Reversible causes of teratozoospermia
Blog / 33 results found
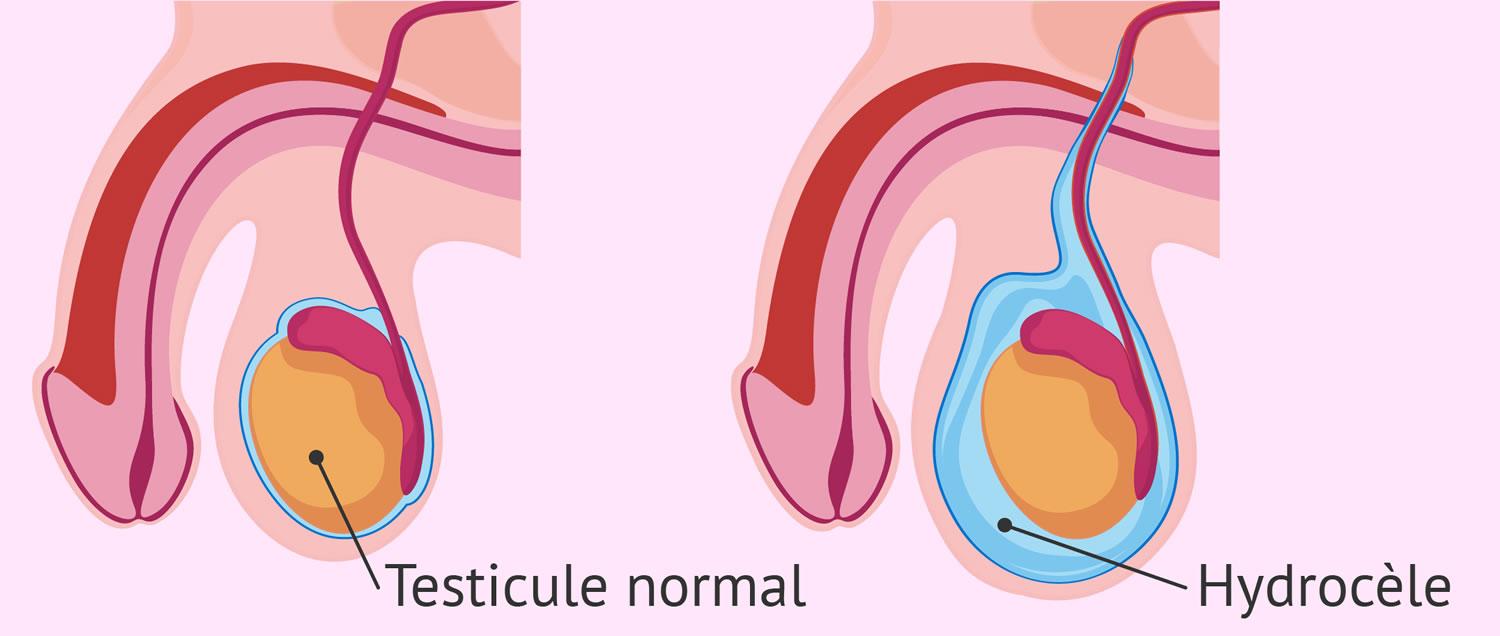
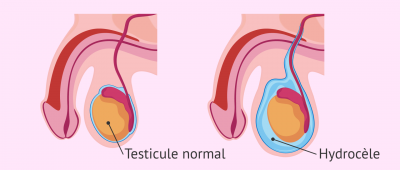
Hydrocele - Symptoms, Causes, Diagnosis and Natural Treatment
The testes are part of the male reproductive system responsible for producing sperm and testosterone. This pair of testicles hang below the penis in a skin sac called the scrotum.
Hydrocele is the buildup of fluid around the testicles, which is usually painless and harmless. However, this accumulation of fluid can cause the scrotum (testicular sac) to swell and cause discomfort. Adult males with hydrocele generally feel uncomfortable due to the increased size of the scrotum, and the weight becomes heavier as well.
A man will be more at risk of suffering from hydrocele after he reaches the age of 40. Additionally, men who suffer from infections (including sexually transmitted infections) or have a history of scrotal damage are also at risk of developing this condition. While in infants, the risk of hydrocele will increase in the case of premature birth.
Natural remedy to cure testicular hydrocele with herbs
The natural remedy to permanently cure testicular hydrocele that we offer is composed of two elements: a herbal tea and an ointment. The combined action of the decoction of the powder and the ointment results in the efficient absorption of all the liquid contained in the scrotum. The first effects will be felt very quickly and you will notice that your testicles will gradually return to normal. The use of natural plants very often give positive results and act significantly against hydrocele. This natural remedy is the secret to permanently curing testicular hydrocele.
Trust us ! It is the perfect solution for those who want to cure testicular hydrocele naturally and especially for those who want to avoid the operation.
The natural remedy against testicular hydrocele that we offer is effective, fast, durable and above all, it will prevent you from going through an operation. It is a miracle solution to cure testicular hydrocele. Being natural products based on plants and herbs, our herbal teas have no side effects, either on the body or on health.
Our treatment is not dangerous. You will, therefore, be able to overcome testicular hydrocele without operation and without fear of the appearance of side effects. To discover this remedy click here!
To contact our experts please call or write to us on the following number, tel / WhatsApp
: https://wa.me/22996374527
Symptoms of hydrocele
In many cases, there are no specific symptoms that indicate a hydrocele. However, some experience pain, the scrotal skin turns red, and a feeling of pressure at the base of the penis. Usually, pain is not felt until the size of the scrotum increases. The swelling can change within a day. In babies, the hydrocele swelling usually goes away on its own.
Seek immediate medical attention if:
- You feel a sudden pain in the scrotum, even though there is no swelling.
- You notice swelling in the scrotum.
- You have a baby with a hydrocele that does not go away after a year.
Causes of hydrocele
Most of the causes of hydrocele are unknown. In babies, this condition can form before birth. Hydrocele can also be a sign of open space between the stomach and the scrotum.
In the uterus, the baby's testicles in the abdomen descend into the scrotum through the space between the abdominal cavity and the scrotum. Both testicles are wrapped in a bag filled with fluid. Normally, the gap between the stomach and the scrotum will close before the baby is born or immediately after birth. Then the liquid in the bag will be absorbed by the body itself. However, the liquid may still remain after closing the gap, it is a non-communicating hydrocele. This fluid will usually be absorbed slowly during the first year after the baby is born. It is also possible that the space does not close and fluid continues to flow from the abdominal cavity or that there is reflux into the abdominal cavity when the scrotum is full. This condition is called communicating hydrocele and may be accompanied by inguinal hernias.
In adults, hydrocele can appear as a result of infection of the scrotum. Filariasis or elephantiasis, a parasitic infection caused by the Wuchereria bancrofti worm, is the most common cause of hydrocele in adults worldwide.
Hydrocele diagnosis
To diagnose hydrocele, the doctor will first make a complaint and examine the physical condition of the scrotum by:
- Checking the tenderness of the swollen scrotum.
- Illuminating the scrotum with a flashlight until light penetrates inwards ( transillumination ). If there is a hydrocele, the flashlight will indicate the presence of fluid around the testicles.
- Pressing on the stomach and scrotum to test for symptoms of inguinal hernia.
- If the doctor suspects that the swelling of the scrotum is the result of an infection, a urine or blood test will be done to confirm this. During this time, if the doctor suspects a hernia or testicular tumor as the cause of scrotal swelling, an ultrasound will be done.
Hydrocele treatment
- In babies, hydrocele usually goes away on its own until they are two years old. If the hydrocele still exists after this age or even shows pain, surgery is needed to remove it. The operation to remove a hydrocele is called a hydrocelectomy.
- In adults, hydrocele also goes away on its own within six months. Medical treatment will only be done if the hydrocele is causing pain or is bothersome. In addition, the hydrocele removal operation is performed only if the size of the hydrocele is large enough to cause discomfort and pressure on other parts of the body.
Some risks that may be faced by patients with hydrocele who undergo hydrocelectomy surgery are:
- Infection.
- Heart rhythm disturbances.
- Bleeding.
- Blood clots.
- Allergic reaction.
- Lesion of the scrotal nerve.
- Difficulty in breathing.
After undergoing a hydrocelectomy, the doctor will usually advise patients to use scrotal support and compress the scrotum with ice cubes to reduce swelling.
Complications of hydrocele
Male fertility will not be affected by the presence of hydrocele. However, the problem is that some serious diseases can be characterized by the appearance of hydrocele. One of them is an inguinal hernia, which gets trapped in the intestine in the abdominal wall and can lead to fatal complications. Additionally, hydrocele can also be an early sign of an infection or tumor.
Prevention of hydrocele
One of the causes of hydrocele is filariasis. To avoid filariasis, the best way is to avoid the bites of mosquitoes that carry the worm, for example by using mosquito nets.
Cirrhosis of the liver: causes and natural preventive treatment
Cirrhosis is a disease caused by long-term liver damage. In cirrhosis, liver damage leaves scars that prevent the liver from functioning normally, such as producing new proteins, fighting infections, removing unnecessary substances from the blood, digesting food, and storing energy from food. Now, this liver that is not functioning properly causes various problems in all parts of the body.
The experts at Dawasante have developed a special herbal tea for you to prevent the development of cirrhosis of the liver. This herbal treatment is 100% natural and also helps your liver to function properly. This treatment is for the treatment of hepatitis b and c. These two diseases being linked, treating hepatitis from the start is preventing cirrhosis of the liver. This treatment is preventative therefore to avoid when you already have a declared cirrhosis. To discover the treatment against hepatitis b and c click here!
Telephone / whatsapp: 00229 90312738 and +33644661758
THE DIFFERENT CAUSES OF CIRRHOSIS
Cirrhosis, actually, develops in several situations:
1- Chronic alcoholism: excessive and prolonged alcohol consumption is responsible for 50 to 75% of cases of cirrhosis.
Alcoholic cirrhosis is the most serious liver disease linked to alcohol consumption. According to the American Liver Foundation, between 10 and 20% of heavy alcohol drinkers will be at risk of suffering from cirrhosis of the liver.
Alcoholic cirrhosis is actually the last stage of liver disease caused by alcohol consumption. Initially, the disease that people addicted to alcohol will suffer from is fatty liver (alcoholic fatty liver), then if this habit persists and does not take proper treatment, this condition turns into alcoholic hepatitis, then becomes alcoholic cirrhosis.
However, a person can also have cirrhosis of the liver without ever having alcoholic hepatitis. In cirrhosis, the liver cells are damaged and can no longer regenerate, so the liver can no longer function normally.
Stopping alcohol consumption will not restore the function of damaged liver cells, but only serves to prevent damage from being generalized. Additionally, by immediately stopping drinking alcohol, you can increase your life expectancy with this condition.
A person with alcoholic cirrhosis who does not stop drinking has less than 50% chance of living for at least five years.
2- Chronic viral hepatitis type B, C and D (liver disease due to viral infection). In 15 to 25% of cases, hepatitis C is implicated, against 5% for hepatitis B.
Cirrhosis and hepatitis C are serious liver diseases. Although the two conditions are different, this disease turns out to be linked. Hepatitis C is one of the causes of cirrhosis of the liver. Hepatitis C and cirrhosis are health problems that can damage and inflame the liver. Hepatitis C is caused by a virus, while cirrhosis occurs due to the appearance of scar tissue in the liver that causes permanent damage. These two diseases have been shown to have a relationship. Hepatitis C is one of the causes of cirrhosis of the liver. Quoted by Healthline, out of 75 to 85 people who suffer from chronic hepatitis C, about 5 to 20 of them suffer from cirrhosis which can occur 20-30 years after having suffered from hepatitis C.
When someone has this virus for the first time, the liver problem is usually not that bad, even the symptoms are still mild. In addition, hepatitis C often appears unnoticed.
However, after a long time, the virus that enters the body will multiply in all liver cells. As a result, this virus destroys and damages cells. This damage will eventually form scar tissue (fibrosis) and over time, the scar tissue will fuse to form cirrhosis.
With the presence of extensive scars (cirrhosis), blood flow cannot flow to the liver, so the function of the heart also changes. This process can take time and get worse if left untreated.
3- Metabolic syndrome (NAFLD) (responsible for fat accumulation in the liver, galactosemia or glycogenosis for example) often exhorted by obesity and diabetes.
Non-alcoholic liver disease or non-alcoholic fatty liver disease (NAFLD) is a spectrum of liver disorders similar to alcoholic liver disease, occurring in patients who do not consume alcohol. Possible complications of non-alcoholic fatty liver disease
Because it rarely causes significant symptoms, many people with nonalcoholic fatty liver disease are unaware of the disease. In fact, without early detection and proper treatment, this condition can worsen and cause serious liver damage. Here are some serious complications that can result from nonalcoholic fatty liver disease:
Fibrosis: It is an inflammatory condition that causes sores around the liver and nearby blood vessels.
Cirrhosis: It is a fairly serious complication, where the liver shrinks and becomes marked. This liver damage is permanent and can cause liver failure and liver cancer.
However, the development of fibrosis or cirrhosis can take years. Therefore, it is important to change the lifestyle to prevent the disease from getting worse.
4- Other diseases, such as hereditary diseases (genetic hemochromatosis or Wilson's disease) or autoimmune diseases (primary biliary cholangitis CBP or primary sclerosing cholangitis CSP), are involved in 5% of cases.
5- Toxic hepatitis caused by certain drugs or by prolonged exposure to environmental toxins.
As cited by the Mayo Clinic, Tuesday (09/09/2013), toxic hepatitis is a disease in which the liver becomes inflamed due to certain substances that contain toxins, such as alcohol, drugs, products chemical or nutritional supplements. This inflammation can cause permanent liver damage and lead to the formation of scar tissue in the liver (cirrhosis) and can lead to liver failure. In addition, this disease can also develop when you take drugs in higher than normal doses. Many drugs can interfere with and / or damage the liver. Among these drugs, we have statins (used to treat high cholesterol), which can increase liver enzyme levels and cause liver damage (usually minor) without causing symptoms. Hundreds of plants contain pyrrolizidine alkaloids, which can damage the liver. Among these plants we can cite comfrey, borage and certain Chinese plants such as kuan dong hua (coltsfoot), zi cao (groomwell), pei lan (eupatory) and qian li guang (vieterula). Some plants used to make herbal teas contain pyrrolizidine alkaloids. Sometimes milk, honey and cereals are contaminated with these alkaloids which are consumed without knowing it. Liver damage can also occur with plants such as Atractylis gummifera, Camellia sinensis (used in the making of green and black teas), celandine (from the poppy family), chaparral, Canada germander, jin bu huan, kawa , ma huang (Ephedra), mistletoe, essence of pennyroyal (used in making teas) and syo-saiko-to (mixture of plants).
6- Heart failure with congestion of the liver
7-Diabetes and obesity
Diabetes and obesity can lead to cirrhosis of the liver through accumulation of fat in the liver.

VAGINAL MYCOSIS CAUSES: Natural treatment
The thrush is an infection of the vagina extremely widespread, caused by a fungus. It also affects the vulva. We are actually talking about vulvovaginal yeast infection "explains Dr. Loudi Khawach-Alissa, obstetrician-gynecologist. The fungus causing the yeast infection is generally Candida Albicans. Here is the natural treatment of the experts at Dawasanté against vaginal yeast infection. Click here. on the image below to discover this natural treatment.

Already present in the vagina in its natural state, it lives alongside bacteria which are part of the vaginal flora and protect the intimate area. These bacteria create acidity which acts as a shield against infection. Thus, Candida cannot develop further. Only when the vaginal flora is disturbed and the area becomes too acidic, Candida proliferates. "However, not all women develop a yeast infection as soon as their flora weakens or the acidity of the vagina fluctuates", specifies the gynecologist.
"We are talking about recurrent mycosis from four mycoses per year, with mycological proof (by vaginal sample). That is to say with symptoms. Beyond that, the case is considered severe. It is often a question of mycoses occurring during the period of the rules ", notifies doctor Patrick Cohen-Scali, obstetrician-gynecologist. This is the case of Morgane, 30, who for nearly seven years contracted yeast infection almost every month during her period. "At best, it was two out of three months and the seizures lasted between 4-7 days."
"The yeast infection is not a sexually transmitted infection since a yeast infection develops without sexual intercourse, underlines Patrick Cohen-Scali. It is only very rarely contagious. It sometimes happens that the man feels irritated after sexual intercourse. with a woman who has a yeast infection, but it is only treated if it shows symptoms (redness, burning, itching) because it in turn becomes contagious.
From this brief explanation, we will list the causes of vaginal yeast infection.
To the number of causes we have:
Genital yeast infection is linked to an excess of Candida albicans yeast on the skin. This proliferation can be linked:
- hormonal changes linked to the rules. Postmenopausal women suffer less from yeast infections than other women;
- during pregnancy (often in the third trimester);
- vaginal acidity linked to excessive hygiene in this area;
- poor local hygiene. It is imperative to wipe from front to back to avoid contaminating the vagina;
- diabetes;
- taking certain antibiotics;
- wearing synthetic or tight clothing;
- sexual intercourse even if the genital yeast infection is neither a sexually transmitted infection nor a sexually transmitted disease.
To be more precise in our explanations
A vaginal imbalance can trigger a yeast infection. If the vaginal flora is weakened, so too is the protective barrier of the vagina. The vaginal flora is weakened when taking antibiotics for example, which kill "good bacteria", but also during the excessive intimate toilets. Too much rubbing and especially washing the inside of her vagina - while it is self-cleaning - damages the flora. In addition, improper care changes the pH of the vagina. It is also noted that stress and fatigue lower the immune system.
In addition, fungi love moisture: “It can cause local maceration and call for a yeast infection,” says Loudi Khawach-Alissa. Irritation is also a cause of yeast infection because it is an inflammatory reaction that increases heat and maintains the humidity of the intimate area. " Thus, wearing the thong is not recommended: it creates friction and therefore irritation. In addition, thongs are rarely made of cotton, a material that absorbs moisture. Irritation can also be due to poorly lubricated intercourse or hygienic protection in some women.
"If Candida likes humidity, it also likes sugar. An unbalanced diet too rich in sugar nourishes fungi. Diabetic women are more prone to yeast infections," Loudi Khawach-Alissa tells us.
"The flora can also be disturbed by a hormonal imbalance. Thus, the mycoses occur according to the periods of life. A high estrogen level causes a modification of the wall of the vagina and a weakening of the local immunity", explains Patrick Cohen -Scali. During pregnancy, the risk of a yeast infection increases because estrogen levels are high. This is also the case just before the period.
But a lack of estrogens, such as in the case of the microdose pill or menopause, can lead to hormonal disorders and weaken the defenses of the vagina. "No direct link has ever been established between mycosis and the pill, but the latter may play a role since it controls hormones", states Dr. Khawach-Alissa
Anything that destabilizes the vaginal flora can cause the development of a yeast infection. To be banned in particular: an excess of personal hygiene, the use of unsuitable soaps or the wearing of too tight clothes which can cause its appearance.
Other factors that can promote the development of a mycosis:, travel to an exotic country, excessive exercise, or heat. In these cases, it is important to follow measures in order to avoid it.
If the natural balance of microorganisms is altered, the yeast can multiply and become the dominant organism in the vagina. This phenomenon is so common that most women suffer from infections with yeasts at least once in their lives. Disruption of the normal and normal vaginal environment can occur in any of the following cases:
- An immune system weakened (eg because of HIV / AIDS, of steroid use, pregnancy, of the cancer chemotherapy or other drugs that suppress the immune system)
- Use of showers or feminine hygiene sprays
- Cotton underwear, tight or not
- Hormonal changes
- Ovulation
- Menopause
- Pregnancy
- The use of birth control pills
- Use of hormone therapy
- Vaginal yeast infections are caused by a fungus.
- The most common fungus in women is called Candida albicans.
- This condition is also called candidiasis , genital candidiasis, or vulvovaginal candidiasis (CVV).
- In difficult cases, there may be a yeast resistant organism or a mixed infection with Candida as one of the organisms.
- Yeast infection can spread to other parts of the body, including the skin, mucous membranes, heart valves, esophagus, and other areas.
- In rare cases, a yeast infection can cause life-threatening systemic infections, especially in people with weakened immune defenses.
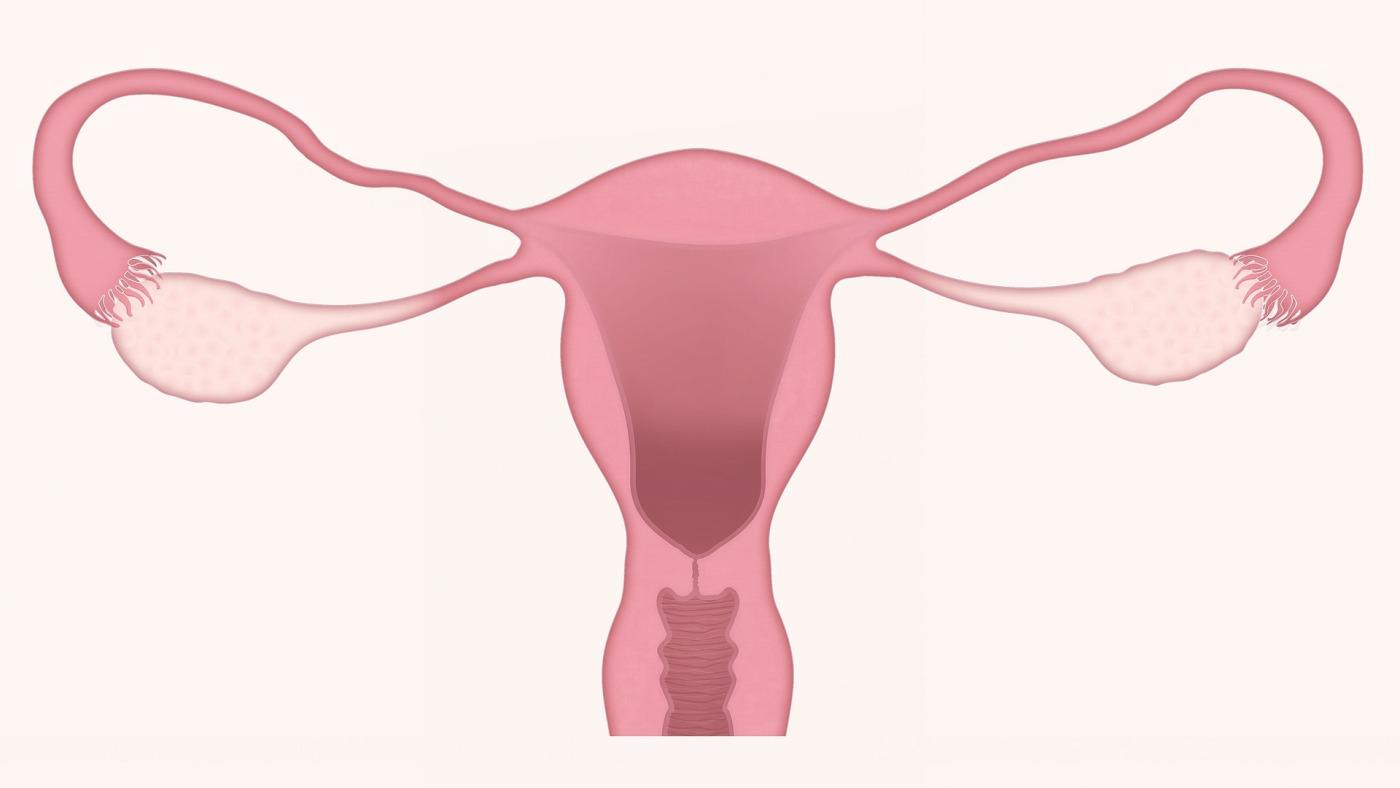
CLOGGED FALLOPIAN TUBES: What you need to know
The infertility is not only related to ovulation problems. Problems can also arise with the tubes when they are blocked or damaged. The egg and the sperm just can't seem to meet. However, Dawasanté experts provide you with a natural herbal treatment to unblock your tubes permanently without side effects and without surgery.
Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
What are the tubes?
- The uterine tubes or fallopian tubes are part of the genital system. There are two, which are on either side of the uterus. They connect the ovaries and the uterus via the pinna.
- The tube-shaped uterine tubes are used to receive the oocytes released every month from the ovaries and to transport them to the uterus. When the egg is expelled by the ovaries during ovulation, it is sucked in through the pinna of the tube. Fertilization (meeting between the egg and the sperm ) takes place in the tubes, during the journey from the egg to the uterus.
- For a woman to get pregnant and have a baby, the tubes must be functioning normally and be intact (at least one!). In 15% of cases of fertility disorders, the causes are linked to an abnormality of the tubes.
Tubal obstruction: what is happening?
- When the tubes are blocked , it will interfere with the movement and progression of the egg and sperm. Either the egg cannot meet the sperm (and there is no fertilization) or there is fertilization, but the egg cannot progress to the uterus.
- When fertilization does not take place or remains impossible, the egg is automatically lost in the abdominal cavity. We are talking about tubal sterility.
- If the blockage is not complete, the fertilized egg will be able to circulate, but will have difficulty making its way to the uterus. The egg will then implant in the tube and evolve into an ectopic pregnancy. At some point, the tube will rupture, causing internal bleeding.
Tubal abnormalities: what are the causes?
Many conditions can lead to blockages in the tubes and cause infertility. This anomaly is linked to genital infections, endometriosis or a sequel to surgery (adhesion for example).
Genital infections
- Genital infections are most often the result of sexually transmitted diseases that affect the tubes.
- Salpingitis is an inflammation of the tubes due to a genital infection. It can be acute (that is, the infection is recent) or chronic (the infection has occurred in the past and still persists) and causes obstruction of the tubes. Infections associated with salpingitis are usually caused by Chlamydia, mycoplasmas or gonococci. These are the germs responsible for sexually transmitted diseases, but which often go unnoticed.
- To prevent these infections, it is recommended to protect yourself during sexual intercourse (especially in the case of multiple or occasional partners) and regular monitoring by your gynecologist is necessary.
Other infections
- Other infections can infect the tubes. In case of peritonitis (an infection of the peritoneum) for example, following a complicated appendicitis, the tube can be infected.
- Uterine infections can also block the tubes. In the event of a history of abortion or miscarriage, tissue scars after these events will develop and form obstacles in the tubes. This is also the case with one or more history of ectopic pregnancy.
Endometriosis
- The Endometriosis is a gynecological condition in which the endometrial tissue which normally covers the uterine wall, is found in the fallopian tubes. The abnormal presence of this uterine lining in the tubes will block the progression of spermatozoa to the egg and prevent fertilization.
Surgical sequelae
- We talk about adhesion when the walls of the tubes stick together, preventing the movement of the egg and sperm. These adhesions are sometimes post-operative complications. They can form following an appendectomy or surgery of the ovaries or uterus. These post-operative complications are rare today because they are easily controlled.
How do you know if the tubes are blocked?
-
The obstruction in the tubes is often difficult to detect because there are few symptoms (possibly some abdominal pain or more abundant vaginal discharge). Consultations and analyzes are only carried out during the infertility assessment carried out when the woman who wants a child cannot get pregnant, after having had regular and unprotected sex for 1 year. During this assessment, in addition to the questioning and clinical examinations, the doctor will have to prescribe several examinations and analyzes to identify the problem.
- The specific test to detect an abnormality in the patency of the tubes is hysterosalpingography. It consists of injecting opaque product from the cervix and following the progress of this product in the tubes by an x-ray.
- In addition to the hysterosalpingography, the doctor may need to perform a hysteroscopy, an examination which allows the uterine cavity to be visualized using an endoscope (an optical fiber) through natural channels.
- A laparoscopy can also be considered: under general anesthesia, it allows the tubes to be examined from "inside" with an optical device after having made a small incision at the navel.
Tubal abnormalities, what treatment?
- Treatment will depend on the cause of the obstruction. Only the doctor is able to prescribe the appropriate drugs or treatment methods. The need for treatment depends mainly on the state of patency of the tubes, the state of the genitals and the state of health in general. You are free to discuss all the treatment options that may be available to you to find the most suitable for you.
- The doctor may indicate laparoscopic surgery (laparoscopy), if your state of health allows it and according to certain parameters evaluated by the doctor. It is a surgical procedure performed under general anesthesia.
- Depending on the state of the patency of the tubes, the doctor may suggest a salpingectomy, a surgical procedure that involves removing the blocked and diseased tube, especially in the case of a hydrosalpinx (the tube is full of liquid). You can then be a candidate for in vitro fertilization.
- Tubal cannulation is a less burdensome surgical procedure than laparoscopic surgery, performed when the obstruction is located closer to the uterus. The operation consists of introducing a cannula through the uterus to unblock the tube.
Good to know: if only one of your tubes is blocked, treatment is not always mandatory, pregnancy is possible. If both are blocked, there are other options available to help you get pregnant, especially if the methods of treating blocked tubes remains thin. The IVF is now the oldest method, but the most appropriate for getting pregnant if tubes plugged.
If your fallopian tubes are blocked, it will cause temporary infertility since the meeting between the sperm and your oocyte cannot take place. What are the causes of blocked tubes ? Are there any treatments to remedy blocked tubes
The uterine or fallopian tubes are an integral part of the female genital system . These tubes, since there are two, play an essential role in reproduction: they connect the ovaries and the uterus by the pinna. Their main objective is to receive the eggs released every month during the period of ovulation and to lead them to the uterus. The phenomenon of fertilization occurs in the tubes during the path between the egg and the uterus. In order to get pregnant, the tubes have to work properly. Indeed, this would prevent the meeting between the male and female gametes. Note that 15% of infertility cases result precisely from this style of abnormality in the tubes .
The causes
There are many reasons for the blocked fallopian phenomenon . First of all, there is salpingitis which is an inflammation of the tubes. Then comes the case of genital infections , usually caused by sexually transmitted diseases. That's why doctors recommend protecting yourself with each intercourse , especially in the case of multiple partners. This can indeed lead to infertility in some cases. The endometriosis is itself a disease that can also affect the fallopian tubes. It can interfere with the path of sperm to the oocyte feminine. Inflammation of the small pelvis can affect and obstruct the upper part of the reproductive organs. As for abnormalities affecting the vagina and uterus , they can also be a source of possible infertility . Myomas, which are usually benign growths, can also come into a tube and block it. Finally, certain surgical sequelae can play a role in the malfunction of the tubes .
Tubal obstruction and treatment
Obstruction in detail
First of all, you must first be sure that your tubes are well blocked. The symptoms are not necessarily obvious to detect because the pain is minimal. It is when you go for analyzes (such as during the infertility assessment ) that we can see if this is the case or not. This very specific examination consists of injecting a product from your cervix and following its progress to the tubes using an X-ray. The blocked tubes can also be detected in other tests such as hysteroscopy and laparoscopy. If your fallopian tubes are indeed blocked, it will upset or simply make fertilization impossible. When this is impossible, we speak of tubal sterility. If the obstruction is not complete, the fertilized egg will implant in the tube before creating a uterine pregnancy, possibly causing internal bleeding if the tube ruptures.
Possible treatments
The treatment of this pathology will depend both on the nature and on the cause of the obstruction. You will need to go through stimulation of ovulation by administering drugs in order to produce eggs in each cycle . The intervention is recommended for women with both tubes blocked, but it is not always enough to improve fertility . In some cases, women will then use IVF to get pregnant.
When the fallopian tubes are blocked, the meeting between a sperm and an oocyte cannot occur. This obstruction therefore constitutes a temporary cause of infertility or, in the most severe cases, of sterility. There are many reasons for the obstruction of one or both uterine ducts. What are they ? What are the possible treatments? Response elements.
What are the fallopian tubes used for?
Better known as the uterine tubes , the fallopian tubes are an integral part of the female genital system. Thus, the two tubes play a major role in the process of human reproduction since they connect the ovaries and the uterus. It is in them that the oocyte, resulting from the ovary, transits and can be fertilized by a sperm. In some cases, these uterine tubes can become blocked, preventing the meeting of male and female gametes.
Blocked fallopian tubes: what are the causes?
There are many possible reasons for the obstruction of one or both fallopian tubes :
- the PID : it corresponds to inflammation of the fallopian tubes. It is mainly caused by bacteria from the Chlamydiae family , although in some cases gonococci or mycoplasmas can be responsible.
- genital infections: these are often caused by sexually transmitted infections (STIs). It can lead to cases of infertility or sterility.
- the Endometriosis : This disorder is due to an abnormal proliferation of endometrial tissue outside the uterine cavity. This gynecological pathology can affect the fallopian tubes and hinder the progression of sperm to the oocyte.
- inflammation of the small pelvis: this is an upper genital infection (IGH), that is to say of the upper part of the reproductive organs.
- congenital anomalies of the uterus or vagina: these so-called "Mullerian" anomalies can reduce a woman's chances of getting pregnant.
- the myomas : these benign growths can be housed in a trunk and obstruct the passage.
Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.

WOMEN'S INFERTILITY: CAUSES, SYMPTOMS AND NATURAL TREATMENT
WOMEN 'S INFERTILITY : CAUSES, SYMPTOMS AND NATURAL TREATMENT
What is female infertility? What are its causes ?
The infertility is the inability for a couple to achieve pregnancy or to a woman, to lead his term gestation. It is estimated that infertility is established after two years of unprotected sex. Unlike infertility, female infertility is not permanent. It can result from various gynecological disorders or dysfunctions: endometriosis, ovarian dysfunction, uterine polyps, obstruction of the fallopian tubes, obesity, stress, excessive alcohol consumption. However, to remedy this problem, Dawasanté experts provide you with a natural treatment based on medicinal plants to permanently cure infertility.
HERBAL TEA AGAINST FEMALE INFERTILITY
Our natural remedies are the secret to cure any form of female infertility. We offer you a definite advantage: the absence of undesirable effects and contraindications. The natural approach is often the best approach to find a solution. Our natural remedies have allowed many women to have children. Being natural products based on plants and herbs, our natural remedies have no side effects, either on the body or on health. Our natural treatment is not dangerous. You can therefore cure female infertility without fear of the appearance of side effects.
CLICK ON THIS LINK TO GET THIS PRODUCT !!
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
What are the symptoms of female infertility?

The main symptom of female infertility is the absence of pregnancy. But beware, conceiving a child can naturally take time. So do not worry if the baby tests follow one another without the expected result. The process of fertilization is complex and can take time. However, it is advisable to consult a gynecologist if the absence of pregnancy is associated with menstrual cycle disorders ( amenorrhea , dysmenorrhea, etc.), abnormal vaginal discharge, or pelvic pain.
Who are the people at risk?
From the age of 30, female fertility tends to decrease. In addition, tobacco, alcohol and caffeine consumption also represent potential impediments to fertilization and can increase the risk of spontaneous abortion. Finally, physical condition is also an essential parameter. Thus, women who are overweight or, on the contrary, very thin may have difficulty in getting pregnant.
How is the diagnosis of female infertility made?
In the event of difficulty in obtaining a pregnancy, it is essential to consult a gynecologist, the only practitioner authorized to carry out an appropriate medical investigation. For this, the health professional has a battery of tests to confirm and detect the exact cause of infertility: blood tests, vaginal smear, pelvic ultrasound, hormonal assessment ... For the most difficult cases, he can also perform the Hühner test, a post-coital test that allows, among other things, to analyze the quality of cervical mucus.
What are the treatments for female infertility?
Indeed, the management of female infertility will depend on its origin. If it is menstrual disorders, hormonal treatments (ovulation stimulators, etc.) may be recommended. In addition, the surgical route will be preferred in the presence of ovarian cysts or obstruction of the fallopian tubes, while the use of medically assisted procreation techniques will be offered to certain couples.
Plants for hormonal detoxification
Due to the number of pollutants present in our daily environment, we are constantly exposed to many products that disrupt our hormones. (1,2,3) We call them, moreover, endocrine disruptors. These substances or compounds interfere with the proper functioning of our hormonal system and can increase the risk of suffering from infertility. Even by eating well, by not taking the car, by making your cosmetics and cleansers yourself, you risk coming into contact with certain endocrine disruptors, if only in the air you breathe. One interesting strategy for preserving your fertility is to help the body detoxify itself from endocrine disruptors. Here are some interesting herbs to help the liver with this task:
Dandelion (root)

Dandelion is one of the best liver plants. We know that it is the liver that takes care of breaking down the surplus hormones with a view to their elimination and the dandelion takes care of decongesting it while helping the intestinal elimination of hormones via the bile.
Milk thistle (flower)

Another beautiful liver plant! Milk thistle will help protect the body from toxic and fertility-damaging substances and help decrease excess estrogen in circulation.
Turmeric (rhizome)

Turmeric is one of the most antioxidant and anti-inflammatory plants. It helps stimulate the liver and the gallbladder and therefore promote the elimination of excess hormones. It also helps reduce inflammation and prevent the formation of free radicals, 2 factors that are highly harmful to reproductive health.
Plants to reduce stress
Stress is very damaging to reproductive health. Among other things, it can disrupt the normal production of hormones, lengthen the menstrual cycle, prevent ovulation and adversely affect the quality of the ovum and sperm. To calm daily stress, here are some interesting plants to take in herbal tea:
Lemon balm (leaf)

It is the plan of letting go! Have you been told that it is by letting go that you will get pregnant ? If you have difficulty, choose lemon balm. Plus, it will help your mood and digestion.
Oats (straw)

Oats are a great tonic for the nervous system. In addition, it contains several nutrients favorable to fertility and the cycle of women, including calcium. To be taken long term.
The motherwort (flower)
The motherwort is used for a range of problems including anxiety, depression, irritability, mood swings, etc. It is one of the best herbs to have on hand when the nervous system seems exhausted.
Plants that nourish the reproductive system
In addition, to get pregnant, it is important that the body has all the essential nutrients. The most important nutrients for male fertility are: copper, omega, zinc, selenium and vitamins B, C, D. For women: Omega 3, calcium, magnesium, iron, manganese, zinc and vitamins A (especially beta-carotenes), B, C, D, E. A good way to get the most vitamins and minerals possible, is to add nutritious plants to your daily life. Here are a few examples:
Nettle (leaf): Nettle is one of the richest nutritious plants! It contains a lot of iron, beta-carotene, B vitamins and vitamin C.
Raspberry (leaves): The raspberry, in addition to being the tonic par excellence of the reproductive system of women, contains a lot of iron, vitamin C and beta-carotenes. It also contains certain B vitamins, calcium, magnesium and potassium among others.
Although herbs are wonderful allies in improving your fertility, if you have a particular or long-standing infertility condition, consult a qualified naturopath or herbalist for more personalized recommendations. And more in-depth monitoring of your condition. Remember to consult a doctor for medical advice or if in doubt.
CLICK ON THIS LINK TO GET THIS PRODUCT !!
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
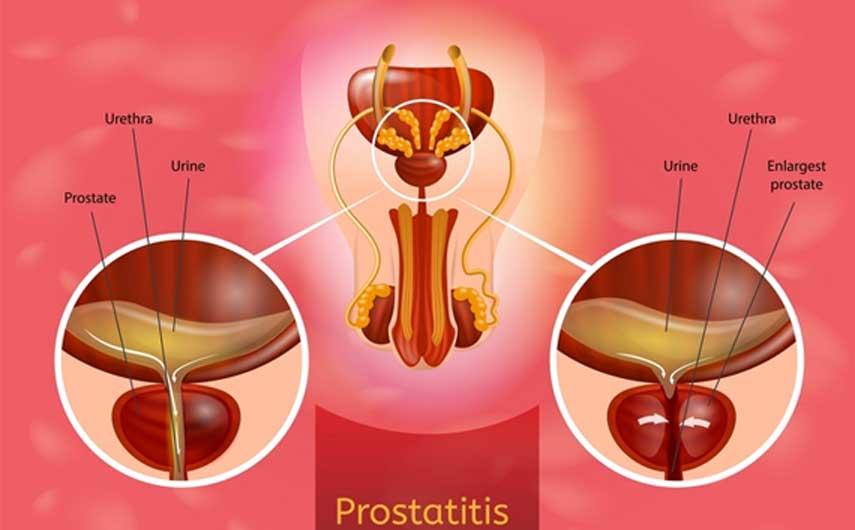
CAUSES OF PROSTATITIS : Natural treatment
WHAT BRINGS ABOUT PROSTATITIS?
The prostate is a walnut-sized gland that all men have. It is located under your bladder and in front of your rectum. The job of the prostate is to make a fluid that contains semen. This fluid protects the sperm as they travel to a woman's egg.
If your prostate becomes swollen, painful, and inflamed, you have a condition called prostatitis.
The Prostatitis is the infection, acute or chronic, prostate (gland located below the bladder, found only in humans). In some cases of chronic prostatitis, no causal germ is found on examinations. This is called chronic non-bacterial prostatitis. Any urinary tract infection accompanied by fever in men is prostatitis, except pyelonephritis (kidney infections).
The chronic prostatitis is the result of urinary tract infections repeated. The prostate is an anatomical crossroads between the urinary tract and the male genital tract. Any prostatitis can therefore be the consequence of bacterial contamination of the urethra, but also of an infection of the entire urinary tract (bladder, ureters, kidneys).
The most common prostate diseases are cancer, adenoma (benign enlargement of the gland) and prostatitis. This is characterized by acute or chronic infection of the prostate. It can affect men of all ages, with a predominance around 30 or 40 years old, unlike cancer or adenoma that affects older men.
It's not cancer, and it's different from an enlarged prostate. Here is the natural herbal treatment to cure prostatitis and increase fertility.
NATURAL TREATMENT FOR PROSTATITIS
This natural treatment to permanently and quickly cure prostatitis that we offer is composed of two elements: a herbal tea and an ointment. It also helps relieve urinary symptoms, including those caused by an enlarged prostate without having to have an operation. It works in particular by reducing the swelling of the prostate gland and providing immense relief. The natural treatment also helps cure urination difficulties and it restores sexual balance. So this is the secret to cure prostatitis by plants without surgery and without side effects.
CLICK HERE TO GET THIS PRODUCT!!
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
So in the rest of this article we will list the causes of this condition.
Prostatitis is a group of diseases affecting the prostate that present with similar symptoms such as pain or discomfort in the perineal region and genitourinary tract.
The condition is not always caused by an infection and there is not necessarily inflammation of the prostate. Prostatitis can be divided into four categories:
- Acute bacterial prostatitis : This is an acute infection of the prostate.
- Chronic bacterial prostatitis : This is due to poorly treated acute prostatitis or recurrent urinary tract infection.
- Chronic non-bacterial prostatitis or chronic pelvic pain syndrome : Symptoms of prostatitis are present, but infection is not the cause. It can be taken with or without inflammation.
- Asymptomatic inflammatory prostatitis : Infection and inflammation occur, but there are no symptoms.
In cases where prostatitis is caused by bacterial infection, the diagnosis is simple, and in its acute form, treatment is effective. However, in chronic non-bacterial forms, the origin is not entirely clear, so diagnosis and treatment are complicated.
Prostatitis can cause problems with sexual activity and infertility in men.
Causes and risk factors of prostatitis :

Different factors may be involved: food, urine, sex, influence of stress, sports practice including cycling ... Chronic bacterial prostatitis is the most common cause of recurrent urinary tract infection in men and 5 to 10 % of all prostatitis.
Prostatitis is sometimes the consequence of sexual contamination (sexually transmitted disease). But very often, no triggering factor is found.
In the elderly, prostatitis is frequently the consequence of a urinary infection , itself secondary to an enlarged prostate which promotes urinary stasis. We then speak of adenomitis.
To be more specific Prostatitis can affect men of all ages, but it is more common in young and middle-aged men. Other risk factors for the development of prostatitis are:
- History of prostatitis
- Have a recent urinary tract infection
- Recent use of a urinary catheter or recent urologic procedure
- Enlarged prostate gland
- Having rectal sex
- Structural or functional abnormality of the urinary tract
- Dehydration (not enough fluid)
- Trauma or injury to the local pelvis such as cycling or horseback riding
Acute prostatitis is caused by bacterial damage. Chronic prostatitis can be bacterial or non-bacterial, inflammatory or non-inflammatory. Different factors may be involved: food, urine, sex, influence of stress, sports practice including cycling ... Chronic bacterial prostatitis is the most common cause of recurrent urinary tract infection in men and 5 to 10 % of all prostatitis. Chronic non-bacterial prostatitis is the most common prostatitis. Although other, rarer problems can affect the prostate, the most common are prostatitis, benign prostatic hyperplasia, and cancer.
Prostatitis is inflammation of the prostate, often due to a bacterial infection. Most often, it is the E. Coli bacteria that is involved (more than 80% of cases).
Most of the time, acute prostatitis is due to a bacterial infection of urinary origin. The most frequently encountered germ is the bacterium Escherichia coli. The contamination can be sexual, but this is infrequent. Infection can also appear when urine is stagnant in the bladder due to the presence of an adenoma that blocks the complete emptying of the bladder. More rarely, an infection can occur following the insertion of a urinary catheter or a prostate biopsy (removal of a fragment of the prostate to analyze it). Chronic prostatitis (which lasts at least 3 months), which corresponds to a significant inflammation of the prostate, often results from acute prostatitis that is poorly treated or recurrent. Acute bacterial prostatitis is often caused by common bacterial strains. The infection can start when bacteria in the urine get into your prostate. Antibiotics are used to treat the infection. If they do not kill bacteria, prostatitis may recur or be difficult to treat (chronic bacterial prostatitis).
Nerve damage in the lower urinary tract, which can be caused by surgery or trauma to the area, could contribute to prostatitis not caused by bacterial infection. In many cases of prostatitis, the cause is not identified.
Prostatitis being a seminal infection; the latter are invasions of pathogenic microorganisms that occur somewhere in the male reproductive and urinary tract, so that they may be present in seminal fluid. They can affect the testes, causing orchitis, the epididymis causing epididymitis, or prostatitis if it occurs in the prostate.
In the path that sperm and seminal fluid must follow to go outward, contact with the infected area will take place, which can impair the ability of the sperm to fertilize the egg. Inflammation from the infection can cause a blockage and prevent semen or ejaculate from coming out.
Likewise, It can also result from various sexually transmitted organisms such as Neisseria gonorrhea, Chlamydia trachomatis or HIV (learn how to eat right with AIDS). The other organisms responsible for the infection are the same as those most often found in urinary tract infections, such as Escherichia coli. In many cases (especially in the chronic form of prostatitis), no specific cause for prostatitis can be found.
CLICK HERE TO GET THIS PRODUCT!!
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD

OLIGO-ASTHENO-TERATOSPERMIE
OLIGO-ASTHENO-TERATOSPERMIA
You have been trying to have a baby for several months, but it is late. After tests, your doctor told you that your loved one has oligoasthenoteratospermia (OATS). What are OATS and what are the consequences?
However, the experts at Dawasanté provide you with a natural treatment to permanently cure oligo- asthenoteratospermia.
Click HERE or on the image below to discover this natural treatment
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
What is Oligoasthenoteratospermia or OATS?
OATS designates a set of abnormalities found during the spermogram during a male infertility assessment. The OATS groups together a low concentration of sperm (oligo) with therefore too few spermatozoa to naturally fertilize an oocyte, too low mobility of these spermatozoa (astheno) which does not allow them to join the oocyte and too large a proportion abnormal sperm (terato). However, OATS can present varying degrees. It can be severe, with very low mobility and concentration indices while the malformation index is very high. It can be moderate with indices closer to normal. Intermediate forms exist with indices of the same degree or which may be of different degrees: severe for one or two types of indices (eg: mobility and concentration) and moderate for the third.
What happens after diagnosis of the OATS?
Once the OATS is discovered, the doctor will look to determine if there are any causes for these abnormalities. Indeed, OATS can be reduced, at least in part, depending on its origin. He will look first for signs of infections, old or recent. Some infections, such as chlamydia, can cause a decrease in male fertility. Their treatment can help regain better fertility. Likewise, the treatment of a varicocele (varicose veins in one or both testicles) or stopping smoking may improve the results of a spermogram. Further research will be carried out to find out if there is a malformation in the testes or seminal tract. In all cases, a second spermogram will be done because it is possible that significant variations appear and allow to hope for other opportunities for natural fertilization.
What to do to have a child in the event of OATS?
If the diagnosis of OATS is confirmed, the possibility of natural fertilization is reduced. However, it does exist, especially if it is a moderate form. However, certain factors, such as the woman's age or the length of time contraception has been stopped must be taken into account and assisted reproduction (ART) may be considered. Depending on the case, it will be an in utero insemination (IUI) where the sperm is introduced directly into the uterus, and in vitro fertilization (IVF) where the sperm is brought into contact with one or more oocytes in the laboratory or an intracytoplasmic sperm injection (ICSI) where sperm is introduced directly into an oocyte in the laboratory. These different techniques will be offered depending on the degree of OATS. The success of IVF or ICSI is of the order of 25 to 30% which leaves hope to those who are concerned by this difficulty.
Asthenospermia is an abnormality of the sperm that is characterized by insufficient mobility while their number remains normal. Also called asthenozoospermia, this sperm fatigue is one of the possible causes of male fertility problems. What are the main causes? How is asthenospermia diagnosed? What treatment is there to promote procreation?
What is asthenospermia due to?
The main causes that can explain unsatisfactory sperm mobility are:
- a morphological anomaly of the male gametes,
- an infection,
- presence of anti-sperm antibodies
- medication,
- a varicocele,
- a dietary deficiency,
- a renal failure,
- liver failure
- chemotherapy,
- exposure to radiation,
- excessive alcohol consumption,
- a deficiency in calcium, vitamin D, or trace element ...
How is asthenospermia diagnosed?
A semen analysis, or spermogram, is used to assess the mobility of the sperm. It should be remembered that only mobile gametes can fertilize the egg. Many medical analysis laboratories rely on the classification decreed by the World Health Organization to classify spermatozoa:
- Level A (or I): progressive rapid sperm advance quickly and in a straight line,
- Level B (or II): the slow progressive spermatozoa advance slowly or in a curved line,
- Level C (or III): non-progressive spermatozoa move but do not progress,
- Level D (or IV): the sperm are immobile.
To be qualified as normal, the spermogram must show a minimum of 40% of motile spermatozoa and 32% of spermatozoa showing progressive mobility.
What solutions to have a child?
The management of asthenospermia varies mainly according to its origin. Thus, an infection will have to be treated according to its nature with appropriate antibiotic drugs while certain testicular abnormalities may, in some cases, be the subject of surgery. While there is no curative treatment for asthenospermia, certain drugs help improve the quality of sperm: vitamins, hormones, alternative medicine (herbal medicine, homeopathy, aromatherapy, etc.). When the treatments do not give satisfactory results, in vitro fertilization with donor sperm or an intracytoplasmic injection of sperm may be considered in the context of Medically Assisted Reproduction ( MAP).) when the couple wants a child.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
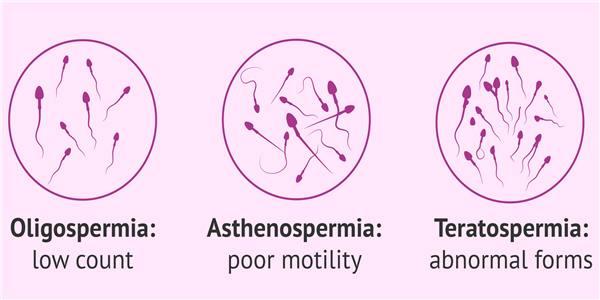
MALE INFERTILITY TERATOSPERMIA
The teratospermia (or teratospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. However, the experts at Dawasanté provide you with a natural treatment to permanently cure teratospermia and allow you to conceive quickly.
Click here or on the image below to find out what treatment
We deliver all over the world.
For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number.
Teratospermia is a sperm abnormality characterized by sperm with morphologic defects. These abnormalities can affect different parts of the sperm:
- the head, which contains the nucleus carrying the 23 paternal chromosomes;
- the acrosome, a small membrane at the front of the head that, at the time of fertilization, will release enzymes that will allow the sperm to cross the pellucid area of the oocyte;
- the flagellum, this "tail" which allows it to be mobile and therefore to move up from the vagina to the uterus and then the tubes, for a possible encounter with the oocyte;
- the intermediate part between the flagellum and the head.
Often, the anomalies are polymorphic: they can be multiple, in size or shape, affect both the head and the flagellum, vary from one sperm to another. It may be globozoospermia (absence of acrosome), double flagellum or double head, coiled flagellum, etc.
All these abnormalities have an impact on the fertilizing power of the sperm, and therefore on the fertility of the man. The impact will be more or less important depending on the percentage of normal sperm remaining. Teratospermia can decrease the chances of conception and even lead to male infertility if it is severe.
Often, teratospermia is associated with other spermatic abnormalities: oligospermia (insufficient number of spermatozoa-, asthenospermia (defect in sperm mobility. We then speak of oligo-asthenic-teratozoospermia (OATS).
Like all sperm abnormalities, the causes can be hormonal, infectious, toxic, drug-related. The morphology of spermatozoa is in fact the first parameter to be altered by an external factor (exposure to toxicants, infection, etc.). More and more specialists also consider that atmospheric and food pollution (via pesticides in particular) has a direct impact on the morphology of spermatozoa.
But sometimes, no cause is found.
The main symptom of teratospermia is difficulty conceiving. The fact that the shape of the sperm is abnormal does not affect the occurrence of malformations in the unborn child, but only the chances of pregnancy.
Teratospermia is diagnosed using a spermogram, one of the first examinations systematically performed in men during an infertility assessment. It allows a qualitative and quantitative study of sperm thanks to the analysis of different biological parameters:
- the volume of the ejaculate;
- pH;
- sperm concentration;
- the mobility of sperm;
- sperm morphology;
- the vitality of sperm.
The part about sperm morphology is the longest and most difficult part of the spermogram. In a test called a spermocytogram, 200 sperm are fixed and stained on smear slides. Then the biologist will study the different parts of the sperm under a microscope in order to assess the percentage of morphologically normal sperm.
The type of morphological abnormalities is also taken into account to estimate the impact of teratospermia on fertility. Several classifications exist:
- the David classification modified by Auger and Eustache, still used by certain French laboratories;
- the Kruger classification, the WHO international classification, is the most widely used in the world. Carried out using an automatic machine, this more “severe” classification classifies as atypical spermatozoa any spermatozoon which deviates, even very little, from the form considered as normal.
If the proportion of correctly formed sperm is less than 4% according to the WHO classification, or 15% according to the modified David classification, teratospermia is suspected. But as for any spermatic abnormality, a second or even a third spermogram will be carried out 3 months apart (the duration of a spermatogenesis cycle being 74 days) in order to make a firm diagnosis, especially as various factors can influence on sperm morphology (long abstinence time, regular cannabis intake, feverish episode, etc.).
A migration-survival test (TMS) usually completes the diagnosis. It makes it possible to have an evaluation of the number of spermatozoa able to end up in the uterus and able to fertilize the oocyte.
A sperm culture is often coupled with the spermogram in order to detect an infection which could alter spermatogenesis and lead to morphological defects of the sperm.
Teratospermia occurs when less than 4% of the sperm present in the male ejaculate is said to be “typical” or normal. The remaining 96% are carriers of abnormalities or have an alteration in their morphology. A normal sperm consists of an oval head, an intermediate body one and a half times longer than the head, and a long, thin tail (the flagellum) which promotes its mobility. The abnormalities detected can affect the head of the spermatozoon as well as its intermediate part or even its flagellum. There are also combined forms of anomalies.
Teratospermia is usually the cause of male infertility. Indeed, alterations in the morphology of spermatozoa can affect their mobility and prevent them from reaching the egg. There are different degrees of severity of teratospermia which can be classified as mild, moderate, or severe. The higher the degree of severity, the more difficult natural procreation will be.
Little is known about the causes of this anomaly. The origin can be infectious, medicinal, genetic, anatomical (varicocele or varicose veins of the testes), environmental or related to the hygiene of life. Finally, there are reversible forms of teratospermia. This is why the patient is generally asked to perform a second examination, 3 months apart from the first, in order to detect the persistence of the anomaly.
We deliver all over the world.
For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number.
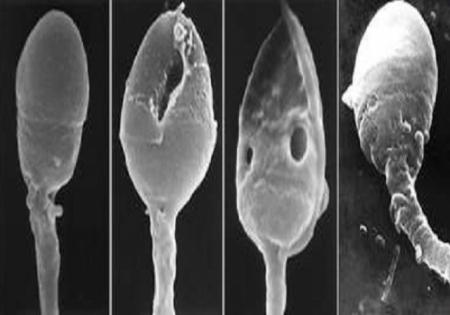
THE CAUSES OF TERATOSPERMIA: Natural treatment
The teratospermia (or teratozoospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. Dawasanté experts advise you to opt for a natural treatment without operation, against teratospermia.
Click HERE or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Teratozoospermia refers to the poor morphology of the sperm in a man's ejaculated semen.
These men have lower seminal quality and sometimes suffer from infertility and difficulty achieving pregnancy.
The causes of teratozoospermia are mostly unknown. However, we are going to address the possible alterations caused by these abnormal sperms in semen.
1-Defects in spermatogenesis
Most experts agree that the morphological changes in sperm occur during the last phase of their formation.
The spermatogenesis is the process by which sperm are formed in the testicles, which lasts about 3 months.
More precisely, spermiogenesis is the last phase of spermatogenesis, during which the spermatozoa, which already have their genetic content formed, undergo a process of maturation and acquire their characteristic morphology.
Once the sperm have their oval head and tail formed, they are released into the seminiferous tubules to follow their path.
Therefore, it is not surprising that any abnormality or alteration in spermiogenesis results in abnormalities in the head, neck or tail.
2-Reversible teratospermia
Teratozoospermia can be reversible or irreversible depending on the specific cause.
With reversible teratospermia, men can regain their seminal quality after a few months if they have received the appropriate treatment.
To check this, it is necessary to do another spermogram and compare it with the previous one.
We will now discuss the possible causes of reversible teratozoospermia:
2-1 Way of life
Although it may seem surprising, the lifestyle of men greatly affects the quality of their semen.
During times of stress and anxiety, sperm morphology may deteriorate, as many other parameters such as concentration and mobility.
The abuse of alcohol, tobacco, or other drugs are also factors linked to alterations in sperm.
Prolonged exposure to testicular heat affects spermatogenesis. Therefore, the bad habit of placing the computer on your legs, wearing tight clothes, or driving for a long time can cause teratozoospermia.
Testicular heat causes teratozoospermia

Finally, diet and sport also contribute to male fertility.
Men who are planning to become pregnant with their partner are recommended to maintain a good lifestyle, eat a balanced diet, exercise regularly and not consume substances that are harmful to the body.
2-2 Seminal infections
Semen infections refer to the invasion of microorganisms, bacteria, and viruses, into the male reproductive system.
Its presence is found in urine and semen, causing alterations in the sperm, as well as inflammation and obstruction of the seminal ducts.
The most common bacterial infections in the testes are chlamydia and gonorrhea. These infections can be fought with antibiotics and male fertility can be restored. If you would like more information on this, you can access the following article: Types of infections in seminal fluid.
The episodes of fever caused by flu or another disease may also occasionally affect sperm quality.
2-3 Pharmaceuticals
Sex hormones like testosterone, LH, FSH and inhibin have a very important role in the regulation of spermatogenesis.
Therefore, any drug that changes the appropriate levels of these hormones or affects their secretion by the brain has negative consequences for sperm production.
As we have already said, the alteration of the phase of spermiogenesis prevents the correct maturation of sperm and causes teratozoospermia.
Reversible causes of teratozoospermia
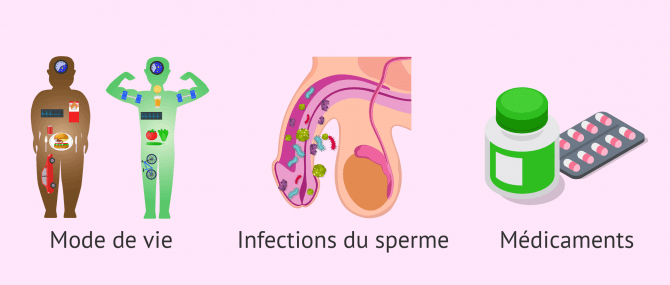
3-Irreversible teratospermia
If a man with teratozoospermia fails to improve his second spermogram after receiving treatment, one may begin to suspect that the teratozoospermia is irreversible.
In these cases, the couple will have to resort to assisted reproduction if they want to become a parent because it will naturally be very difficult to obtain a pregnancy.
In addition, there are other pathologies or situations that cause irreversible or prolonged teratozoospermia. The most relevant cases are examined below:
3-1 Cancer treatment
Chemotherapy and radiation therapy alters both sperm stem cells and sperm production, causing severe teratozoospermia and other more serious changes.
For these reasons, all men with cancer are advised to save a semen sample if they wish to have children in the future after they have overcome the disease.
3-2 Genetic diseases
It is one of the most difficult causes of diagnosis. Normally, when it has not been possible to determine the pathology that causes teratozoospermia, it is attributed to a genetic factor.
Defects in the genes or chromosomes of the sperm are a serious problem because they cannot be corrected.
3-3 Associated pathologies
Teratozoospermia can also result from other diseases that mainly affect the testes, for example:
- Trauma or blows to the testicles, especially in childhood
- Testicular varicocele
- Meningitis
- Diabetic sugar
In addition to all this, the age of males can also affect the morphology of the sperm. In particular, it has been observed that men over 45 have a higher rate of abnormal sperm in their semen.
Irreversible causes of teratozoospermia

4-Your frequently asked questions
4-1 Can live sperm have poor morphology?
By Zaira Salvador (embryologist).
Yes, teratozoospermia can be present in both living and dead sperm.
Dead sperm do not always have a bad morphology. Sometimes they are confused with immobile sperm and it is necessary to make a tincture to find out whether they are viable or not.
4-2 Can leukospermia cause teratospermia and male infertility?
By Zaira Salvador (embryologist).
Leukospermia, also known as leukocytospermia, is the appearance of leukocytes in semen, with a concentration level greater than 1 million per milliliter. The cause of this seminal pathology is an infection of the male reproductive tract which must be treated with antibiotics as it can affect spermatogenesis and cause oligospermia or teratozoospermia.
You can find the information in our article: Leukocytes in semen.
4-3 Are the causes of teratozoospermia and asthenozoospermia the same?
By Zaira Salvador (embryologist).
In most cases, asthenospermia and teratospermia have the same causes. The two seminal parameters are usually changed in the seminogram, known as astenoteratozoospermia. However, this is not always the case.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
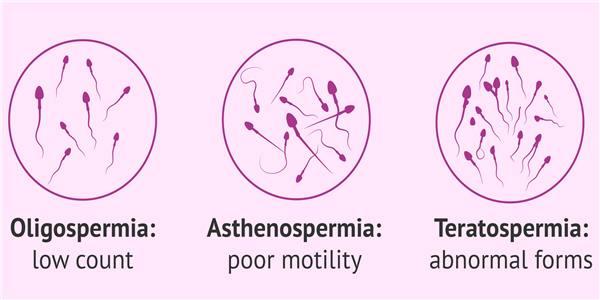
TERATOSPERMIA OR TERATOZOOSPERMIA: definition and treatment
Teratozoospermia or teratospermia is an alteration that occurs in men when more than 95% of their sperm have an abnormal morphology.
Therefore, teratospermia is considered a cause of male infertility due to a sperm factor, and its origin is varied and sometimes unrecognized. This is why the Dawasanté experts provide you with a natural treatment to improve the quality and quantity of your sperm; which will allow you to quickly conceive.
Click HERE or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number
There are several treatments to be able to conceive a child with sperm affected by teratospermia depending on whether the man's sperm has other spermatic disorders, such as, for example, sperm concentration or mobility.
1-Teratozoospermia: what is it?
Poor morphology of the spermatozoa, indeed the latter can present defects in the head, middle part or neck, or the tail.
The WHO estimates that a man with 4% sperm with a normal form (at least) does not have fertility problems. In lower quantity, we are talking about male infertility by teratospermia. This baseline changed in 2010, previously it was 14%, so it is possible that on other sites you will find that teratospermia is considered to be more than 85% abnormal.
According to the strict Kruger criterion, values equal to or greater than 15% of sperm with normal morphology are considered normal. This criterion is always stricter than that of the WHO, but the WHO is the one that is taken as a global reference.
The count of sperm of good or bad morphology is carried out through a medical examination called a spermogram, where the structure of the sperm is analyzed under a microscope.
There are several laboratories which in addition to the Kruger criteria, add those of the WHO.
If the medical report does not specify the details of the analysis to the laboratory, the parameters dictated by the WHO in 2010 are the reference values used.
Diagnosis of teratozoospermia

2-Causes
Teratozoospermia involves male infertility because the sperm that reach the oocyte are unable to fertilize it due to their poor morphology.
The causes that cause the existence of amorphous sperm in human semen are manifold and difficult to diagnose. Here they are:
- Genetic disorders
- Chemotherapy and radiotherapy
- Seminal infections and orchitis
- Varicocele and other testicular disorders
- Febrile period
- Diabetes or meningitis
- Tobacco, alcohol and drug abuse
- Poor lifestyle: poor diet, exposure to toxic substances, clothes that are too tight
Some of these factors can cause reversible teratozoospermia, which goes away with fever, infection, or periods of stress. In the same way, it is possible to recover a good spermatic morphology by improving one's lifestyle, diet, quitting smoking, etc.
3-Types
Sperm morphology defects are classified according to their position on the head, at the neck or at the tail. However, to diagnose teratospermia, all defects are taken into account.
Sperm is considered normal when it has a head with an oval shape and an acrosome inside. The neck or middle piece is slightly larger than the tail, and the tail is elongated and straight.
After analyzing the morphology of the sperm during the spermogram, it is possible to determine the degree of teratozoospermia depending on the seminal quality. For this, the laboratories use the Kruger criteria. Here is their classification:
- Mild teratozoospermia
- 10% to 14% of spermatozoa have normal morphology.
- Moderate teratozoospemia
- the percentage of normal sperm varies between 5% and 9%.
- Severe teratozoospemia
- less than 5% of sperm have normal morphology.
As we have commented before, it is the WHO criteria that are used to diagnose teratospermia, and therefore, this classification is obsolete. However, it is still possible to find it on some spermograms.

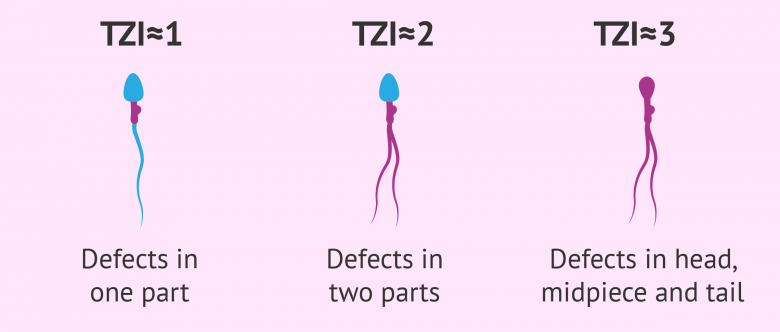
3-1 Teratozoospermia index
This seminal parameter is used to know the number of defects that each sperm has. It is possible that sperm has only one malformation, or several distributed over several parts.
In order to calculate the rate of teratospermia (TZI), we use the following formula: TZI = (c + p + q) / x , where each variable means:
- c = head malformations
- p = malformations of the middle part of neck
- q = tail malformations
- x = total number of abnormal sperm
The interpretation of these results is carried out as follows:
- TZI close to 1
- sperm with abnormalities in one area
- TZI close to 2
- spermatozoa with abnormalities in two areas
- TZI nearly 3
- sperm with defects on the head, neck and tail
It is important to note that the same seminal sample can present sperm of three types: one malformation, two, or three. The rate of teratospermia will indicate which type is most present.
4-Teratospermia and pregnancy
A man with teratospermia could have a natural pregnancy without problems if the rest of the seminal parameters such as concentration or mobility are not affected.
However, in cases where the pregnancy is delayed, it is possible to follow the doctor's recommendations to recover the correct sperm morphology.
On the other hand, if teratospermia has a genetic cause or is congenital, it is more difficult to find an effective treatment to cure it.
4-1 Natural treatments
First of all, men who suffer from teratospermia need to change their lifestyle and put aside bad habits like tobacco or alcohol.
A healthy and balanced diet always helps to recover some of the fertility. In concrete terms, foods rich in antioxidants and essential acids such as L-carnitine help improve sperm quality.
Oily fish is another product rich in omega 3 acids which bring great benefits to human reproductive health.
These nutritional contributions can also be taken by food supplements such as Andean maca or vitamin E supplements, a powerful antioxidant.
4-2 Assisted reproduction (ART)
In the case of fertility treatment to be able to achieve pregnancy and mild teratozoospermia, it is possible to perform artificial insemination (AI), if the concentration and mobility of the sperm allow it.
This is the first option to consider if the woman has no problems with fertility and the only cause of the lack of a pregnancy is teratozoospermia.
Faced with cases of moderate or severe teratospermia, it is necessary to do IVF - ICSI. It is an in vitro fertilization technique that uses the intracytoplasmic injection of sperm for the fertilization of oocytes.
If this topic interests you, you will find information here: IVF.
If you need to undergo IVF treatment to become a mother, we recommend that you use the Fertility Report. In 3 simple steps, which will allow you to know the clinics abroad that meet our rigorous quality criteria. In addition, you will receive a report with useful tips before you make clinic visits.
Finally, there is a new technique which is a variation of the previous one. It is known as IMSI and consists of amplifying the image before the micro-injection to be able to observe the sperm morphology in more detail.
The microscope used by IMSI to select the sperm has an objective that amplifies the image to such an extent that morphological abnormalities are detected.
5-Your frequently asked questions
5-1 What is the cause of teratozoospermia?
Teratozoospermia is an alteration that affects male semen and involves most of the sperm having an abnormal shape.
Due to their poor morphology, sperm cannot fertilize the oocyte and cause sterility.
The causes of teratozoospermia are as follows:
- Genetic alterations
- Chemotherapy and radiotherapy
- Semen infections and orchitis
- Testicular trauma
- Varicocele
- Fever
- Diabetes and meningitis
- Tobacco, alcohol, drugs
Bad eating habits, clothes that are too close to the body ...
Certain causes can be resolved (fever, quitting smoking, healthy habits ...), which implies that in some cases, the pathology is reversible.
5-2 Does teratozoospermia cause miscarriages?
In principle, the poor morphology of the sperm does not cause any miscarriage once the fertilization of the oocyte has taken place and the embryo has implanted. If, on the other hand, the sperm also have genetic disorders, this may be a cause of miscarriage.
5-3 How to improve the amorphous sperm of semen?
If the pathology of teratospermia is not specific, the man should follow some indications to modify his lifestyle, which could negatively influence his reproductive state. Some men who stop smoking or alcohol consumption and change their diet may see an improvement in their sperm quality after 3 months.
5-4 Can leukospermia cause teratospermia and male infertility
Leukospermia, also known as leukocytospermia, is the appearance of leukocytes in semen, with a concentration level greater than 1 million per milliliter. The cause of this seminal pathology is an infection of the male reproductive tract which must be treated with antibiotics as it can affect spermatogenesis and cause oligospermia or teratozoospermia.
You can find the information in our article: Leukocytes in semen.
We deliver all over the world.
For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number
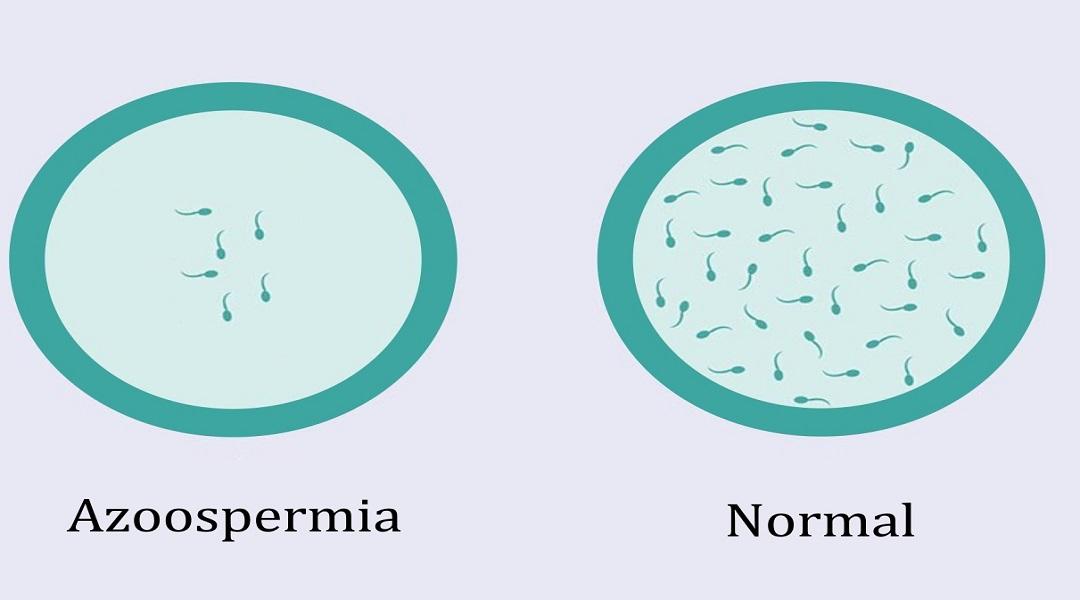
AZOOSPERMIA CAUSES: natural treatment
What is Azoospermia?
The azoospermia is a sperm abnormality characterized by the total absence of sperm in the ejaculate. It obviously leads to infertility in men, because in the absence of sperm there can be no fertilization. However, Dawasanté experts provide you with a natural herbal treatment to improve the quality and quantity of your sperm. Click here or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.

Azoospermia affects less than 1% of men in the general population or 5 to 15% of infertile men (1).
The causes
Depending on the cause, there are two types of azoospermia:
Secretory azoospermia (or NOA, for non-obstructive azoospermia)
Spermatogenesis is impaired or absent and the testes do not produce sperm. The cause of this spermatogenesis defect can be:
- hormonal, with hypogonadism (absence or abnormality in the secretion of sex hormones) which may be congenital (Kallmann-Morsier syndrome for example) or acquired, due in particular to pituitary tumors which alter the functioning of the hypothalamic-pituitary axis or after a treatment (eg chemotherapy);
- genetics: Klinefelter syndrome (presence of an extra X chromosome), which affects 1 in 1,200 men (2), structural abnormality of chromosomes, (microdeletion, i.e. loss of a fragment, of the Y chromosome in particular), translocation (one segment of the chromosome detaches and attaches to another). These chromosomal abnormalities are the cause of 5.8% of male infertility problems (3);
- bilateral cryptorchidism: the two testes have not descended into the bursa, which impairs the process of spermatogenesis;
- infection: prostatitis, orchitis.
Obstructive or excretory azoospermia (OA, obstructive azoospermia)
The testes do indeed produce sperm but they cannot be exteriorized due to a blockage of the ducts (epididymis, vas deferens or ejaculatory ducts). The cause may be of origin:
- congenital: the seminal tract has been altered from embryogenesis, resulting in an absence of the vas deferens. In men with cystic fibrosis, a mutation in the CFTR gene can cause the absence of vas deferens;
- infectious: the passages have been blocked following an infection (epididymitis, prostato-vesiculitis, prostatic utricle).
1-Pre-testicular causes
In this case, the origin of azoospermia is due to alterations at the endocrine level, that is, it is manifested by irregularities in the levels of the hormones responsible for regulating sperm production or spermatogenesis. . These are therefore cases of secretory azoospermia.
Among the main endocrine disorders that can cause azoospermia, we can find:
- Hypogonadotropic hypogonadism: this is a deficiency of the hormones released by the pituitary gland and responsible for stimulating the production of sperm in the testes. The main hormones are FSH (follicular stimulation) and LH (luteinizing). This problem can be due to genetic alterations such as Kallmann syndrome, tumors, trauma, pharmacological treatments, consumption of anabolic agents, etc.
- Hyperprolactinemia: it is the excessive increase in the hormone prolactin release. It blocks the hormone GnRH (a hormone that releases gonadotropins), whose function is to regulate the release of FSH and LH. This can be due to the consumption of antihypertensive drugs, stress, tumors, antidepressants, etc.
- Androgen insensitivity syndrome: this is mainly due to genetic mutations that cause resistance to androgens so that full virilization of the patient does not take place. Depending on the degree of severity, testosterone levels can be low, which prevents or hinders spermatogenesis, among other related consequences.
Patients who suffer from azoospermia due to this syndrome will have slightly decreased testicular volume, they will not produce sperm in the testes, and their FSH levels will generally below, except in cases of androgen resistance. In this case, the LH is elevated but the FSH and testosterone concentrations are usually normal or slightly elevated.
Testicular causes
The absence of sperm is due to problems in the testis which hamper spermatogenesis and therefore lead to errors or even blockage of sperm production.
The most common testicular pathologies are:
- Varicocele: dilation of the spermatic veins.
- Cryptorchidism: no descent of the testis from the inguinal canal to the scrotal pocket.
- Orchitis: Inflammation of the testicle, usually due to infection, as is often the case with mumps.
- Genetic alterations
- Testicular torsion
- Trauma
- Continuous increase in testicular temperature
The type of azoospermia from which these patients suffer is also secretory, but the clinical picture is different from the previous one: they have a lower testicular volume (due to non-production of sperm) but the FSH levels are high.
FSH, which is responsible for stimulating the testes to produce sperm, increases. This is why the testes do not respond to their stimulus, the body sends more FSH for the testes to function.
Post-testicular causes
When the cause of azoospermia is post-testicular, it is obstructive azoospermia. In this case, the testes are able to produce sperm properly, but there is a problem in the seminal ducts (vas deferens, epididymis or urethra) responsible for transporting sperm in an ejaculation.
Among these problems, we can highlight:
- Absence of vas deferens: this is a congenital pathology which, if it affects bilaterally, prevents sperm from coming out during ejaculate. This happens, for example, in some cases of cystic fibrosis.
- Obstruction of the vas deferens, the epididymis, or the urethra: it may be involuntary (trauma, surgery or disease) or voluntary. This is called a vasectomy.
Patients have a normal testicular size and FSH hormone levels are also average. Obstructive azoospermia is the least serious compared to fertility. It allows the man to obtain a pregnancy, either naturally, by a medical intervention which makes it possible to unblock the channels, or by obtaining sperm directly from the testicle and the subsequent application of a medically assisted procreation technique.
Your frequently asked questions
Is varicocele a cause of infertility in men?
By Victoria Moliner (embryologist).
Yes, varicocele can be a cause of male infertility. This pathology can manifest itself in different degrees of affection, so its harmful effect on male fertility (which mainly causes seminal and hormonal changes) can also be from mild to severe.
Is hormonal azoospermia always secretory?
By Andrea Rodrigo (embryologist).
Yes, when the lack of sperm is caused by hormonal problems, it is secretory azoospermia because of the lack of regulation by hormones prevents or complicates spermatogenesis.
Can cycling be the cause of my testicular factor azoospermia?
By Andrea Rodrigo (embryologist).
Continued use of the bicycle does not necessarily cause azoospermia, provided that the correct position is taken on the bicycle and, in some cases, certain testicular protection systems are used.
Routine improper use of the bicycle can increase the temperature of the scrotal region and thus prevent the proper production of sperm, which can reduce the quality of sperm.
As an added note, it is important to note that excessive exercise can affect sperm production in addition to other bodily functions.
Is azoospermia reversible?
By Andrea Rodrigo (embryologist).
It is possible that azoospermia is transient or punctual and, therefore, we can speak of reversible azoospermia. This means that, although it is unusual, a man may have a certain period of azoospermia, for example, due to stress or some other situation, and after this period recover the production of sperm and, with it, the presence of these in the ejaculate.
Read more
Why is there an absence of sperm in the spermogram?
By Zaira Salvador (embryologist).
When a man gets zero sperm as a result of his semen analysis, he may have azoospermia. First of all, this diagnosis should always be confirmed by a second spermogram, in case an error may have occurred while handling the first sample.
If azoospermia is confirmed, there are several causes of this seminal alteration, from blockage of the seminal ducts to problems with sperm production. More human testing should be done to find a more complete diagnosis.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Epididymis cyst: causes, symptoms, natural remedies and advice
The epididymis (from the Greek epididumis) is an organ of the male reproductive system located in the wall of the testicle.
The epididymis cyst or also called testicular cyst or spermatocele. Develops at the expense of the swollen part of the upper part or head of the epididymis. There may be one or more cysts within the same epididymis. Epididymal cysts can occur at any age. The epididymis is located in the wall of the testicle and is essential for the maturation and transport of sperm. Relatively frequent, these cysts are sometimes very painful and require an intervention.
However, the experts of Dawasanté provide you with a natural treatment based on medicinal plant to cure definitively the cysts of the epididymis without surgery. Click on the image below to discover this natural treatment.

The testicular cyst in men is a benign neoplasm.
The appendix itself is a long, narrow canal that serves to develop, accumulate and promote sperm. It also produces the fluid necessary for the maturation and motor activity of male sex cells. Under normal conditions, should be emptied regularly exit channels of male sperm in good body health, but under certain violations of the dander filled with sperm, and it appears cystic formation with capsular connective tissue sheath.
Further increase in the cyst causes excessive pressure on the vas deferens of the epididymis, which leads to disruption of the normal flow of seminal fluid. This can cause a breakdown in reproductive function in men.
Epididymal cysts usually originate in adolescence, progressing and developing over time. The peak of development occurs at the age of 30 to 40 years and by the age of 50 years, a full clinical picture of the disease has been observed, which can affect about 30% of the total male population. It is often caused by a sexually transmitted infection (STI) but can also have other causes
We have a very effective natural treatment to cure epididymal cysts permanently.
Order it and start the natural Epididymal Cyst treatment early. Support is offered during the whole period of its intake. To reach us, click on the WhatsApp button in the right corner of your screen or contact us at +229 66 23 89 56
We have representation in all African countries and actively in the following countries: Cameroon, Ivory Coast, Mali, Senegal, Burkina Faso, Togo, Kenya, Nigeria, Gabon, Central African Republic, Benin, Chad, Congo-Brazzaville and Kinshasa. So rest assured that you will receive your products immediately after your order.
Delivery is free of charge anywhere in the world.
Causes of the epididymis cyst
There are several reasons and options for the development of epididymis cysts:
Epididymis cyst may form before birth, as a result of some defects in the period of intra-uterine growth of the embryo (for example, non-infection of the parameconephrotic canal). Cysts of this type contain a sperm-free fluid in their cavity;
The formation of epididymis cysts in 40% of cases can be preceded by scrotal traumatic lesions, infectious and inflammatory processes in the genital region, which lead to the coalescence of one or two deferential ducts. As a result, the output of seminal fluid overlaps, and the accumulation of male sex cells in the channel light. The walls of the canal, respectively, are stretched and a cyst is formed, containing in its cavity seminal fluid accumulated with neutral or alkaline activity.
In addition to sperm, lipid cells, leukocytes and epithelial particles can be found in the contents of the cyst, from which the walls of the cystic cavity are aligned.
- Ethnic and socio-economic causes:
Several studies have shown the impact of these factors in the occurrence of MIT, without showing the causal link. Predominance in black males, and low socioeconomic status was observed.
- Genetic Causes:
Several genes are implicated in the occurrence of MIT: +Senseless mutation of the gene Phosphodiesterase 11A(PDE11A) which encodes a protein that plays a role in regulating the intracellular concentration of cAMP and cGMP. [34] + other mutations of other genes have been identified including the mutation of the gene SLC34A2 and GALNT3, both encode a protein involved in phosphate transport and metabolism
- Family history of first degree.
Other contributing factors are discussed such as certain environmental factors such as maternal estrogen intake during pregnancy, exposure to certain chemical industry substances, or to certain substances in the environment (insecticides, herbicides).
- Atypical acute scholarship:
The problem arises in a young man with an acute sore bursa, but without the clinical signs characteristic of a twisted spermatic cord or an orchi-epididymitis. This is the problem of differential diagnosis with a germinal tumor with acute revelation (about 10% of testicular tumors).
- Important risk factors include:
Factors that increase the risk of testicular cyst vary due to various causes of testicular abnormalities. History of testicular cancer or contralateral intratubular germinal neoplasia.
The presence of gonadal dysgenesia syndrome associating more or less:
a history of cryptorchidia (homo- or contralateral). Present in almost 10% of cases, it multiplies the cancer risk by 5 to 10 times depending on the age and date of treatment. Surgical testicular lowering, if it does not reduce the risk of cancer, has the advantage of facilitating testicular palpation;
. testicular atrophy;
. a hypospade;
. Fertility problems.
. Klinefelter syndrome.
. Infertility.
Testis not lowered or retracted
An undrawn testicle does not leave the abdomen and does not enter the scrotum during fetal development or early childhood. A retractable testicle descends into the scrotum but withdraws into the abdomen. Either may increase the risk of:
- Inguinal hernia
- Testicular torsion
- Testicular cancer
- Anomalies present at birth
- Abnormalities of the testicles, penis or kidneys present at birth (congenital) could increase the risk of scrotal mass and testicular cancer later in life.
Symptoms of epididymis cysts
Epididymal cysts usually have no symptoms before forming in the epididymis. Once formed, you may notice a ball the size of a pea (or larger) behind, above or below one of your testicles where sperm is produced. For spermatoceles, the cyst is usually on the top of the testicles.
Other symptoms of an epididymal cyst may include:
- Dull pain in the scrotum (the pocket containing the testicles)
- A feeling of heaviness in the scrotum
- Redness in the region of the scrotum
- Increased pressure at the bottom of the penis
- Sensitive or swollen epididymis
- Soft, swollen or hardened testicles
- Pain in the groin or lower back and abdomen
Epididymal cysts generally do not present acute and intense pain symptoms and are generally completely painless. If any of the above symptoms occur, a complete and immediate examination by a urologist is warranted.
We have a very effective natural treatment to cure epididymal cysts permanently.
Order it and start the natural Epididymal Cyst treatment early. Support is offered during the whole period of its intake. To reach us, click on the WhatsApp button in the right corner of your screen or contact us at +229 66 23 89 56
We have representation in all African countries and actively in the following countries: Cameroon, Ivory Coast, Mali, Senegal, Burkina Faso, Togo, Kenya, Nigeria, Gabon, Central African Republic, Benin, Chad, Congo-Brazzaville and Kinshasa. So rest assured that you will receive your products immediately after your order.
Delivery is free of charge anywhere in the world.
NATURAL REMEDIES FOR THE EPIDIDYMIS CYST
- Amanita
 You can get rid of the pathology without surgery with the help of Amanita. To dye, you must take fresh mushrooms, clean well so that there is no dirt and forest debris, and put it in a pot to the brim. Pour alcohol on the edges – at least 70%. In extreme cases, you can use regular vodka. After the container is closed and put in a dark place for a period of at least fourteen days. Insist until the liquid acquires a characteristic red-brown hue and a particular smell. As soon as the desired effect is achieved, the dye must be filtered and the resulting liquid poured into bottles.
You can get rid of the pathology without surgery with the help of Amanita. To dye, you must take fresh mushrooms, clean well so that there is no dirt and forest debris, and put it in a pot to the brim. Pour alcohol on the edges – at least 70%. In extreme cases, you can use regular vodka. After the container is closed and put in a dark place for a period of at least fourteen days. Insist until the liquid acquires a characteristic red-brown hue and a particular smell. As soon as the desired effect is achieved, the dye must be filtered and the resulting liquid poured into bottles.
To cure spermatocele in men, it is necessary to follow a certain pattern of consumption of dye, which first increases and then decreases. That is to say, on the first day of administration – 1 drop, the second – 2 and so on up to 15 drops in one dose, then, on the contrary, from 15 drops a day to one at the end. Thus, the duration of treatment should be 30 days.
- Quercetin
 Quercetin can also help fight inflammation associated with the epididymis cyst.
Quercetin can also help fight inflammation associated with the epididymis cyst.
- Arnica Mountain
 Another equally effective alternative therapy method is to add the mountain arnica flowers to a glass of boiling water. Let stand for 2 hours. You should drink 1 tablespoon daily three times a day, but only after eating.
Another equally effective alternative therapy method is to add the mountain arnica flowers to a glass of boiling water. Let stand for 2 hours. You should drink 1 tablespoon daily three times a day, but only after eating.
- Turmeric and Curcumin
 Turmeric and curcumin can help reduce inflammation and can be useful for men with epididymis. Curcumin can be a great help in reducing chronic inflammation, which is good for epididymitis.
Turmeric and curcumin can help reduce inflammation and can be useful for men with epididymis. Curcumin can be a great help in reducing chronic inflammation, which is good for epididymitis.
- Jasmine
 You can also treat a cyst with jasmine. To do this, prepare the ointment. About fifty grams of the plant’s flowers are taken; placed in a bowl and poured with a glass of oil on top (it is best to use olive oil). The mixture must be well infused, so you must wait at least ten days before using the ointment. After this time, the mass must be filtered, after which you can use the tool; it is rubbed daily at the site of localization of the cyst, mainly in the morning. This treatment method works well when combined with other popular remedies; for example, decoctions, dyes, etc.
You can also treat a cyst with jasmine. To do this, prepare the ointment. About fifty grams of the plant’s flowers are taken; placed in a bowl and poured with a glass of oil on top (it is best to use olive oil). The mixture must be well infused, so you must wait at least ten days before using the ointment. After this time, the mass must be filtered, after which you can use the tool; it is rubbed daily at the site of localization of the cyst, mainly in the morning. This treatment method works well when combined with other popular remedies; for example, decoctions, dyes, etc.
We have a very effective natural treatment to cure epididymal cysts permanently.
Order it and start the natural Epididymal Cyst treatment early. Support is offered during the whole period of its intake. To reach us, click on the WhatsApp button in the right corner of your screen or contact us at +229 66 23 89 56
We have representation in all African countries and actively in the following countries: Cameroon, Ivory Coast, Mali, Senegal, Burkina Faso, Togo, Kenya, Nigeria, Gabon, Central African Republic, Benin, Chad, Congo-Brazzaville and Kinshasa. So rest assured that you will receive your products immediately after your order.
Delivery is free of charge anywhere in the world.
- The buchu leaf
 The buchu leaf is also good for treatment as it is a disinfectant and diuretic of the urinary tract. It is used to treat prostate inflammation and urinary tract infections.
The buchu leaf is also good for treatment as it is a disinfectant and diuretic of the urinary tract. It is used to treat prostate inflammation and urinary tract infections.
- Chestnut
 In addition, for the treatment of the pathology, the chestnut juice of the plant flowers is perfect. It is necessary to collect fresh flowers; to squeeze all the juice and to consume 20 drops a day, previously diluted with water.
In addition, for the treatment of the pathology, the chestnut juice of the plant flowers is perfect. It is necessary to collect fresh flowers; to squeeze all the juice and to consume 20 drops a day, previously diluted with water.
- Traditional plantain seed recipes
 The healing properties of plantain are thought to help restore male strength. They will also help get rid of the symptoms and cyst of the testicles.
The healing properties of plantain are thought to help restore male strength. They will also help get rid of the symptoms and cyst of the testicles.
- Flax
 You can also cure the pathology using flax grass. It is necessary to take flax, to press the juice, to add butter (the ratio of the proportions must be of 2: 5) and to light a small fire. The mixture should languish until all the excess liquid has completely evaporated. Use the ointment after it has completely cooled and infused. It is applied as a cream on the testic
You can also cure the pathology using flax grass. It is necessary to take flax, to press the juice, to add butter (the ratio of the proportions must be of 2: 5) and to light a small fire. The mixture should languish until all the excess liquid has completely evaporated. Use the ointment after it has completely cooled and infused. It is applied as a cream on the testic
- Corn silk
 Corn silk is also an excellent herbal remedy for the treatment of epididymis cyst, as it is a powerful antibacterial that also helps to relieve pain.
Corn silk is also an excellent herbal remedy for the treatment of epididymis cyst, as it is a powerful antibacterial that also helps to relieve pain.
We have a very effective natural treatment to cure epididymal cysts permanently.
Order it and start the natural Epididymal Cyst treatment early. Support is offered during the whole period of its intake. To reach us, click on the WhatsApp button in the right corner of your screen or contact us at +229 66 23 89 56
We have representation in all African countries and actively in the following countries: Cameroon, Ivory Coast, Mali, Senegal, Burkina Faso, Togo, Kenya, Nigeria, Gabon, Central African Republic, Benin, Chad, Congo-Brazzaville and Kinshasa. So rest assured that you will receive your products immediately after your order.
Delivery is free of charge anywhere in the world.
- The Goldenseal of Canada
 The Canadian goldenseal is an antibacterial and anti-inflammatory drug used by many in conjunction with other herbs to combat prostatitis. It also fights urinary tract infections.
The Canadian goldenseal is an antibacterial and anti-inflammatory drug used by many in conjunction with other herbs to combat prostatitis. It also fights urinary tract infections.
- Ginger
 Ginger fights prostate cancer cells and can therefore be added to any diet.
Ginger fights prostate cancer cells and can therefore be added to any diet.
- The root of hydrangea
 Hydrangea root is also used as an herbal remedy to promote treatment and relieve symptoms of bladder, prostate and other urinary tract infections, including benign prostate hypertrophy and urethritis.
Hydrangea root is also used as an herbal remedy to promote treatment and relieve symptoms of bladder, prostate and other urinary tract infections, including benign prostate hypertrophy and urethritis.
- The rutin
 Rutin is a flavonoid that reduces inflammation
Rutin is a flavonoid that reduces inflammation
- Extract of juniper berries
 Juniper berry extract excels in urinary tract evacuation, which is very important in case of prostatic hypertrophy. It also helps treat urinary tract infections and prostate infections by activating and cleaning the entire system.
Juniper berry extract excels in urinary tract evacuation, which is very important in case of prostatic hypertrophy. It also helps treat urinary tract infections and prostate infections by activating and cleaning the entire system.
We have a very effective natural treatment to cure epididymal cysts permanently.
Order it and start the natural Epididymal Cyst treatment early. Support is offered during the whole period of its intake. To reach us, click on the WhatsApp button in the right corner of your screen or contact us at +229 66 23 89 56
We have representation in all African countries and actively in the following countries: Cameroon, Ivory Coast, Mali, Senegal, Burkina Faso, Togo, Kenya, Nigeria, Gabon, Central African Republic, Benin, Chad, Congo-Brazzaville and Kinshasa. So rest assured that you will receive your products immediately after your order.
Delivery is free of charge anywhere in the world.
- Dandelion root
 Dandelion root has anti-inflammatory properties that reduce inflammation.
Dandelion root has anti-inflammatory properties that reduce inflammation.
- Parsley
 Parsley is a powerful antioxidant and anti-inflammatory.
Parsley is a powerful antioxidant and anti-inflammatory.
Some tips to relieve and avoid Epididymis cyst
What to do to relieve the epididymis cyst
- Get some rest in bed.
- Lie down so that your scrotum is raised.
- Apply cold compresses to your scrotum if tolerated.
- Wear an athletic support.
- Avoid lifting heavy objects.
- Avoid intercourse until the infection is gone.
Foods to avoid in case of epididymitis
When it comes to eating well to promote healing and relieve the pain of epididymitis and strengthen the health of the testicles, there are certain foods you should avoid.
In general, these are mainly high-fat foods, processed foods, sweet foods and spicy foods. The reason is that these foods feed inflammation.
Foods of the epididymitis to be avoided or restricted include: sugary foods, sweets and artificial sweeteners; caffeine; alcohol; processed foods; white flour products; fast foods; hydrogenated foods, trans fats, Fried foods, fatty foods; margarine; sodas; spicy foods; onions, pepper, mustard, fennel
Foods to eat in case of epididymitis
When it comes to following a diet adapted to the health of the testicles, you should consume foods that fight and reduce inflammation and avoid eating pro-inflammatory foods.
These foods are:
Anti-inflammatory foods for the testicles: Epinards; Blueberries; Strawberries and other flavonoid-rich foods
Foods rich in vitamin C for testicular health: Kiwi; Orange; Watermelon; Lemon; Grapefruit; Bitter melon; Tomatoes
Fiber-rich foods for the testicles: Banana; Sweet potatoes; Celery
Whole grains, nuts, beans and seeds: Walnuts; Flax seeds; Pumpkin seeds
Foods rich in omega-3 fats: Salmon; Mackerel; Herring; Sardine; Rapeseed oil; Fish oil
We have a very effective natural treatment to cure epididymal cysts permanently.
Order it and start the natural Epididymal Cyst treatment early. Support is offered during the whole period of its intake. To reach us, click on the WhatsApp button in the right corner of your screen or contact us at +229 66 23 89 56
We have representation in all African countries and actively in the following countries: Cameroon, Ivory Coast, Mali, Senegal, Burkina Faso, Togo, Kenya, Nigeria, Gabon, Central African Republic, Benin, Chad, Congo-Brazzaville and Kinshasa. So rest assured that you will receive your products immediately after your order.
Delivery is free of charge anywhere in the world.
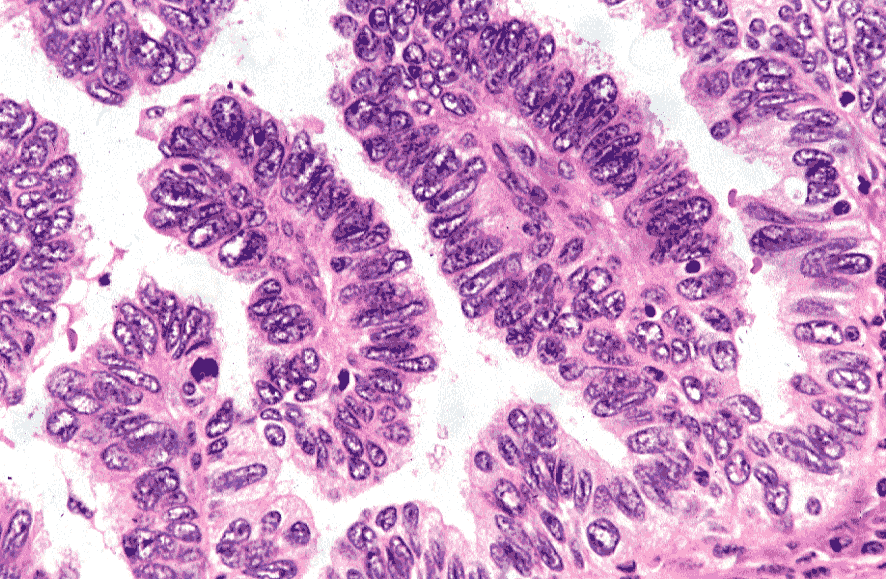
CAUSES OF VERGE ADENOCARCINOMA: NATURAL TREATMENT
CAUSES ADENOCARCINOMA THE VERGE: NATURAL TREATMENT
The adenocarcinoma verge or penile cancer is a disease in which malignant (cancer) cells form in the tissues of the penis.
Adenocarcinoma of the penis or cancer of the penis is usually found on the glans or foreskin of the penis, but can also occur on the shaft of the penis. Almost all penile cancers start in the skin of the penis.
The cancer of the penis or the penis is rare cancer in France.
But before going any further in our writing, and in case you are concerned by this condition and want to avoid surgery at all costs, the health experts at DAWABIO after much research offer you a very effective solution based on herbal remedies for adenocarcinoma of the penis or cancer of the penis. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Different types of cancer
Penile cancer can develop at the expense of the skin or the internal tissues of the penis: it is called squamous cell carcinoma.
More rarely, it can be low cell carcinoma, melanoma.
Causes of adenocarcinoma of the penis
Certain factors predispose to the development of penile cancer or adenocarcinoma of the penis :
The lack of hygiene, aggravated by the existence of phimosis (affection of the penis) preventing any removal of coring, increases the risk of penile cancer. "Indeed, microbial development can lead to inflammation involved in the development of cancer, explains Dr. Ludovic Ferretti, member of the committee of andrology and sexual medicine of the French Association of Urology. Thus, we recommend a classic cleaning to water and soap after scalping (without forcing), then drying. And after urinating, wipe the glans well so as not to let acid urine infiltrate under the foreskin, which would promote inflammation.
· Phimosis (phimosis corresponds to a narrowing of the tip of the foreskin which prevents pull the foreskin);
· Dermatological disease of the glans or the foreskin which can become secondarily cancerous, like a mole for example;
The causes and risk factors of developing penile cancer include the infection with the human papillomavirus ( HPV )
The use of regular hygiene care, with systematic removal of the cores, remains the best prevention.
The dupenis cancer or carcinoma of the penis is a disease in which malignant (cancer) cells form in the tissues of the penis.
The penis is a rod-shaped male reproductive organ that transmits semen and urine from the body. It contains two types of erectile tissue (spongy tissue with blood vessels that fill with blood to make an erection):
Corpora cavernosa: The two columns of erectile tissue that make up most of the penis.
Corpus spongiosum: The single column of erectile tissue that forms a small part of the penis. The spongy body surrounds the urethra (the tube through which urine and sperm pass from the body).
Erectile tissue is wrapped in connective tissue and covered with skin. The glans (head of the penis) is covered with loose skin called the foreskin.
Infection with human papillomavirus can increase the risk of developing penile cancer.
Anything that increases your chances of getting a disease is called a risk factor. Having a risk factor doesn't mean you'll get cancer; not having risk factors doesn't mean you won't get cancer. Talk to your doctor if you think you are at risk. The risk factors for penile cancer or adenocarcinoma of the penis are as follows:
Circumcision can help prevent infection with the human papillomavirus ( HPV ). A circumcision is an operation in which the doctor removes part or all of the foreskin from the penis. Many boys are circumcised soon after birth. Men who were not circumcised at birth may have a higher risk of developing penile cancer.
The other risk factors for penile cancer are:
Be 60 years of age or older.
Have phimosis (a condition in which the foreskin of the penis cannot be pulled over the glans).
Have poor personal hygiene.
Having many sexual partners.
Use of tobacco products.
Symptoms
Changes in the skin of the penis are the most common symptom of penile cancer. They can appear on the foreskin of uncircumcised men, or on the tip of the penis (the glans) or the shaft.
Warning signs of the disease may include:
- Changes in skin thickness or color on the penis
- A bump on it
- A rash or small “crusty” bumps on it; it may look like an unhealed scab.
- Growths on the penis that appear bluish-brown
- A smelly discharge under the foreskin
- A sore on the penis, which may bleed
- Swelling at the tip of the penis
- Lumps under the skin in the groin area
Most men with these symptoms do not have penile cancer. Rather, it is an infection or an allergic reaction. Nonetheless, it's important to check for any unusual symptoms on or near your penis immediately. Early treatment is preferable.
Men at risk
There is convincing evidence that there are certain factors that increase the risk of penile cancer. Among them :
Chronic inflammation of the penis due to poor genital hygiene;
Human papillomavirus ( HPV ) infection ;
A narrowing of the foreskin, also called phimosis: this condition prevents the foreskin from retracting to reveal the glans, which makes genital hygiene more difficult and may mask a skin lesion;
· Smoking;
Precancerous lesions such as Queyrat erythroplakia or Bowen's disease.
Signs of penile cancer include sores, discharge, and bleeding.
These signs and others can be caused by penile cancer or adenocarcinoma of the penis or by other conditions. Check with your doctor if you have any of the following:
Redness, irritation or sore on the penis.
A lump on the penis.
Penile cancer and circumcision
In contrast, a circumcision performed in childhood provides some protection against cancer of the penis. HPV vaccination can also decrease the risk of developing the disease.
Usually, follow-up visits are first semiannual and then decrease in frequency over time. The duration of follow-up is in all cases a minimum of 5 years because 90% of recurrences are in the first 5 years, 75% of which are in the first 2 years.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.