natural remedy to unblock the tubes
Blog / 307 results found
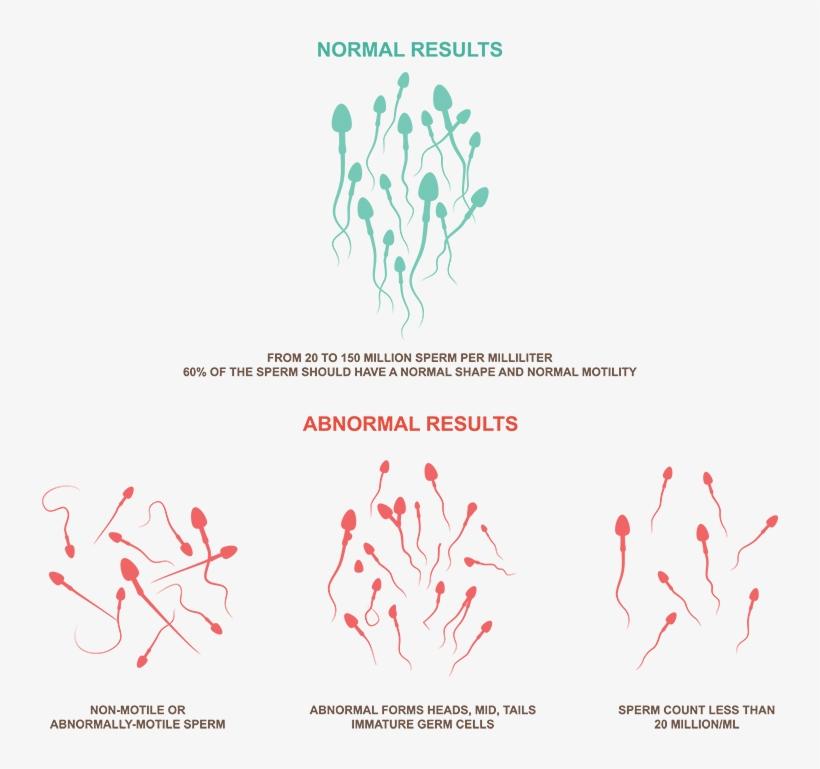
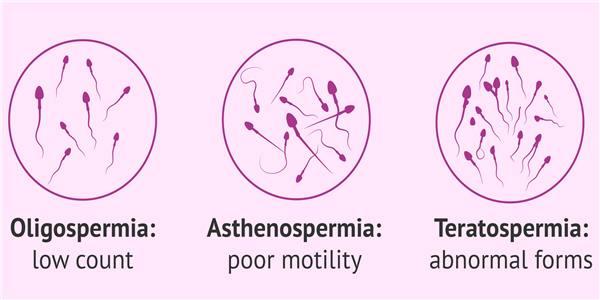
TYPES OF TERATOSPERMIA: mild, moderate, and severe
The teratospermia (or teratozoospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. This is how the Dawasanté experts provide you with a natural treatment to treat all your fertility problems related to the quality and quantity of your sperm.
Click HERE or on the image below to discover this natural treatment
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Teratozoospermia or teratospermia is a seminal alteration that involves a high percentage of abnormally shaped sperm.
It is a cause of male infertility, the severity of which will depend on the greater or lesser number of amorphous sperm cells in the semen.
According to the different criteria used to assess the degree of teratozoospermia, we can distinguish 3 types: mild, moderate, or severe.
1-Classification of teratozoospermia
When a man performs a spermogram to assess the quality of his sperm, in the results report, he will obtain the values of all seminal parameters, including sperm morphology.
A man is considered to have teratozoospermia when the percentage of sperm with normal morphology in his seminogram is less than 4%, according to criteria established by the World Health Organization (WHO) in 2010.
On the other hand, some labs also use Kruger's strict criteria to diagnose teratozoospermia. According to Kruger, a man suffers from teratozoospermia when less than 15% of his sperm has a normal form.
Percentage of normal sperm
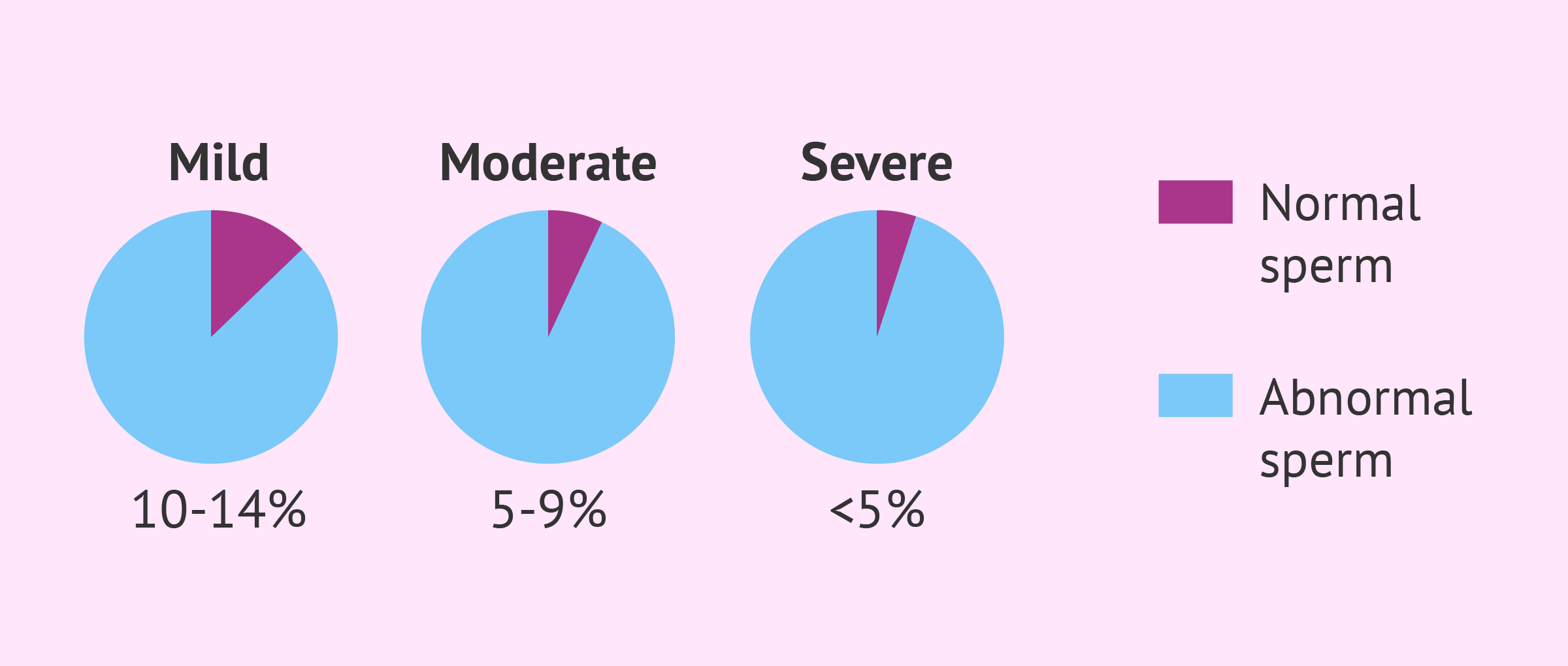
Since the WHO benchmark is so low, there is no point in talking about types of teratozoospermia based on the number of normal sperm. Therefore, for the classification of spermatozoa in this sense, it is better to use Kruger's criterion, which is stricter than the previous one.
1-1 Mild teratozoospermia
A man suffers from mild teratozoospermia when the number of normal sperm in his spermogram ranges from 14% to 10%.
The rest of the sperm will have an abnormality in their head, neck or tail. Despite this, men with mild teratospermia do not have a bad prognosis for having children.
If assisted reproduction techniques are necessary to achieve pregnancy, artificial insemination (AI) and in vitro fertilization ( IVF ) may be performed, depending on the concentration and mobility of the sperm.
The shape of the sperm is important for the fertilization of the egg. However, men with mild teratozoospermia can achieve a natural pregnancy.
In addition, there are various dietary supplements that contain vitamins and antioxidants that help in the maturation of sperm and can improve their morphology.
If you are interested in this topic, you can read the following article: Treatment of teratozoospermia.
1-2 Moderate teratozoospermia
Moderate or severe teratozoospermia is diagnosed when sperm results show that only 9-5% of sperm have a normal shape.
With this diagnosis, it is quite complicated to have children naturally. To achieve a pregnancy with moderate teratozoospermia, an in vitro fertilization technique such as ICSI will most likely be necessary.
The ICSI (Intracytoplasmic Sperm Injection) is based on the selection of spermatozoa under a microscope and their direct injection into each egg and fertilization.
PMA, like any medical treatment, requires that you trust the professionalism of the doctors and clinic you have chosen. Obviously, not all are the same. The Fertility Report selects the most advantageous clinics for you based on our rigorous quality criteria. In addition, the system performs a comparison of prices and conditions offered by different clinics to facilitate your decision making.
1-3 Severe teratozoospermia
When the spermogram morphology test shows a normal sperm value of less than 5%, the man has severe or severe teratozoospermia.
Sperm with good morphology is therefore very few in number and, therefore, the possibility of achieving natural pregnancy is very low.
Spermatozoa with alterations in their morphology have problems progressing gradually, they have more difficulty reaching the egg, penetrating its thick pellucid layer and also fusing its male nucleus with the female one. The consequence of all this is that they can lead to fertilization failures.
Teratozoospermia and fertilization failure

The most suitable assisted reproduction technique for extreme teratozoospermia is ICSI or its improved variant: IMSI.
The IMSI is the same as intracytoplasmic sperm injection, but with the use of a microscope magnification of 6300, so it is possible to get very close to the sperm morphology and make a better selection.
2-Your frequently asked questions
2-1 Can we cure severe teratozoospermia?
If a man has less than 5% of sperm with normal morphology, it is very difficult to regain a normal value with natural or pharmacological treatment. Improvement can be seen over time, especially if the man maintains a healthy lifestyle.
On the other hand, if the teratozoospermia appears associated with another pathology such as, for example, varicocele, it is possible that the spermogram improves its parameters during a surgical intervention to eliminate the varicocele.
2-2 What is isolated teratozoospermia?
Discrete teratozoospermia means that the affected parameter, in this case, the morphology of the sperm, does not have a value much lower than the reference value. Therefore, it would be a mild teratozoospermia.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
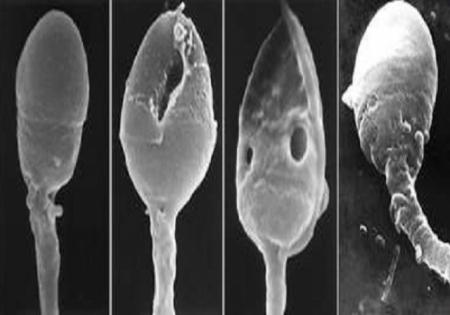
THE CAUSES OF TERATOSPERMIA: Natural treatment
The teratospermia (or teratozoospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. Dawasanté experts advise you to opt for a natural treatment without operation, against teratospermia.
Click HERE or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Teratozoospermia refers to the poor morphology of the sperm in a man's ejaculated semen.
These men have lower seminal quality and sometimes suffer from infertility and difficulty achieving pregnancy.
The causes of teratozoospermia are mostly unknown. However, we are going to address the possible alterations caused by these abnormal sperms in semen.
1-Defects in spermatogenesis
Most experts agree that the morphological changes in sperm occur during the last phase of their formation.
The spermatogenesis is the process by which sperm are formed in the testicles, which lasts about 3 months.
More precisely, spermiogenesis is the last phase of spermatogenesis, during which the spermatozoa, which already have their genetic content formed, undergo a process of maturation and acquire their characteristic morphology.
Once the sperm have their oval head and tail formed, they are released into the seminiferous tubules to follow their path.
Therefore, it is not surprising that any abnormality or alteration in spermiogenesis results in abnormalities in the head, neck or tail.
2-Reversible teratospermia
Teratozoospermia can be reversible or irreversible depending on the specific cause.
With reversible teratospermia, men can regain their seminal quality after a few months if they have received the appropriate treatment.
To check this, it is necessary to do another spermogram and compare it with the previous one.
We will now discuss the possible causes of reversible teratozoospermia:
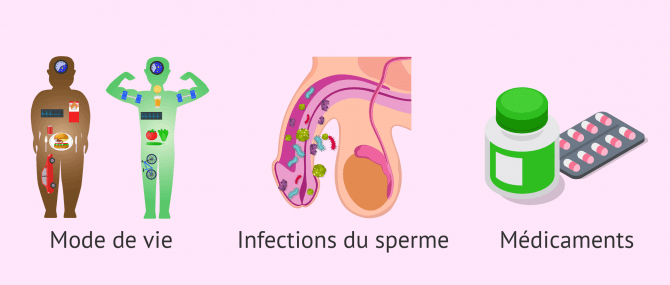
2-1 Way of life
Although it may seem surprising, the lifestyle of men greatly affects the quality of their semen.
During times of stress and anxiety, sperm morphology may deteriorate, as many other parameters such as concentration and mobility.
The abuse of alcohol, tobacco, or other drugs are also factors linked to alterations in sperm.
Prolonged exposure to testicular heat affects spermatogenesis. Therefore, the bad habit of placing the computer on your legs, wearing tight clothes, or driving for a long time can cause teratozoospermia.
Testicular heat causes teratozoospermia

Finally, diet and sport also contribute to male fertility.
Men who are planning to become pregnant with their partner are recommended to maintain a good lifestyle, eat a balanced diet, exercise regularly and not consume substances that are harmful to the body.
2-2 Seminal infections
Semen infections refer to the invasion of microorganisms, bacteria, and viruses, into the male reproductive system.
Its presence is found in urine and semen, causing alterations in the sperm, as well as inflammation and obstruction of the seminal ducts.
The most common bacterial infections in the testes are chlamydia and gonorrhea. These infections can be fought with antibiotics and male fertility can be restored. If you would like more information on this, you can access the following article: Types of infections in seminal fluid.
The episodes of fever caused by flu or another disease may also occasionally affect sperm quality.
2-3 Pharmaceuticals
Sex hormones like testosterone, LH, FSH and inhibin have a very important role in the regulation of spermatogenesis.
Therefore, any drug that changes the appropriate levels of these hormones or affects their secretion by the brain has negative consequences for sperm production.
As we have already said, the alteration of the phase of spermiogenesis prevents the correct maturation of sperm and causes teratozoospermia.
Reversible causes of teratozoospermia
3-Irreversible teratospermia
If a man with teratozoospermia fails to improve his second spermogram after receiving treatment, one may begin to suspect that the teratozoospermia is irreversible.
In these cases, the couple will have to resort to assisted reproduction if they want to become a parent because it will naturally be very difficult to obtain a pregnancy.
In addition, there are other pathologies or situations that cause irreversible or prolonged teratozoospermia. The most relevant cases are examined below:
3-1 Cancer treatment
Chemotherapy and radiation therapy alters both sperm stem cells and sperm production, causing severe teratozoospermia and other more serious changes.
For these reasons, all men with cancer are advised to save a semen sample if they wish to have children in the future after they have overcome the disease.
3-2 Genetic diseases
It is one of the most difficult causes of diagnosis. Normally, when it has not been possible to determine the pathology that causes teratozoospermia, it is attributed to a genetic factor.
Defects in the genes or chromosomes of the sperm are a serious problem because they cannot be corrected.
3-3 Associated pathologies
Teratozoospermia can also result from other diseases that mainly affect the testes, for example:
- Trauma or blows to the testicles, especially in childhood
- Testicular varicocele
- Meningitis
- Diabetic sugar
In addition to all this, the age of males can also affect the morphology of the sperm. In particular, it has been observed that men over 45 have a higher rate of abnormal sperm in their semen.
Irreversible causes of teratozoospermia

4-Your frequently asked questions
4-1 Can live sperm have poor morphology?
By Zaira Salvador (embryologist).
Yes, teratozoospermia can be present in both living and dead sperm.
Dead sperm do not always have a bad morphology. Sometimes they are confused with immobile sperm and it is necessary to make a tincture to find out whether they are viable or not.
4-2 Can leukospermia cause teratospermia and male infertility?
By Zaira Salvador (embryologist).
Leukospermia, also known as leukocytospermia, is the appearance of leukocytes in semen, with a concentration level greater than 1 million per milliliter. The cause of this seminal pathology is an infection of the male reproductive tract which must be treated with antibiotics as it can affect spermatogenesis and cause oligospermia or teratozoospermia.
You can find the information in our article: Leukocytes in semen.
4-3 Are the causes of teratozoospermia and asthenozoospermia the same?
By Zaira Salvador (embryologist).
In most cases, asthenospermia and teratospermia have the same causes. The two seminal parameters are usually changed in the seminogram, known as astenoteratozoospermia. However, this is not always the case.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
TERATOSPERMIA OR TERATOZOOSPERMIA: definition and treatment
Teratozoospermia or teratospermia is an alteration that occurs in men when more than 95% of their sperm have an abnormal morphology.
Therefore, teratospermia is considered a cause of male infertility due to a sperm factor, and its origin is varied and sometimes unrecognized. This is why the Dawasanté experts provide you with a natural treatment to improve the quality and quantity of your sperm; which will allow you to quickly conceive.
Click HERE or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number
There are several treatments to be able to conceive a child with sperm affected by teratospermia depending on whether the man's sperm has other spermatic disorders, such as, for example, sperm concentration or mobility.
1-Teratozoospermia: what is it?
Poor morphology of the spermatozoa, indeed the latter can present defects in the head, middle part or neck, or the tail.
The WHO estimates that a man with 4% sperm with a normal form (at least) does not have fertility problems. In lower quantity, we are talking about male infertility by teratospermia. This baseline changed in 2010, previously it was 14%, so it is possible that on other sites you will find that teratospermia is considered to be more than 85% abnormal.
According to the strict Kruger criterion, values equal to or greater than 15% of sperm with normal morphology are considered normal. This criterion is always stricter than that of the WHO, but the WHO is the one that is taken as a global reference.
The count of sperm of good or bad morphology is carried out through a medical examination called a spermogram, where the structure of the sperm is analyzed under a microscope.
There are several laboratories which in addition to the Kruger criteria, add those of the WHO.
If the medical report does not specify the details of the analysis to the laboratory, the parameters dictated by the WHO in 2010 are the reference values used.
Diagnosis of teratozoospermia

2-Causes
Teratozoospermia involves male infertility because the sperm that reach the oocyte are unable to fertilize it due to their poor morphology.
The causes that cause the existence of amorphous sperm in human semen are manifold and difficult to diagnose. Here they are:
- Genetic disorders
- Chemotherapy and radiotherapy
- Seminal infections and orchitis
- Varicocele and other testicular disorders
- Febrile period
- Diabetes or meningitis
- Tobacco, alcohol and drug abuse
- Poor lifestyle: poor diet, exposure to toxic substances, clothes that are too tight
Some of these factors can cause reversible teratozoospermia, which goes away with fever, infection, or periods of stress. In the same way, it is possible to recover a good spermatic morphology by improving one's lifestyle, diet, quitting smoking, etc.
3-Types
Sperm morphology defects are classified according to their position on the head, at the neck or at the tail. However, to diagnose teratospermia, all defects are taken into account.
Sperm is considered normal when it has a head with an oval shape and an acrosome inside. The neck or middle piece is slightly larger than the tail, and the tail is elongated and straight.
After analyzing the morphology of the sperm during the spermogram, it is possible to determine the degree of teratozoospermia depending on the seminal quality. For this, the laboratories use the Kruger criteria. Here is their classification:
- Mild teratozoospermia
- 10% to 14% of spermatozoa have normal morphology.
- Moderate teratozoospemia
- the percentage of normal sperm varies between 5% and 9%.
- Severe teratozoospemia
- less than 5% of sperm have normal morphology.
As we have commented before, it is the WHO criteria that are used to diagnose teratospermia, and therefore, this classification is obsolete. However, it is still possible to find it on some spermograms.

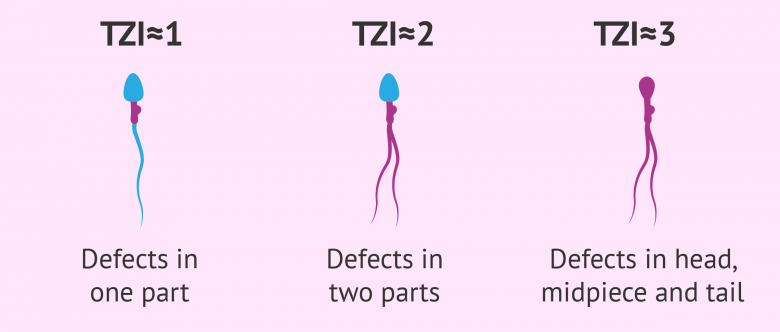
3-1 Teratozoospermia index
This seminal parameter is used to know the number of defects that each sperm has. It is possible that sperm has only one malformation, or several distributed over several parts.
In order to calculate the rate of teratospermia (TZI), we use the following formula: TZI = (c + p + q) / x , where each variable means:
- c = head malformations
- p = malformations of the middle part of neck
- q = tail malformations
- x = total number of abnormal sperm
The interpretation of these results is carried out as follows:
- TZI close to 1
- sperm with abnormalities in one area
- TZI close to 2
- spermatozoa with abnormalities in two areas
- TZI nearly 3
- sperm with defects on the head, neck and tail
It is important to note that the same seminal sample can present sperm of three types: one malformation, two, or three. The rate of teratospermia will indicate which type is most present.
4-Teratospermia and pregnancy
A man with teratospermia could have a natural pregnancy without problems if the rest of the seminal parameters such as concentration or mobility are not affected.
However, in cases where the pregnancy is delayed, it is possible to follow the doctor's recommendations to recover the correct sperm morphology.
On the other hand, if teratospermia has a genetic cause or is congenital, it is more difficult to find an effective treatment to cure it.
4-1 Natural treatments
First of all, men who suffer from teratospermia need to change their lifestyle and put aside bad habits like tobacco or alcohol.
A healthy and balanced diet always helps to recover some of the fertility. In concrete terms, foods rich in antioxidants and essential acids such as L-carnitine help improve sperm quality.
Oily fish is another product rich in omega 3 acids which bring great benefits to human reproductive health.
These nutritional contributions can also be taken by food supplements such as Andean maca or vitamin E supplements, a powerful antioxidant.
4-2 Assisted reproduction (ART)
In the case of fertility treatment to be able to achieve pregnancy and mild teratozoospermia, it is possible to perform artificial insemination (AI), if the concentration and mobility of the sperm allow it.
This is the first option to consider if the woman has no problems with fertility and the only cause of the lack of a pregnancy is teratozoospermia.
Faced with cases of moderate or severe teratospermia, it is necessary to do IVF - ICSI. It is an in vitro fertilization technique that uses the intracytoplasmic injection of sperm for the fertilization of oocytes.
If this topic interests you, you will find information here: IVF.
If you need to undergo IVF treatment to become a mother, we recommend that you use the Fertility Report. In 3 simple steps, which will allow you to know the clinics abroad that meet our rigorous quality criteria. In addition, you will receive a report with useful tips before you make clinic visits.
Finally, there is a new technique which is a variation of the previous one. It is known as IMSI and consists of amplifying the image before the micro-injection to be able to observe the sperm morphology in more detail.
The microscope used by IMSI to select the sperm has an objective that amplifies the image to such an extent that morphological abnormalities are detected.
5-Your frequently asked questions
5-1 What is the cause of teratozoospermia?
Teratozoospermia is an alteration that affects male semen and involves most of the sperm having an abnormal shape.
Due to their poor morphology, sperm cannot fertilize the oocyte and cause sterility.
The causes of teratozoospermia are as follows:
- Genetic alterations
- Chemotherapy and radiotherapy
- Semen infections and orchitis
- Testicular trauma
- Varicocele
- Fever
- Diabetes and meningitis
- Tobacco, alcohol, drugs
Bad eating habits, clothes that are too close to the body ...
Certain causes can be resolved (fever, quitting smoking, healthy habits ...), which implies that in some cases, the pathology is reversible.
5-2 Does teratozoospermia cause miscarriages?
In principle, the poor morphology of the sperm does not cause any miscarriage once the fertilization of the oocyte has taken place and the embryo has implanted. If, on the other hand, the sperm also have genetic disorders, this may be a cause of miscarriage.
5-3 How to improve the amorphous sperm of semen?
If the pathology of teratospermia is not specific, the man should follow some indications to modify his lifestyle, which could negatively influence his reproductive state. Some men who stop smoking or alcohol consumption and change their diet may see an improvement in their sperm quality after 3 months.
5-4 Can leukospermia cause teratospermia and male infertility
Leukospermia, also known as leukocytospermia, is the appearance of leukocytes in semen, with a concentration level greater than 1 million per milliliter. The cause of this seminal pathology is an infection of the male reproductive tract which must be treated with antibiotics as it can affect spermatogenesis and cause oligospermia or teratozoospermia.
You can find the information in our article: Leukocytes in semen.
We deliver all over the world.
For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number
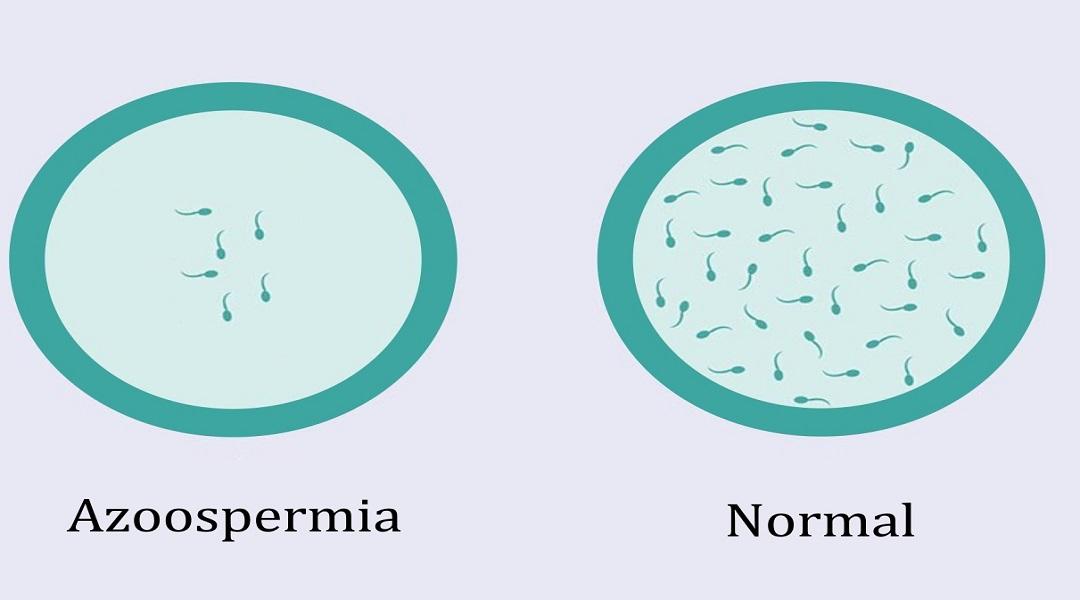
AZOOSPERMIA CAUSES: natural treatment
What is Azoospermia?
The azoospermia is a sperm abnormality characterized by the total absence of sperm in the ejaculate. It obviously leads to infertility in men, because in the absence of sperm there can be no fertilization. However, Dawasanté experts provide you with a natural herbal treatment to improve the quality and quantity of your sperm. Click here or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.

Azoospermia affects less than 1% of men in the general population or 5 to 15% of infertile men (1).
The causes
Depending on the cause, there are two types of azoospermia:
Secretory azoospermia (or NOA, for non-obstructive azoospermia)
Spermatogenesis is impaired or absent and the testes do not produce sperm. The cause of this spermatogenesis defect can be:
- hormonal, with hypogonadism (absence or abnormality in the secretion of sex hormones) which may be congenital (Kallmann-Morsier syndrome for example) or acquired, due in particular to pituitary tumors which alter the functioning of the hypothalamic-pituitary axis or after a treatment (eg chemotherapy);
- genetics: Klinefelter syndrome (presence of an extra X chromosome), which affects 1 in 1,200 men (2), structural abnormality of chromosomes, (microdeletion, i.e. loss of a fragment, of the Y chromosome in particular), translocation (one segment of the chromosome detaches and attaches to another). These chromosomal abnormalities are the cause of 5.8% of male infertility problems (3);
- bilateral cryptorchidism: the two testes have not descended into the bursa, which impairs the process of spermatogenesis;
- infection: prostatitis, orchitis.
Obstructive or excretory azoospermia (OA, obstructive azoospermia)
The testes do indeed produce sperm but they cannot be exteriorized due to a blockage of the ducts (epididymis, vas deferens or ejaculatory ducts). The cause may be of origin:
- congenital: the seminal tract has been altered from embryogenesis, resulting in an absence of the vas deferens. In men with cystic fibrosis, a mutation in the CFTR gene can cause the absence of vas deferens;
- infectious: the passages have been blocked following an infection (epididymitis, prostato-vesiculitis, prostatic utricle).
1-Pre-testicular causes
In this case, the origin of azoospermia is due to alterations at the endocrine level, that is, it is manifested by irregularities in the levels of the hormones responsible for regulating sperm production or spermatogenesis. . These are therefore cases of secretory azoospermia.
Among the main endocrine disorders that can cause azoospermia, we can find:
- Hypogonadotropic hypogonadism: this is a deficiency of the hormones released by the pituitary gland and responsible for stimulating the production of sperm in the testes. The main hormones are FSH (follicular stimulation) and LH (luteinizing). This problem can be due to genetic alterations such as Kallmann syndrome, tumors, trauma, pharmacological treatments, consumption of anabolic agents, etc.
- Hyperprolactinemia: it is the excessive increase in the hormone prolactin release. It blocks the hormone GnRH (a hormone that releases gonadotropins), whose function is to regulate the release of FSH and LH. This can be due to the consumption of antihypertensive drugs, stress, tumors, antidepressants, etc.
- Androgen insensitivity syndrome: this is mainly due to genetic mutations that cause resistance to androgens so that full virilization of the patient does not take place. Depending on the degree of severity, testosterone levels can be low, which prevents or hinders spermatogenesis, among other related consequences.
Patients who suffer from azoospermia due to this syndrome will have slightly decreased testicular volume, they will not produce sperm in the testes, and their FSH levels will generally below, except in cases of androgen resistance. In this case, the LH is elevated but the FSH and testosterone concentrations are usually normal or slightly elevated.
Testicular causes
The absence of sperm is due to problems in the testis which hamper spermatogenesis and therefore lead to errors or even blockage of sperm production.
The most common testicular pathologies are:
- Varicocele: dilation of the spermatic veins.
- Cryptorchidism: no descent of the testis from the inguinal canal to the scrotal pocket.
- Orchitis: Inflammation of the testicle, usually due to infection, as is often the case with mumps.
- Genetic alterations
- Testicular torsion
- Trauma
- Continuous increase in testicular temperature
The type of azoospermia from which these patients suffer is also secretory, but the clinical picture is different from the previous one: they have a lower testicular volume (due to non-production of sperm) but the FSH levels are high.
FSH, which is responsible for stimulating the testes to produce sperm, increases. This is why the testes do not respond to their stimulus, the body sends more FSH for the testes to function.
Post-testicular causes
When the cause of azoospermia is post-testicular, it is obstructive azoospermia. In this case, the testes are able to produce sperm properly, but there is a problem in the seminal ducts (vas deferens, epididymis or urethra) responsible for transporting sperm in an ejaculation.
Among these problems, we can highlight:
- Absence of vas deferens: this is a congenital pathology which, if it affects bilaterally, prevents sperm from coming out during ejaculate. This happens, for example, in some cases of cystic fibrosis.
- Obstruction of the vas deferens, the epididymis, or the urethra: it may be involuntary (trauma, surgery or disease) or voluntary. This is called a vasectomy.
Patients have a normal testicular size and FSH hormone levels are also average. Obstructive azoospermia is the least serious compared to fertility. It allows the man to obtain a pregnancy, either naturally, by a medical intervention which makes it possible to unblock the channels, or by obtaining sperm directly from the testicle and the subsequent application of a medically assisted procreation technique.
Your frequently asked questions
Is varicocele a cause of infertility in men?
By Victoria Moliner (embryologist).
Yes, varicocele can be a cause of male infertility. This pathology can manifest itself in different degrees of affection, so its harmful effect on male fertility (which mainly causes seminal and hormonal changes) can also be from mild to severe.
Is hormonal azoospermia always secretory?
By Andrea Rodrigo (embryologist).
Yes, when the lack of sperm is caused by hormonal problems, it is secretory azoospermia because of the lack of regulation by hormones prevents or complicates spermatogenesis.
Can cycling be the cause of my testicular factor azoospermia?
By Andrea Rodrigo (embryologist).
Continued use of the bicycle does not necessarily cause azoospermia, provided that the correct position is taken on the bicycle and, in some cases, certain testicular protection systems are used.
Routine improper use of the bicycle can increase the temperature of the scrotal region and thus prevent the proper production of sperm, which can reduce the quality of sperm.
As an added note, it is important to note that excessive exercise can affect sperm production in addition to other bodily functions.
Is azoospermia reversible?
By Andrea Rodrigo (embryologist).
It is possible that azoospermia is transient or punctual and, therefore, we can speak of reversible azoospermia. This means that, although it is unusual, a man may have a certain period of azoospermia, for example, due to stress or some other situation, and after this period recover the production of sperm and, with it, the presence of these in the ejaculate.
Read more
Why is there an absence of sperm in the spermogram?
By Zaira Salvador (embryologist).
When a man gets zero sperm as a result of his semen analysis, he may have azoospermia. First of all, this diagnosis should always be confirmed by a second spermogram, in case an error may have occurred while handling the first sample.
If azoospermia is confirmed, there are several causes of this seminal alteration, from blockage of the seminal ducts to problems with sperm production. More human testing should be done to find a more complete diagnosis.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
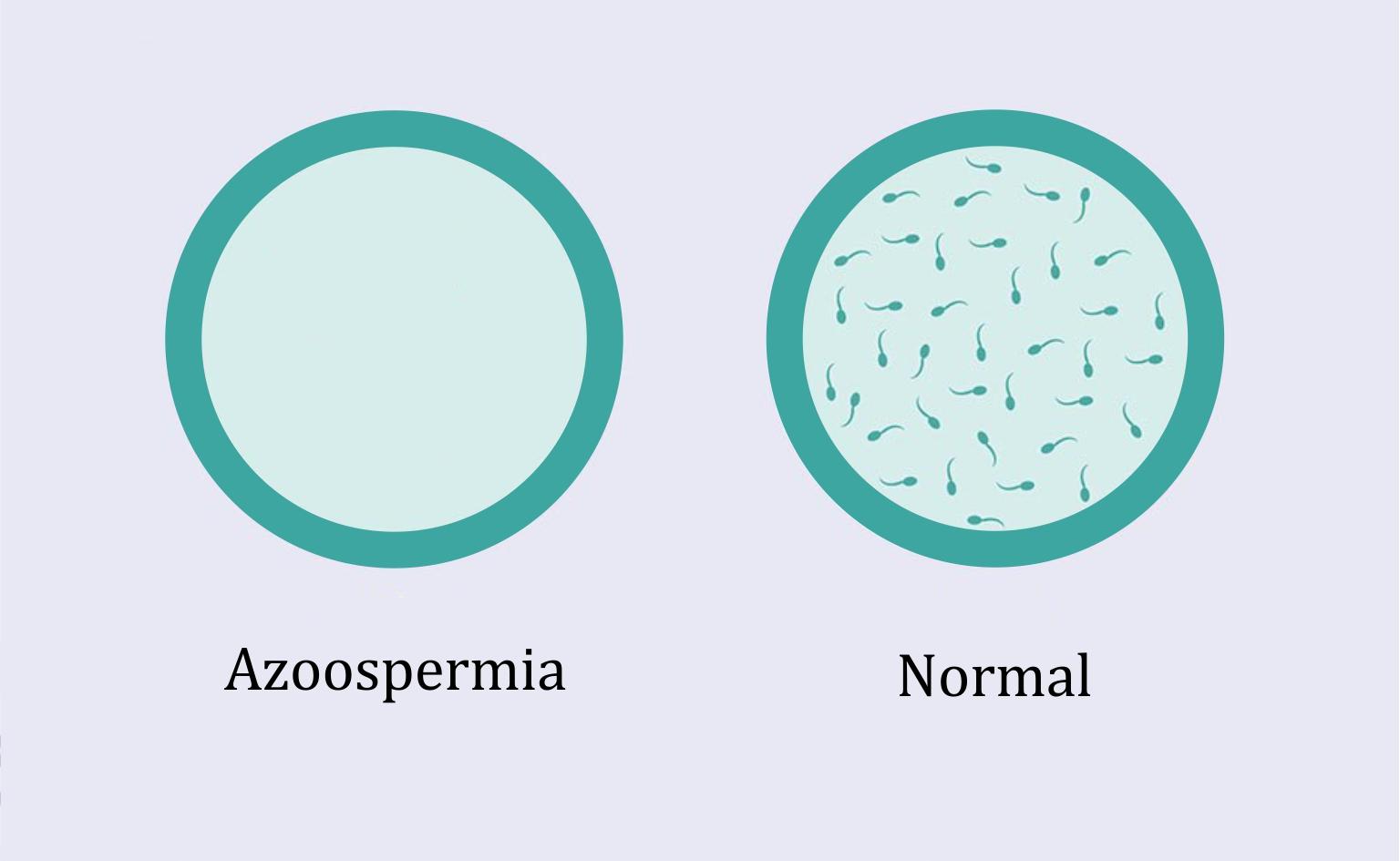
AZOOSPERMIA AND PREGNANCY: Natural treatment
Natural pregnancy in a woman whose partner has secretory or obstructive azoospermia is not possible. However, when the treatments applied do not solve the problem, Dawasanté experts offer you a natural herbal treatment to cure your azoospermia and allow your partner to quickly get pregnant.
Click here or on the image below to discover this natural treatment .
To discover our natural solution to treat azoospermia click here!
Contact our experts, tel / WhatsApp: +22990312738
1: Aspiration of sperm
In men with obstructive azoospermia , no sperm is seen in the ejaculate, but sperm is produced in the testis.
One option is to extract the sperm directly from the testis or epididymis. In this way, it is possible to obtain sperm, but in low quantity and of poor quality in relation to mobility and morphology.
For this reason, in the event of obtaining sperm by aspiration, it will be necessary to resort to the technique of ICSI (intracytoplasmic sperm micro-injection). ICSI is the ideal in vitro fertilization technique because only one sperm is needed for each egg to be fertilized. In addition, in this process, it is the specialist himself who introduces the sperm into the egg.
There are several procedures for extracting sperm, and their names come from the acronyms in English:
1.1: MESA
Corresponds to the term: microsurgical epididymal sperm aspiration , i.e., microsurgical aspiration of epididymal sperm. It is used in patients with obstruction of the genital tract. This involves making a small incision in the epididymis and extracting the sperm from inside the epididymis.
It is a complicated operation and the costs are high. For this reason, although it allows to collect more sperm than with a PESA, it is not the most chosen technique.
1.1.1: PESA
It is the percutaneous aspiration of epididymal sperm ( percutaneous epididymal sperm aspiration ). This is a simpler and less invasive procedure than the previous one and does not require as many skills on the part of the doctor. It is performed under sedation, so that the patient does not feel any pain.
A needle is inserted through the skin of the scrotum to reach the epididymis. The downside is that the needle is inserted blind, and although this is unusual, it is possible that no sperm will be aspirated.
1.1.2: TESA
Its English name is: testicular sperm aspiration , and it is referred to as the aspiration of sperm from the testis. It is also performed percutaneously, just like PESA. The difference is that the aspiration is done from the testes and not from the epididymis.
This type of aspiration is usually performed when the other options (MESA and PESA) are not applicable due to changes such as absence or obstruction of the epididymis.
2: Testicular biopsy
Also known as TESE ( testicular sperm extraction ). It is performed under local anesthesia and consists of the following elements:
- The specialist opens the different testicular layers using a scalpel or a laser until it reaches the testicle, from which he will extract small pieces. About 2-3 cm of testicular layers are opened. They will then be closed with one or two stitches.
- After the biopsy is performed or at the same time as the biopsy, the tissues are analyzed under a microscope for sperm, which will then be used in the ICSI technique in the hope of pregnancy.
- Although it is indicated in patients with obstructive azoospermia , it is also applied in certain situations of secretory azoospermia. In many of these cases, although no sperm is produced in the testes, foci of spermatogenesis can be found, that is, if you search exhaustively, it is possible to find a sperm.
- In any case, the possibility of achieving pregnancy by applying ICSI with the few sperm found after testicular biopsy of patients with secretory azoospermia is low.
3: Sperm donation
The above procedures may be effective for obstructive azoospermia , but they are not usually applied to secretory azoospermia. In patients with this alteration, where no treatment is able to reverse spermatogenesis, it is recommended to resort to sperm donation .
This is artificial insemination or in vitro fertilization with sperm donated by a healthy young man . This donor is subjected to a series of physical and psychological examinations to verify his good state of health and to confirm the safety of the use of his sperm.
The choice of one or the other reproductive technique will depend on certain qualities of the woman such as her age, the patency of the fallopian tubes, etc.
This is an alternative with a high probability of success . However, it has a major drawback: humans give up transmitting their genetic heritage. This means that the children born will not be the biological children of their father, since they will inherit the traits of the donor who gave the sperm.
4: Your frequently asked questions
If my husband has total azoospermia, should we consider donating sperm as the only option so that I can get pregnant?
If as total azoospermia you hear irreparable secretory azoospermia, yes, sperm donation is the best option for you to achieve pregnancy.
In severe cases of secretory azoospermia, it is very difficult to obtain viable sperm with fertilizing ability, so it is necessary to resort to sperm donation.
After 11 years of vasectomy, will I be able to have children if I have a testicular biopsy?
A testicular biopsy is used to obtain sperm directly from the testis, which is the place of production. However, after so long a time of voluntary obstruction, that is, after preventing the produced sperm from coming out, it is possible that the organism itself has reduced production. However, since only one sperm per egg is needed for ICSI treatment, you may be able to achieve pregnancy in your partner from the sperm found during the biopsy.
In any case, you should be aware that it is quite possible that no viable sperm will be found after the biopsy.
Pregnancy was detected by measuring serum HCG on two independent occasions, at least 15 days after the embryo replacement. Clinical pregnancy was determined by observing a gestational sac with a fetal heartbeat on a transvaginal ultrasound at 6–7 weeks gestation. The clinical embryo implantation rate was defined as the number of gestational sacs seen during ultrasound screening at 6-7 weeks gestation divided by the number of embryos transferred.
To discover our natural solution to treat azoospermia click here!
Contact our experts, tel / WhatsApp: +22990312738
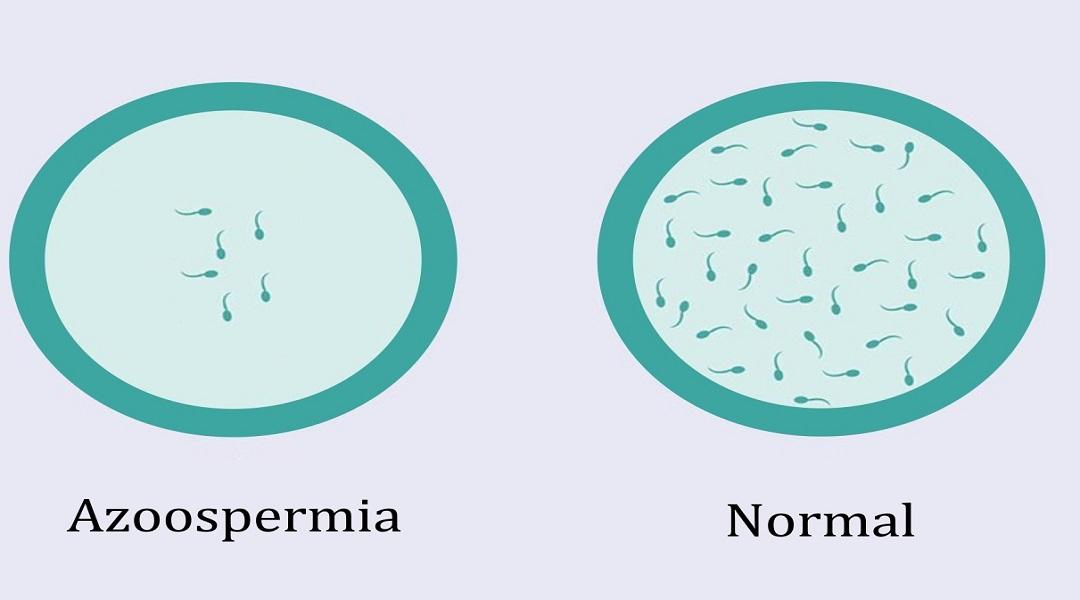
NONOBSTRUCTIVE AZOOSPERMIA: Natural treatment
Azoospermia is a total absence of sperm in the ejaculate. Depending on the cause, we distinguish two forms of azoospermia: obstructive and secretory. The prognosis for achieving pregnancy is different in each case. However, Dawasanté experts provide you with a natural treatment to boost your fertility by improving your sperm, allowing you to conceive quickly. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
1: Azoospermia: definition and diagnosis
In order to study male fertility, the most common test is a spermogram. It consists of collecting a sample of ejaculate and examining it in the laboratory to check, among other things, the concentration and mobility of sperm.
Once the result is obtained, we compare the reference rates of the World Health Organization (WHO) to carry out the diagnosis:
zero sperm in the ejaculate.
less than 100,000 sperm / ml.
less than 15 million / ml.
- Normozoospermia
no seminal parameters are altered.
Therefore, azoospermia can be defined as the absence of sperm in the ejaculate. It is considered to be responsible for between 3 and 10% of cases of male infertility.
Azoospermia is imperceptible to humans, so it is necessary to take a spermogram to diagnose it.
It is also helpful to determine FSH hormone levels. This is produced by the brain and is responsible for spermatogenesis (formation of sperm) in the testes. If the FSH levels are high, it can be inferred that the mother cells of the sperm are reduced or even absent.
You can also analyze the concentration of testosterone and fructose to get a more accurate diagnosis.
Causes
The absence of sperm in the ejaculate is mainly due to two causes:
- Secretory or non-obstructive azoospermia
the testes are not able to produce sperm.
- Azoospermia obstructive
sperm are produced, but cannot be expelled during ejaculate due to obstruction of the vas deferens.
To determine the type of azoospermia, it is necessary to perform a testicular biopsy, which consists of obtaining a small fragment of each testicle and analyzing the presence or absence of sperm. In this way, it will be easy to distinguish an obstructive azoospermia from a secretory.
Through hormonal analysis, the type of azoospermia can be determined, because if there are disturbances in the levels of hormones involved in spermatogenesis , it is secretory azoospermia. However, this method is not as reliable as a biopsy to find out if there are sperm available for ART treatment.
1: Secretory azoospermia
The azoospermia secretory or non-obstructive is the most severe and frequent and assumes 70% of cases of azoospemie. It can be congenital (from birth) or acquired (by disease or toxic treatment). Its most common causes are:
- Abnormalities of testicular descent.
- Exposure to toxic substances: drugs, radiotherapy and chemotherapy.
- Genetics: Gene disorders related to spermatogeneses, such as mutations or deletions.
- Hormonal disorders, such as hypogonadotropic hypogonadism (deficiency of hormones released by the pituitary gland and responsible for stimulating sperm production in the testes).
- Testicular problems: mumps, trauma, inflammation and sever varicocele.
The recovery of sperm from secretory azoospermia is complex, as spermatogenesis is strongly affected. Despite this, pregnancy is possible.
Some patients with this pathology have presented slight foci of spermatogenesis in the testes. To do this, doctors do multiple small testicular biopsies to find sperm.
If sperm are indeed found, the sample is frozen and is then used in an intracytoplasmatic sperm injection (ICSI).
Depending on the cause of the azoospermia, in some cases, it is possible to restore spermatogenesis by hormonal treatments and thus achieve pregnancy.
In cases where it is not possible to collect sperm, it is necessary to use donor sperm to become parents.
2 :Azoospermie obstructive
Obstructive azoospermia is caused by a problem with the ducts that carry sperm from the testes to the urethra, where ejaculate occurs. Here are the most common causes:
- Absence of vas deferens (either from birth or after surgery).
- Inflammation or trauma to the testis, epiydima, vas deferens or prostate.
In patients with this type of disorder, it is easier to obtain sperm. In some cases, this azoospermia can be reversible and thanks to several techniques of micro-surgery, the obstruction can sometimes be resolved or the ducts united so that the sperm can reach the spermatic fluid.
Otherwise, the sperm are obtained directly from the testes by testicular biopsy and are used in assisted reproduction therapy (ICSI). A single biopsy is normally sufficient, as spermatogenesis is produced normally.
Azoospermia and varicocele
The relationship between azoospermia and varicocele is relatively common: 5% of varicocele cases turn into azoospermia. However, for this to happen, the varicocele must be severe.
Varicocele is a dilation of the veins that form the spermatic cord and directly affects spermatogenesis, which is the production of sperm.
In secretory azoosperm patients who have corrected their varicocele by surgery (surgical treatment of varicocele ), approximately 50% of the testicular tissue and 55% of the sperm mobility will be recovered.
Azoospermia following vasectomy
Vasectomy is a method of male sterilization that results in the absence of sperm in the ejaculate. The goal is to intentionally induce obstructive azoospermia by severing the vas deferens, thus preventing the passage of sperm from the testis to the urethra.
As the vas deferens are blocked, the sperm will be stored in the epididymis and, over time, will be reabsorbed by the body itself.
Vasectomy does not affect sperm production, although it is true that over time the body can decrease sperm production or it can be altered slightly.
Your frequently asked questions
No. Azoospermia is the absence of sperm in the ejaculate, but the man has no problems ejaculating. In the case of aspermia, the problem is the lack of ejaculation, it does not refer to the sperm.
What are the symptoms of azoospermia?
By Andrea Rodrigo (embryologist).
Azoospermia does not lead to symptoms that are visible in everyday life such as pain, discomfort, swelling, etc. Therefore, the safe way to diagnose it is not based on the symptoms, but only on the result of the spermogram.
Secretory azoospermia is more serious. It prevents the production of sperm and, therefore, it is not possible to have biological children even by applying assisted reproduction techniques. As we mentioned, the only option for getting pregnant if you are suffering from this type of azoospermia is sperm donation.
Can I use artificial insemination in the case of azoospermia?
No. To achieve pregnancy by artificial insemination , it is necessary to have a good sperm concentration and that patients suffering from azoospermia do not have any sperm in the ejaculate.
Can you be naturally pregnant with secretory azoospermia?
The only way to achieve a natural pregnancy with secretory azoospermia is through hormonal treatment, as it restores spermatogenesis. However, in many cases it is difficult for this to happen, as it all depends on the cause of azoospermia.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
AZOOSPERMIA NATURAL TREATMENT: the experts at Dawasanté
What is azoospermia?
The azoospermia is a lack of sperm in the semen. If, after a year of unprotected sex, no pregnancy has occurred, it means that the man, woman, or both may have a fertility problem. In 40% of infertile couples, the man has a fertility problem. However, Dawasanté experts provide you with a natural herbal treatment to improve the quality of your sperm and allow you to conceive quickly.
Click here or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
How common is azoospermia?
About 1% of all men and 10% to 15% of infertile men have azoospermia.
Treatment
Here we are going to offer you a mixture of African plants, roots and bark that will help you heal your azoospermia. Our blend of plants and roots has already enabled many men around the world to heal from infertility and experience the joy of being a father. What allows us to have excellent results is that we produce all these plants and roots ourselves and that we select only the best plants so that they retain all their therapeutic and medicinal virtues. They are the best roots and plants against azoospermia.
Here are five plants and roots that will help you cure azoospermia:
1. Saw palmetto

Saw palmetto helps boost libido by stopping the breakdown of testosterone in the body. In men, sperm production is guided by testosterone. Too little testosterone results in a low sperm count. Likewise, too little testosterone reduces a woman's egg production. Saw palmetto can therefore increase male and female fertility by altering the balance of free testosterone in the body.
2. Ashwagandha

Ashwagandha is traditionally used to improve sexual health. It supports the endocrine system and promotes its better functioning. It also strengthens the hormonal balance in the body. It stimulates libido and improves sperm count in men. It improves stamina and also improves sexual performance.
3. Saw Palmetto

Saw Palmetto nourishes the entire endocrine system, which can help improve overall reproductive function in humans. Men with high stress, poor immune function, poor lifestyle and eating habits are found to respond well to this plant. This plant is classified as an adaptogen and is antiandrogenic, anti-inflammatory, softening, urinary antiseptic and immuno-amphoteric. Saw Palmetto is also a reproductive amphoteric. What does this mean though? It just means that it normalizes reproductive function.
Saw Palmetto nourishes the body deeply when taken regularly for many months. Constant use of this herb is beneficial in improving the quality and quantity of sperm.
4. Ginseng

Ginseng is often referred to as the king of all herbs and is proven to be the panacea for improving overall well-being. Ginseng is also an aphrodisiac and is used to treat sexual dysfunction and to improve sexual behavior in traditional Chinese medical practices. Data from animal studies have shown a positive correlation between ginseng's performance, libido and copulation, and these effects have been confirmed in case-control studies in humans. In addition, ginseng improves the quality of sperm and their number. We highly recommend it.
5. Maca

Maca has the ability to improve female fertility, which is why it is getting a lot of attention. It balances female hormones to improve fertility. However, this herb also has the ability to boost male fertility. This plant effectively improves the quality of sperm (poor sperm quality is a cause of male infertility). According to a study, men who consume maca regularly have more mobile sperm, more sperm and more semen per ejaculation.
The natural treatment that we offer to cure azoospermia consists mainly of natural herbal teas. The herbal tea is composed of plants and roots whose active ingredients are able to restore the male hormonal balance, by increasing the level of testosterone, the number and the mobility of your sperm. It is the miracle solution to cure azoospermia.
To find out about our natural remedy to cure azoospermia, click here
Cause of azoospermia
Depending on the cause, there are two types of azoospermia:
Secretory azoospermia (or NOA, for non-obstructive azoospermia)
Spermatogenesis is impaired or absent and the testes do not produce sperm. The cause of this spermatogenesis defect can be:
- Hormonal, with hypogonadism (absence or abnormality in the secretion of sex hormones) which may be congenital (Kallmann-Morsier syndrome for example) or acquired, due in particular to pituitary tumors which impair the functioning of the hypothalamic-pituitary axis or after a treatment (eg chemotherapy);
- Genetics: Klinefelter syndrome (presence of an additional X chromosome), which affects 1 in 1,200 men, structural abnormality of the chromosomes (microdeletion, i.e. loss of a fragment, of the Y chromosome in particular), translocation (one segment of the chromosome detaches and attaches to another). These chromosomal abnormalities are the cause of 5.8% of male infertility problems;
- Bilateral cryptorchidism: the two testes have not descended into the bursae, which impairs the process of spermatogenesis;
- An infection: prostatitis, orchitis.
Obstructive or excretory azoospermia (OA, obstructive azoospermia)
The testes do indeed produce spermatozoa but they cannot be exteriorized due to a blockage of the ducts (epididymis, vas deferens or ejaculatory ducts). The cause may be of origin:
- congenital: the seminal tract has been altered from embryogenesis, resulting in an absence of the vas deferens. In men with cystic fibrosis, a mutation in the CFTR gene can cause the absence of vas deferens;
- infectious: the passages have been blocked following an infection (epididymitis, prostato-vesiculitis, prostatic utricle).
Symptoms
The main symptom of azoospermia is infertility.
Diagnostic
The diagnosis of azoospermia is made during an infertility consultation, which in men systematically includes a spermogram. This examination consists of analyzing the content of the ejaculate (semen), evaluating various parameters and comparing the results with the standards established by the WHO.
In the event of azoospermia, no sperm is found after centrifugation of the entire ejaculate. To make the diagnosis, however, it is necessary to carry out one or even two other spermograms, each 3 months apart, because spermatogenesis (cycle of sperm production) lasts about 72 days. In the absence of sperm production over 2 to 3 consecutive cycles, the diagnosis of azoospermia will be made.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
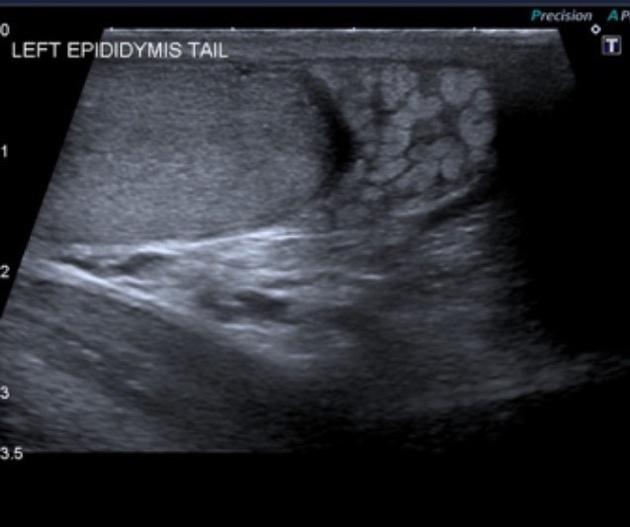
VARICOCELE THROMBOSIS: Natural treatment
THROMBOSED VARICOCELE
Acute scrotal pain has various causes. Testicular torsion, twisting of the appendages, and epididymal-orchitis are common causes, while varicocele thrombosis is a rare cause. Read till the end to uncover the secret of natural herbal treatment for varicocele.
HOW DOES THIS COME ABOUT?
The thrombosis varicocele can occur after the operation or spontaneously. Five cases of postoperative thrombosis and five cases of spontaneous thrombosis have been described to date. The traditional advice in the management of thrombosed varicocele has been managed by the pharmacist and the patient. Here we present an unusual case of spontaneous varicocele thrombosis, as well as its presentation and surgical treatment. We would like to highlight the points of differentiation between spontaneous thrombosis and postoperative in vitro clot formation in varicoceles, these two entities being often confused.
But before that, Dawasanté experts provide you with a natural herbal treatment to treat spontaneous varicocele thrombosis. Click on the image below to discover this natural treatment.
How to cure varicocele with plants?
First, varicocele is not a fatality whose only way out is an operation. The use of natural plants makes it possible to permanently cure varicocele by avoiding surgical operation. The natural remedy for curing varicocele that we offer is completely herbal treatment. It is a natural remedy that cures varicocele successfully by strengthening the valves or valves located in the veins of the spermatic cords. So the veins become tonic and tenacious to facilitate the dynamic rise of blood along the veins. This to join the most important veins like the left renal vein and the inferior vena cava. So, it has proven its effectiveness with dozens of resolved cases. Associated with a suitable diet, it can treat varicocele quite easily.
Take advantage of this opportunity to discover our natural remedy for varicocele
To contact our experts please call or write to us on the following number, tel / WhatsApp: +22990431727
WE DELIVER ALL OVER THE WORLD
Presentation of the case
A 68-year-old man was presented with excruciating scrotal pain lasting a week. Doppler study of the scrotum revealed a left varicocele without a sign of epididymal-orchitis. He was treated with intravenous antibiotics, pain relievers, and an elevated scrotum. He had no relief and continued to have severe pain. The clinical examination was normal. The patient underwent semi-emergent exploratory surgery. Exploration revealed a normal testis with thrombosed varicoceles. The patient underwent a varicocelectomy. The postoperative patient had immediate pain relief. Histopathology revealed a varicocele significant thrombosis. A varicocelectomy sample (performed for primary infertility) was used for comparison. The points of differentiation between the two entities were noted.
Conclusion
Spontaneous varicocele thrombosis is a rare cause of acute scrotal pain. Pain out of proportion to clinical features is characteristic. Patients unresponsive to medical treatment may require varicocelectomy. Varicocelectomy can provide immediate relief. Histopathology is helpful in this disorder.
Acute scrotal pain has multiple etiologies. Torsion of the testis or its appendages and epididymal-orchitis are common, while varicocele thrombosis is a rare cause. Varicocele thrombosis can occur after the operation (5 cases) or spontaneously (5 cases). Spontaneous thrombosis can occur as a result of trauma or in patients with coagulation abnormalities. Kayes had reported that strenuous sexual or sports activities, infections, trauma, long hours theft, and medication could be the cause of the condition. There was no major predisposing mechanism to spontaneous thrombosis in our patient, but it is possible that vigorous sexual activity was the cause, because the patient developed pain after intercourse. Varicocele thrombosis (both spontaneous and postoperative) has been managed conservatively in all patients to date with medication (antibiotics and anti-inflammatory drugs) and scrotal support without a description of surgical treatment. There are conflicting reports regarding the timing and requirement of surgery in patients with thrombosed varicocele. Recommend non-operative conservative management, despite having submitted their patients to surgery. Therefore, the timing and necessity of surgery in patients with thrombosed varicocele become an extremely moot point. We present here a case of spontaneous thrombosis due to Varicocele, with particular emphasis on its presentation and surgical treatment. Spontaneous in vivo thrombi have always been confused with in vitro post varicocelectomy clot formation in the veins. We would like to highlight the histopathological differentiation between these two distinct entities.
OTHER NATURAL METHODS TO TRY
Perform Cooling Showers
Cooling is a method of reducing the body’s temperature. Testicular overheating is a major cause of concern for men with varicoceles, and can also cause infertility.[8]
It is shown to reduce inflammation markers.
Of note for varicocele, cooling can improve vein contractility and reduce the swelling of the veins.
How to Perform
- While taking a shower, run cold water over your testicles for 15–30 seconds.
- It helps to wash the whole scrotum, including the pubic area with cold water, because the veins run throughout the entire region.
- Perform cooling treatments as many times as needed per day to reduce testicular temperature but avoid overcooling.
Ginger for varicocele

Take a cup of ginger tea every day for 1 month.
Garlic for varicocele

Take 2 to 3 garlic pods and mash them.
Leave it for 15 mins.
Have it with a glass of water after 15mins.
Take it for 2 weeks.
Take advantage of this opportunity to discover our natural herbal treatment for varicocele
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022990431727
WE DELIVER ALL OVER THE WORLD
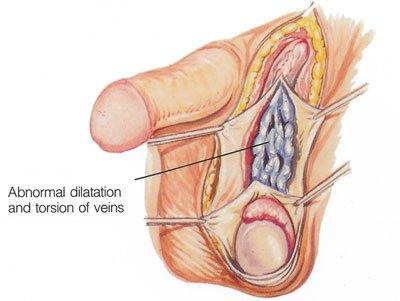
NATURAL TREATMENT AGAINST VARICOCELE: Dawasanté Experts
NATURAL TREATMENT AGAINST VARICOCELE
What is a varicocele?
The varicocele is characterized by the expansion of a vein (varix) at the spermatic cord, fibrous cord located in the purses above each testicle, and connecting each of the scrota.
Varicocele usually affects only one side, mostly the left because of the anatomy of the venous network of the male genitals. On the left side, blood from the testis is drained to the renal vein, while on the right it is drained to the vena cava, where the pressure is lower than in the renal vein. Here is a natural herbal treatment from the experts at Dawasanté to treat varicocele without surgery. Click on the image below to discover this natural treatment.

Treatment
First of all, varicocele is not inevitable and the only way out is an operation. The use of natural plants makes it possible to permanently cure varicocele by avoiding surgical operation. The natural remedy for curing varicocele that we offer is completely herbal. It contains two elements namely: an herbal tea and an ointment. Trust us! Because it is the secret to cure varicocele without operation thanks to the plants.
Herbal tea to cure testicular varicose veins is vasculoprotective and venotonic. It is a natural remedy that cures varicocele successfully by strengthening the valves or valves located in the veins of the spermatic cords. So the veins become tonic and tenacious to facilitate the dynamic rise of blood along the veins. This to join the most important veins like the left renal vein and the inferior vena cava. The operation for varicocele is very expensive and is of little benefit. As for our remedy, it has proven its effectiveness with dozens of resolved cases. So, this is one of the best natural herbal remedies to cure varicocele and prevent operation.
Using herbal teas to cure varicocele usually gives excellent results as it helps prevent the operation. So our natural remedy is the best herbal therapy for Varicocele. The solution to cure varicocele is in plants. Being natural products based on plants and herbs, our herbal teas to treat varicocele do not cause any side effects, either on the body or on health. Our natural remedy is the miracle solution to cure varicocele without operations or side effects. So it is the best natural remedy to cure varicocele.
To discover our natural remedy for varicocele click here
Tips for fighting varicocele
To cure varicocele, here are the tips we give you:
Wear suitable underpants or sports clothing
Apply cold compresses of water to your testicles when they heat up for 10 minutes
· You should cut out spices, alcohol, coffee, tea, and all exciting drinks, as well as alcohol and tobacco. These foods dramatically increase the inflammation of varicose veins and thus increase discomfort.
Space your sexual relations as best as you can throughout the treatment in order to put the veins to rest
Avoid playing sports during the entire treatment period
· Hot baths will help reduce inflammation.
Our doctor's opinion
First, varicocele is a varicose dilation of the veins of the spermatic cord (located in the bursa, above and around each testicle). She usually does not have any specific symptoms. But it can be manifested by a heaviness in the stock market. At an advanced stage, it causes an increase in the size of the testicle. It is therefore very troublesome. Most of the time, the treatment is surgical, but many people refuse to be operated on for fear or otherwise. However, there is a very effective solution: Medicinal plants. The purpose of these plants is to make it disappear. Also, it is important to trust us because your satisfaction is our priority. Above we offer you the best natural remedy to cure varicocele quickly without operation or surgery.
Symptoms of varicocele
The symptoms of varicocele vary greatly from one individual to another. In some cases, you may have a varicocele and not have any symptoms (asymptomatic varicocele). But in other cases, varicocele can manifest itself as heaviness and pain in the bursae. Especially at the end of the day, when you are standing, during physical exertion or in hot weather. These pains may worsen over time. In some cases, varicocele is only bothersome in periods.
The causes of varicocele
First, no one can tell you exactly what causes varicocele, but we do know that it results from a malfunction of the one-way valves that allow blood flow from the testes to the heart. The pressure in the vein increases and the venous valves of the spermatic cord are weakened. This increase in pressure results in dilations in the venous plexus.
Although the relationship is not yet well established between male infertility and varicoceles, recent studies have shown that many boys who suffer from infertility have varicoceles and once varicoceles are treated, infertility goes away. The figures, therefore, show a very close link between varicocele and fertility. In fact, one in three men affected by primary infertility has a varicocele, 80% in the case of secondary infertility, against only 15% in the general population. Nevertheless, a varicocele can even lead to infertility.
However, the links between varicocele and subfertility are not obvious. Testicular varicose veins are a very common problem for which we do not yet fully understand the consequences on fertility, nor the mechanisms involved. There is no link of certainty, only a reasonable doubt.
However, varicocele could directly affect spermatogenesis, which is the production of sperm. Varicose veins (dilated veins) can appear in the scrotum. These varicose veins will increase the temperature in the testicles. The heat weakens the sperm and can interfere with sperm production. The relationship between azoospermia and varicocele is relatively common: 5% of varicocele cases turn into azoospermia. Many men with testicular varicose veins also have azoospermia.
To discover our natural remedy for varicocele click here
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022990431727
WE DELIVER ALL OVER THE WORLD

HOMEMADE RECIPE AGAINST TESTICLE VARICES OR VARICOCELE
HOME RECIPE TO TREAT VARICES OF TESTICLES OR VARICOCELE
What is Varicocele?
The varicocele is a varicose dilation of veins (varices) spermatic cord (located in exchanges, over and around each testicle). This dilation is the consequence of a malfunction of valves located in the veins. The blood is no longer able to go back up along the veins to reach the larger veins (left renal vein and inferior vena cava). We provide you with a simple homemade recipe to treat varicose veins of the testicles or varicocele.

Take advantage of this opportunity to discover our natural herbal treatment for varicocele
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022990431727
WE DELIVER ALL OVER THE WORLD
Varicocele is a unilateral or bilateral varicose dilation of the veins (varicose veins) of the spermatic cord located in the bursa, above and around each testicle.
Often, this dilation is the consequence of a malfunction of the valves located in the veins. Thus the blood no longer manages to go up correctly (towards the heart) along the veins to reach the larger veins. That is to say the left renal vein and the inferior vena cava. Thus, part of the blood escapes and stagnates in the veins, swelling them and this constitutes a dangerous obstacle for the migration of spermatozoa. It is one of the causes of male infertility, especially when the varicocele is bilateral.
The left side is more often affected than the right (on the left side, the spermatic veins join the left renal vein while on the right side they join the inferior vena cava). Both sides can be reached symmetrically or asymmetrically.
Simple Homemade Recipe For Varicocele
First of all, varicocele is not inevitable and the only way out is an operation. The use of natural plants makes it possible to permanently cure varicocele by avoiding surgical operation. The natural remedy for curing varicocele that we offer is completely herbal. It contains two elements namely: an herbal tea and an ointment. Trust us! Because it is the secret to cure varicocele without operation thanks to the plants.
This homemade recipe for varicocele is a herbal tea to cure testicular varicose veins is a vasculoprotective and venotonic. It is a natural remedy that cures varicocele successfully by strengthening the valves or valves located in the veins of the spermatic cords. So the veins become tonic and tenacious to facilitate the dynamic rise of blood along the veins. This to join the most important veins like the left renal vein and the inferior vena cava. The operation for varicocele is very expensive and is of little benefit. As for our remedy, it has proven its effectiveness with dozens of resolved cases. So, this is one of the best natural herbal remedies to cure varicocele and prevent operation.
Using herbal teas to cure varicocele usually gives excellent results as it helps prevent the operation. So our natural remedy is the best herbal therapy for Varicocele. The solution to curing varicocele is in plants. Being natural products based on plants and herbs, our herbal teas to treat varicocele do not cause any side effects, either on the body or on health. Our natural remedy is the miracle solution to cure varicocele without operations or side effects. So it is the best natural remedy to cure varicocele.
Take advantage of this opportunity to discover our natural herbal treatment for varicocele
What are the causes of varicocele?
Varicocele is caused due to the malfunction of a valve located in the veins (which allows blood to flow to the testes). As the cause of this dysfunction is still unknown, it is impossible to explain the exact causes of varicocele.
What are the symptoms of varicocele?
Since a varicocele rarely produces symptoms, it is not uncommon for a man to realize that he has one, unless it is causing fertility problems or is not noticeable on a physical exam. routine. When symptoms do appear, they tend to be felt as a dull ache or a feeling of heaviness in the testicle, which gets worse during the day, especially in hot weather or after physical exertion. Dilated veins in the scrotum can often be felt or seen, and the testicle is smaller on the varicocele side.
Probable Causes of Varicocele Disease
- Constipation over a long period.
- Standing for many hours
- The practice of violent exercises that solicit the muscles of the pubis, the perineum without appropriate support.
- The problem of the formation of non-toned flaccid veins (congenital cause).
The embolization technique is performed under local anesthesia. A small catheter is introduced through the femoral artery to the dilated spermatic veins, through which substances are injected to block the vein. The disappearance of By embolization:
It is performed either through a conventional incision (inguinal or abdominal) or by laparoscopy (a camera is introduced through a reduced incision in the abdomen). It consists in ligating the spermatic veins in their upper part, so as to cause an involution (regressive modification) of the veins of the cord; Surgical varicocele at 3 months is obtained in 98% of cases. This minimally invasive technique is as effective as surgical treatment.
Frequency and person at risk
It is a rare condition in children under the age of 15 but becomes more and more common from the age of 19. She will later be responsible for the problems of male infertility which are unfortunately very common nowadays due to prostitution and poorly treated infections. According to WHO statistics, about 40% of men consulting for infertility or subfertility problems have varicoceles.
Beneficial effects of the varicose vein potion on the testicles
The Potion treats and heals varicose veins in the testicles or varicocele successfully by strengthening the valves or valves located in these veins of the spermatic cord. The astringent elements it contains invigorates the veins, activates the circulation in the small vessels, and prevents the blood from stagnating. Its depurative elements relieve the liver and facilitate the drainage of toxins. A varicocele detected in time and well treated allows man to regain all his fertilizing power. Almost 100% effective remedy.
This homemade recipe has been studied and has proven effective for many, why not you?
Take advantage of this opportunity to discover our natural herbal treatment for varicocele
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022990431727
WE DELIVER ALL OVER THE WORLD
VARICOCEL AND FERTILITY: Natural treatment
VARICOCEL AND FERTILITY
Many men have dilated veins in the scrotum, which is the pouch containing the testicles. Doctors call these veins varicoceles. Many men with varicocel have no symptoms, but some may have fertility problems. Varicoceles are common and affect 10 to 15% of men. Doctors continue to debate the role of varicoceles in infertility. However, Dawasanté experts provide you with a natural herbal treatment to cure varicocele and treat your infertility. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Some research suggests that treating a varicocele may improve fertility outcomes. However, a systematic review indicates that the available evidence is weak and that doctors need to do more research.
In this article, find out if a varicocele affects fertility.
What is a varicocele?
A varicocele occurs when a bulge results from dilated veins inside the scrotum. The swelling usually looks like a magnification above the testis, without discoloration. A pampiniform plexus is a group of veins inside the scrotum. These veins help cool the blood before it goes to the testicular artery, which supplies the testes with blood.
If the testicles are too hot, they cannot produce healthy semen. The health of sperm affects fertility. It is therefore essential that the veins can cool the blood. Most people with a varicocele don't have symptoms, but some may have fertility problems. When a person has a varicocele, they may also experience swelling and tenderness in the scrotum.
Treatment
First, varicocele is not inevitable, the only way out is an operation. The use of natural plants makes it possible to cure varicocele permanently by avoiding surgical operation. The natural remedy for curing varicocele that we offer is completely herbal. It contains two elements namely: an herbal tea and an ointment. Trust us! Because it is the secret to cure varicocele without operation thanks to the plants.
Herbal tea to cure testicular varicose veins is vasculoprotective and venotonic. It is a natural remedy that cures varicocele successfully by strengthening the valves or valves located in the veins of the spermatic cords. So the veins become tonic and tenacious to facilitate the dynamic rise of blood along the veins. This to join the most important veins like the left renal vein and the inferior vena cava. The operation for varicocele is very expensive and is of little benefit. As for our remedy, it has proven its effectiveness with dozens of resolved cases. So, this is one of the best natural herbal remedies to cure varicocele and prevent operation.
Using herbal teas to cure varicocele usually gives excellent results as it helps prevent the operation. So our natural remedy is the best herbal therapy for Varicocele. The solution to curing varicocele is in plants. Being natural products based on plants and herbs, our herbal teas to treat varicocele do not cause any side effects, whether on the body or on health. Our natural remedy is the miracle solution to cure varicocele without operations or side effects. So it is the best natural remedy to cure varicocele.
To discover our natural remedy for varicocele click here
Do Varicoceles Cause Infertility?
Most men with varicoceles do not have fertility problems. Infertility rates in people with varicoceles, however, are higher than in those without. This difference may be due to the fact that varicoceles interfere with the body's ability to make and store semen.
A 2014 study found that varicoceles are sometimes, but not always, a factor in infertility.
Research on whether treating varicoceles can improve fertility is mixed.
A 2012 meta-analysis of previous studies found that treating a varicocele could improve fertility, especially if the cause of a couple's infertility is unknown. However, the researchers stress that the evidence is weak and therefore more research is needed.
The main concern with varicoceles is that the bulging of the veins can damage the sperm and reduce their number. In individuals with an average sperm count, a varicocele is unlikely to cause infertility.
When a couple cannot conceive, it is essential to do a variety of tests, including a sperm count, and not to assume that varicocele is necessarily the only cause.
Causes and risk factors
A varicocele occurs when the veins in the scrotum grow larger. Each vein has a valve that prevents blood from flowing back, but sometimes the valve fails. This causes blood to flow back, damaging the vein and causing swelling. Doctors do not fully understand what causes valve failure and varicocele. They are common and usually do not mean that a person has an underlying health problem.
Studies have proven that smoking can be a risk factor for varicocele because it damages a person's blood vessels. The same study found no link between alcohol or occupation and varicoceles.
Rarely, growth in the stomach can put pressure on the veins, causing a varicocele. This problem is more common in men over 45.
In many people, a varicocele has no apparent cause.
Diagnostic
Most men with varicoceles don't notice anything unusual, although some people report an occasional thrill or throbbing in the scrotum. Many affected people only find out that they have a varicocele after having had problems with infertility. A doctor can often diagnose a varicocele during a physical exam by examining the scrotum and looking for any unusual lumps and blood vessels.
If a doctor suspects a varicocele, they may order an ultrasound. This is a painless imaging test that allows the doctor to see the veins inside the scrotum.
If the person has fertility problems, the doctor may also order a semen analysis to check the quality of the semen.
Medical treatment
Varicoceles that do not cause symptoms do not require treatment. A varicocele may need treatment when:
- · A man has varicocele and low sperm count or other semen problems.
- · Varicocele causes pain or swelling.
- · A couple has unexplained infertility and the male has a varicocele.
When people choose to undergo treatment, they have two different options:
Embolization
Embolization is a surgical procedure that temporarily cuts off the blood supply. A doctor can perform this procedure in their office under local anesthesia, which means that a person will not feel any pain in the area.
During embolization, a doctor inserts a needle into a vein usually through the groin. Sometimes they can insert a needle through the neck. The needle helps the doctor access the veins in the scrotum and block the varicocele. A person may experience pain and tenderness after the procedure, but the recovery time is short and the person can immediately resume normal activities.
Surgery
A doctor can surgically remove a varicocele by blocking blood flow to the damaged vein. This operation is called a varicocelectomy.
A person will undergo general anesthesia before the varicocelectomy in order to be asleep and unable to feel any pain during the procedure. A person may experience pain and tenderness for several days.
Surgery is more effective is embolization with a failure rate of less than 5%. Laparoscopic surgery uses a smaller incision than open surgery and requires less recovery time but also requires a very skilled surgeon. Open surgery uses a wider cut in the scrotum.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
ASTHENOSPERMIA: NATURAL TREATMENT
What is asthenospermia?
The asthenospermia or asthenozoospermia is a sperm abnormality characterized by insufficient mobility of spermatozoa. It can alter a man's fertility and reduce the couple's chances of pregnancy because if they are not sufficiently mobile, the sperm cannot migrate from the vagina to the tube to fertilize the oocyte. However, Dawasanté experts provide you with a natural plant-based treatment to permanently cure asthenospermia.
Click here or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Asthenospermia can be isolated or associated with other sperm abnormalities. In the case of OATS, or oligo-astheno-teratozoospermia, it is associated with oligospermia (sperm concentration below normal values) and teratozoospermia (too high a proportion of abnormally shaped sperm). The impact on human fertility will be even greater.
Treatment
Here we are going to offer you a mixture of African plants, roots and barks that will help you heal your asthenospermia. Our blend of plants and roots has already enabled many men around the world to recover from their asthenospermia and experience the joy of being a father. What allows us to have excellent results is that we produce all these plants and roots ourselves and that we select only the best plants so that they retain all their therapeutic and medicinal virtues. They are the best roots and plants against asthenospermia.
Here are five plants and roots that will help you cure asthenospermia:
1. ROOTS MALE INFERTILITY
The effects of herbal remedies for treating asthenospermia problems have been proven by studies and hundreds of years of use. Here we are going to offer you a mixture of African plants, roots and bark that will help you heal your infertility. Our blend of plants and roots has already enabled many men around the world to heal from infertility and experience the joy of being a father. What allows us to have excellent results is that we produce all these plants and roots ourselves and that we select only the best plants so that they retain all their therapeutic and medicinal virtues.
2.The fruit of the Tribulus (Tribulus Terrestris)

Tribulus is expected to be very effective in improving sperm count, motility, and morphology when combined with changes in diet and exercise.
The main part of Tribulus that contributes to fertility in men is a constituent called protodioscin. This constituent improves the levels of DHEA in the male body. In men with erectile dysfunction, their DHEA levels have been found to below. Some studies have shown that protodioscin, extracted from Tribulus, increases the natural levels of DHEA necessary for a proper erection. Protodioscin is also the main constituent responsible for the aphrodisiac qualities of Tribulus. The increase in sexual desire while using this herb has been reported by both men and women.
A study by dawabio experts showed a 61% increase in conception in couples with anti-sperm antibodies (the immune system attacking sperm) taking Tribulus. The average duration of conception for a couple after treatment was 5 months. Tribulus is one of the best herbs for improving male fertility. Tribulus supports the production of LH and testosterone in men.
It also helps increase sperm count, motility, and health. It reduces the effects of anti-sperm antibodies.
3. Ginseng
Ginseng is often referred to as the king of all herbs and is proven to be the panacea for improving overall well-being. Ginseng is also an aphrodisiac and is used to treat sexual dysfunction and to improve sexual behavior in traditional Chinese medical practices. Data from animal studies have shown a positive correlation between ginseng's performance, libido and copulation, and these effects have been confirmed in case-control studies in humans. In addition, ginseng improves the quality of sperm and their number. We highly recommend it.
4. Maca

Maca has the ability to improve female fertility, which is why it is getting a lot of attention. It balances female hormones to improve fertility. However, this herb also has the ability to boost male fertility. This plant effectively improves the quality of sperm (the poor quality of sperm is a cause of male infertility). According to a study, men who consume maca regularly have more mobile sperm, more semen and more semen per ejaculation.
5. Ashwagandha

Ashwagandha is traditionally used to improve sexual health. It supports the endocrine system and promotes its better functioning. It also strengthens the hormonal balance in the body. It stimulates libido and improves sperm count in men. It improves stamina and also improves sexual performance.
The natural treatment that we offer to cure asthenospermia consists essentially of natural herbal teas. The herbal tea is composed of plants and roots whose active ingredients can restore the male hormonal balance, by increasing the level of testosterone, the number and the mobility of your sperm. It is the miracle solution to cure asthenospermia.
To discover our natural remedy to cure asthenospermia, click here
Causes of asthenospermia
As with all semen abnormalities, the causes of asthenospermia can be numerous:
- a morphological anomaly of the male gametes,
- an infection,
- presence of anti-sperm antibodies
- medication,
- a varicocele,
- a dietary deficiency,
- a renal failure,
- liver failure
- chemotherapy,
- exposure to radiation,
- excessive alcohol consumption,
- a deficiency in calcium, vitamin D or trace element ...
Symptoms
Asthenospermia does not show any symptoms other than difficulty conceiving.
Diagnostic
A semen analysis, or spermogram, is used to assess the mobility of the sperm. It should be remembered that only mobile gametes can fertilize the egg. Many medical analysis laboratories rely on the classification issued by the World Health Organization to classify spermatozoa:
- Level A (or I): progressive rapid sperm advance quickly and in a straight line,
- Level B (or II): the slow progressive spermatozoa advance slowly or in a curved line,
- Level C (or III): non-progressive spermatozoa move but do not progress,
- Level D (or IV): the sperm are immobile.
To be qualified as normal, the spermogram must show a minimum of 40% of motile sperm and 32% of sperm showing progressive mobility.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
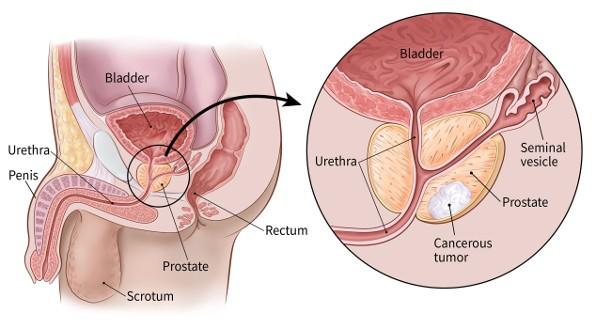
PROSTATE CANCER AND IMPOTENCE: Natural Treatment
Prostate Cancer and Impotence: Natural Treatment
Prostate cancer is the most common cancer, both in men and in the general population.
The prostate is a gland in the male reproductive system that plays a hormonal role and in the production of sperm. The appearance of cancer prostate is the transformation of prostate cells. Initially healthy, they multiply in an anarchic manner until they form a malignant tumor. In 95% of cases, cancers are in the histologic form of adenocarcinoma which develops from the cells making up the lining tissue of the prostate. If cancer starts out in the prostate, the tumor can then grow and invade other parts of the body. The course of this patient is often slow. As with all cancers, there are several stages of development. The evolution of cancer can be local or distant depending on the time of diagnosis. Prostate cancer can range from stage 1 to 4 depending on how widespread it is. To avoid having to suffer from this ailment which could have an impact on your whole life, we suggest that you approach Dawabio experts who are specialized in traditional treatments; as soon as you feel even a little pain or have doubts about your state of health. Here is the natural herbal treatment to permanently cure prostate cancer. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
What are the symptoms of prostate cancer?
This cancer is sometimes never discovered during the patient's lifetime. It is therefore only at a more advanced stage of development that the first symptoms appear. In the majority of cases, these are mainly urinary symptoms that affect urination (the action of urinating):
<> urge to urinate, excessive frequency of urination, painful urination, hematuria, acute retention of urine, dysuria. Difficulty urinating: difficulty starting to urinate or holding urine, inability to urinate, need to urinate frequently (especially at night), poor urine output, a burning sensation or pain when passing urine 'urinate. Blood in urine or semen. Frequent pain or stiffness in the lower back, hips, or upper thighs. Changes in urinary function: frequent urge, urge to urinate, urge to push, retention of urine, burning while urinating. Genital changes: painful ejaculations, or difficulty getting an erection. Predisposed people. benign prostatic hyperplasia. This enlarges, causing abnormalities in the functioning of the bladder and the sexual system. Thus, we can observe both urinary disorders (frequent urges to urinate, decrease in the force of the jet ...) and, often, more or less severe erection difficulties.
Prostate cancer does not cause sexual difficulties at the time. Rather, it is the treatment (intervention, certain medications, etc.) that can have repercussions on sexuality.
Treatment
It is possible to treat the prostate by a gentler method than surgery: ultrasound. This method called "ablatherm" or High-Intensity Focused Ultrasound consists of high-intensity ultrasound focused on the tumor. However, it remains less frequent and around fifty clinics or hospitals offer it in France.
Promising treatments
Certain molecules hold hope in the treatment of advanced forms, such as olaparib. The immunotherapy is also tested to boost the patient's immune system during chemotherapy.
Doctors also have other weapons at their disposal, such as hormone therapy which blocks the development of cancer by reducing the level of male hormones, or radiation therapy.
Several options are available to the doctor for treating prostate cancer, depending on its stage and speed of progression: resection surgery, external or internal radiotherapy (brachytherapy) or even simple monitoring. All these treatments should be discussed with the patient according to their risks and benefits. Thus, the risk of erectile dysfunction, more or less important depending on the treatment chosen, often comes into play in the decision.
Consequences of the operation
The operation often leaves after-effects. During the prostatectomy, the nerves of the erection can be damaged. This results in impotence in 60-90% of patients. But sometimes the erection can be recovered. It depends on the age and the damage to the erectile nerves. When this is not the case, there are treatments to cure impotence.
Another negative consequence of the operation: its impact on the urinary tract. The sphincters which allow the evacuation of urine are very close to the prostate. And when the prostate is removed, they are often damaged. Of urinary leakage appear mostly to the effort.
What are the risks of becoming impotent after prostate cancer surgery?
"It all depends on the treatments but there is a risk of impotence with the surgery. Now when the diagnosis is early enough, the surgery is a minimum. There are minimally invasive surgeries that allow preserving the shameful nerves. It is absolutely necessary to do so. talk with the doctor. There is less risk with irradiation or hormonal treatments but it all depends on the clinical case. If there is a loss of erection after the operation, there are still ways to 'intervene. If the shameful nerves have been preserved, one can act on the libido. Medicines can also help erection. Intra-cavernous injections and possibly penile prostheses can also be considered. But we must talk about it and we must especially not treat ourselves because we fear this kind of problem.
"Prostate cancer is very treatable if caught on time. However, impotence can be a complication of prostate cancer treatments and have an impact on the daily life of the cancer patient.
Several factors can increase the risk of impotence after the operation of prostate cancer, age, but also the frequency of sexual intercourse and erections: if they were low before the operation, this will increase the risk of impotence.
However, in some cases, impotence can be long-lasting. Treatments are then offered to bypass it such as injections and tablets.
The sooner the prostate cancer is treated, the lower the risk of impotence after the procedure.
Typically, impotence decreases and resolves within 18 months after the operation.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
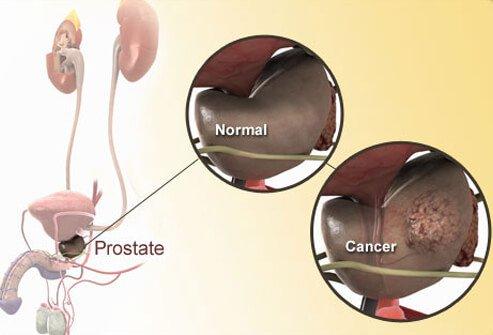
PROSTATE CANCER AND FERTILITY: Natural treatment
PROSTATE CANCER AND FERTILITY: Natural Treatment
The prostate cancer is common cancer affecting the prostate, a gland in the male reproductive system. Cancer develops from the tissues of the prostate when cells there mutate and multiply out of control. These can then spread (metastasize) by migrating from the prostate to other parts of the body, especially the bones and lymph nodes in the pelvis.
Men with fertility problems are statistically more likely to develop prostate cancer than others, according to a Swedish study, which strengthens the hypothesis that these two health problems could have common causes. However, Dawasanté experts have a natural herbal treatment available to treat prostate cancer and improve fertility. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Herbal remedy for prostate cancer
Here we offer you a mixture of seeds, roots, and bark from Africa that can prevent and cure cancer (breast cancer, liver cancer, prostate cancer, tyroid cancer, cervical cancer. uterus, kidney cancer) and cardiovascular disease. These plants are very little known to scientists and they have extraordinary qualities against cancer. Their use against cancer is much more effective than chemotherapy.
Rich in antioxidants and trace elements, our plants for curing cancer delay the development of cancer cells thanks to a pigment it contains, phycocyanin. The root extract very selectively kills cells. Healthy cells are not killed, while cancer cells are. Our natural treatment kills cancer in an all-natural way without nausea, weight loss, or hair loss, while protecting the immune system.
No one can tell you that these herbs definitely cure any type of cancer, that would be lying. But thanks to these plants, you can improve the quality of life of patients by cancer, a fact verified. Best of all, they can even relieve some symptoms of cancer! How does it work?
These African plants are powerful antimicrobials and antifungals. They make it possible to stop metastatic processes by reducing the size of the tumors. This will significantly slow the advance of cancer.
However, even if these roots are very effective, we recommend that you accompany them with conventional treatments. We are definitely not asking you to give up your cancer treatment. Indeed, one should never completely leave aside a medical treatment to start a therapy resulting from the natural African herbal medicine. You will put your health and your life in danger. Our natural anti-cancer treatment should be combined with conventional therapy.
Sexuality and fertility
Prostate cancers and their treatments influence sexuality and fertility. Dedicated support for sexuality is in place, as well as measures to prevent infertility if you are considering a fatherhood project.
There is no harm or risk of having sex during treatment. In the case of brachytherapy treatment with permanent implants (iodine 125 grains), your doctor will give you the recommendations for protecting sexual intercourse. In addition, in the event of radiotherapy, chemotherapy, or hormone therapy, during treatments and six months after the end of treatments, it is necessary to use a suitable means of contraception (for you or your partner) in order to avoid any risk of fertilization from an altered sperm.
SEXUALITY DURING AND AFTER CANCER
After diagnosis, stress, worry, and fatigue often lead to decreased desire. But sexuality is not limited to sexual relations, it encompasses affection, tenderness, speech ... and over time, desire often returns little by little.
Physical difficulties, in particular erectile dysfunction or urinary continence, may appear. They are variable and depend on the erectile and urinary problems that you may have had before the treatments, as well as the treatments received. Erectile dysfunction can appear immediately after treatment or more gradually, in the months or even years that follow. Do not hesitate to talk to your medical team and ask all your questions. Doctors and health professionals are used to this type of request and will direct you to the solutions adapted to your situation and your needs.
If it is difficult to get an erection sufficient to have sex, you may be offered different treatments. Some are to be taken by mouth (5-phosphodiesterase inhibitors); others are injected into the cavernous bodies at the base of the penis (we speak of intracavernous injections), still others are presented as a gel to be inserted into the urinary meatus. A vacuum pump can also be a way to get erections.
FERTILITY
Cancer treatments most often lead to loss of fertility. If you are considering fatherhood, talk to your doctor before starting treatment in order to implement fertility preservation measures.
Freezing (cryopreserving) sperm is the most effective way to preserve male fertility before cancer treatment. The most common way to collect the semen sample is through masturbation. Men who cannot ejaculate can have vibratory or electrical stimulation to help them do so. The semen will stay frozen or stored until you need it. Freezing, even for many years, does not damage the sperm.
According to the Prostate Cancer Treatment Guide, hormone therapy generally has the lowest risk of fertility loss. If fertility problems exist, they will usually only be apparent during treatment. Then the ability to produce sperm should return to normal. For those undergoing radiation therapy, the risk of fertility loss is highly dependent on the dose of radiation received. If fertility can return to normal, it may take up to five years. What is promising, however, is that more precise dosage planning has started to reduce this risk of infertility, the PCF noted.
Infertility
Infertility or the inability to conceive is a potential side effect of prostatectomy or radiation therapy.
The surgery involves removing the prostate as well as the seminal vesicles that produce semen. Men who have had a radical prostatectomy can still reach orgasm but without ejaculation.
Radiation therapy can affect the transport of semen. Men who want to father a child should consider freezing their sperm.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.

PROSTATE CANCER DIET: Natural treatment
What is Prostate Cancer?
The prostate is a gland in the male reproductive system. It is located just below the bladder and, like a ring, it surrounds the urethra, the channel through which urine and semen exit the body. The role of the prostate is to produce prostatic fluid, one of the components of semen along with seminal fluid and sperm, to temporarily store semen before ejaculation, and then to contract at the time of ejaculation, thus participating in the process. expulsion of semen.
Prostate cancer is the most common type of cancer in men: it is estimated that 1 in 7 men will be diagnosed with it, most often in their sixties. Although no specific cause has been discovered, there is a genetic predisposition.
Most prostate cancers grow very slowly. Moreover, the vast majority of men in whom this cancer is detected will die of another cause. Often, the tumor remains in the prostate and has limited health effects, sometimes causing urinary or erectile dysfunction. However, some cancers can grow and spread more quickly.
Treatment
We offer you here a mixture of seeds, roots and bark from Africa which can prevent and cure cancer (breast cancer, liver cancer, prostate cancer, thyroid cancer, cervical cancer. uterus, kidney cancer) and cardiovascular disease. These plants are very little known to scientists and they have extraordinary qualities against cancer. Their use of cancer is much more effective than chemotherapy.
Rich in antioxidants and trace elements, our plants for curing cancer delay the development of cancer cells thanks to a pigment they contain, phycocyanin. The root extract very selectively kills cells. Healthy cells are not killed, while cancer cells are. Our natural treatment kills cancer in the all-natural way without nausea, weight loss, or hair loss while protecting the immune system.
No one can tell you that these herbs definitely cure any type of cancer, that would be lying. But thanks to these herbs, you can improve the quality of life of cancer patients, a proven fact. Best of all, they can even relieve some symptoms of cancer.
Click on the image below to discover our treatment against prostate cancer
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Food and Nutrition
Good nutrition can help reduce the risk of prostate cancer, slow disease progression, and prevent aggressive disease. In this section, we discuss healthy diet recommendations for good prostate health and healthy diet guidelines during treatment for prostate cancer. However, these tips should never be used as a substitute for treatment.
Healthy diet
We know that improved nutrition reduces the risk of heart disease, cancer, diabetes, and obesity and generally improves the overall quality of life. It is estimated that one-third of cancer deaths are attributable to the diet of adults, including the effects of diet on obesity. In addition, a healthy diet helps increase energy levels, aids recovery and strengthens the immune system. According to the World Health Organization, a person with a body mass index (BMI) of 30 or more is considered obese.
Experts now believe that our diet choices account for the vast majority of prostate cancer cases. It is important to assess food choices when it comes to prostate cancer risk. Scientists have discovered a list of anti-cancer superfoods and supplements to optimize your diet while discovering foods and supplements that may actually contribute to cancer risk and aggression.
Guidelines for healthy eating
Your diet should be:
- Mainly herbal
- Include lots of fruits and vegetables
- Rich in fiber
- · Low fat
- Limited in the number of simple sugars
Diet tips for prostate health
Eat fruits and vegetables
Fruits and vegetables contain large amounts of substances that fight cancer and reduce inflammation, such as vitamins, polyphenols, antioxidants, minerals and natural fibers. Most men and women do not eat the recommended daily allowance of fruits and vegetables. If you are working to change the way you eat, try to make manageable changes. Try to include a variety of fruits and vegetables in your diet.
· Cruciferous vegetables (such as broccoli, cauliflower, Brussels sprouts, kale and cabbage) have phytochemical properties that reduce oxidative stress or oxygen free radicals in the body, reducing the risk of prostate cancer and its aggressiveness.
· Carrots are rich in nutrients and contain beta-carotene and antioxidants falcarinol that reduces cancer risk
· Tomatoes are a rich source of a phytochemical called lycopene, which attacks free radicals and helps the body reduce the risk of prostate cancer and its attacks.
· The fungi help the fight against cancer by strengthening the immune system with a set of compounds called beta-glucans and proteins called lectins, which have demonstrated their ability to attack cancer cells
Pomegranate, especially pomegranate juice, has been shown to slow down PSA doubling time and may help prevent recurrence of prostate cancer after primary treatment.
· Grapes and grape juice are rich sources of resveratrol, a type of natural phytochemical that belongs to a larger group of phytochemicals called polyphenols, which have potent antioxidant and anti-inflammatory properties.
· Grapefruit contains several phytochemicals, including naringin limonin, beta-carotene and lycopene
· Oranges, lemons and other citrus fruits help protect against free radicals DNA damaging because they contain hundreds of bioactive compounds, including flavonoids and monoterpenes
Avocados contain the highest amount of luteinutein carotenoid of all fruits
· The peppers and jalapenos contain a chemical, capsaicin, which neutralizes some carcinogens
· Apples are a good source of fiber, vitamin C and contain quercetin, a flavonoid that has both anti-oxidant and anti-inflammatory.
· Berries (raspberries and blueberries) are an excellent source of vitamins C and K, manganese and fiber, and blueberries are among the fruits with the highest antioxidant power due to the many phytochemicals they contain.
v Limit the consumption of animal proteins
Diets high in red meat, dairy products and animal fat have often been linked to the development of prostate cancer. Red meat (such as beef, pork, and lamb) is particularly linked to aggressive prostate cancer.
v Look for vegetable proteins
Plant-based proteins such as beans, flax, and walnuts contain quercetin and lignans which inhibit the growth of many types of cancer, including prostate cancer.
v Green tea
Green tea contains polyphenols and flavonoids which are powerful antioxidants. Tea is the best source of catechins studied for their anticancer properties. Green tea has been shown to slow down and / or prevent the development of prostate cancer.
v Whole grains
Whole grains include brown rice, oatmeal, corn, whole wheat bread, barley, bulgar, kasha, millet, farro, quinoa and more. Whole grains are great sources of fiber and magnesium and provide protein. Choose foods made from whole grains rather than processed foods.
v Limit sugary drinks
Reduce Surgery Soft drinks and clean water can speed up metabolism and rid the body of carcinogens.
v Choose organic foods when possible
Foods from organic farming are free from harmful chemicals and pesticides, including BPA, a known carcinogen of prostate cancer. Foods from organic farming contain more nutrients than they tend to taste better.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
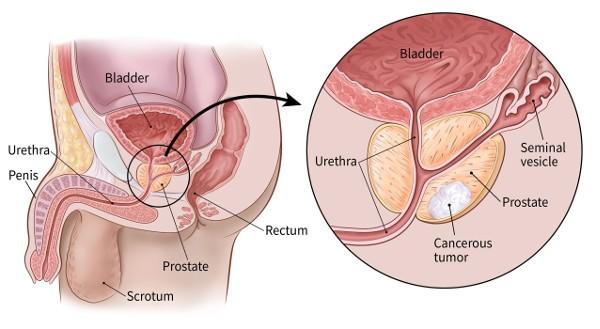
PROSTATE CANCER: TERMINAL PHASE SYMPTOMS
PROSTATE CANCER: TERMINAL PHASE SYMPTOMS
Prostate cancer is the most common cancer, both in men and in the general population. First signs, causes, diagnosis and treatment ... Lighting from Pierre-Olivier Bosset, urological surgeon.
Definition: location and role of the prostate
The prostate is a gland in the male reproductive system that plays a hormonal role and in the production of sperm. The appearance of prostate cancer corresponds to the transformation of prostate cells. Initially healthy, they multiply in an anarchic manner until they form a malignant tumor. In 95% of cases, the cancers are in the histological form of adenocarcinoma which develops from the cells making up the lining tissue of the prostate. If cancer starts out in the prostate, the tumor can then grow and invade other parts of the body.
Stadiums
The course of this disease is often slow. As with all cancers, there are several stages of development. The evolution of cancer can be local or distant depending on the time of diagnosis. Prostate cancer can range from stage 1 to 4 depending on how far it has spread. It is with a view to saving more human lives that Dawasanté experts provide you with a mixture of seeds, roots and bark from Africa to prevent and cure prostate cancer. Click on the image below to discover this natural treatment

Prostate cancer in numbers
Cancer of the prostate is the most common cancer. In 2015, 50,430 new cases were diagnosed (InVs figures). With 8,512 deaths in 2015, it ranks third among cancer deaths in humans. More than 5 out of 10 prostate cancers are linked to a hereditary predisposition. The average age of prostate cancer is around 60-70 years, but some men are affected at an earlier age. A decrease in mortality from prostate cancer has been observed since 2000. The improvement in treatment largely explains the reasons for this decrease.
Symptoms
Often, early-stage prostate cancer does not have any symptoms or signs. It is usually detected by a PSA scan or by a DRE, a process called detection. If prostate cancer is suspected based on a PSA or DRE scan, more checks and tests are needed to diagnose prostate cancer. When prostate cancer effectively causes symptoms or signs, it is usually diagnosed at a later stage. These signs and symptoms include:
Frequent urination
Poor or interrupted urination flow, or need to exert force to empty the bladder.
Urge to urinate frequently at night.
Blood in the urine
Blood in seminal fluid.
· New appearance of erectile dysfunction.
Pain or burning sensation when urinating, which is much less common.
Discomfort or pain when sitting caused by an enlarged prostate.
- voiding pain,
- hematuria,
- dysuria.
Sometimes men with prostate cancer don't have any of these changes. Other non-cancerous prostate conditions, such as BPH or an enlarged prostate, can produce similar symptoms. Or the cause of these symptoms may be some other medical condition other than cancer. Urinary symptoms can also result from a bladder infection or other conditions.
If cancer has spread outside of the prostate, a man may feel:
Pain in the back, hips, thighs, shoulders, or other bones.
Swelling or accumulation of fluid in the legs or feet.
· Weight loss for no apparent reason.
· Tired
· Change bowel habits.
If you are concerned about any changes you have experienced, tell your doctor Your doctor will ask you since when and how often you have had the symptom (s), among other questions. This helps to find the cause of the problem, which is called the diagnosis.
This cancer is sometimes never discovered during the patient's lifetime. It is therefore only at a more advanced stage of development that the first symptoms appear
PSA screening and assay: recommendations on age and frequency
As age is a major risk factor, men over 60 are subject to increased medical surveillance. The rectal examination is the most effective method for detecting the possible presence of a mass in the prostate.
Regularly or in case of doubt, the doctor also recommends a blood test of the level of Prostate Specific Antigen (PSA), the main reflection of the functioning of the prostate gland. " In the interview, it is also necessary to look for other risk factors for prostate cancer: family background (history of prostate cancer) and ethnic origins (DOM-TOM, Africans) ", explains Dr. Pierre-Olivier Bosset, surgeon urologist. The PSA assay, a prostate-specific antigen, is a protein produced exclusively by the prostate which makes it possible to suggest the diagnosis and to monitor the progression of prostate cancer. This is a very sensitive assay in cancer screening.
THE PHASES OF CANCER
The stages of cancer range from the first mutations of cells until the disease reaches its final stage. This is known as natural history.
WHAT ARE THE PHASES OF CANCER?
The duration of this process in adults depends on the type of cancer and ranges from a few months to several decades. In the case of children, this whole process goes much faster and may even last only a few months. In fact, the cells that make up tumors in children are more immature cells that divide and multiply more quickly than those that make up adult cancers so that tumors develop and grow in children. in a short period of time.
STEP 0
The first thing that happens is the cellular changes that give the cells the characteristics of malignancy, that is, uncontrolled multiplication and the ability to invade. This is the longest phase of the disease and is called the induction phase. In no case is it diagnosable or produces symptoms. This phase can last up to 30 years.
STEP I
The second step is called the "in situ" phase. It is characterized by the existence of the microscopic cancerous lesion located in the tissue where it originates. In adults, it usually lasts between 5 and 10 years depending on the type of cancer.
In it, there are no symptoms or discomfort in the patient. In some cases, such as breast, cervical or colon cancer, the disease can be diagnosed at this stage using techniques that allow for early detection.
STEP-II
Subsequently, the lesion begins to spread outside its place of origin and invades adjacent tissues or organs. We are facing the local invasion phase. In adulthood, it lasts between 1 and 5 years. The appearance of symptoms of the disease depends on the type of cancer, how it is growing, and where it is.
METASTASIS
Finally, the disease spreads outside its place of origin as distant tumor lesions called metastases. This is the stage of the remote invasion. The symptomatology presented by the patient is generally complex. It depends on the type of tumor, location and extent of metastasis.
STEP IV: TERMINAL PHASE
This phase is characterized by the existence of advanced, irreversible and irreversible (incurable) cancer. It is also referred to as terminal cancer.
It does not respond to commonly used treatments. It is accompanied by multiple symptoms that cause great discomfort in the patient, affecting his quality of life and that of his family.
It is a time of intense pain, but also of transcendental importance. If the patient and his family have prepared, this time makes it easier to reunite with oneself and with loved ones.
The area of medicine that deals with the care of patients at this stage of illness is that of palliative care or palliative medicine.
HOW DOES CANCER EVOLVE?
The course of each cancer is subject to multiple factors that will interact with each other. These factors vary depending on the tumor and the patient.
Remember that " there are no diseases, but sick people ."
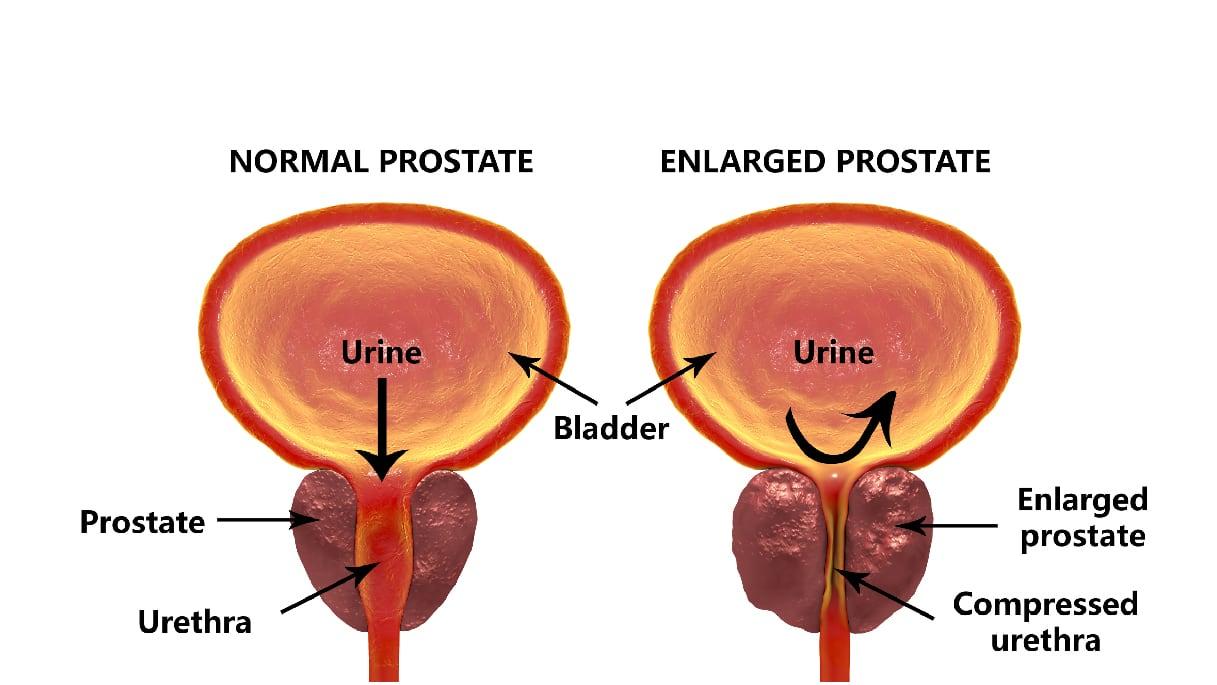
PROSTATE CANCER AND RADIATION THERAPY
PROSTATE CANCER AND RADIOTHERAPY
General
The prostate cancer is cancer frequently touching the prostate, a gland of the reproductive system of man. Cancer develops from the tissues of the prostate when cells there mutate and multiply out of control. These can then spread ( metastasize ) by migrating from the prostate to other parts of the body, especially the bones and lymph nodes in the pelvis.
Malignant prostate cancer occurs independently of benign prostatic hyperplasia (BPH), or prostatic adenoma. In the vast majority of cases, it is an adenocarcinoma, especially of the acinar type. However, Dawasanté experts have a natural African plant-based treatment to permanently cure prostate cancer and the effects of radiotherapy. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Malignant prostate cancer can cause pain, difficulty urinating, and erectile dysfunction, among other things. Symptoms originating from an adenocarcinoma of the prostate often signal an advanced stage of the disease. Other prostate diseases cause the same symptoms: pelvic pain in prostatitis and difficulty urinating in BPH.
The most common treatments are surgery (radical prostatectomy), radiotherapy ( external radiotherapy and brachytherapy, in particular) and hormone therapy. The chemotherapy is used only in advanced forms. Here we will talk about radiotherapy. However, if you feel the need to be analyzed and treated, the Dawabio center is at your disposal to provide you with a treatment worthy of the name, natural of course.
Causes, risk factors
Its causes are still poorly understood, and could often be multiple:
- a genetic predisposition and the responsibility of certain genes seem possible but weakly correlated with the onset of the disease.
In particular, a mutation on chromosome 8 could explain the greater frequency of this cancer in black Americans; - A link with bioavailable testosterone seems frequent. Charles Brenton Huggins (inventor of hormone therapy for cancer) first (from the 1940s and based on studies of metastatic prostate cancer) concluded that this cancer was induced by excess testosterone (or facilitated by this hormone). But more recently (the 2010s) the available data suggests that a more common cause is testosterone deficiency. Low testosterone before surgery for this cancer was linked in 2010 to an increased risk of tumor aggressiveness
- higher adult height correlates with a higher risk of prostate cancer;
- Nutritional factors have been mentioned. Certain foods seem to increase the risk of prostate cancer;
According to several studies, the consumption of cow's milk increases this risk after 50 years, but other studies consider that this link is not significant or would be weak. The increased risk appears to be related to the increased level of IGF-1 in the blood, which itself correlates with milk consumption. Some studies suggest that casein may also have an effect on prostate cancer. Excessive dietary intake of phytanic acid from dairy products, especially butter has also been linked (2012) to a high risk of prostate cancer; for these reasons, in the name of the precautionary principle, the consumption of dairy products is no longer recommended for men. Overconsumption of calcium appears to be an established risk factor. Several scientific studies retain milk as a risk factor for hormone-dependent cancers such as those of the prostate, ovaries and breast.
Other foods seem to play a protective role; the lycopene for example, dried fruits, legumes ;
- similarly, physical exercise may have a slightly protective effect;
- an endocrine disrupting effect of certain products ( pesticides in particular) could be involved;
- exposure to pesticides is a possible factor because agricultural populations are over-represented for this cancer, which remains etiologically poorly understood, and which therefore still requires research, in particular on gene-environment relationships and interactions . The cadmium very present in phosphate fertilizers could also be involved;
- The smoking ;
- a viral infection could sometimes be involved (unless it is favored by the process of cancerization or a decrease in immunity which also favored cancer);
the XMRV retrovirus ( Xenotropic MLV - Related Virus, variant of MLV ( murine leukemia virus responsible for leukemia in mice) and capable of infecting humans, was detected in 2006 in certain tumors of the prostate. It belongs to the gammaretrovirus genus already associated with leukemia and certain cancers in rodents, felines, and primates.
According to a US study published in 2010 and involving 334 human prostate tissue samples, proteins appearing to come from this virus were found in 23% of cancerous tissue (against 4% of "healthy" samples). And they were more present in the more aggressive tumors. It remains to be identified whether the virus is the cause or one of the causes of these cancers or if it infects the prostate of patients because they have previously weakened immunity. If it is involved, we may have additional biomarkers for this cancer or even new avenues of prevention; - The night work is also mentioned (as for other cancers called "hormone").
- according to a study published in 2004, more frequent ejaculations are associated with a reduced risk of prostate cancer.
What are its symptoms and how is it detected?
This cancer is most often asymptomatic, that is to say, it is discovered when it does not cause any manifestation of its own. It is most often found:
- during blood tests including the study of PSA (specific antigen of the prostate, whose predictive value and use, without proven benefit in terms of public health , have recently been called into question). PSA is a protein normally secreted by prostate cells, but a cancer cell secretes 10 times more than a normal cell. This property has raised many hopes in terms of screening. The blood level of PSA can however be increased by many other factors (prostate volume, infections and / or inflammations, mechanical constraints (rectal examination, other) ...) or decreased by certain treatments for benign hypertrophy ( finasteride). The significance thresholds are therefore difficult to establish. It is accepted, however, that a PSA level of between 4 and 10 ng/ml is doubtful, but that it is clearly significant beyond. Some authors have proposed to relate the rate to the effective weight of the prostate or to assess the free PSA / total PSA ratio, or even the growth kinetics of the rate over 2 years.
A still uncertain marker for screening, the PSA level is, on the other hand, an essential indicator for the monitoring and treatment of declared cancers; - during a digital rectal examination; performed routinely, or due to symptoms related to another disease (in particular benign prostatic hypertrophy);
- fortuitously, on parts of prostatic resection during the surgical treatment of prostatic adenoma.
When symptomatic, prostate cancer is most often at an advanced stage. It can lead to:
- acute urinary retention ;
- hematuria ;
- sexual impotence (erectile dysfunction);
- a deterioration of the general condition ;
- of pain and/or the malfunction or failure of other organs related to the presence of metastases .
Radiotherapy is one of the treatments conventionally offered in prostate cancer
External or internal radiotherapy?
A second option in the treatment of localized prostate cancer is radiation therapy.
Two types of radiotherapy are used to treat this pathology, external radiotherapy and internal radiotherapy also called brachytherapy or brachytherapy.
The external radiation corresponds to conventional radiation: radiation from an external source are directed so focused on the patient's tumor. The dose of radiation needed to destroy the tumor is delivered over several sessions, often five per week for one to two months.
Internal radiation therapy is based on the implantation of radioactive needles into the prostate. The needles are put in place during surgery, under general anesthesia. This method has the advantage of sparing the organs neighboring the prostate since the radioactive radiation is delivered directly into the prostate gland.
The various complications of radiotherapy are described in the chapter devoted to radiotherapy and accessible in the treatment section itself in the health section of the site.
External radiotherapy and brachytherapy are among the potentially curative therapeutic modalities offered in the treatment of non-metastatic prostate cancer. Few data have been published on their management and their prevention is essential. An assessment as precise as possible of the risk / benefit ratio is necessary before any treatment decision and clear and objective information for the patient must be made, including the risk of late morbidity and the possible impact of late side effects on quality of life.
The immediate digestive side effects during irradiation are very frequent and almost constant even if they are mostly very moderate and with limited impact. They consist of transit disorders sometimes linked to enterocolitis and accompanied by abdominal pain and above all by a rectal syndrome with a fractionation of the stools which become mucus and some false needs. Patients with hemorrhoids develop anal discomfort earlier and more readily, sometimes with bleeding and should be treated early.
Most of these side effects disappear a few weeks after the end of the irradiation.
Late complications are much rarer, around 7 to 10% for grade 1-2 complications and have become exceptional for serious complications (3.5% grade 3 and 0.5% grade 4). These late complications, when they occur, are essentially anorectal, with the risk of enteritis only occurring when large volumes of hail have been included in a large volume of pelvic irradiation. The evaluation of these complications is done according to the score, LENT SOMA (Late Effects on Normal Tissue Scale) of the RTOG-EORTC:
Grade 1: no change.
Grade 2: mild diarrhea; some colic pain; less than 5 bowel movements per day; mucus stool.
Grade 3: moderate diarrhea; more than 5 bowel movements per day; mucous or haemorrhagic proctitis.
Grade 4: obstruction or rectal bleeding requiring surgery.
Grade 5: necrosis, perforation, fistula.
Urinary complications from radiotherapy are rare even if during irradiation, irritative phenomena are very frequent. However, it is the rule not to irradiate a very large adenomatous prostate in patients with high IPSS, otherwise, a retention syndrome may occur during treatment. The removal of the previous obstacle will call for the usual medical or surgical treatments. The start of irradiation should be postponed after a transurethral resection to avoid increasing the risk of urinary incontinence or subsequent stenosis and will not begin until after complete healing of the resection pocket, generally in the third month.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
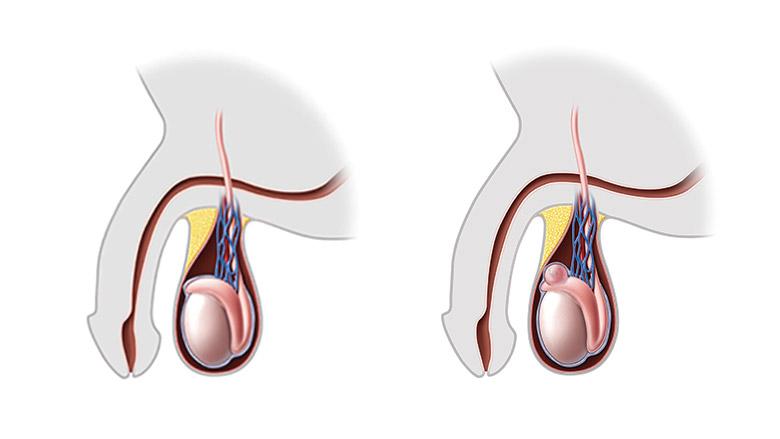
Epididymis cyst: causes, symptoms, natural remedies and advice
The epididymis (from the Greek epididumis) is an organ of the male reproductive system located in the wall of the testicle.
The epididymis cyst or also called testicular cyst or spermatocele. Develops at the expense of the swollen part of the upper part or head of the epididymis. There may be one or more cysts within the same epididymis. Epididymal cysts can occur at any age. The epididymis is located in the wall of the testicle and is essential for the maturation and transport of sperm. Relatively frequent, these cysts are sometimes very painful and require an intervention.
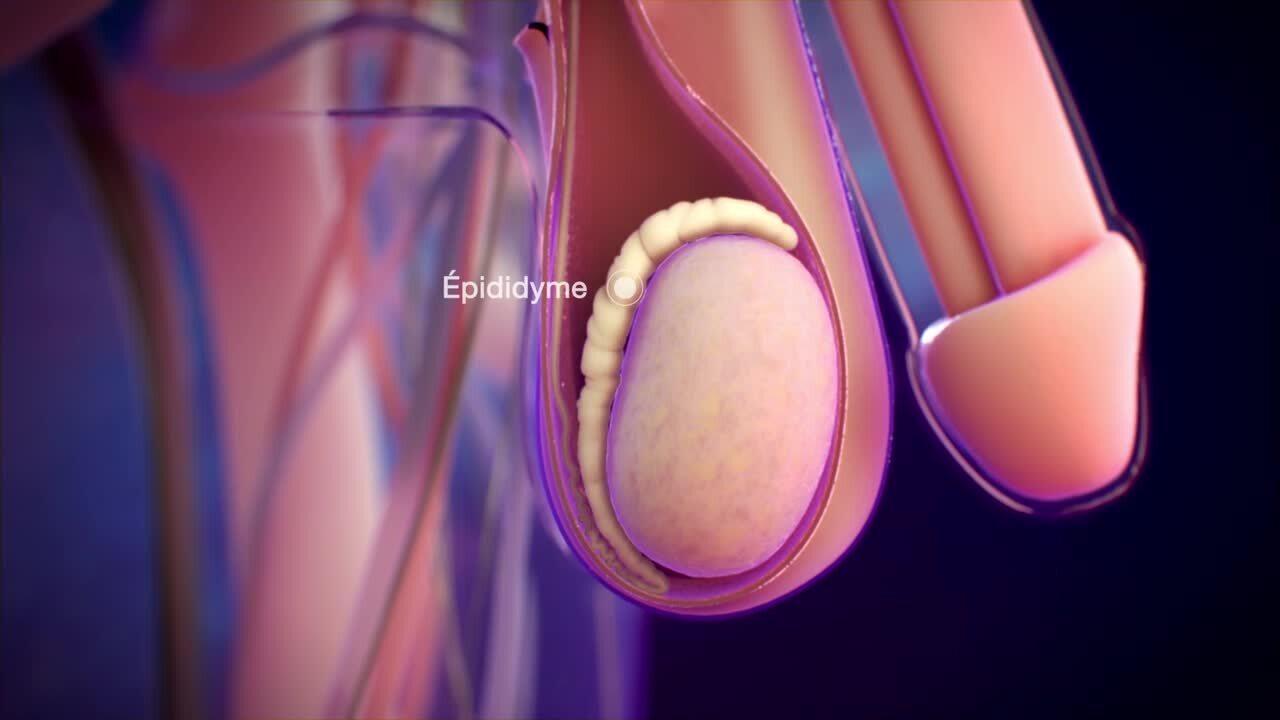
However, the experts of Dawasanté provide you with a natural treatment based on medicinal plant to cure definitively the cysts of the epididymis without surgery. Click on the image below to discover this natural treatment.

The testicular cyst in men is a benign neoplasm.
The appendix itself is a long, narrow canal that serves to develop, accumulate and promote sperm. It also produces the fluid necessary for the maturation and motor activity of male sex cells. Under normal conditions, should be emptied regularly exit channels of male sperm in good body health, but under certain violations of the dander filled with sperm, and it appears cystic formation with capsular connective tissue sheath.
Further increase in the cyst causes excessive pressure on the vas deferens of the epididymis, which leads to disruption of the normal flow of seminal fluid. This can cause a breakdown in reproductive function in men.
Epididymal cysts usually originate in adolescence, progressing and developing over time. The peak of development occurs at the age of 30 to 40 years and by the age of 50 years, a full clinical picture of the disease has been observed, which can affect about 30% of the total male population. It is often caused by a sexually transmitted infection (STI) but can also have other causes
We have a very effective natural treatment to cure epididymal cysts permanently.
Order it and start the natural Epididymal Cyst treatment early. Support is offered during the whole period of its intake. To reach us, click on the WhatsApp button in the right corner of your screen or contact us at +229 66 23 89 56
We have representation in all African countries and actively in the following countries: Cameroon, Ivory Coast, Mali, Senegal, Burkina Faso, Togo, Kenya, Nigeria, Gabon, Central African Republic, Benin, Chad, Congo-Brazzaville and Kinshasa. So rest assured that you will receive your products immediately after your order.
Delivery is free of charge anywhere in the world.
Causes of the epididymis cyst
There are several reasons and options for the development of epididymis cysts:
Epididymis cyst may form before birth, as a result of some defects in the period of intra-uterine growth of the embryo (for example, non-infection of the parameconephrotic canal). Cysts of this type contain a sperm-free fluid in their cavity;
The formation of epididymis cysts in 40% of cases can be preceded by scrotal traumatic lesions, infectious and inflammatory processes in the genital region, which lead to the coalescence of one or two deferential ducts. As a result, the output of seminal fluid overlaps, and the accumulation of male sex cells in the channel light. The walls of the canal, respectively, are stretched and a cyst is formed, containing in its cavity seminal fluid accumulated with neutral or alkaline activity.
In addition to sperm, lipid cells, leukocytes and epithelial particles can be found in the contents of the cyst, from which the walls of the cystic cavity are aligned.
- Ethnic and socio-economic causes:
Several studies have shown the impact of these factors in the occurrence of MIT, without showing the causal link. Predominance in black males, and low socioeconomic status was observed.
- Genetic Causes:
Several genes are implicated in the occurrence of MIT: +Senseless mutation of the gene Phosphodiesterase 11A(PDE11A) which encodes a protein that plays a role in regulating the intracellular concentration of cAMP and cGMP. [34] + other mutations of other genes have been identified including the mutation of the gene SLC34A2 and GALNT3, both encode a protein involved in phosphate transport and metabolism
- Family history of first degree.
Other contributing factors are discussed such as certain environmental factors such as maternal estrogen intake during pregnancy, exposure to certain chemical industry substances, or to certain substances in the environment (insecticides, herbicides).
- Atypical acute scholarship:
The problem arises in a young man with an acute sore bursa, but without the clinical signs characteristic of a twisted spermatic cord or an orchi-epididymitis. This is the problem of differential diagnosis with a germinal tumor with acute revelation (about 10% of testicular tumors).
- Important risk factors include:
Factors that increase the risk of testicular cyst vary due to various causes of testicular abnormalities. History of testicular cancer or contralateral intratubular germinal neoplasia.
The presence of gonadal dysgenesia syndrome associating more or less:
a history of cryptorchidia (homo- or contralateral). Present in almost 10% of cases, it multiplies the cancer risk by 5 to 10 times depending on the age and date of treatment. Surgical testicular lowering, if it does not reduce the risk of cancer, has the advantage of facilitating testicular palpation;
. testicular atrophy;
. a hypospade;
. Fertility problems.
. Klinefelter syndrome.
. Infertility.
Testis not lowered or retracted
An undrawn testicle does not leave the abdomen and does not enter the scrotum during fetal development or early childhood. A retractable testicle descends into the scrotum but withdraws into the abdomen. Either may increase the risk of:
- Inguinal hernia
- Testicular torsion
- Testicular cancer
- Anomalies present at birth
- Abnormalities of the testicles, penis or kidneys present at birth (congenital) could increase the risk of scrotal mass and testicular cancer later in life.
Symptoms of epididymis cysts
Epididymal cysts usually have no symptoms before forming in the epididymis. Once formed, you may notice a ball the size of a pea (or larger) behind, above or below one of your testicles where sperm is produced. For spermatoceles, the cyst is usually on the top of the testicles.
Other symptoms of an epididymal cyst may include:
- Dull pain in the scrotum (the pocket containing the testicles)
- A feeling of heaviness in the scrotum
- Redness in the region of the scrotum
- Increased pressure at the bottom of the penis
- Sensitive or swollen epididymis
- Soft, swollen or hardened testicles
- Pain in the groin or lower back and abdomen
Epididymal cysts generally do not present acute and intense pain symptoms and are generally completely painless. If any of the above symptoms occur, a complete and immediate examination by a urologist is warranted.
We have a very effective natural treatment to cure epididymal cysts permanently.
Order it and start the natural Epididymal Cyst treatment early. Support is offered during the whole period of its intake. To reach us, click on the WhatsApp button in the right corner of your screen or contact us at +229 66 23 89 56
We have representation in all African countries and actively in the following countries: Cameroon, Ivory Coast, Mali, Senegal, Burkina Faso, Togo, Kenya, Nigeria, Gabon, Central African Republic, Benin, Chad, Congo-Brazzaville and Kinshasa. So rest assured that you will receive your products immediately after your order.
Delivery is free of charge anywhere in the world.
NATURAL REMEDIES FOR THE EPIDIDYMIS CYST
- Amanita
 You can get rid of the pathology without surgery with the help of Amanita. To dye, you must take fresh mushrooms, clean well so that there is no dirt and forest debris, and put it in a pot to the brim. Pour alcohol on the edges – at least 70%. In extreme cases, you can use regular vodka. After the container is closed and put in a dark place for a period of at least fourteen days. Insist until the liquid acquires a characteristic red-brown hue and a particular smell. As soon as the desired effect is achieved, the dye must be filtered and the resulting liquid poured into bottles.
You can get rid of the pathology without surgery with the help of Amanita. To dye, you must take fresh mushrooms, clean well so that there is no dirt and forest debris, and put it in a pot to the brim. Pour alcohol on the edges – at least 70%. In extreme cases, you can use regular vodka. After the container is closed and put in a dark place for a period of at least fourteen days. Insist until the liquid acquires a characteristic red-brown hue and a particular smell. As soon as the desired effect is achieved, the dye must be filtered and the resulting liquid poured into bottles.
To cure spermatocele in men, it is necessary to follow a certain pattern of consumption of dye, which first increases and then decreases. That is to say, on the first day of administration – 1 drop, the second – 2 and so on up to 15 drops in one dose, then, on the contrary, from 15 drops a day to one at the end. Thus, the duration of treatment should be 30 days.
- Quercetin
 Quercetin can also help fight inflammation associated with the epididymis cyst.
Quercetin can also help fight inflammation associated with the epididymis cyst.
- Arnica Mountain
 Another equally effective alternative therapy method is to add the mountain arnica flowers to a glass of boiling water. Let stand for 2 hours. You should drink 1 tablespoon daily three times a day, but only after eating.
Another equally effective alternative therapy method is to add the mountain arnica flowers to a glass of boiling water. Let stand for 2 hours. You should drink 1 tablespoon daily three times a day, but only after eating.
- Turmeric and Curcumin
 Turmeric and curcumin can help reduce inflammation and can be useful for men with epididymis. Curcumin can be a great help in reducing chronic inflammation, which is good for epididymitis.
Turmeric and curcumin can help reduce inflammation and can be useful for men with epididymis. Curcumin can be a great help in reducing chronic inflammation, which is good for epididymitis.
- Jasmine
 You can also treat a cyst with jasmine. To do this, prepare the ointment. About fifty grams of the plant’s flowers are taken; placed in a bowl and poured with a glass of oil on top (it is best to use olive oil). The mixture must be well infused, so you must wait at least ten days before using the ointment. After this time, the mass must be filtered, after which you can use the tool; it is rubbed daily at the site of localization of the cyst, mainly in the morning. This treatment method works well when combined with other popular remedies; for example, decoctions, dyes, etc.
You can also treat a cyst with jasmine. To do this, prepare the ointment. About fifty grams of the plant’s flowers are taken; placed in a bowl and poured with a glass of oil on top (it is best to use olive oil). The mixture must be well infused, so you must wait at least ten days before using the ointment. After this time, the mass must be filtered, after which you can use the tool; it is rubbed daily at the site of localization of the cyst, mainly in the morning. This treatment method works well when combined with other popular remedies; for example, decoctions, dyes, etc.
We have a very effective natural treatment to cure epididymal cysts permanently.
Order it and start the natural Epididymal Cyst treatment early. Support is offered during the whole period of its intake. To reach us, click on the WhatsApp button in the right corner of your screen or contact us at +229 66 23 89 56
We have representation in all African countries and actively in the following countries: Cameroon, Ivory Coast, Mali, Senegal, Burkina Faso, Togo, Kenya, Nigeria, Gabon, Central African Republic, Benin, Chad, Congo-Brazzaville and Kinshasa. So rest assured that you will receive your products immediately after your order.
Delivery is free of charge anywhere in the world.
- The buchu leaf
 The buchu leaf is also good for treatment as it is a disinfectant and diuretic of the urinary tract. It is used to treat prostate inflammation and urinary tract infections.
The buchu leaf is also good for treatment as it is a disinfectant and diuretic of the urinary tract. It is used to treat prostate inflammation and urinary tract infections.
- Chestnut
 In addition, for the treatment of the pathology, the chestnut juice of the plant flowers is perfect. It is necessary to collect fresh flowers; to squeeze all the juice and to consume 20 drops a day, previously diluted with water.
In addition, for the treatment of the pathology, the chestnut juice of the plant flowers is perfect. It is necessary to collect fresh flowers; to squeeze all the juice and to consume 20 drops a day, previously diluted with water.
- Traditional plantain seed recipes
 The healing properties of plantain are thought to help restore male strength. They will also help get rid of the symptoms and cyst of the testicles.
The healing properties of plantain are thought to help restore male strength. They will also help get rid of the symptoms and cyst of the testicles.
- Flax
 You can also cure the pathology using flax grass. It is necessary to take flax, to press the juice, to add butter (the ratio of the proportions must be of 2: 5) and to light a small fire. The mixture should languish until all the excess liquid has completely evaporated. Use the ointment after it has completely cooled and infused. It is applied as a cream on the testic
You can also cure the pathology using flax grass. It is necessary to take flax, to press the juice, to add butter (the ratio of the proportions must be of 2: 5) and to light a small fire. The mixture should languish until all the excess liquid has completely evaporated. Use the ointment after it has completely cooled and infused. It is applied as a cream on the testic
- Corn silk
 Corn silk is also an excellent herbal remedy for the treatment of epididymis cyst, as it is a powerful antibacterial that also helps to relieve pain.
Corn silk is also an excellent herbal remedy for the treatment of epididymis cyst, as it is a powerful antibacterial that also helps to relieve pain.
We have a very effective natural treatment to cure epididymal cysts permanently.
Order it and start the natural Epididymal Cyst treatment early. Support is offered during the whole period of its intake. To reach us, click on the WhatsApp button in the right corner of your screen or contact us at +229 66 23 89 56
We have representation in all African countries and actively in the following countries: Cameroon, Ivory Coast, Mali, Senegal, Burkina Faso, Togo, Kenya, Nigeria, Gabon, Central African Republic, Benin, Chad, Congo-Brazzaville and Kinshasa. So rest assured that you will receive your products immediately after your order.
Delivery is free of charge anywhere in the world.
- The Goldenseal of Canada
 The Canadian goldenseal is an antibacterial and anti-inflammatory drug used by many in conjunction with other herbs to combat prostatitis. It also fights urinary tract infections.
The Canadian goldenseal is an antibacterial and anti-inflammatory drug used by many in conjunction with other herbs to combat prostatitis. It also fights urinary tract infections.
- Ginger
 Ginger fights prostate cancer cells and can therefore be added to any diet.
Ginger fights prostate cancer cells and can therefore be added to any diet.
- The root of hydrangea
 Hydrangea root is also used as an herbal remedy to promote treatment and relieve symptoms of bladder, prostate and other urinary tract infections, including benign prostate hypertrophy and urethritis.
Hydrangea root is also used as an herbal remedy to promote treatment and relieve symptoms of bladder, prostate and other urinary tract infections, including benign prostate hypertrophy and urethritis.
- The rutin
 Rutin is a flavonoid that reduces inflammation
Rutin is a flavonoid that reduces inflammation
- Extract of juniper berries
 Juniper berry extract excels in urinary tract evacuation, which is very important in case of prostatic hypertrophy. It also helps treat urinary tract infections and prostate infections by activating and cleaning the entire system.
Juniper berry extract excels in urinary tract evacuation, which is very important in case of prostatic hypertrophy. It also helps treat urinary tract infections and prostate infections by activating and cleaning the entire system.
We have a very effective natural treatment to cure epididymal cysts permanently.
Order it and start the natural Epididymal Cyst treatment early. Support is offered during the whole period of its intake. To reach us, click on the WhatsApp button in the right corner of your screen or contact us at +229 66 23 89 56
We have representation in all African countries and actively in the following countries: Cameroon, Ivory Coast, Mali, Senegal, Burkina Faso, Togo, Kenya, Nigeria, Gabon, Central African Republic, Benin, Chad, Congo-Brazzaville and Kinshasa. So rest assured that you will receive your products immediately after your order.
Delivery is free of charge anywhere in the world.
- Dandelion root
 Dandelion root has anti-inflammatory properties that reduce inflammation.
Dandelion root has anti-inflammatory properties that reduce inflammation.
- Parsley
 Parsley is a powerful antioxidant and anti-inflammatory.
Parsley is a powerful antioxidant and anti-inflammatory.
Some tips to relieve and avoid Epididymis cyst
What to do to relieve the epididymis cyst
- Get some rest in bed.
- Lie down so that your scrotum is raised.
- Apply cold compresses to your scrotum if tolerated.
- Wear an athletic support.
- Avoid lifting heavy objects.
- Avoid intercourse until the infection is gone.
Foods to avoid in case of epididymitis
When it comes to eating well to promote healing and relieve the pain of epididymitis and strengthen the health of the testicles, there are certain foods you should avoid.
In general, these are mainly high-fat foods, processed foods, sweet foods and spicy foods. The reason is that these foods feed inflammation.
Foods of the epididymitis to be avoided or restricted include: sugary foods, sweets and artificial sweeteners; caffeine; alcohol; processed foods; white flour products; fast foods; hydrogenated foods, trans fats, Fried foods, fatty foods; margarine; sodas; spicy foods; onions, pepper, mustard, fennel
Foods to eat in case of epididymitis
When it comes to following a diet adapted to the health of the testicles, you should consume foods that fight and reduce inflammation and avoid eating pro-inflammatory foods.
These foods are:
Anti-inflammatory foods for the testicles: Epinards; Blueberries; Strawberries and other flavonoid-rich foods
Foods rich in vitamin C for testicular health: Kiwi; Orange; Watermelon; Lemon; Grapefruit; Bitter melon; Tomatoes
Fiber-rich foods for the testicles: Banana; Sweet potatoes; Celery
Whole grains, nuts, beans and seeds: Walnuts; Flax seeds; Pumpkin seeds
Foods rich in omega-3 fats: Salmon; Mackerel; Herring; Sardine; Rapeseed oil; Fish oil
We have a very effective natural treatment to cure epididymal cysts permanently.
Order it and start the natural Epididymal Cyst treatment early. Support is offered during the whole period of its intake. To reach us, click on the WhatsApp button in the right corner of your screen or contact us at +229 66 23 89 56
We have representation in all African countries and actively in the following countries: Cameroon, Ivory Coast, Mali, Senegal, Burkina Faso, Togo, Kenya, Nigeria, Gabon, Central African Republic, Benin, Chad, Congo-Brazzaville and Kinshasa. So rest assured that you will receive your products immediately after your order.
Delivery is free of charge anywhere in the world.
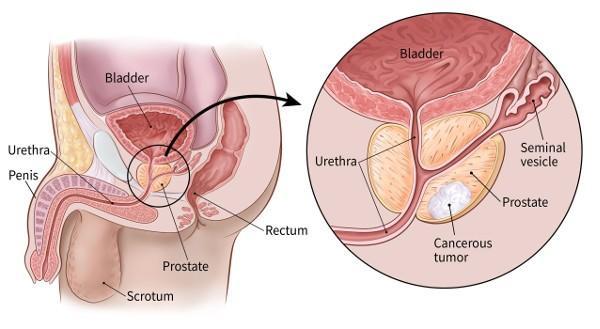
MEDICAL TREATMENT OF THE EPIDIDYMAL CYST
MEDICAL TREATMENT OF THE EPIDIDYMAL CYST
A cyst is a lesion that develops within a tissue or organ. Testicular cysts are benign pathologies that can develop sometimes on the right testicle, sometimes on the left. They particularly affect children and young adults. There are two types of testicular cysts:
Cysts of the epididymis,
Dermoid cysts of the testis.
Cysts of the epididymis are benign tumors of unknown origin. They appear in the form of regular and painless swellings (single or multiple), located at the head of the epididymis.
To permanently cure this disease, Dawasanté experts provide you with a natural treatment based on medicinal plants. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
The cyst of the epididymis grows at the expense of the swollen part of the upper part or head of the epididymis. There may be one or more cysts within the same epididymis.
The intervention is proposed because of the discomfort or local pain that this cyst can cause. It aims to remove the lesion by the surgical opening of the bursa.
The absence of treatment has no consequence in itself, apart from the fact of a possible increase in the size of the cyst, discomfort, or local pain, which it can cause.
Symptoms and Pains
Concerning the cysts of the epididymis, the manifestations are mainly an increase in the volume of the bursa giving the sensation of having "a ball of fat" at this level, most often accompanied by local discomfort. As for dermoid cysts, the most evocative symptom is the increase in the volume of the bursa. Cysts "rarely cause pain, except in cases of large volume," said Dr. Antoine Faix, surgeon urologist and head of Andrology and Sexual Medicine of the French Urology Association Committee.
The spermatocele kystesdu often contain pools of dead sperm. Doctors don't know what is the cause. Often, epididymal cysts or spermatocele cysts develop for no particular reason.
There are no specific causes for the appearance of a cyst.
Most of the time, cysts in the epididymis don't hurt, so you may not have symptoms. You may only feel a lump when you examine your testicles. Your doctor might find it during an exam. As the cyst gets bigger, you may feel a heaviness in your testicle. You might also notice a lump or swelling behind or above your testicle.
Diagnosis: Who to conduct and what tests to do
If you experience the slightest discomfort and in any doubt, consult your doctor or herbalist quickly, as the symptoms suggesting the presence of testicular cysts are very similar to those suggesting the presence of malignant testicular tumors.
To make a diagnosis on the cysts of the epididymis, it is necessary to do an ultrasound, and possibly a histological examination (sample and tissue analysis) which will reveal the cystic nature of the tumor, and rule out the hypothesis of a cancerous tumor.
The diagnosis of cysts of the epididymis also involves a scrotal ultrasound. This may reveal rounded nodular and cystic formations of varying sizes in the testicular parenchyma (tissue). However, the definitive diagnosis is only established after the histological examination (tissue analysis) which makes it possible to rule out the cancerous hypothesis.
Treatments: What to do if a testicular cyst gets bigger?
Most of the time, this is not the case. Your doctor may prescribe pain relievers to make you more comfortable.
Aspiration is a procedure that can help relieve some of the pain and pressure from the spermatoceles. Your doctor will insert a needle into the cyst to remove some of the fluid.
If the cyst fills up and comes back, your doctor may perform a procedure called sclerotherapy. It will drain some of the fluid from the spermatocele. Then he will use a substance that causes the sac to fill with scar tissue. This tissue could reduce the risk of the spermatocele returning. But it can damage the epididymis. Your doctor can suggest this option only if you are not interested in having children.
In rare cases (if the spermatocele is interfering with your daily life) your doctor may remove it with surgery. It will numb the area, make a small incision (cut) in your scrotum or groin, and remove the growth.
Treatment of epididymal cysts relies on clinical and ultrasound monitoring when the benign cystic nature is evident.
Treatment of an epididymal cyst
The intervention takes place under general or locoregional anesthesia. A short incision is made at the level of the bursa. After checking the underlying testis, the cyst is completely removed by opening the envelope of the epididymis and dissecting as close as possible to the wall of the cyst. Sometimes the surgeon may need to remove part or all of the epididymis.
The intervention is carried out within the framework of an outpatient surgery hospitalization. It may, in some cases, require 1 or 2 days of hospitalization.
Pain at the incision is usually minimal and temporary.
For a few weeks, the bursa remains enlarged and small swelling around the testicle can sometimes persist.
Removal of the epididymal cyst is suggested in the event of an increase in the volume of the bursa and/or any local discomfort or pain associated with its presence. "A short incision is made at the level of the bursa. After checking the underlying testis, the cyst is completely removed by opening the envelope of the epididymis and dissecting as close as possible to the wall of the cyst. The surgeon can sometimes be having to remove part or all of the epididymis ", develops the site of the French Association of Urology. Surgery is also considered in the case of certain dermoid cysts, in the presence of small lesions.
Complicated cases of epididymal cyst
In the majority of cases, the operation takes place without complications. However, any surgical procedure carries a number of risks and complications, which are described below:
Hematoma: bleeding after the operation can lead to the constitution of a hematoma of the bursa, possibly extended to the external genitalia, a reoperation to drain the hematoma may be necessary.
Delayed healing: it may require prolonged local care.
Infection: the existence of discharge through the incision, general signs of infection such as fever, or local signs such as inflammation of the bursa can lead to the initiation of appropriate antibiotic treatment and the treatment of a possible abscess by your surgeon.
Testicular atrophy: it occurs exceptionally after surgery of the epididymis
Recurrence: his risk is extremely low.
Impact on fertility: partial or total removal of the epididymis will permanently prevent the passage of spermatozoa on this side. This risk is rarer in the event of simple removal of the cyst.
Persistence of local discomfort or pain: Removal of the cyst does not guarantee the total disappearance of discomfort or pain.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
MEDICINAL PLANTS TO TREAT HEPATITIS B AND C
WHAT MEDICINAL PLANT CAN BE USED AGAINST HEPATITIS B AND C?
Hepatitis is an inflammation of the liver. This disease may progress on its own to healing or progress to fibrosis (scarring), cirrhosis, or liver cancer. Hepatitis viruses are the most common cause worldwide, but other infections, toxic substances (such as alcohol or certain drugs), and autoimmune diseases can also be the cause of cases of hepatitis. 'hepatitis. However, there is a medicinal plant(s) that can work against the negative effects of the hepatitis virus. Among them is one that has proven more effective and has led to several testimonies.
Dawasanté experts have a natural treatment based on medicinal plants to cure hepatitis B and C permanently.
Click on the image below to discover this natural treatment.
BEST MEDICINAL PLANT FOR HEPATITIS CURE
Our natural remedy also has anti-inflammatory and antioxidant properties, which help in the treatment and prevention of liver problems, so it is the best natural remedy for curing hepatitis B and C. It also fights against viruses that cause liver disease. 'hepatitis. It also provides antioxidants that help maintain the overall health of the liver. Simply put, it helps the body fight viral infections and cleanse the liver. It is the miracle solution to cure hepatitis B or C.
Our herbal teas have no side effects, either on the body or on health. Our treatment is therefore not dangerous. This natural remedy is a secret to cure your hepatitis without side effects.
Worldwide delivery!!
You can contact us by Whatsapp at +33644661758 or at +22990312738 direct calls and WhatsApp
MEDICINAL PLANT FOR HEPATITIS
Ginseng protects the liver from alcohol:
Among the main active ingredients of Panax ginseng are ginsenosides. From this family of natural molecules, we have been able to identify to date more than thirty representatives, each having different or complementary virtues. One of them, ginsenoside Rg1, could, according to recent animal studies, help protect the liver from liver damage following alcohol poisoning. The analysis of the inflammatory parameters and the state of the hepatic tissues after ingestion of a high dose of alcohol, much better in mice treated preventively with ginseng, shows the interest that this plant could have in addictology, in particular in support for weaning and prevention of cirrhosis often associated with alcoholic hepatitis.
Basil

Another virus-killing herb that is rarely known is bacilli. Basil is often used as a spice for Asian food, such as in Thailand. The antiviral compounds ursolic acid and apigenin in it have the potential to overcome enterovirus, hepatitis B, and herpes.
Oregano

For lovers of Italian cuisine, you must be familiar with the oregano sprinkled on pizza. Oregano is a virus-killing herbal plant because it contains the antiviral compound carvacrol.
Rosemary

You may often see rosemary in grilled chicken dishes. In fact, rosemary contains oleanolic acid which has the potential to treat hepatitis, influenza, herpes, and HIV in animals.
Licorice

Licorice is often found in traditional Chinese cough medicines and contains antiviral compounds liquiritigenin, glabridin, and glycyrrhizin. The root of the medicinal plant licorice has the potential to fight viral infections in the respiratory tract, HIV, and herpes.
Astragalus

Astragalus is a virus-killing herbal plant from China that has antiviral compounds and plays a role in boosting the immune system and protecting astrocyte cells in the body.
Elderberry
Elderberry or Sambucus is a medicinal plant that is often made in supplement form. This virus-killing herbal plant is often used to treat colds and flu.
Echinacea

Apart from elderberry, another virus-killing herbal plant that is often used as raw material for health supplements is echinacea. This medicinal plant has antiviral compounds that are effective against influenza and herpes.
Sage

You may rarely hear of the sage plant, which is a typical Western spice. However, this herbal plant has long been used in traditional medicine for viral infections. The antiviral content in this virus-killing herbal plant is located on the leaves and stems.
CLICK HERE TO DISCOVER THE BEST MEDICINAL PLANT FOR HEPATITIS
Worldwide delivery!!
You can contact us by Whatsapp at +33644661758 or at +22990312738 direct calls and WhatsApp









