infertility?
By Zaira Salvador (embryologist).
Leukospermia, also known as leukocytospermia, is the appearance of leukocytes in semen, with a concentration level greater than 1 million per milliliter. The cause of this seminal pathology is an infection of the male reproductive tract which must be treated with antibiotics as it can affect spermatogenesis and cause oligospermia or teratozoospermia.
You can find the information in our article: Leukocytes in semen.
4-3 Are the causes of teratozoospermia and asthenozoospermia the same?
By Zaira Salvador (embryologist).
In most cases, asthenospermia and teratospermia have the same causes. The two seminal parameters are usually changed in the seminogram, known as astenoteratozoospermia. However, this is not always the case.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
TERATOSPERMIA OR TERATOZOOSPERMIA: definition and treatment
Teratozoospermia or teratospermia is an alteration that occurs in men when more than 95% of their sperm have an abnormal morphology.
Therefore, teratospermia is considered a cause of male infertility due to a sperm factor, and its origin is varied and sometimes unrecognized. This is why the Dawasanté experts provide you with a natural treatment to improve the quality and quantity of your sperm; which will allow you to quickly conceive.
Click HERE or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number
There are several treatments to be able to conceive a child with sperm affected by teratospermia depending on whether the man's sperm has other spermatic disorders, such as, for example, sperm concentration or mobility.
1-Teratozoospermia: what is it?
Poor morphology of the spermatozoa, indeed the latter can present defects in the head, middle part or neck, or the tail.
The WHO estimates that a man with 4% sperm with a normal form (at least) does not have fertility problems. In lower quantity, we are talking about male infertility by teratospermia. This baseline changed in 2010, previously it was 14%, so it is possible that on other sites you will find that teratospermia is considered to be more than 85% abnormal.
According to the strict Kruger criterion, values equal to or greater than 15% of sperm with normal morphology are considered normal. This criterion is always stricter than that of the WHO, but the WHO is the one that is taken as a global reference.
The count of sperm of good or bad morphology is carried out through a medical examination called a spermogram, where the structure of the sperm is analyzed under a microscope.
There are several laboratories which in addition to the Kruger criteria, add those of the WHO.
If the medical report does not specify the details of the analysis to the laboratory, the parameters dictated by the WHO in 2010 are the reference values used.
Diagnosis of teratozoospermia

2-Causes
Teratozoospermia involves male infertility because the sperm that reach the oocyte are unable to fertilize it due to their poor morphology.
The causes that cause the existence of amorphous sperm in human semen are manifold and difficult to diagnose. Here they are:
- Genetic disorders
- Chemotherapy and radiotherapy
- Seminal infections and orchitis
- Varicocele and other testicular disorders
- Febrile period
- Diabetes or meningitis
- Tobacco, alcohol and drug abuse
- Poor lifestyle: poor diet, exposure to toxic substances, clothes that are too tight
Some of these factors can cause reversible teratozoospermia, which goes away with fever, infection, or periods of stress. In the same way, it is possible to recover a good spermatic morphology by improving one's lifestyle, diet, quitting smoking, etc.
3-Types
Sperm morphology defects are classified according to their position on the head, at the neck or at the tail. However, to diagnose teratospermia, all defects are taken into account.
Sperm is considered normal when it has a head with an oval shape and an acrosome inside. The neck or middle piece is slightly larger than the tail, and the tail is elongated and straight.
After analyzing the morphology of the sperm during the spermogram, it is possible to determine the degree of teratozoospermia depending on the seminal quality. For this, the laboratories use the Kruger criteria. Here is their classification:
- Mild teratozoospermia
- 10% to 14% of spermatozoa have normal morphology.
- Moderate teratozoospemia
- the percentage of normal sperm varies between 5% and 9%.
- Severe teratozoospemia
- less than 5% of sperm have normal morphology.
As we have commented before, it is the WHO criteria that are used to diagnose teratospermia, and therefore, this classification is obsolete. However, it is still possible to find it on some spermograms.

3-1 Teratozoospermia index
This seminal parameter is used to know the number of defects that each sperm has. It is possible that sperm has only one malformation, or several distributed over several parts.
In order to calculate the rate of teratospermia (TZI), we use the following formula: TZI = (c + p + q) / x , where each variable means:
- c = head malformations
- p = malformations of the middle part of neck
- q = tail malformations
- x = total number of abnormal sperm
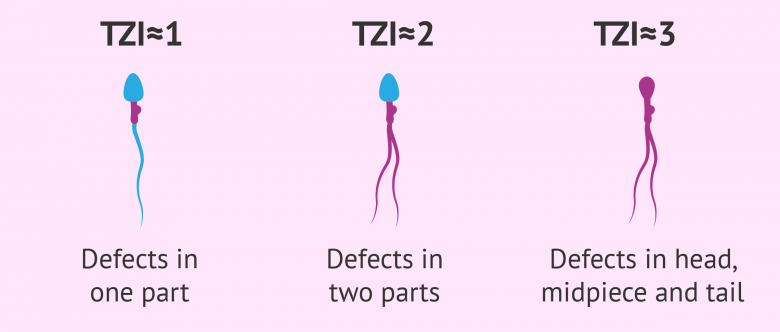
The interpretation of these results is carried out as follows:
- TZI close to 1
- sperm with abnormalities in one area
- TZI close to 2
- spermatozoa with abnormalities in two areas
- TZI nearly 3
- sperm with defects on the head, neck and tail
It is important to note that the same seminal sample can present sperm of three types: one malformation, two, or three. The rate of teratospermia will indicate which type is most present.
4-Teratospermia and pregnancy
A man with teratospermia could have a natural pregnancy without problems if the rest of the seminal parameters such as concentration or mobility are not affected.
However, in cases where the pregnancy is delayed, it is possible to follow the doctor's recommendations to recover the correct sperm morphology.
On the other hand, if teratospermia has a genetic cause or is congenital, it is more difficult to find an effective treatment to cure it.
4-1 Natural treatments
First of all, men who suffer from teratospermia need to change their lifestyle and put aside bad habits like tobacco or alcohol.
A healthy and balanced diet always helps to recover some of the fertility. In concrete terms, foods rich in antioxidants and essential acids such as L-carnitine help improve sperm quality.
Oily fish is another product rich in omega 3 acids which bring great benefits to human reproductive health.
These nutritional contributions can also be taken by food supplements such as Andean maca or vitamin E supplements, a powerful antioxidant.
4-2 Assisted reproduction (ART)
In the case of fertility treatment to be able to achieve pregnancy and mild teratozoospermia, it is possible to perform artificial insemination (AI), if the concentration and mobility of the sperm allow it.
This is the first option to consider if the woman has no problems with fertility and the only cause of the lack of a pregnancy is teratozoospermia.
Faced with cases of moderate or severe teratospermia, it is necessary to do IVF - ICSI. It is an in vitro fertilization technique that uses the intracytoplasmic injection of sperm for the fertilization of oocytes.
If this topic interests you, you will find information here: IVF.
If you need to undergo IVF treatment to become a mother, we recommend that you use the Fertility Report. In 3 simple steps, which will allow you to know the clinics abroad that meet our rigorous quality criteria. In addition, you will receive a report with useful tips before you make clinic visits.
Finally, there is a new technique which is a variation of the previous one. It is known as IMSI and consists of amplifying the image before the micro-injection to be able to observe the sperm morphology in more detail.
The microscope used by IMSI to select the sperm has an objective that amplifies the image to such an extent that morphological abnormalities are detected.
5-Your frequently asked questions
5-1 What is the cause of teratozoospermia?
Teratozoospermia is an alteration that affects male semen and involves most of the sperm having an abnormal shape.
Due to their poor morphology, sperm cannot fertilize the oocyte and cause sterility.
The causes of teratozoospermia are as follows:
- Genetic alterations
- Chemotherapy and radiotherapy
- Semen infections and orchitis
- Testicular trauma
- Varicocele
- Fever
- Diabetes and meningitis
- Tobacco, alcohol, drugs
Bad eating habits, clothes that are too close to the body ...
Certain causes can be resolved (fever, quitting smoking, healthy habits ...), which implies that in some cases, the pathology is reversible.
5-2 Does teratozoospermia cause miscarriages?
In principle, the poor morphology of the sperm does not cause any miscarriage once the fertilization of the oocyte has taken place and the embryo has implanted. If, on the other hand, the sperm also have genetic disorders, this may be a cause of miscarriage.
5-3 How to improve the amorphous sperm of semen?
If the pathology of teratospermia is not specific, the man should follow some indications to modify his lifestyle, which could negatively influence his reproductive state. Some men who stop smoking or alcohol consumption and change their diet may see an improvement in their sperm quality after 3 months.
5-4 Can leukospermia cause teratospermia and male infertility
Leukospermia, also known as leukocytospermia, is the appearance of leukocytes in semen, with a concentration level greater than 1 million per milliliter. The cause of this seminal pathology is an infection of the male reproductive tract which must be treated with antibiotics as it can affect spermatogenesis and cause oligospermia or teratozoospermia.
You can find the information in our article: Leukocytes in semen.
We deliver all over the world.
For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number
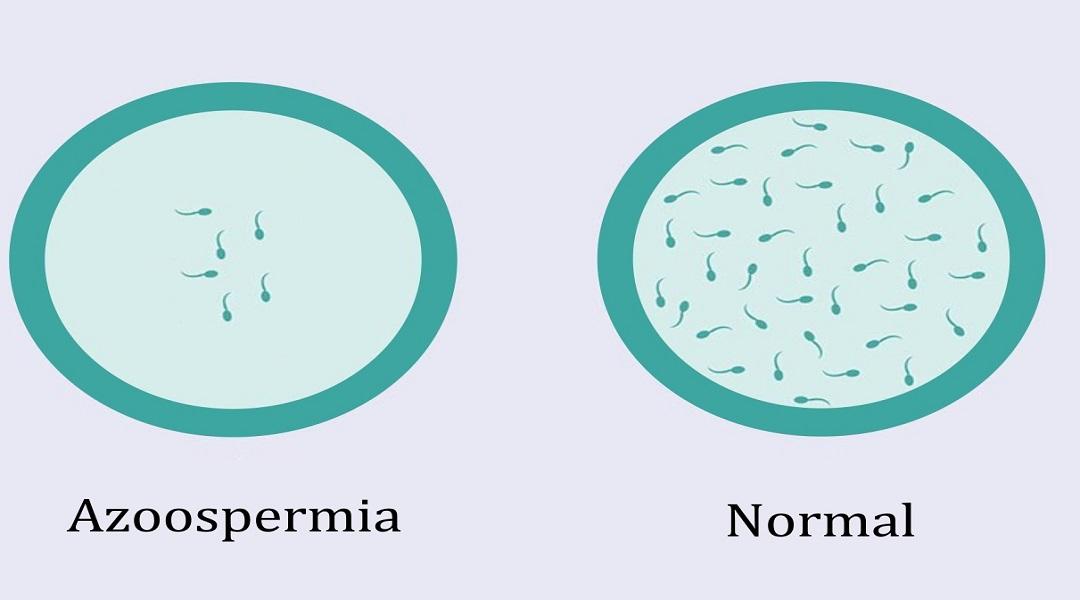
AZOOSPERMIA CAUSES: natural treatment
What is Azoospermia?
The azoospermia is a sperm abnormality characterized by the total absence of sperm in the ejaculate. It obviously leads to infertility in men, because in the absence of sperm there can be no fertilization. However, Dawasanté experts provide you with a natural herbal treatment to improve the quality and quantity of your sperm. Click here or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.

Azoospermia affects less than 1% of men in the general population or 5 to 15% of infertile men (1).
The causes
Depending on the cause, there are two types of azoospermia:
Secretory azoospermia (or NOA, for non-obstructive azoospermia)
Spermatogenesis is impaired or absent and the testes do not produce sperm. The cause of this spermatogenesis defect can be:
- hormonal, with hypogonadism (absence or abnormality in the secretion of sex hormones) which may be congenital (Kallmann-Morsier syndrome for example) or acquired, due in particular to pituitary tumors which alter the functioning of the hypothalamic-pituitary axis or after a treatment (eg chemotherapy);
- genetics: Klinefelter syndrome (presence of an extra X chromosome), which affects 1 in 1,200 men (2), structural abnormality of chromosomes, (microdeletion, i.e. loss of a fragment, of the Y chromosome in particular), translocation (one segment of the chromosome detaches and attaches to another). These chromosomal abnormalities are the cause of 5.8% of male infertility problems (3);
- bilateral cryptorchidism: the two testes have not descended into the bursa, which impairs the process of spermatogenesis;
- infection: prostatitis, orchitis.
Obstructive or excretory azoospermia (OA, obstructive azoospermia)
The testes do indeed produce sperm but they cannot be exteriorized due to a blockage of the ducts (epididymis, vas deferens or ejaculatory ducts). The cause may be of origin:
- congenital: the seminal tract has been altered from embryogenesis, resulting in an absence of the vas deferens. In men with cystic fibrosis, a mutation in the CFTR gene can cause the absence of vas deferens;
- infectious: the passages have been blocked following an infection (epididymitis, prostato-vesiculitis, prostatic utricle).
1-Pre-testicular causes
In this case, the origin of azoospermia is due to alterations at the endocrine level, that is, it is manifested by irregularities in the levels of the hormones responsible for regulating sperm production or spermatogenesis. . These are therefore cases of secretory azoospermia.
Among the main endocrine disorders that can cause azoospermia, we can find:
- Hypogonadotropic hypogonadism: this is a deficiency of the hormones released by the pituitary gland and responsible for stimulating the production of sperm in the testes. The main hormones are FSH (follicular stimulation) and LH (luteinizing). This problem can be due to genetic alterations such as Kallmann syndrome, tumors, trauma, pharmacological treatments, consumption of anabolic agents, etc.
- Hyperprolactinemia: it is the excessive increase in the hormone prolactin release. It blocks the hormone GnRH (a hormone that releases gonadotropins), whose function is to regulate the release of FSH and LH. This can be due to the consumption of antihypertensive drugs, stress, tumors, antidepressants, etc.
- Androgen insensitivity syndrome: this is mainly due to genetic mutations that cause resistance to androgens so that full virilization of the patient does not take place. Depending on the degree of severity, testosterone levels can be low, which prevents or hinders spermatogenesis, among other related consequences.
Patients who suffer from azoospermia due to this syndrome will have slightly decreased testicular volume, they will not produce sperm in the testes, and their FSH levels will generally below, except in cases of androgen resistance. In this case, the LH is elevated but the FSH and testosterone concentrations are usually normal or slightly elevated.
Testicular causes
The absence of sperm is due to problems in the testis which hamper spermatogenesis and therefore lead to errors or even blockage of sperm production.
The most common testicular pathologies are:
- Varicocele: dilation of the spermatic veins.
- Cryptorchidism: no descent of the testis from the inguinal canal to the scrotal pocket.
- Orchitis: Inflammation of the testicle, usually due to infection, as is often the case with mumps.
- Genetic alterations
- Testicular torsion
- Trauma
- Continuous increase in testicular temperature
The type of azoospermia from which these patients suffer is also secretory, but the clinical picture is different from the previous one: they have a lower testicular volume (due to non-production of sperm) but the FSH levels are high.
FSH, which is responsible for stimulating the testes to produce sperm, increases. This is why the testes do not respond to their stimulus, the body sends more FSH for the testes to function.
Post-testicular causes
When the cause of azoospermia is post-testicular, it is obstructive azoospermia. In this case, the testes are able to produce sperm properly, but there is a problem in the seminal ducts (vas deferens, epididymis or urethra) responsible for transporting sperm in an ejaculation.
Among these problems, we can highlight:
- Absence of vas deferens: this is a congenital pathology which, if it affects bilaterally, prevents sperm from coming out during ejaculate. This happens, for example, in some cases of cystic fibrosis.
- Obstruction of the vas deferens, the epididymis, or the urethra: it may be involuntary (trauma, surgery or disease) or voluntary. This is called a vasectomy.
Patients have a normal testicular size and FSH hormone levels are also average. Obstructive azoospermia is the least serious compared to fertility. It allows the man to obtain a pregnancy, either naturally, by a medical intervention which makes it possible to unblock the channels, or by obtaining sperm directly from the testicle and the subsequent application of a medically assisted procreation technique.
Your frequently asked questions
Is varicocele a cause of infertility in men?
By Victoria Moliner (embryologist).
Yes, varicocele can be a cause of male infertility. This pathology can manifest itself in different degrees of affection, so its harmful effect on male fertility (which mainly causes seminal and hormonal changes) can also be from mild to severe.
Is hormonal azoospermia always secretory?
By Andrea Rodrigo (embryologist).
Yes, when the lack of sperm is caused by hormonal problems, it is secretory azoospermia because of the lack of regulation by hormones prevents or complicates spermatogenesis.
Can cycling be the cause of my testicular factor azoospermia?
By Andrea Rodrigo (embryologist).
Continued use of the bicycle does not necessarily cause azoospermia, provided that the correct position is taken on the bicycle and, in some cases, certain testicular protection systems are used.
Routine improper use of the bicycle can increase the temperature of the scrotal region and thus prevent the proper production of sperm, which can reduce the quality of sperm.
As an added note, it is important to note that excessive exercise can affect sperm production in addition to other bodily functions.
Is azoospermia reversible?
By Andrea Rodrigo (embryologist).
It is possible that azoospermia is transient or punctual and, therefore, we can speak of reversible azoospermia. This means that, although it is unusual, a man may have a certain period of azoospermia, for example, due to stress or some other situation, and after this period recover the production of sperm and, with it, the presence of these in the ejaculate.
Read more
Why is there an absence of sperm in the spermogram?
By Zaira Salvador (embryologist).
When a man gets zero sperm as a result of his semen analysis, he may have azoospermia. First of all, this diagnosis should always be confirmed by a second spermogram, in case an error may have occurred while handling the first sample.
If azoospermia is confirmed, there are several causes of this seminal alteration, from blockage of the seminal ducts to problems with sperm production. More human testing should be done to find a more complete diagnosis.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
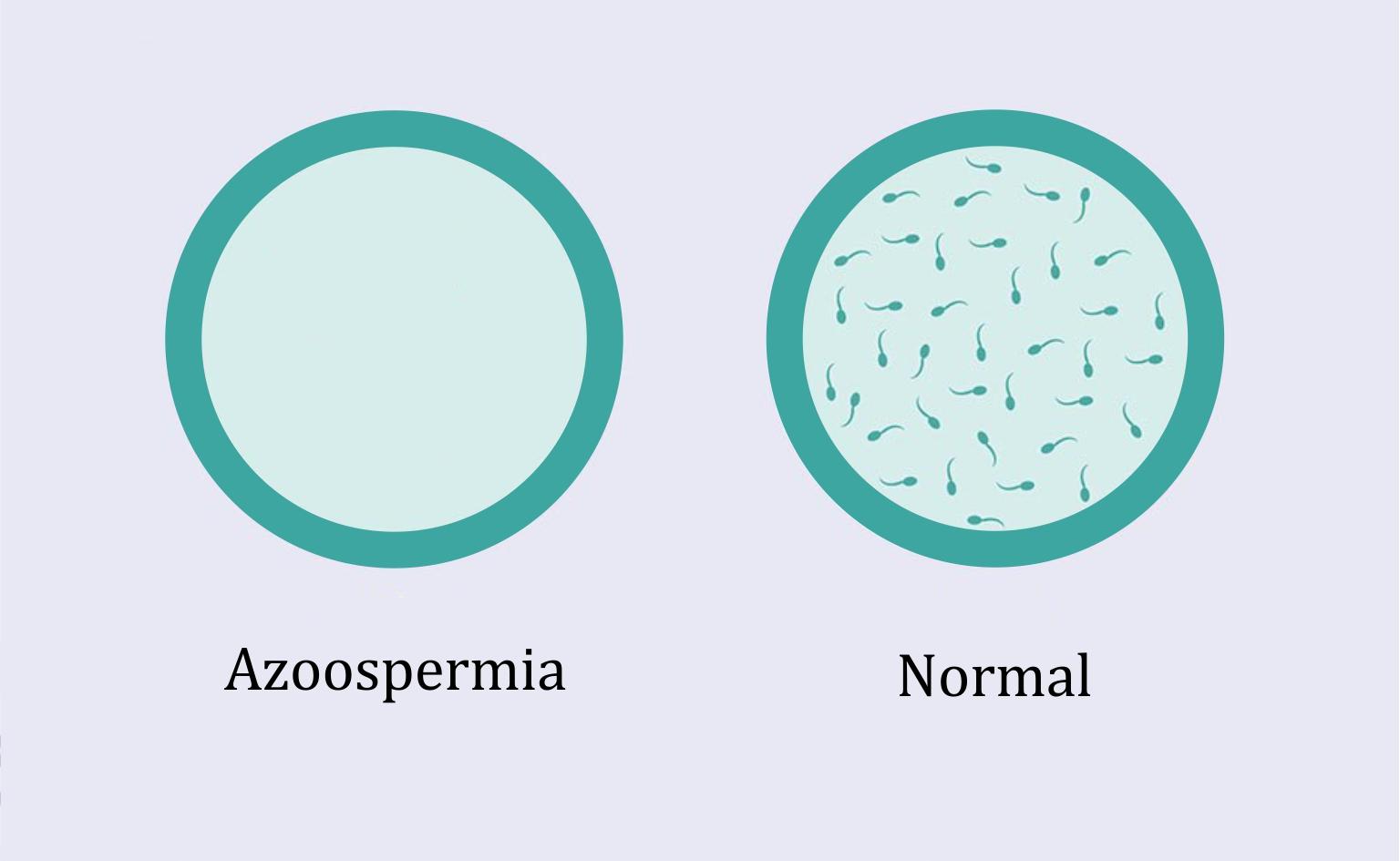
AZOOSPERMIA AND PREGNANCY: Natural treatment
Natural pregnancy in a woman whose partner has secretory or obstructive azoospermia is not possible. However, when the treatments applied do not solve the problem, Dawasanté experts offer you a natural herbal treatment to cure your azoospermia and allow your partner to quickly get pregnant.
Click here or on the image below to discover this natural treatment .
To discover our natural solution to treat azoospermia click here!
Contact our experts, tel / WhatsApp: +22990312738
1: Aspiration of sperm
In men with obstructive azoospermia , no sperm is seen in the ejaculate, but sperm is produced in the testis.
One option is to extract the sperm directly from the testis or epididymis. In this way, it is possible to obtain sperm, but in low quantity and of poor quality in relation to mobility and morphology.
For this reason, in the event of obtaining sperm by aspiration, it will be necessary to resort to the technique of ICSI (intracytoplasmic sperm micro-injection). ICSI is the ideal in vitro fertilization technique because only one sperm is needed for each egg to be fertilized. In addition, in this process, it is the specialist himself who introduces the sperm into the egg.
There are several procedures for extracting sperm, and their names come from the acronyms in English:
1.1: MESA
Corresponds to the term: microsurgical epididymal sperm aspiration , i.e., microsurgical aspiration of epididymal sperm. It is used in patients with obstruction of the genital tract. This involves making a small incision in the epididymis and extracting the sperm from inside the epididymis.
It is a complicated operation and the costs are high. For this reason, although it allows to collect more sperm than with a PESA, it is not the most chosen technique.
1.1.1: PESA
It is the percutaneous aspiration of epididymal sperm ( percutaneous epididymal sperm aspiration ). This is a simpler and less invasive procedure than the previous one and does not require as many skills on the part of the doctor. It is performed under sedation, so that the patient does not feel any pain.
A needle is inserted through the skin of the scrotum to reach the epididymis. The downside is that the needle is inserted blind, and although this is unusual, it is possible that no sperm will be aspirated.
1.1.2: TESA
Its English name is: testicular sperm aspiration , and it is referred to as the aspiration of sperm from the testis. It is also performed percutaneously, just like PESA. The difference is that the aspiration is done from the testes and not from the epididymis.
This type of aspiration is usually performed when the other options (MESA and PESA) are not applicable due to changes such as absence or obstruction of the epididymis.
2: Testicular biopsy
Also known as TESE ( testicular sperm extraction ). It is performed under local anesthesia and consists of the following elements:
- The specialist opens the different testicular layers using a scalpel or a laser until it reaches the testicle, from which he will extract small pieces. About 2-3 cm of testicular layers are opened. They will then be closed with one or two stitches.
- After the biopsy is performed or at the same time as the biopsy, the tissues are analyzed under a microscope for sperm, which will then be used in the ICSI technique in the hope of pregnancy.
- Although it is indicated in patients with obstructive azoospermia , it is also applied in certain situations of secretory azoospermia. In many of these cases, although no sperm is produced in the testes, foci of spermatogenesis can be found, that is, if you search exhaustively, it is possible to find a sperm.
- In any case, the possibility of achieving pregnancy by applying ICSI with the few sperm found after testicular biopsy of patients with secretory azoospermia is low.
3: Sperm donation
The above procedures may be effective for obstructive azoospermia , but they are not usually applied to secretory azoospermia. In patients with this alteration, where no treatment is able to reverse spermatogenesis, it is recommended to resort to sperm donation .
This is artificial insemination or in vitro fertilization with sperm donated by a healthy young man . This donor is subjected to a series of physical and psychological examinations to verify his good state of health and to confirm the safety of the use of his sperm.
The choice of one or the other reproductive technique will depend on certain qualities of the woman such as her age, the patency of the fallopian tubes, etc.
This is an alternative with a high probability of success . However, it has a major drawback: humans give up transmitting their genetic heritage. This means that the children born will not be the biological children of their father, since they will inherit the traits of the donor who gave the sperm.
4: Your frequently asked questions
If my husband has total azoospermia, should we consider donating sperm as the only option so that I can get pregnant?
If as total azoospermia you hear irreparable secretory azoospermia, yes, sperm donation is the best option for you to achieve pregnancy.
In severe cases of secretory azoospermia, it is very difficult to obtain viable sperm with fertilizing ability, so it is necessary to resort to sperm donation.
After 11 years of vasectomy, will I be able to have children if I have a testicular biopsy?
A testicular biopsy is used to obtain sperm directly from the testis, which is the place of production. However, after so long a time of voluntary obstruction, that is, after preventing the produced sperm from coming out, it is possible that the organism itself has reduced production. However, since only one sperm per egg is needed for ICSI treatment, you may be able to achieve pregnancy in your partner from the sperm found during the biopsy.
In any case, you should be aware that it is quite possible that no viable sperm will be found after the biopsy.
Pregnancy was detected by measuring serum HCG on two independent occasions, at least 15 days after the embryo replacement. Clinical pregnancy was determined by observing a gestational sac with a fetal heartbeat on a transvaginal ultrasound at 6–7 weeks gestation. The clinical embryo implantation rate was defined as the number of gestational sacs seen during ultrasound screening at 6-7 weeks gestation divided by the number of embryos transferred.
To discover our natural solution to treat azoospermia click here!
Contact our experts, tel / WhatsApp: +22990312738
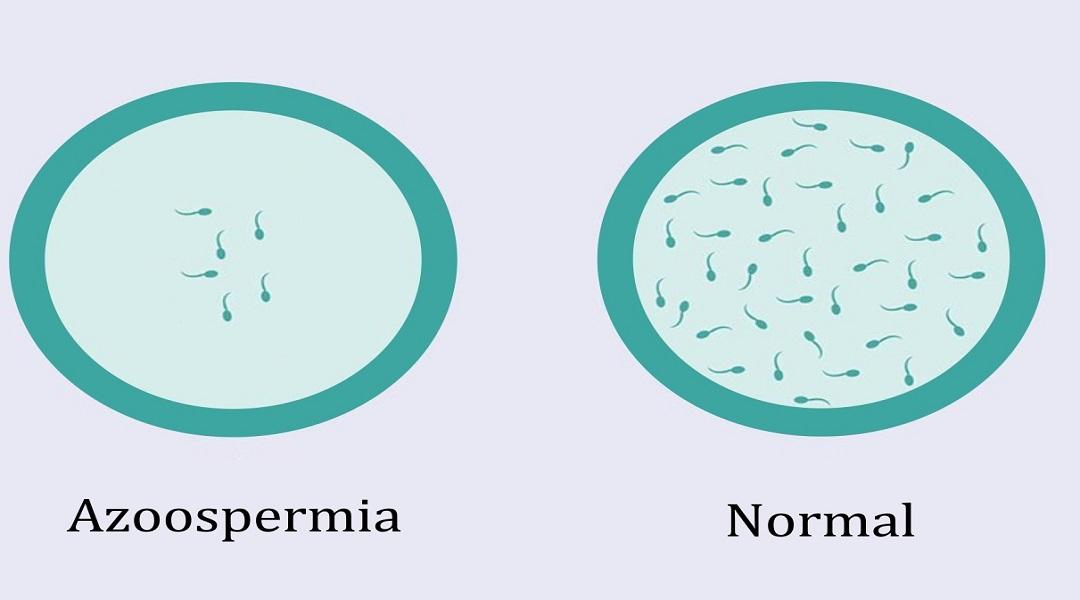
NONOBSTRUCTIVE AZOOSPERMIA: Natural treatment
Azoospermia is a total absence of sperm in the ejaculate. Depending on the cause, we distinguish two forms of azoospermia: obstructive and secretory. The prognosis for achieving pregnancy is different in each case. However, Dawasanté experts provide you with a natural treatment to boost your fertility by improving your sperm, allowing you to conceive quickly. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
1: Azoospermia: definition and diagnosis
In order to study male fertility, the most common test is a spermogram. It consists of collecting a sample of ejaculate and examining it in the laboratory to check, among other things, the concentration and mobility of sperm.
Once the result is obtained, we compare the reference rates of the World Health Organization (WHO) to carry out the diagnosis:
zero sperm in the ejaculate.
less than 100,000 sperm / ml.
less than 15 million / ml.
- Normozoospermia
no seminal parameters are altered.
Therefore, azoospermia can be defined as the absence of sperm in the ejaculate. It is considered to be responsible for between 3 and 10% of cases of male infertility.
Azoospermia is imperceptible to humans, so it is necessary to take a spermogram to diagnose it.
It is also helpful to determine FSH hormone levels. This is produced by the brain and is responsible for spermatogenesis (formation of sperm) in the testes. If the FSH levels are high, it can be inferred that the mother cells of the sperm are reduced or even absent.
You can also analyze the concentration of testosterone and fructose to get a more accurate diagnosis.
Causes
The absence of sperm in the ejaculate is mainly due to two causes:
- Secretory or non-obstructive azoospermia
the testes are not able to produce sperm.
- Azoospermia obstructive
sperm are produced, but cannot be expelled during ejaculate due to obstruction of the vas deferens.
To determine the type of azoospermia, it is necessary to perform a testicular biopsy, which consists of obtaining a small fragment of each testicle and analyzing the presence or absence of sperm. In this way, it will be easy to distinguish an obstructive azoospermia from a secretory.
Through hormonal analysis, the type of azoospermia can be determined, because if there are disturbances in the levels of hormones involved in spermatogenesis , it is secretory azoospermia. However, this method is not as reliable as a biopsy to find out if there are sperm available for ART treatment.
1: Secretory azoospermia
The azoospermia secretory or non-obstructive is the most severe and frequent and assumes 70% of cases of azoospemie. It can be congenital (from birth) or acquired (by disease or toxic treatment). Its most common causes are:
- Abnormalities of testicular descent.
- Exposure to toxic substances: drugs, radiotherapy and chemotherapy.
- Genetics: Gene disorders related to spermatogeneses, such as mutations or deletions.
- Hormonal disorders, such as hypogonadotropic hypogonadism (deficiency of hormones released by the pituitary gland and responsible for stimulating sperm production in the testes).
- Testicular problems: mumps, trauma, inflammation and sever varicocele.
The recovery of sperm from secretory azoospermia is complex, as spermatogenesis is strongly affected. Despite this, pregnancy is possible.
Some patients with this pathology have presented slight foci of spermatogenesis in the testes. To do this, doctors do multiple small testicular biopsies to find sperm.
If sperm are indeed found, the sample is frozen and is then used in an intracytoplasmatic sperm injection (ICSI).
Depending on the cause of the azoospermia, in some cases, it is possible to restore spermatogenesis by hormonal treatments and thus achieve pregnancy.
In cases where it is not possible to collect sperm, it is necessary to use donor sperm to become parents.
2 :Azoospermie obstructive
Obstructive azoospermia is caused by a problem with the ducts that carry sperm from the testes to the urethra, where ejaculate occurs. Here are the most common causes:
- Absence of vas deferens (either from birth or after surgery).
- Inflammation or trauma to the testis, epiydima, vas deferens or prostate.
In patients with this type of disorder, it is easier to obtain sperm. In some cases, this azoospermia can be reversible and thanks to several techniques of micro-surgery, the obstruction can sometimes be resolved or the ducts united so that the sperm can reach the spermatic fluid.
Otherwise, the sperm are obtained directly from the testes by testicular biopsy and are used in assisted reproduction therapy (ICSI). A single biopsy is normally sufficient, as spermatogenesis is produced normally.
Azoospermia and varicocele
The relationship between azoospermia and varicocele is relatively common: 5% of varicocele cases turn into azoospermia. However, for this to happen, the varicocele must be severe.
Varicocele is a dilation of the veins that form the spermatic cord and directly affects spermatogenesis, which is the production of sperm.
In secretory azoosperm patients who have corrected their varicocele by surgery (surgical treatment of varicocele ), approximately 50% of the testicular tissue and 55% of the sperm mobility will be recovered.
Azoospermia following vasectomy
Vasectomy is a method of male sterilization that results in the absence of sperm in the ejaculate. The goal is to intentionally induce obstructive azoospermia by severing the vas deferens, thus preventing the passage of sperm from the testis to the urethra.
As the vas deferens are blocked, the sperm will be stored in the epididymis and, over time, will be reabsorbed by the body itself.
Vasectomy does not affect sperm production, although it is true that over time the body can decrease sperm production or it can be altered slightly.
Your frequently asked questions
No. Azoospermia is the absence of sperm in the ejaculate, but the man has no problems ejaculating. In the case of aspermia, the problem is the lack of ejaculation, it does not refer to the sperm.
What are the symptoms of azoospermia?
By Andrea Rodrigo (embryologist).
Azoospermia does not lead to symptoms that are visible in everyday life such as pain, discomfort, swelling, etc. Therefore, the safe way to diagnose it is not based on the symptoms, but only on the result of the spermogram.
Secretory azoospermia is more serious. It prevents the production of sperm and, therefore, it is not possible to have biological children even by applying assisted reproduction techniques. As we mentioned, the only option for getting pregnant if you are suffering from this type of azoospermia is sperm donation.
Can I use artificial insemination in the case of azoospermia?
No. To achieve pregnancy by artificial insemination , it is necessary to have a good sperm concentration and that patients suffering from azoospermia do not have any sperm in the ejaculate.
Can you be naturally pregnant with secretory azoospermia?
The only way to achieve a natural pregnancy with secretory azoospermia is through hormonal treatment, as it restores spermatogenesis. However, in many cases it is difficult for this to happen, as it all depends on the cause of azoospermia.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
AZOOSPERMIA NATURAL TREATMENT: the experts at Dawasanté
What is azoospermia?
The azoospermia is a lack of sperm in the semen. If, after a year of unprotected sex, no pregnancy has occurred, it means that the man, woman, or both may have a fertility problem. In 40% of infertile couples, the man has a fertility problem. However, Dawasanté experts provide you with a natural herbal treatment to improve the quality of your sperm and allow you to conceive quickly.
Click here or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
How common is azoospermia?
About 1% of all men and 10% to 15% of infertile men have azoospermia.
Treatment
Here we are going to offer you a mixture of African plants, roots and bark that will help you heal your azoospermia. Our blend of plants and roots has already enabled many men around the world to heal from infertility and experience the joy of being a father. What allows us to have excellent results is that we produce all these plants and roots ourselves and that we select only the best plants so that they retain all their therapeutic and medicinal virtues. They are the best roots and plants against azoospermia.
Here are five plants and roots that will help you cure azoospermia:
1. Saw palmetto

Saw palmetto helps boost libido by stopping the breakdown of testosterone in the body. In men, sperm production is guided by testosterone. Too little testosterone results in a low sperm count. Likewise, too little testosterone reduces a woman's egg production. Saw palmetto can therefore increase male and female fertility by altering the balance of free testosterone in the body.
2. Ashwagandha

Ashwagandha is traditionally used to improve sexual health. It supports the endocrine system and promotes its better functioning. It also strengthens the hormonal balance in the body. It stimulates libido and improves sperm count in men. It improves stamina and also improves sexual performance.
3. Saw Palmetto

Saw Palmetto nourishes the entire endocrine system, which can help improve overall reproductive function in humans. Men with high stress, poor immune function, poor lifestyle and eating habits are found to respond well to this plant. This plant is classified as an adaptogen and is antiandrogenic, anti-inflammatory, softening, urinary antiseptic and immuno-amphoteric. Saw Palmetto is also a reproductive amphoteric. What does this mean though? It just means that it normalizes reproductive function.
Saw Palmetto nourishes the body deeply when taken regularly for many months. Constant use of this herb is beneficial in improving the quality and quantity of sperm.
4. Ginseng

Ginseng is often referred to as the king of all herbs and is proven to be the panacea for improving overall well-being. Ginseng is also an aphrodisiac and is used to treat sexual dysfunction and to improve sexual behavior in traditional Chinese medical practices. Data from animal studies have shown a positive correlation between ginseng's performance, libido and copulation, and these effects have been confirmed in case-control studies in humans. In addition, ginseng improves the quality of sperm and their number. We highly recommend it.
5. Maca

Maca has the ability to improve female fertility, which is why it is getting a lot of attention. It balances female hormones to improve fertility. However, this herb also has the ability to boost male fertility. This plant effectively improves the quality of sperm (poor sperm quality is a cause of male infertility). According to a study, men who consume maca regularly have more mobile sperm, more sperm and more semen per ejaculation.
The natural treatment that we offer to cure azoospermia consists mainly of natural herbal teas. The herbal tea is composed of plants and roots whose active ingredients are able to restore the male hormonal balance, by increasing the level of testosterone, the number and the mobility of your sperm. It is the miracle solution to cure azoospermia.
To find out about our natural remedy to cure azoospermia, click here
Cause of azoospermia
Depending on the cause, there are two types of azoospermia:
Secretory azoospermia (or NOA, for non-obstructive azoospermia)
Spermatogenesis is impaired or absent and the testes do not produce sperm. The cause of this spermatogenesis defect can be:
- Hormonal, with hypogonadism (absence or abnormality in the secretion of sex hormones) which may be congenital (Kallmann-Morsier syndrome for example) or acquired, due in particular to pituitary tumors which impair the functioning of the hypothalamic-pituitary axis or after a treatment (eg chemotherapy);
- Genetics: Klinefelter syndrome (presence of an additional X chromosome), which affects 1 in 1,200 men, structural abnormality of the chromosomes (microdeletion, i.e. loss of a fragment, of the Y chromosome in particular), translocation (one segment of the chromosome detaches and attaches to another). These chromosomal abnormalities are the cause of 5.8% of male infertility problems;
- Bilateral cryptorchidism: the two testes have not descended into the bursae, which impairs the process of spermatogenesis;
- An infection: prostatitis, orchitis.
Obstructive or excretory azoospermia (OA, obstructive azoospermia)
The testes do indeed produce spermatozoa but they cannot be exteriorized due to a blockage of the ducts (epididymis, vas deferens or ejaculatory ducts). The cause may be of origin:
- congenital: the seminal tract has been altered from embryogenesis, resulting in an absence of the vas deferens. In men with cystic fibrosis, a mutation in the CFTR gene can cause the absence of vas deferens;
- infectious: the passages have been blocked following an infection (epididymitis, prostato-vesiculitis, prostatic utricle).
Symptoms
The main symptom of azoospermia is infertility.
Diagnostic
The diagnosis of azoospermia is made during an infertility consultation, which in men systematically includes a spermogram. This examination consists of analyzing the content of the ejaculate (semen), evaluating various parameters and comparing the results with the standards established by the WHO.
In the event of azoospermia, no sperm is found after centrifugation of the entire ejaculate. To make the diagnosis, however, it is necessary to carry out one or even two other spermograms, each 3 months apart, because spermatogenesis (cycle of sperm production) lasts about 72 days. In the absence of sperm production over 2 to 3 consecutive cycles, the diagnosis of azoospermia will be made.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
VARICOCEL AND FERTILITY: Natural treatment
VARICOCEL AND FERTILITY
Many men have dilated veins in the scrotum, which is the pouch containing the testicles. Doctors call these veins varicoceles. Many men with varicocel have no symptoms, but some may have fertility problems. Varicoceles are common and affect 10 to 15% of men. Doctors continue to debate the role of varicoceles in infertility. However, Dawasanté experts provide you with a natural herbal treatment to cure varicocele and treat your infertility. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Some research suggests that treating a varicocele may improve fertility outcomes. However, a systematic review indicates that the available evidence is weak and that doctors need to do more research.
In this article, find out if a varicocele affects fertility.
What is a varicocele?
A varicocele occurs when a bulge results from dilated veins inside the scrotum. The swelling usually looks like a magnification above the testis, without discoloration. A pampiniform plexus is a group of veins inside the scrotum. These veins help cool the blood before it goes to the testicular artery, which supplies the testes with blood.
If the testicles are too hot, they cannot produce healthy semen. The health of sperm affects fertility. It is therefore essential that the veins can cool the blood. Most people with a varicocele don't have symptoms, but some may have fertility problems. When a person has a varicocele, they may also experience swelling and tenderness in the scrotum.
Treatment
First, varicocele is not inevitable, the only way out is an operation. The use of natural plants makes it possible to cure varicocele permanently by avoiding surgical operation. The natural remedy for curing varicocele that we offer is completely herbal. It contains two elements namely: an herbal tea and an ointment. Trust us! Because it is the secret to cure varicocele without operation thanks to the plants.
Herbal tea to cure testicular varicose veins is vasculoprotective and venotonic. It is a natural remedy that cures varicocele successfully by strengthening the valves or valves located in the veins of the spermatic cords. So the veins become tonic and tenacious to facilitate the dynamic rise of blood along the veins. This to join the most important veins like the left renal vein and the inferior vena cava. The operation for varicocele is very expensive and is of little benefit. As for our remedy, it has proven its effectiveness with dozens of resolved cases. So, this is one of the best natural herbal remedies to cure varicocele and prevent operation.
Using herbal teas to cure varicocele usually gives excellent results as it helps prevent the operation. So our natural remedy is the best herbal therapy for Varicocele. The solution to curing varicocele is in plants. Being natural products based on plants and herbs, our herbal teas to treat varicocele do not cause any side effects, whether on the body or on health. Our natural remedy is the miracle solution to cure varicocele without operations or side effects. So it is the best natural remedy to cure varicocele.
To discover our natural remedy for varicocele click here
Do Varicoceles Cause Infertility?
Most men with varicoceles do not have fertility problems. Infertility rates in people with varicoceles, however, are higher than in those without. This difference may be due to the fact that varicoceles interfere with the body's ability to make and store semen.
A 2014 study found that varicoceles are sometimes, but not always, a factor in infertility.
Research on whether treating varicoceles can improve fertility is mixed.
A 2012 meta-analysis of previous studies found that treating a varicocele could improve fertility, especially if the cause of a couple's infertility is unknown. However, the researchers stress that the evidence is weak and therefore more research is needed.
The main concern with varicoceles is that the bulging of the veins can damage the sperm and reduce their number. In individuals with an average sperm count, a varicocele is unlikely to cause infertility.
When a couple cannot conceive, it is essential to do a variety of tests, including a sperm count, and not to assume that varicocele is necessarily the only cause.
Causes and risk factors
A varicocele occurs when the veins in the scrotum grow larger. Each vein has a valve that prevents blood from flowing back, but sometimes the valve fails. This causes blood to flow back, damaging the vein and causing swelling. Doctors do not fully understand what causes valve failure and varicocele. They are common and usually do not mean that a person has an underlying health problem.
Studies have proven that smoking can be a risk factor for varicocele because it damages a person's blood vessels. The same study found no link between alcohol or occupation and varicoceles.
Rarely, growth in the stomach can put pressure on the veins, causing a varicocele. This problem is more common in men over 45.
In many people, a varicocele has no apparent cause.
Diagnostic
Most men with varicoceles don't notice anything unusual, although some people report an occasional thrill or throbbing in the scrotum. Many affected people only find out that they have a varicocele after having had problems with infertility. A doctor can often diagnose a varicocele during a physical exam by examining the scrotum and looking for any unusual lumps and blood vessels.
If a doctor suspects a varicocele, they may order an ultrasound. This is a painless imaging test that allows the doctor to see the veins inside the scrotum.
If the person has fertility problems, the doctor may also order a semen analysis to check the quality of the semen.
Medical treatment
Varicoceles that do not cause symptoms do not require treatment. A varicocele may need treatment when:
- · A man has varicocele and low sperm count or other semen problems.
- · Varicocele causes pain or swelling.
- · A couple has unexplained infertility and the male has a varicocele.
When people choose to undergo treatment, they have two different options:
Embolization
Embolization is a surgical procedure that temporarily cuts off the blood supply. A doctor can perform this procedure in their office under local anesthesia, which means that a person will not feel any pain in the area.
During embolization, a doctor inserts a needle into a vein usually through the groin. Sometimes they can insert a needle through the neck. The needle helps the doctor access the veins in the scrotum and block the varicocele. A person may experience pain and tenderness after the procedure, but the recovery time is short and the person can immediately resume normal activities.
Surgery
A doctor can surgically remove a varicocele by blocking blood flow to the damaged vein. This operation is called a varicocelectomy.
A person will undergo general anesthesia before the varicocelectomy in order to be asleep and unable to feel any pain during the procedure. A person may experience pain and tenderness for several days.
Surgery is more effective is embolization with a failure rate of less than 5%. Laparoscopic surgery uses a smaller incision than open surgery and requires less recovery time but also requires a very skilled surgeon. Open surgery uses a wider cut in the scrotum.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
ASTHENOSPERMIA: NATURAL TREATMENT
What is asthenospermia?
The asthenospermia or asthenozoospermia is a sperm abnormality characterized by insufficient mobility of spermatozoa. It can alter a man's fertility and reduce the couple's chances of pregnancy because if they are not sufficiently mobile, the sperm cannot migrate from the vagina to the tube to fertilize the oocyte. However, Dawasanté experts provide you with a natural plant-based treatment to permanently cure asthenospermia.
Click here or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Asthenospermia can be isolated or associated with other sperm abnormalities. In the case of OATS, or oligo-astheno-teratozoospermia, it is associated with oligospermia (sperm concentration below normal values) and teratozoospermia (too high a proportion of abnormally shaped sperm). The impact on human fertility will be even greater.
Treatment
Here we are going to offer you a mixture of African plants, roots and barks that will help you heal your asthenospermia. Our blend of plants and roots has already enabled many men around the world to recover from their asthenospermia and experience the joy of being a father. What allows us to have excellent results is that we produce all these plants and roots ourselves and that we select only the best plants so that they retain all their therapeutic and medicinal virtues. They are the best roots and plants against asthenospermia.
Here are five plants and roots that will help you cure asthenospermia:
1. ROOTS MALE INFERTILITY
The effects of herbal remedies for treating asthenospermia problems have been proven by studies and hundreds of years of use. Here we are going to offer you a mixture of African plants, roots and bark that will help you heal your infertility. Our blend of plants and roots has already enabled many men around the world to heal from infertility and experience the joy of being a father. What allows us to have excellent results is that we produce all these plants and roots ourselves and that we select only the best plants so that they retain all their therapeutic and medicinal virtues.
2.The fruit of the Tribulus (Tribulus Terrestris)

Tribulus is expected to be very effective in improving sperm count, motility, and morphology when combined with changes in diet and exercise.
The main part of Tribulus that contributes to fertility in men is a constituent called protodioscin. This constituent improves the levels of DHEA in the male body. In men with erectile dysfunction, their DHEA levels have been found to below. Some studies have shown that protodioscin, extracted from Tribulus, increases the natural levels of DHEA necessary for a proper erection. Protodioscin is also the main constituent responsible for the aphrodisiac qualities of Tribulus. The increase in sexual desire while using this herb has been reported by both men and women.
A study by dawabio experts showed a 61% increase in conception in couples with anti-sperm antibodies (the immune system attacking sperm) taking Tribulus. The average duration of conception for a couple after treatment was 5 months. Tribulus is one of the best herbs for improving male fertility. Tribulus supports the production of LH and testosterone in men.
It also helps increase sperm count, motility, and health. It reduces the effects of anti-sperm antibodies.
3. Ginseng
Ginseng is often referred to as the king of all herbs and is proven to be the panacea for improving overall well-being. Ginseng is also an aphrodisiac and is used to treat sexual dysfunction and to improve sexual behavior in traditional Chinese medical practices. Data from animal studies have shown a positive correlation between ginseng's performance, libido and copulation, and these effects have been confirmed in case-control studies in humans. In addition, ginseng improves the quality of sperm and their number. We highly recommend it.
4. Maca

Maca has the ability to improve female fertility, which is why it is getting a lot of attention. It balances female hormones to improve fertility. However, this herb also has the ability to boost male fertility. This plant effectively improves the quality of sperm (the poor quality of sperm is a cause of male infertility). According to a study, men who consume maca regularly have more mobile sperm, more semen and more semen per ejaculation.
5. Ashwagandha

Ashwagandha is traditionally used to improve sexual health. It supports the endocrine system and promotes its better functioning. It also strengthens the hormonal balance in the body. It stimulates libido and improves sperm count in men. It improves stamina and also improves sexual performance.
The natural treatment that we offer to cure asthenospermia consists essentially of natural herbal teas. The herbal tea is composed of plants and roots whose active ingredients can restore the male hormonal balance, by increasing the level of testosterone, the number and the mobility of your sperm. It is the miracle solution to cure asthenospermia.
To discover our natural remedy to cure asthenospermia, click here
Causes of asthenospermia
As with all semen abnormalities, the causes of asthenospermia can be numerous:
- a morphological anomaly of the male gametes,
- an infection,
- presence of anti-sperm antibodies
- medication,
- a varicocele,
- a dietary deficiency,
- a renal failure,
- liver failure
- chemotherapy,
- exposure to radiation,
- excessive alcohol consumption,
- a deficiency in calcium, vitamin D or trace element ...
Symptoms
Asthenospermia does not show any symptoms other than difficulty conceiving.
Diagnostic
A semen analysis, or spermogram, is used to assess the mobility of the sperm. It should be remembered that only mobile gametes can fertilize the egg. Many medical analysis laboratories rely on the classification issued by the World Health Organization to classify spermatozoa:
- Level A (or I): progressive rapid sperm advance quickly and in a straight line,
- Level B (or II): the slow progressive spermatozoa advance slowly or in a curved line,
- Level C (or III): non-progressive spermatozoa move but do not progress,
- Level D (or IV): the sperm are immobile.
To be qualified as normal, the spermogram must show a minimum of 40% of motile sperm and 32% of sperm showing progressive mobility.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
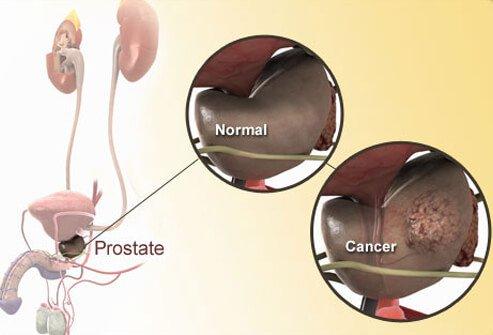
PROSTATE CANCER AND FERTILITY: Natural treatment
PROSTATE CANCER AND FERTILITY: Natural Treatment
The prostate cancer is common cancer affecting the prostate, a gland in the male reproductive system. Cancer develops from the tissues of the prostate when cells there mutate and multiply out of control. These can then spread (metastasize) by migrating from the prostate to other parts of the body, especially the bones and lymph nodes in the pelvis.
Men with fertility problems are statistically more likely to develop prostate cancer than others, according to a Swedish study, which strengthens the hypothesis that these two health problems could have common causes. However, Dawasanté experts have a natural herbal treatment available to treat prostate cancer and improve fertility. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Herbal remedy for prostate cancer
Here we offer you a mixture of seeds, roots, and bark from Africa that can prevent and cure cancer (breast cancer, liver cancer, prostate cancer, tyroid cancer, cervical cancer. uterus, kidney cancer) and cardiovascular disease. These plants are very little known to scientists and they have extraordinary qualities against cancer. Their use against cancer is much more effective than chemotherapy.
Rich in antioxidants and trace elements, our plants for curing cancer delay the development of cancer cells thanks to a pigment it contains, phycocyanin. The root extract very selectively kills cells. Healthy cells are not killed, while cancer cells are. Our natural treatment kills cancer in an all-natural way without nausea, weight loss, or hair loss, while protecting the immune system.
No one can tell you that these herbs definitely cure any type of cancer, that would be lying. But thanks to these plants, you can improve the quality of life of patients by cancer, a fact verified. Best of all, they can even relieve some symptoms of cancer! How does it work?
These African plants are powerful antimicrobials and antifungals. They make it possible to stop metastatic processes by reducing the size of the tumors. This will significantly slow the advance of cancer.
However, even if these roots are very effective, we recommend that you accompany them with conventional treatments. We are definitely not asking you to give up your cancer treatment. Indeed, one should never completely leave aside a medical treatment to start a therapy resulting from the natural African herbal medicine. You will put your health and your life in danger. Our natural anti-cancer treatment should be combined with conventional therapy.
Sexuality and fertility
Prostate cancers and their treatments influence sexuality and fertility. Dedicated support for sexuality is in place, as well as measures to prevent infertility if you are considering a fatherhood project.
There is no harm or risk of having sex during treatment. In the case of brachytherapy treatment with permanent implants (iodine 125 grains), your doctor will give you the recommendations for protecting sexual intercourse. In addition, in the event of radiotherapy, chemotherapy, or hormone therapy, during treatments and six months after the end of treatments, it is necessary to use a suitable means of contraception (for you or your partner) in order to avoid any risk of fertilization from an altered sperm.
SEXUALITY DURING AND AFTER CANCER
After diagnosis, stress, worry, and fatigue often lead to decreased desire. But sexuality is not limited to sexual relations, it encompasses affection, tenderness, speech ... and over time, desire often returns little by little.
Physical difficulties, in particular erectile dysfunction or urinary continence, may appear. They are variable and depend on the erectile and urinary problems that you may have had before the treatments, as well as the treatments received. Erectile dysfunction can appear immediately after treatment or more gradually, in the months or even years that follow. Do not hesitate to talk to your medical team and ask all your questions. Doctors and health professionals are used to this type of request and will direct you to the solutions adapted to your situation and your needs.
If it is difficult to get an erection sufficient to have sex, you may be offered different treatments. Some are to be taken by mouth (5-phosphodiesterase inhibitors); others are injected into the cavernous bodies at the base of the penis (we speak of intracavernous injections), still others are presented as a gel to be inserted into the urinary meatus. A vacuum pump can also be a way to get erections.
FERTILITY
Cancer treatments most often lead to loss of fertility. If you are considering fatherhood, talk to your doctor before starting treatment in order to implement fertility preservation measures.
Freezing (cryopreserving) sperm is the most effective way to preserve male fertility before cancer treatment. The most common way to collect the semen sample is through masturbation. Men who cannot ejaculate can have vibratory or electrical stimulation to help them do so. The semen will stay frozen or stored until you need it. Freezing, even for many years, does not damage the sperm.
According to the Prostate Cancer Treatment Guide, hormone therapy generally has the lowest risk of fertility loss. If fertility problems exist, they will usually only be apparent during treatment. Then the ability to produce sperm should return to normal. For those undergoing radiation therapy, the risk of fertility loss is highly dependent on the dose of radiation received. If fertility can return to normal, it may take up to five years. What is promising, however, is that more precise dosage planning has started to reduce this risk of infertility, the PCF noted.
Infertility
Infertility or the inability to conceive is a potential side effect of prostatectomy or radiation therapy.
The surgery involves removing the prostate as well as the seminal vesicles that produce semen. Men who have had a radical prostatectomy can still reach orgasm but without ejaculation.
Radiation therapy can affect the transport of semen. Men who want to father a child should consider freezing their sperm.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.

ADENOMYOSIS AND INFERTILITY: Natural treatment
The adenomyosis uterus is often defined as the internal endometriosis in the uterus. It corresponds to the infiltration of the cells of the endometrium (uterine lining) into the muscle of the uterine wall (myometrium), which results in the thickening of the myometrium. However, Dawasanté experts provide you with a natural treatment based on medicinal plants to permanently cure adenomyosis.

Adenomyosis can be diffuse or focal (one or a few foci within the myometrium), superficial or deep. Diffuse adenomyosis is the most common. Namely: there is a link between endometriosis and adenomyosis but a woman can have endometriosis without adenomyosis or have adenomyosis without endometriosis.
This uterine pathology can affect fertility.
To discover our natural remedy for adenomyosis, click here
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
HOW ADENOMYOSIS RELATES TO INFERTILE
Adenomyosis is the presence of ectopic endometrial mucosa in the uterine muscle. The clinical symptomatology of adenomyosis is dominated by menometrorrhagia with pelvic pain and infertility. The diagnosis of adenomyosis is accessible on ultrasound, it will be confirmed or confirmed by MRI. Adenomyosis can be isolated or associated with endometriosis. The role of adenomyosis in female infertility is starting to be well-defined (chronic inflammation with ovulation disorder, contractility abnormalities and difficulty of implantation). The therapeutic modalities are medical, surgical and may involve embolization of the uterine arteries.
Always for in-depth the relationship between adenomyosis and infertility :
- Ballester et al. evaluated the cumulative rate of pregnancy after surgical treatment of colorectal endometriosis (68.6%) and found, in women with adenomyosis a rate of 19% against 82.4% in women without adenomyosis (OR: 0.34 with a 95% CI % (0.12-0.99)).
- -Kunz et al. conducted in 2005 a study in 227 infertile women, 160 with endometriosis and 67 without. The prevalence of adenomyosis is 79% in women with endometriosis, rising to 90% in those with a fertile partner (mobility of type “a” sperm greater than 20%), a significant difference (p <0.01). This can be explained by an alteration in the uterine transport of sperm due to changes in the junction area.
- -Kissler et al. studied these disturbances in uterotubal transport in hysterosalpingography. There was a correlation with the increase in the junction area and a difference between focused and diffuse adenomyosis. In the group of women with diffuse adenomyosis, 10% bilateral and 15% contralateral transport was observed. In focused adenomyosis, the rates were 40% and 35%, respectively.
These results are therefore arguments for IVF management of women with adenomyosis. Adenomyosis is responsible for a 30% decrease in the chances of pregnancy in AMP as well as an increase in the rate of spontaneous miscarriages. In infertile women with adenomyosis, there is a decrease in the implantation rate. In the case of gastrointestinal endometriosis surgery, the impact of adenomyosis is even greater, as mentioned above. Indeed, a review of the literature evaluating pregnancy rates after surgery for digestive endometriosis, reports a 68% reduction in the chances of pregnancy in adenomyosis. However, it seems that adenomyosis has an impact on embryo implantation rather than fertilization. However, these data should be qualified with the prospective study by Benaglia, published in 2014, which showed that asymptomatic adenomyosis did not affect the rates of implantation and pregnancy in IVF.
One of the most important parameters for implantation is the junction zone, the thickness of which increases between 20 and 50 years and decreases under treatment with GnRH agonists.
Protocols using a GnRH antagonist have a negative effect on the pregnancy rate. On the other hand, there is no significant difference in IVF / ICSI, between patients with or without adenomyosis, in the event of long protocols (more than 3 months) using a GnRH agonist. Preliminary series argues for a beneficial effect of GnRH analogues, prescribed for a period of 2 to 6 months, on the chances of pregnancy
The adenomyosis is responsible for pathophysiological disturbances decreasing the chances of pregnancy ; however, its effect during IVF / ICSI management is attenuated by the prescription of long protocols with GnRH agonists. There is also an increase in spontaneous miscarriages, probably related to a particular myometrial activity, according to some authors. From a therapeutic point of view, the medical treatment is disappointing (except the agonists ) and the surgical treatment must be reserved for the localized forms ( adenomyosis ). Therefore, the support in AMP should be preferred in cases of adenomyosis but remains complex. In the coming years, the SPRMs (currently under study) could provide satisfaction.
However, the high suspicion of its relation to endometriosis, a much more well-known pathology and having a close relation to infertility, has caused us to think for a long time in possible relation with the difficulty to get pregnant, and also suggested a link with worse outcomes after assisted reproduction treatment.
Currently, in view of the effects that adenomyosis produces on the uterus, it has been verified that there is a high discrepancy between what we observe and what the patient feels. That is to say that it is possible that we are in the presence of a uterus very affected or even deformed by adenomyosis and that this does not cause any symptoms in the patient or, on the contrary, that we observe slight clues and that we were dealing with a patient with severe symptoms. A uterus that is capable of producing very severe symptomatology could equally present difficulty in permitting embryonic implantation and therefore cause infertility which is difficult to resolve via infertility treatment.
Its relationship to repeated embryonic implantation defects has been suggested in much research, but cannot be confirmed due to inconsistency in diagnosing adenomyosis. What is clear is that in a patient with an implantation defect (more than 4 embryos transferred of good quality without obtaining pregnancy) the diagnosis of adenomyosis is of particular interest since a targeted and specific treatment of this pathology could improve the results of reproductive treatment.
To discover our natural remedy for adenomyosis, click here
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
NABOTH CYST AND INFERTILITY: Natural treatment
NABOTH'S CYSTS FOR INFERTILITY
The Naboth cysts are tiny cysts that form on the surface of your cervix. Your cervix connects your vagina to your uterus. It is sometimes called the cervical canal. Naboth's cysts are filled with mucus which is secreted by the cervical glands. Sometimes the small bumps are called cervical cysts, mucinous retention cysts, or epithelial cysts. Naboth's cysts are quite common. They do not pose a threat to your health and are not a sign of cervical cancer.
If you are looking for a natural treatment to fight Naboth cysts, the experts at Dawasanté have the solution for you. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
NATURAL TREATMENT
The natural treatment that we offer to cure Naboth cysts is essentially made from natural herbal teas. Herbal tea is made up of plants whose active ingredients are able to suppress the symptoms that you feel and allow you to have a total recovery. This is the solution to find a normal life.
To discover our natural remedy to cure Naboth cysts, click here
The causes
The cervix is the tissue that connects the uterus to the vagina. The cervix has two distinct parts lined up in two different types of cells:
- Glandular cells, which line the area of the cervix closest to the uterus
- · Squamous cells, which line the part of the cervix closest to the vagina
Glandular and squamous cells meet to form an area called the transformation zone. This area undergoes many changes over the course of a woman's life, especially during pregnancy and childbirth.
Cells in the transformation zone are constantly changing, making this zone very susceptible to abnormal cell growth.
A number of conditions can cause a lump on the cervix and are described in the following sections.
Cervical polyps
A cervical polyp is a bulb-shaped, non-cancerous growth that develops on the cervix. The appearance, size and color of polyps can vary widely. It is not known why cervical polyps develop, but some of the possible causes of these polyps can include:
- High estrogen levels
- Inflammation of the cervix
- Blocked blood vessels
In most cases, cervical polyps are benign, with only 1 in 1,000 being cancerous. The doctor can remove the cervical polyps in a simple procedure.
Pregnant women can develop small white bumps called Naboth's cysts. They can form when excess skin cells block the mucous glands lining the cervix. Women may not know they have a Nabothian cyst until their doctor finds one during a routine pregnancy check-up. Although Naboth's cysts usually don't cause symptoms, they can rupture and release a foul-smelling discharge or blood.
Cervical fibroids
Fibroids, or myomas, are non-cancerous tumors that usually grow in muscle tissue in the uterus. Although rare, fibroids can also grow in the cervix.
Fibroids can vary in size and some can grow large enough to cause weight gain and swelling of the lower abdomen. Fibroids are almost always benign. Cancerous fibroids are rare and occur in less than 1 in 1,000 cases.
Cervical cancer
A lump on the cervix may indicate cervical cancer. Early Stage Cervical Cancer May Not Cause Symptoms Reliable Source. Cervical cancer can affect one or both types of cells that line the cervix.
Symptoms
Naboth cysts can cause a variety of symptoms if any. They can cause the following symptoms:
- Heavy or painful periods
- Bleeding between periods
- Foul-smelling vaginal discharge
- Pressure or swelling of the lower abdomen
- Frequent need to urinate
- Pain in the lower back, pelvis or legs
- Pain during intercourse
To diagnose the underlying cause of a lump on the cervix, the doctor will collect the following information:
- Family history
- · medical background
- Current drugs
They may also perform a physical exam and other diagnostic tests:
· Ultrasound tests use sound waves to create images of structures inside the abdomen and pelvis.
· MRI scans use a strong magnetic field and radio waves to create detailed images of the tissues inside the body.
· Hysteroscopy can help diagnose conditions affecting the uterus. During the procedure, a healthcare professional will guide a thin tubular device called a hysteroscope through the vagina and uterus. The hysteroscope captures images inside the uterus and transmits them to a computer.
· Laparoscopy uses a camera attached to the end of a thin tube to examine female reproductive organs.
· Biopsies are small samples of tissue from the lining of the cervix. After removal, the doctor will send the sample to a laboratory for analysis. Biopsies can detect the presence of precancerous or cancerous cells.
Complications
Usually, fibroids do not cause serious complications. However, untreated fibroids can increase the risk of infertility and cause problems during pregnancy, such as:
- Placental ablation
- · premature delivery
- · miscarriage
Having fibroids does not increase the risk of developing cancerous fibroids. Naboth's cysts rarely cause serious complications and often go away without treatment.
However, large Naboth cysts can distort the shape of the cervix. These cysts may require excision or surgical removal.
Medical treatments
Benign growths, such as cervical polyps and Naboth's cysts, often do not require treatment.
However, even benign growths can cause problems. Cysts and polyps can grow large enough to distort the shape of the cervix and may require surgical removal or drainage.
Treatment options for bumps on the cervix may include:
Surgery
Here are examples of surgical treatments for bumps on the cervix:
· Polypectomy: this method is to remove a polyp of the cervix with forceps or a string. This procedure usually takes place in an outpatient clinic.
· Electro-coagulation ablation: This method uses the heat of an electric current to remove a cervical cyst.
· Myomectomy: During this procedure, a surgeon will remove the fibroids through a small incision in the lower abdomen.
Medication
Gonadotropin-releasing drugs (GnRH) agonists and antagonists can treat symptomatic cervical fibroids.
GnRH drugs cause the body to make less estrogen and progesterone, which effectively reduces the size of fibroids without harming fertility.
Taking over-the-counter pain relievers, such as ibuprofen and acetaminophen, may help reduce cramps and lower back pain associated with the cervical lump.
Risk factors
It is not known exactly what causes the bumps on the cervix. However, there are certain factors that can increase the risk of developing a lump on the cervix.
Risk factors for cervical lumps include:
- Taking birth control pills containing estrogen
- Having a family history of fibroids, polyps, cysts or cervical cancer
- Inflammation of the cervix due to infections such as HPV, herpes, or yeast infections
- Be overweight or obese
- Having a weakened immune system
Prevention
Maintaining a healthy weight and controlling hormone levels can help reduce the risk of developing a lump on the cervix.
However, leading a healthy lifestyle does not guarantee complete protection against conditions that can cause a lump on the cervix. Participating in routine pelvic exams and Pap smears can help detect cervical abnormalities at an early stage.
The widespread use of regular Pap smears over the past decades has resulted in a significant reduction in the rates of cervical cancer deaths and diagnoses.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.





