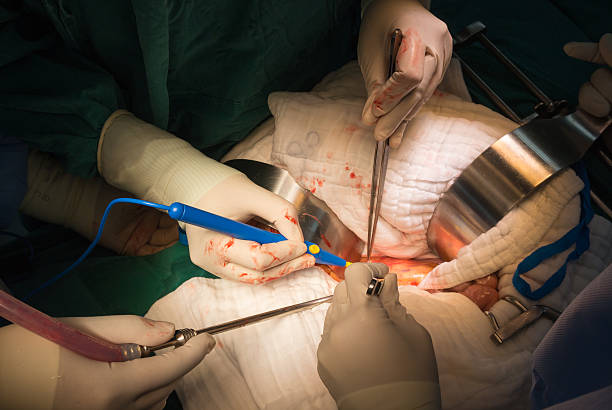
remove all your fibroids
Blog / 139 results found
HERBAL REMEDY FOR UTERINE POLYPS : Dawasanté experts
UTERINE POLYP: HERBAL REMEDY
The Uterine polyps are benign and are formed on the surface of the endometrium, which is located within the uterine cavity. They can be simple and multiple. In some cases, polyps at the offset neck. Neoplasm has a body and a leg, which is attached through the endometrium. Numerous medical observations suggest that polyps are most often found at the bottom of the uterus or its walls. Here is a herbal remedy that the experts at Dawasanté put at your disposal to treat uterine polyps. Click on the image below to discover this herbal treatment for uterine polyps.
The causes of this disease can be different, and tumors appear in young girls and older women. If the doctor put such a diagnosis - do not despair. There are ways not only with medication, you can still treat uterine polyps with an herbal remedy. Both methods are effective in killing polyps and preventing new ones. A woman can choose the most suitable treatment option for yourself, depending on the characteristics of her body.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: https://wa.me/22996374527
Signs and symptoms of uterine polyps

Pronounced symptoms of uterine polyps are few, their presence is easily confused with symptoms of other diseases. The main symptom that should alert a woman - profuse vaginal discharge.
During the early development of the disease, uterine bleeding and failure of the menstrual cycle can occur. A polyp tends to increase. This process leads to involuntary contractions of the uterus, the cervix by which it is relaxed and pushed into the vagina neoplasm. Women may, therefore, feel pain and cramping, vaginal discharge is observed as ichor.
Asymptomatic illness contributes to the fact that patients in the early stages do not pay much attention to minor signals from the body, resulting in seeking medical assistance too late.
Polyps are especially dangerous for pregnant women. In such cases, treatment is only possible with the use of homeopathy and traditional medicine.
To get rid of polyps, use some folk remedies only after histological analysis, which will help determine the exact nature of the polyp. These tumors are glandular, fibrioznymi glandular, fibrioznymi, and adenomatous. Adenomatous polyps - the most dangerous, as they are the main irreversible changes at the cellular level. These tumors are signs of a precancerous condition in the lining of the uterus.
Celandine for the treatment of uterine polyps

To achieve good results from the treatment of uterine polyps herbal remedy can be at an early stage when the disease is only just beginning to develop. Also, folk remedies are often used as prophylaxis before or after drug treatment. But regardless of the folk method, women need to be sure to see your doctor.
Most often, to get rid of polyps in the uterus, used celandine. It is recognized as the most effective and popular way. It is necessary to take and use for douching.
To prepare the healing infusion to collect the fresh celandine cabbage and fill their glass jar, then pour boiling water. In addition, the bank should close the lid, wrap with a blanket or a towel, and infuse it in this way for 12 hours.
The ready infusion should be taken three times a day. The initial dose should be 1 st. g., which should be gradually increased by 100 ml at a time. In this way, the treatment of uterine polyps should be carried out for two weeks after which requires a break - three weeks. In addition, the course must be repeated.
Back to summary
Herbal and berry extracts to deal with polyps
Useful and effective extracts that are able to overcome the disease, usually prepared from rose hips, berries, cranberries, nettle. This type of treatment is considered to be one of the most benign, which traditional medicine offers.
To prepare the infusion of the healing need:
- cranberries
- chopped nettles
- hips
All the ingredients should be mixed together and the mixture pour a glass of hot water. Soak the infusion should be in a closed container for 4 hours. Means should be taken twice a day for 250 ml.
Equally effective is accounted for on the basis of the tincture of golden whiskers. To make this folk remedy, you need to:
- 50 golden mustache seals;
- 500 ml of vodka.
The plant should be crushed and pour vodka, then let it brew for 10 days. The ready infusion should be taken twice a day in the diluted form: a third of a cup of water add 20 drops of medicated liquid. The use of these drugs is necessary before meals. Treatment should be carried out for a month, then take a break for 10 days. Expect full recovery from uterine polyps to be possible only after five treatments.
Pumpkin seeds and garlic as a remedy for polyps

Garlic since ancient times is considered an excellent remedy for a variety of ailments. List of public methods can beat uterine polyps, also it includes this herbal medicine. Based on this, it is possible to make their own medical rod.
This will require a large clove of garlic, crushed and carefully wrapped the entire mass resulting in a two-layer gauze, then tightly bandage. The ready compress should be careful at night to enter as deep as possible into the vagina and pull it out in the morning. To remedy such manipulation of polyps should be repeated for a month every night.

For an indoor reception, it is possible to prepare another useful folk medicine on the basis of pumpkin seeds. Require:
- 7 hard pieces of egg yolks;
- fresh pumpkin seeds;
- 2 cups of vegetable oil.
The seeds should be well ground and add the yolks carefully mashed. Then the resulting mixture should be mixed with vegetable oil, optionally to form a homogeneous paste. This is followed by a mass placed for 30 minutes in a water bath. When the means ready to cool down, it is necessary to take a teaspoon of fasting for five days, then take a break for the same period of time. The repetition rate required to complete recovery. The mixture should be refrigerated, tamped.
Douching using an herbal decoction

In the arsenal of folk remedies are the very popular treatment showers. To combat this way of uterine polyps is used quite often. Typically, douching should be used if the woman against the background of the disease is observed vaginal bleach.
To prepare the solution for irrigation will need:
- yarrow
- rosemary leaves
- Sage leaves
- oak bark
All the ingredients must be crushed and mixed in an enamel container, then pour 2, 5 l of boiling water. Then the mixture should be put on the fire and bring to a boil. Boil the broth and simmer for half an hour should be. When it is ready, it is necessary to cool it to room temperature. Then you need to empty the infusion using a cheesecloth or fine strainer.
The lukewarm solution is used for douching twice a day every day to get rid of the disease.
Medicinal herbal teas based on nettle and knotweed

To cook another decoction for douching can use these herbs:
- nettle
- knotweed grass
- pharmacy chamomile - 1 tbsp.
Herbs need to grind and mix. The resulting mixture should be put in an enamel saucepan and pour boiling water 1 liter. Boil the followed broth for 5 minutes over medium heat and then allow to cool to room temperature.
Strained broth Ready to use for douching. Treatment is effective, it is desirable to carry out the procedure at least twice a day for 2 weeks.
Always remember that the reproductive function is one of the most important for a woman, so in case of alarming symptoms must necessarily be examined by a doctor. It is useful in visits to the doctor and as a prophylactic measure. If the disease is detected and treatment is still necessary to start the independent thoughtless application of various folk remedies is not necessary. It is necessary to consult a gynecologist, who will choose the most suitable and safe way.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: https://wa.me/22996374527
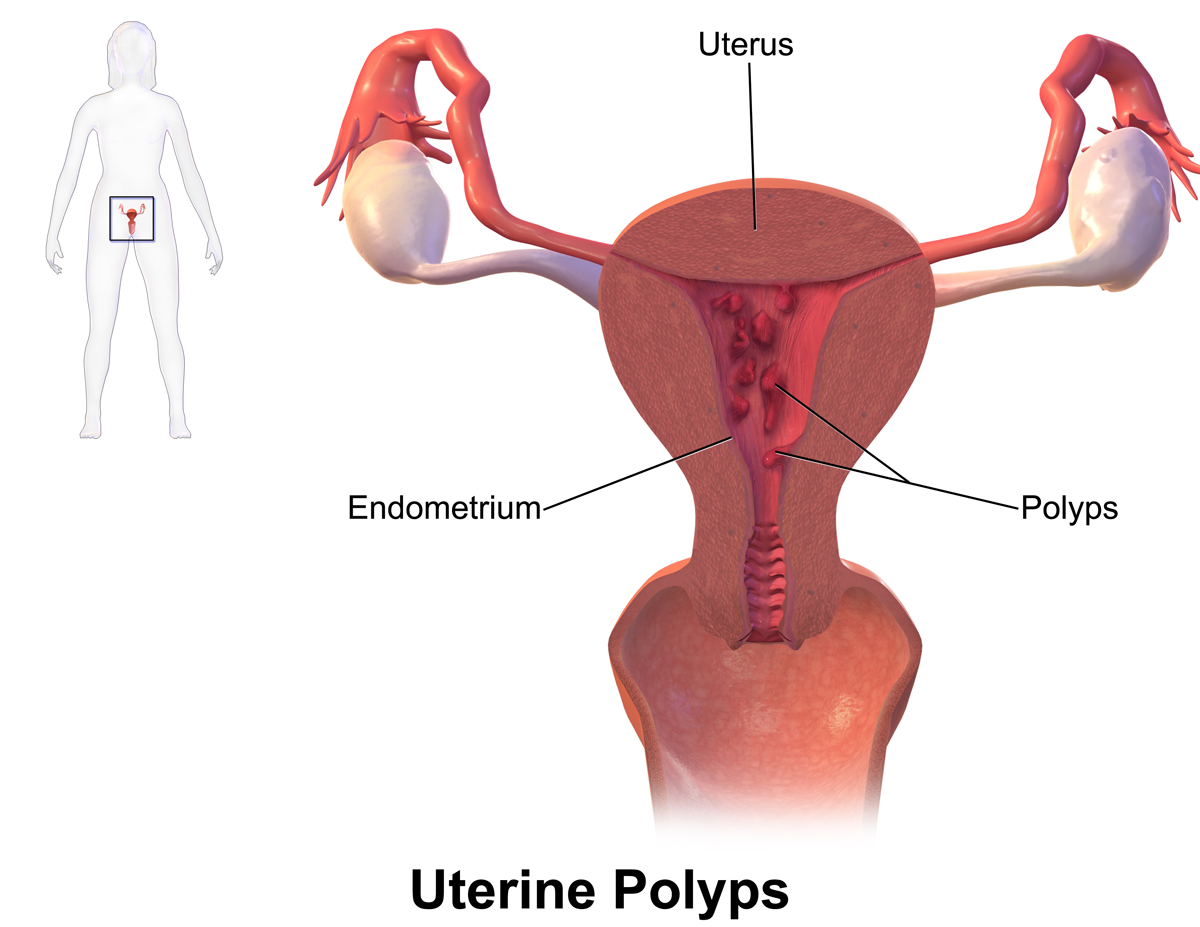
UTERINE POLYPS AND CANCER: Natural treatment
UTERINE POLYPS AND CANCER
A polyp can sometimes seem like a fibroid uterus ( polyp fibrous) or cancer endometrial ( polyp atypical, irregular). Conversely, cancer endometrial can sometimes look like a polyp. The combination of a polyp to cancer endometrial is more common after menopause. However, Dawasanté experts provide you with a natural treatment to cure uterine polyp cancer. Click on the image below to discover this natural treatment.
To contact our experts please call or write to us on the following number, tel / WhatsApp: https://wa.me/22996374527
The uterine polyps are growths that develop at the expense of the lining of the uterus (endometrium), or at the expense of the lining of the cervix (endocervical).
These growths are benign tumors. They can be single or multiple. A polyp can be "pedicle" (comprising an insertion foot) or sessile (broad implantation base). It can be "fibrous" or "mucous". By definition, the development of a polyp occurs at the expense of a mucous membrane. This is why, in addition to the uterus, certain organs or areas of the human body can be invaded by this type of tumor such as the bladder, colon, stomach, vagina, etc.
The uterine polyps are outgrowths attached to the inner wall of the uterus which extends into the uterine cavity. Cellular proliferation in the lining of the womb (endometrium) results in the formation of uterine polyps, also called endometrial polyps. These polyps are usually non-cancerous (benign), although some can be cancerous or turn into cancer (precancerous polyps).
A uterine polyp can look like a fibroid or a cancerous tumor, so be careful not to get the wrong diagnosis. Cancerization of the polyp is possible.
All examinations performed should show whether the uterine polyps are benign or not. Thus, after removing these growths, a complete analysis of them is required. Postmenopausal women are prone to endometrial cancer combined with uterine polyps.
Two forms of treatment are possible to treat polyps, the choice is based on their benignity, size, appearance, etc. Those that are small and less worrying may go away as a result of hormonal drug therapy. With this treatment, the patient takes progestins. In most cases, operative hysteroscopy is necessary, it consists of the removal of the polyps. This form of treatment should be carried out with great care, especially in women who wish to have children later. For postmenopausal women, the risk of recurrence being high, endarterectomy is recommended.
Endometrial cancer is a cancer of the inside of the uterus, where the endometrium is the lining that lines the inside of the uterus. In women with cancer at this level, endometrial cells multiply abnormally. Endometrial cancer usually occurs after menopause, but 10 to 15% of cases affect premenopausal women, including 2 to 5% of women under 40 years old.
A significant proportion of endometrial cancer is thought to be attributable to an excess of estrogenic hormones produced by the ovaries or supplied by the outside. The ovaries produce 2 types of hormones during the female cycle: estrogen and progesterone. These hormones act on the endometrium throughout the cycle, stimulating its growth and then its expulsion during menstruation. An excess of estrogen hormones would create an imbalance conducive to the poorly controlled growth of endometrial cells.
Several factors can increase estrogen levels, such as obesity or hormone therapy with estrogen alone. This type of hormone therapy is therefore reserved for women who have had the uterus removed or hysterectomy who are no longer at risk of endometrial cancer. For more information, see the People at risk and Risk factors sections.
For some women, however, endometrial cancer does not appear to be caused by a higher level of estrogen.
Other causes are involved in endometrial cancer, such as advanced age, overweight or obesity, genetics, hypertension, etc.
Sometimes cancer occurs without a risk factor being identified.
Like any mucous membrane, the endometrium is made up of surface cells called “epithelial” and supporting tissue, the “chorion”. More than 90% of endometrial tumors develop at the expense of the epithelium. This category includes cancerous lesions such as adenocarcinomas and carcinosarcomas, pre-cancerous lesions such as atypical hyperplasias, endometrial polyps, and lesions induced by tamoxifen. Adenocarcinomas, the most common form, are developed from "glandular" type epithelial cells.
Other metabolic factors: diabetes and glycemic load
Diabetes is a risk factor for endometrial cancer. The risk of developing this cancer is twice as high (significant relative risk) in diabetic patients than in people without diabetes (Larsson, 2006).
It is the development of insulin resistance that is responsible for the increased risk of cancer. Insulin is then in large quantities in the blood and will be able to stimulate growth factors acting on the endometrium. The precise mechanisms are not well known. This is confirmed in the 2013 WCRF / AIRC report. This same international report also found that increased glycemic load (which estimates the ability of foods eaten to increase blood glucose) is a risk factor for endometrial cancer with a probable level of scientific evidence to account. based on current scientific data; these are not as convincing as for obesity.
Early puberty and late menopause
Age at puberty determines when the ovaries start producing estrogen, and menopause determines when they stop producing estrogen. Earlier puberty or late menopause, therefore, exposes a woman to estrogen for a longer period of her life and therefore represents a risk factor.
Not having had a child (nulliparity)
The menstrual cycle of women experiences a period during which the functional area of the endometrium collapses. In order to accommodate the future fertilized egg, the endometrium must regenerate. For this, estrogen plays a role in stimulating cell growth in the endometrium.
During pregnancy, there is no ovulation for 9 months. The estrogen stimulation does not stop, however, but is much less than if there had been 9 ovarian cycles. Thus, women without children are exposed to greater amounts of estrogen: this is considered a risk factor for the development of endometrial cancer (Lochen, 1997).
This is sort of how polyp can be the root cause of cancer or various tumors.
To contact our experts please call or write to us on the following number, tel / WhatsApp: https://wa.me/22996374527

NABOTH CAUSE CYST: Natural treatment
NABOTH CAUSE CYST
A cyst Nabothian (or egg Naboth ) is a cyst mucous that develops at the neck of the uterus; it is due to the obliteration of the excretory ducts of the glands of the uterine cervix. Here is the natural herbal treatment to cure Naboth cysts. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
This is the accumulation of mucus produced by the glands of the endocervix (columnar epithelium) which cannot be evacuated due to the physiological covering of the gland by squamous epithelium (a phenomenon of repair). These cysts are most often visible at the level of the ectocervix, presenting on colposcopy as a translucent cyst whose wall is covered with vessels. They can also sit in the endocervix and be visible on ultrasound.
Causes of Naboth's cyst
The Naboth cysts are formed:
- Either because there is a development of the tissue of the cervix (following childbirth for example).
- Either in older women, because the natural secretions are retained in the thinned tissue of the cervix.
The cause of the appearance of a Nabothian cyst is the obstruction of the ducts carrying the secretions from the mucus glands. It is a common phenomenon in a woman after childbirth, the lining of the cervix develops, or in postmenopausal women, in whom the lining of the uterus becomes thinner.
The cysts of Naboth often appear after repair ectropion: epithelium squamous metaplasia (newly formed) covers the glandular endocervical crypts, without colonizing, and locked glands continue to secrete, which is responsible for their expansion; the glands then form small cysts which protrude under the squamous epithelium.
These retentional glandular cysts are visible on the ectocervix.
Nabothian cysts form when the mucus-producing glands in your cervix become covered with skin cells and become blocked. The skin cells clog the glands, causing mucus to build up. This causes a cyst to form on the neck that looks like a small white bump.
Childbirth and physical trauma to the cervix can cause Nabothian Trusted Source cysts in some women. During childbirth, excess skin cells can grow on the mucous gland and trap the mucus, causing cysts to form. Physical trauma around the cervix can cause excess tissue on top of the mucous glands during the healing process and trap mucus, which can also cause these cysts to appear. Cysts caused by physical trauma are especially common during recovery from chronic cervicitis, in which cervical tissue is inflamed.
You are more likely to develop these cysts if you are pregnant or of childbearing age. Childbearing age lasts from puberty until the onset of menopause, which can sometimes reach 40 or 50 years.
You might also be at risk of developing similar cysts if you have a disorder called malignant adenoma. This condition is a type of neoplasia that affects the production of mucus in the cervix of your uterus. These cysts are often identical to Naboth's cysts. Talk to your doctor about screening for malignant adenoma if you are concerned that your Naboth cyst is the result of this condition rather than other causes.
In most cases, Nabothian cysts appear when new tissue grows back on the cervix after childbirth. This new tissue blocks the openings of the nabothian glands in the cervix, trapping their mucous secretion in tiny pockets under the skin. Nabothian cysts are a normal finding on the cervix of women who have had children. They are also seen in postmenopausal women whose cervical skin has thinned with age. Less often, nabothian cysts are linked to chronic cervicitis, long-term infection of the cervix.
The mucus-producing gland in the cervix is covered with cells and skin clogs. Physical trauma and childbirth cause additional skin cells to grow in the mucous gland and trap the mucus, resulting in the cyst forming.
Infection: The cervical glands produce large amounts of mucus to protect the area from all kinds of infections and inflammation. This process can be understood as the body's natural way to wash away foreign objects that can cause health problems.
As the level of mucus production increases, there will obviously be an increased risk of blockage and cyst formation. Therefore, infections and inflammation can cause the growth of Naboth cysts.
Hormonal changes: the changes hormonal play a direct role in the formation of such cysts. For example, menopause is a stage in which a woman may experience thinning of the skin of the cervix. It causes inflammation of the cervix causing cervical infection.
The cervix connects the two most important parts of the female reproductive system. Therefore, hormonal changes will have a direct effect on him.
These cysts mainly develop during pregnancy, childbirth or menopause. Therefore, the development of these cysts could be the result of changes in hormone levels.
Trauma: Injury or scarring of the tissues lining the cervix could lead to the formation of Naboth's cysts. The body tries to grow new tissue to repair and heal the injured area, but sometimes there can be an overgrowth of the tissue.
Pregnancy: Normally, the cervix remains open to allow the movement of semen from the vagina to the uterus and the flow of menstrual fluid from the uterus to the vagina.
However, during pregnancy, the body's mechanism closes the cervix to ensure the development of the fetus in the womb. New tissue grows on the mucous gland after childbirth due to the process of metaplasia.
If these tissues grow excessively, they could block the glands and prevent mucus from draining out, leading to the development of Naboth cysts.
Neck Problems: Postmenopausal women may experience thinning of the skin of the cervix. Inflammation of the cervix is a common effect of cervicitis.
These problems, along with other sexually transmitted infections of the cervix, could lead to the development of cysts on the surface of the cervix.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
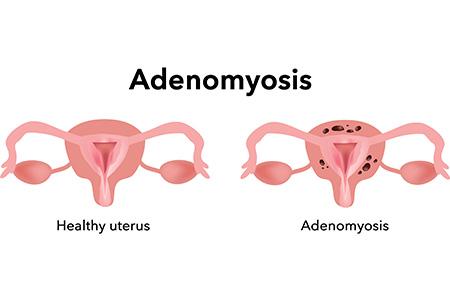
ADENOMYOSIS NATURAL TREATMENT
We talk about adenomyosis when the tissue that normally lines the uterus (the endometrium) grows in the muscular wall of the uterus. Adenomyosis can cause menstrual cramps, low abdominal pressure, and bloating before your period and can lead to heavy periods. It is even responsible in some cases of infertility in women. Here is the natural herbal treatment from Dawasanté experts to treat adenomyosis. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Adenomyosis is most common in women who have had several children.
If you have adenomyosis and want to avoid the operation at all costs, you have come to the right place. Here we offer you a natural remedy made from medicinal plants very effective to permanently cure adenomyosis. It is specially designed for patients who do not want to have surgery because every operation carries a risk.
Natural treatment
The natural treatment that we offer to cure adenomyosis consists mainly of natural herbal teas. This natural herbal treatment for adenomyosis will remove the pain you feel during your period and allow you to have normal cycles. It outperforms conventional treatments that relieve pain, but don't get to the root of the pain. Our herbal tea contains plants that reduce the estrogen level in the blood. This helps block the proliferation and bleeding of adenomyosis lesions. These herbal remedies are rich in an antioxidant that inhibits the enzymes that lead to pro-inflammatory prostaglandins. These are nutrients in high doses anti-inflammatory. This will definitely put an end to the pain you feel during your period. We know that many of you have had adenomyosis treatment or surgery, but the pain returned years later. No panics ladies! With us, no recurrence, no side effects. You will be permanently cured of adenomyosis.
This natural herbal tea also facilitates cell multiplication relating to fertility, growth, healing and immunity; to the synthesis and secretion of many hormones. Thanks to these medicinal plants, you will avoid miscarriages. It is nature's secret to cure adenomyosis and get pregnant quickly.
Our natural remedy to treat adenomyosis very often gives positive results and acts significantly on the reduction of the pain felt. It has an efficiency rate of 98%. Trust us ladies and you will get pregnant once more.
To discover our natural remedy to cure Naboth cysts, click here
Symptoms
Sometimes adenomyosis does not cause any signs or symptoms or causes only mild discomfort. However, adenomyosis can cause:
-
Heavy or prolonged menstrual bleeding
-
Severe cramping or sharp, knife-like pelvic pain during menstruation (dysmenorrhea)
-
Chronic pelvic pain
The causes
The cause of adenomyosis is not known. There have been a lot of theories, including:
· Invasive tissue growth. Some experts believe that adenomyosis results from the direct invasion of endometrial cells through the lining of the uterus into the muscle that forms the walls of the uterus. Uterine incisions made during an operation such as a cesarean section could promote the direct invasion of endometrial cells into the lining of the uterus.
· Developmental origins. Other experts suspect that adenomyosis originates in the uterine muscle from endometrial tissue deposited there during the formation of the uterus in the fetus.
· Inflammation uterine is related to childbirth. Another theory suggests a link between adenomyosis and childbirth. Inflammation of the lining of the uterus during the postpartum period can cause the normal boundary of the cells that line the uterus to rupture. Surgery on the uterus can have a similar effect.
· Origin of stem cells. A recent theory suggests that stem cells from the bone marrow could invade the uterine muscle, causing adenomyosis.
Regardless of the course of adenomyosis, its growth depends on the circulation of estrogen in the female body.
Risk factors
Risk factors for adenomyosis include:
-
Previous uterine surgery, such as cesarean or fibroid removal
-
Childbirth
-
Middle Ages
Most cases of adenomyosis occur in women between the ages of 40 and 50. Adenomyosis in these women could be linked to longer exposure to estrogen compared to that in younger women. However, current research suggests that the condition might be common in younger women.
Complications
If you often have heavy and prolonged bleeding during your period, you can develop chronic anemia, which can lead to fatigue and other health problems.
While not harmful, the pain and excessive bleeding associated with adenomyosis can disrupt your lifestyle. You may be avoiding activities that you have done in the past because you are in pain or are worried about bleeding.
Diagnostic
Your doctor may suspect adenomyosis based on:
-
Signs and symptoms
-
A pelvic exam that reveals an enlarged and tender uterus
-
Ultrasound of the uterus
-
Magnetic resonance imaging (MRI) of the uterus
In some cases, your doctor may take a sample of uterine tissue (endometrial biopsy) to check that your abnormal uterine bleeding is not associated with another serious condition. But an endometrial biopsy will not help your doctor confirm the diagnosis of adenomyosis.
The only way to confirm adenomyosis is to examine the uterus after a hysterectomy. However, pelvic imaging such as ultrasound and MRI can detect signs of it.
Other uterine diseases can cause signs and symptoms similar to adenomyosis, making adenomyosis difficult to diagnose. The conditions include fibroids (leiomyomas), uterine cells growing outside the uterus (endometriosis), and growths in the lining of the womb (endometrial polyps).
Your doctor may conclude that you only have adenomyosis if you have chosen other possible causes of your signs and symptoms.
Medical treatments
Adenomyosis often goes away after menopause, so treatment may depend on how close you are to this stage of life.
Treatment options for adenomyosis include:
· Anti-inflammatory. Your doctor may recommend anti-inflammatory drugs, such as ibuprofen, to control the pain. By starting an anti-inflammatory medication one to two days before your period starts and taking it during your period, you can reduce menstrual blood flow and help relieve pain.
· Hormonal Drugs. Birth control pills that combine estrogen and progestins, patches containing hormones, or vaginal rings can reduce the heavy bleeding and pain associated with adenomyosis. Progestin-only contraception, such as an intrauterine device, or continuous-use birth control pills often lead to amenorrhea - the absence of periods - which may provide some relief.
· Hysterectomy. If your pain is severe and no other treatment has worked, your doctor may suggest surgery to remove your uterus. Removing your ovaries is not necessary to control adenomyosis.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
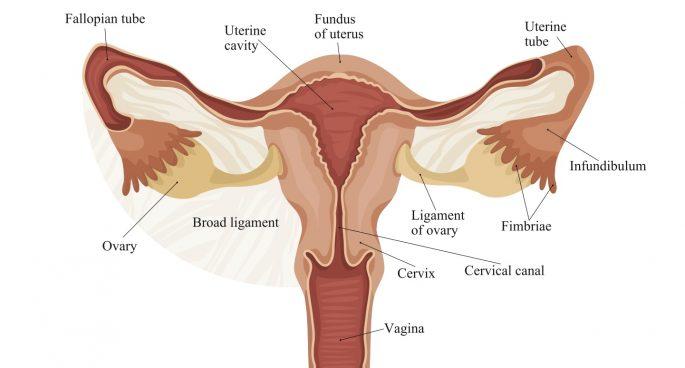
OBSTRUCTION OF FALLOPIAN TUBE: Natural treatment
Endometriosis is a common and painful disease that affects thousands of women around the world in North America as in Africa and South, other continent and is one of the three main causes of infertility in women.
During a normal menstrual cycle, the lining of your uterus - called the endometrium - begins to thicken before you become pregnant. If you don't get pregnant that month, your body loses its endometrium during your period and the process starts all over again. In endometriosis, for reasons that researchers don't fully understand, tissue very similar to the endometrium begins to grow outside the uterus in various places that it shouldn't. It can appear in or on the ovaries, fallopian tubes, the various structures that support the uterus and the lining of the pelvic cavity. Sometimes it is also found in other places, including the cervix, vagina, rectum, bladder, bowel and elsewhere.
The problem is, this tissue behaves like normal endometrial tissue - it builds up and breaks down with your menstrual cycle - but it can't shed like normal endometrial tissue during your period. As a result, unwanted tissue causes irritation and inflammation. This build-up of tissue can prevent the eggs from leaving the ovaries or from being fertilized by the sperm. It can also leave scars and block the fallopian tubes, preventing the meeting between the egg and the sperm.
Finally, endometriosis problems can be the cause of tubal obstruction. This is because pieces of the uterine lining can end up in the tubes or on the ovaries and block the progression of sperm to the egg, thus preventing fertilization. Dawasanté experts provide you with a natural herbal treatment to unblock your tubes and allow you to quickly get pregnant.
Click on the image below to discover this natural treatment.
However, obstruction of the fallopian tubes is a major cause of female infertility. The blocked fallopian tubes do not allow the egg and sperm to converge, making fertilization impossible. The fallopian tubes are also called oviducts, uterine tubes, and salpines (singular salpinx).
Tubal obstruction
About 20% of female infertility can be attributed to the causes of the tubes. occlusion of the distal tubes (affecting the tip towards the ovary) is usually associated with the formation of hydrosalpinx and is often caused by Chlamydia trachomatis. Pelvic adhesions can be associated with such an infection. In less severe forms, the fimbriae may be clumped and damaged, but some permeability may still be preserved. Tubal obstruction in the middle of the segment may be due to tubal ligation procedures, as this part of the tube is a common target for sterilization procedures. Proximal tubal occlusion can occur after infection, such as. In addition, some tubal sterilization procedures such as the Essure procedure target the part of the tube near the uterus.
A blockage of the uterine tubes can be caused by various disorders, and in some rare cases even be present from birth without causing symptoms until the desire to conceive a child. Obstruction of the fallopian tubes is very often involved in cases of female infertility.
There are various causes of obstruction, or even lesions, of the tubes:
- Pelvic infections;
- Use of an intrauterine device;
- Rupture of the appendix;
- Pelvic or lower abdominal surgery;
- Certain pathologies, for example, tuberculosis;
- Ectopic pregnancy in the fallopian tubes;
- Congenital malformations of the tubes;
- Uterine fibroma ;
- Endometriosis ;
- Asherman's syndrome (lesions or infections during surgery).
We speak of proximal tubal obstruction when the tubal isthmus is involved. It can follow an abortion, miscarriage, cesarean section, pelvic inflammatory disease or the contraceptive pill.
If the distal tubes are blocked, it is the end of the tube on the side of the ovary that is affected. This type of obstruction is often associated with a "hydrosalpinx" which refers to the abnormal presence of a pocket of fluid in the fallopian tube. Usually, hydrosalpinx is caused by infection with Chlamydia trachomatis (sexually transmitted infection).
In other cases, the ovarian fringes, which have an important role in the conduction of the oocyte in the tubes, are damaged or stick together.
Several elements are at the origin of this obstruction
GENITAL INFECTIONS
The majority of the causes of obstruction are infections of the genital tract, especially of the tubes ( salpingitis ) which have occurred in the past. Most of the time, they are due to sexually transmitted diseases (such as chlamydia), which may have gone unnoticed. Nevertheless, they were sufficient to block the proboscis and make it waterproof. This is why it is important for all women to prevent the risk of STDs, in particular through safe sex with occasional partners and regular gynecological monitoring.
MEMBERSHIP
Aside from infections, adhesions, where the two sides of the tube wall stick together, can also be present.
ENDOMETRIOSIS
Endometriosis problems may be the cause of obstruction of the fallopian tubes. This is because pieces of the uterine lining can end up in the tubes or on the ovaries and block the progression of sperm to the egg, thus preventing fertilization.
Most often, a catheter can become blocked due to an infection such as pelvic inflammatory disease (PID). The tubal infertility rate would be 12% after one, 23% after two and 53% after three episodes of PID. The fallopian tubes can also be blocked or disabled by endometritis, infections after childbirth, and intra-abdominal infections, including appendicitis and peritonitis. The formation of adhesions may not block a fallopian tube, but make it dysfunctional by deforming it or separating it from the ovary. It has been reported that women with distal tubal occlusion have a higher rate of HIV infection.
The fallopian tubes can be blocked as a method of birth control. In these situations, the tubes tend to be healthy and, in general, patients requesting the procedure had children. Tubal ligation is considered a permanent procedure.

NATURAL TREATMENT FOR CLOGGED FALLOPIAN TUBES
The fallopian tubes are muscle tubes lined with delicate hair-like structures. These “hairs” work in both directions; help egg travel from the ovaries to the uterus and help sperm come up from the uterus.
Each fallopian tube ends in fimbriae, which are finger-like structures. Fimbriae grab and guide an egg when the ovary releases it.
The fallopian tubes play an important role in conception because they are the place where most of the eggs are fertilized. If part of the fallopian tube is damaged, for example by surgery or an infection, it may be blocked with scar tissue.
The fallopian tubes blocked are one of the possible causes of female infertility. Usually, there are no symptoms, but certain risk factors can increase the risk of developing the disease. The medical term for a blocked fallopian tube is tubal occlusion. However, Dawasanté experts provide you with a natural herbal treatment to unblock the tubes without surgery, allowing you to quickly get pregnant.
Dawasante's natural treatment to unclog blocked fallopian tubes

What if I have blocked tubes and want to get pregnant?
Here is the best African herbal remedy for unblocking the tubes and getting pregnant quickly . These herbs are very effective at unblocking the fallopian tubes. They have already enabled many women around the world who had blocked tubes to regain their fertility without operations. If you have blocked tubes, here are the medicinal plants that will allow you to experience the joy of being a mother
Click on the image below to discover this natural treatment.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
What are the best natural treatment for unclogging your tubes?
Thanks to our research, we have identified several effective homemade natural remedies to unblock the tubes and get pregnant quickly in addition we have:
11 remèdes naturels contre les trompes bouchées
1-Turmeric

Turmeric is a natural anti-inflammatory. It can be very effective in unblocking the fallopian tubes. Curcumin, the active ingredient in turmeric is very effective in reducing inflammation. You can consume curcumin in supplement form, add turmeric to your food, or drink a glass of turmeric.
Turmeric has no known side effects when taken in small doses. However, at doses of more than 8 grams per day, it can have unwanted effects. Make sure you take the correct dosage of turmeric or, better yet, add the spice to your cooking.
2-Garlic

Garlic is a great way to improve fertility and unclog the fallopian tubes. Garlic has always been consumed for its many health benefits as the aphrodisiac properties present in garlic help to improve blood circulation in the body. Eating raw garlic daily on an empty stomach helps fight infertility in women, lowers blood pressure and cholesterol
3- Cleansing with a fertility diet

The fertility diet helps cleanse the entire reproductive system and increase blood flow to the reproductive organs. The herbs in this cleansing regimen are absorbed by the body and will work where they are needed. The fertility cleanse creates a "clean slate" in the body which helps the body respond better and use other natural remedies.
This fertility diet cleans up the food waste that you need to avoid and synthesizes more that you need. Foods that you should avoid are alcohol, cigarettes, non-organic meats and dairy products, processed foods, processed white seeds, white sugar, fried foods, soy foods.
When it comes to what you should eat, the following should be suitable for fertility cleansing:
- Eat all organic vegetables.
- Eat low amounts of dairy products and make sure the ones you eat are organic.
- Eat fish at least three times a week.
- All types of red meats are recommended.
- Avoid chicken or chicken products.
- Seeds are also highly recommended
- Consume foods with high enzymatic proportions
- Avoid all refined sugars or fruit juices (unless it is freshly squeezed).
- Drink plenty of clean water.
4- Castor oil

the castor oil has been used for centuries to enhance fertility in women, and in particular to unblock fallopian tubes. How is it used?
-dip a cloth in castor oil
-Place this cloth on the skin on the lower abdomen. This will improve circulation and promote healing of the tissues and organs under the skin. Castor oil therapy helps the fallopian tubes by softening tissue and improving circulation in the pelvic area.
5- Apple cider vinegar

Apple cider vinegar is a fermentation product that produces yeasts and bacteria that are beneficial for unblocking the tubes. This is because vinegar contains a number of vitamins and minerals, including magnesium, potassium, copper, group B vitamins, and vitamin C. Taken daily, it can help unblock the fallopian tubes by balancing hormones and shrinking fibroids.
Instructions for use:
-Mix 2 tablespoons of apple cider vinegar in 1 glass of water
-You can add a touch of honey or molasses to soften the mixture.
-You can drink the mixture right away or sip it for 30 minutes.
6-Meditation

Meditating daily will help lower stress levels and promote general healing. However, reducing stress reduces deterioration and inflammation of the fallopian tubes.
As an additional tip, don't forget to start meditating with a short session consisting of breathing exercises and relaxation techniques. Even if you only do it for a few minutes, meditation will provide you with positive energy to start your day and reduce your stress.
7- Fertility massage

Some alternative medicine practitioners suggest fertility massages to unblock the fallopian tubes. These usually involve hot oil massages on the abdominal area. How to do a fertility massage?
- Lie down on an exercise mat with your face up and a pillow under your lower back.
-Relax and apply almond, olive, or lavender oil to your hands and apply by massaging your pubic bone, as the uterus is below this bone.
-Gently massage from bottom to bottom and pull your abdominal wall towards the navel. Maintain this position, count to 10 and release your hands. Repeat this maneuver 10 to 20 times.
NB: Do not do this if you are bleeding or are pregnant. Also, if possible, visit a massage therapist who specializes in abdominal massage for best results.
8- Mugwort

Mugwort is a plant sometimes recommended to improve female fertility. It is also recommended for unblocking the fallopian tubes.
Mugwort has a long history of use for fertility in a number of different cultures. It has been used all over Europe and Asia for centuries. It is often used in Chinese medicine in the form of moxibustion, which involves burning a mugwort above an acupressure point.
9- Green clay

The use of green clay to unclog the proboscis is very common in East Africa.
The blocked tubes are released by the serious treatment of green clay and the follow-up of a feeding program made by a dietician or a naturotherapist.
10- Foods with antioxidants

Try to avoid things like meat from animals as they contain hormones that can affect a woman's hormones like estrogen. Replace them with foods rich in antioxidants to promote wound healing. Foods rich in antioxidants are:
- Fresh fruits, vegetables (all kinds)
- Vegetable oils like sunflower oil, coconut oil, olive oil.
- Tea, chocolate, soy, coffee, and cinnamon are high in flavonoids (a type of antioxidant).
- Carotenoids are plant enzymes that have antioxidant activity and can reduce the build-up of free radicals in the body. Carotenoids can be stored by consuming eggs, fruits and red-yellow vegetables like carrots, mangoes, peppers, papayas, citrus fruits, spinach, etc.
11-Stop drinking and smoking

The blockage of the fallopian tubes most often occurs when you are under excessive stress. So, you need to improve the quality of your life to be on track to naturally unblock the fallopian tubes.
Alcohol and smoking are considered to be primary factors for such illnesses and are important for relief by permanently giving up these habits. Not only will this action improve the conditions of the fallopian tubes, it will also improve the health of your body, nails, hair, teeth and even your skin.
If you are a regular smoker or an alcoholic, now is the time to start working out and quit altogether.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
CLOGGED FALLOPIAN TUBES AND FIBROIDS: Natural treatment
The fibroid uterine cancer are not common tumors (benign) of the uterus and are the most common reason for recommending a hysterectomy. They grow from the muscle wall of the uterus and are made up of muscle and fibrous tissue. Many women over the age of 35 have fibroids but usually have no symptoms. Fibroids can be the cause of blocked tubes. Here is a treatment to cure fibroids naturally and prevent blocked tubes. Click on the image below to discover this natural treatment.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
In some women, however, fibroids (myomas) can cause heavy bleeding, pelvic discomfort and pain, and occasionally put pressure on other organs. These symptoms may require treatment. Treatment may take the form of drugs to control pain and bleeding, hormone therapy to shrink the tumor, surgery to remove the tumor, or a hysterectomy. There are promising new investigational drugs that can temporarily shrink tumors. These drugs can have serious side effects and are usually very expensive. These treatments may be sufficient or provide temporary relief and allow a woman to delay a hysterectomy, especially if she still wants to have children. In more severe cases, a hysterectomy may be recommended.
Some women choose to do nothing because fibroids will often shrink in size as a woman goes through menopause.
As for the fallopian tubes, they are an essential organ of the female reproductive system. Measuring about ten centimeters each, these two ducts formed by smooth muscles and covered by the peritoneum connect the ovaries to the uterus. During ovulation, the oocyte expelled by the ovary is captured in the pinna, the terminal part of the proboscis, and moved to the ampulla, the central part of the duct. This is where fertilization by a sperm can take place. Then, for 3 to 4 days, the embryo develops in the tube, the time necessary for its transport to the uterine cavity.
There is a link between blocked tubes and fibroids
First of all, in case of blocked or damaged tubes, know that there are three reviews to explore their functionality.
- Hysterosalpingography
- Laparoscopy
- Fertiloscopy
Many interventions, however banal, can damage the tubes: an appendectomy, a gynecological surgery on the ovaries or the operation of a uterine fibroid.
It is indeed essential that the uterine cavity is strictly normal in order to restore fertility. When fibroids are in the uterine cavity, they should be removed by hysteroscopic resection. A 5 mm or more conventionally 9 mm resectoscope is used to cut them chip by chip. Fibroids located far from the uterine cavity are rarely responsible for infertility and do not require surgery. In case of blocked tubes, they will also have to be removed by an operating technique identical to that used for fibroids.
Also depending on the extent of the tumor and its location, uterine fibroids can put fertility at risk.
This is because the tumor can block the fallopian tubes, deform the uterine cavity, and prevent the implantation of the embryo. Under these conditions, a uterine fibroid makes pregnancy impossible.
Fibroids , being a benign tumor, the size of which can sometimes lead to complications during pregnancy. Perhaps the cause of the obstruction of the fallopian tubes
which can occur after salpingitis (inflammation of the tubes of infectious origin), and can prevent sperm from coming into contact with oocytes.
It is important to remember that the advantages of operative laparoscopy over conventional surgery are numerous. It makes it possible to avoid the opening of the abdominal cavity and therefore results in the absence of postoperative scar, with an obvious aesthetic interest for the woman.
In addition, the duration of hospitalization is shorter than in the context of conventional surgery. Finally, the postoperative period is more comfortable for the patient, and there is a faster resumption of activity with a lower number of postoperative sequelae.
Finally, it should be noted that certain surgical indications may be justified even when the couple also has recourse to In Vitro Fertilization (IVF) or IVF with ICSI (Intra Cytoplasmic Sperm Injection), in order to improve the chances of pregnancy.
The tube-shaped uterine tubes are used to receive the oocytes released every month from the ovaries and to transport them to the uterus. When the egg is expelled by the ovaries during ovulation, it is sucked in through the pinna of the tube. Fertilization (meeting between the egg and the sperm) takes place in the tubes, during the journey from the egg to the uterus. In order for a woman to get pregnant and have a baby, the tubes must be functioning normally and be intact (at least one!). In 15% of cases of fertility disorders, the causes are linked to an abnormality of the tubes.
The exact reasons why some women develop fibroids are unknown. Fibroids tend to grow in families, and affected women often have a family history of fibroids. Women of African descent are two to three times more likely to develop fibroids than women of other races.
The fibroids develop in response to stimulation by the hormone estrogen produced naturally in the body and are sometimes the cause of wrong bite thus preventing fertilization. These growths can appear as early as age 20 but tend to decrease after menopause when the body stops making large amounts of estrogen.
Fibroids can be tiny and not a problem, or they can weigh several pounds. Fibroids generally tend to grow slowly.
The following factors have been associated with the presence of fibroids:
- Being overweight, obese
- Never having given birth to a child (called nulliparity)
- The onset of menstruation before the age of 10
How do I know if my tubes are blocked
The obstruction in the tubes is often difficult to detect because there are few symptoms (possibly some abdominal pain or more abundant vaginal secretions). Consultations and analyzes are only carried out during the infertility assessment carried out when the woman who wants a child cannot get pregnant, after having had regular and unprotected sex for 1 year.
When the tubes are blocked, it will interfere with the movement and progression of the egg and sperm. Either the egg cannot meet the sperm (and there is no fertilization) or there is fertilization, but the egg cannot progress to the uterus.
When fertilization does not take place or remains impossible, the egg is automatically lost in the abdominal cavity. We are talking about tubal sterility.
If the obstruction is not complete, the fertilized egg will be able to circulate, but will have difficulty making its way to the uterus. The egg will then implant itself in the tube and develop into an ectopic pregnancy. At some point, the tube will rupture, causing internal bleeding.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
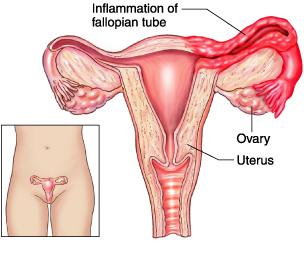
SALPINGITIS NATURAL TREATMENT
Salpingitis, what is this?
A PID is an infection of one or both fallopian tubes. A germ of sexually transmitted diseases is always responsible for the primary infection (gonococci and chlamydia especially), the infection by other pathogenic bacteria occurring only secondarily through the vaginal, blood, lymphatic or peritoneal route. However, Dawasanté experts have a natural herbal treatment for a tubal infection. Click on the image below to discover this natural treatment.
Thanks to our research, we have identified several natural home remedies that are very effective in unblocking the tubes and getting pregnant quickly. It is:
Turmeric is a natural anti-inflammatory. It can be very effective in unblocking the fallopian tubes. Curcumin, the active ingredient in turmeric, is very effective in reducing inflammation. You can consume curcumin in supplement form, add turmeric to your food, or drink a glass of turmeric.
Turmeric has no known side effects when taken in small doses. However, at doses of more than 8 grams per day, it can have unwanted effects. Make sure you take the correct dosage of turmeric or, better yet, add the spice to your cooking.
2-Garlic
Garlic is a great way to improve fertility and unclog fallopian tubes. Garlic has always been consumed for its many health benefits as the aphrodisiac properties present in garlic help in improving blood circulation in the body. Eating raw garlic every day on an empty stomach helps fight infertility in women, lowers blood pressure and cholesterol.
3- Vitamin C
Vitamin C is an antioxidant that can reduce inflammation by helping your immune system to function better. For this reason, it is ideal for healing scars and may have a positive effect on the fallopian tubes.
If you suspect that the cause of the blocked fallopian tubes is an infection, vitamin C can help you overcome it. To unclog your tubes, we recommend that you use natural vitamin C. It's easy to get vitamin C from food sources, especially when you like citrus fruits. Eat as many oranges, lemons, and grapefruit as possible. Aside from, you can try strawberries, broccoli and green peppers to heal yourself with a good vitamin C.
4- Castor
oil Castor oil has been used for centuries to improve fertility in women, and more especially to unblock the fallopian tubes. How is it used?
- dipped a rag in castor oil
-Place this cloth on the skin on the lower abdomen. This will improve circulation and promote healing of the tissues and organs under the skin. Castor oil therapy helps the fallopian tubes by softening tissue and improving circulation in the pelvic area.
5- Apple cider
vinegar Apple cider vinegar is a fermentation product that produces yeasts and bacteria that are beneficial for unblocking the tubes. This is because vinegar contains a number of vitamins and minerals, including magnesium, potassium, copper, group B vitamins, and vitamin C. Taken daily, it can help unblock the fallopian tubes by balancing hormones and shrinking fibroids.
Directions:
-Mix 2 tablespoons of apple cider vinegar in 1 glass of water
-You can add a touch of honey or molasses to soften the mixture.
-You can drink the mixture right away or sip it for 30 minutes.
6-Meditation
Meditating daily will help you decrease stress levels and promote general healing. However, reducing stress reduces deterioration and inflammation of the fallopian tubes.
As an additional tip, don't forget to start meditating with a short session consisting of breathing exercises and relaxation techniques. Even if you only do it for a few minutes, meditation will provide you with positive energy to start your day and reduce your stress.
7- Fertility massage
Some practitioners of alternative medicine suggest fertility massages unblock the fallopian tubes. These usually involve hot oil massages in the abdominal area. How to do a fertility massage?
- Lie down on an exercise mat with your face up and a pillow under your lower back.
-Relax and apply almond, olive, or lavender oil to your hands and apply by massaging your pubic bone, as the uterus is below this bone.
-Gently massage from bottom to bottom and pull your abdominal wall towards the navel. Maintain this position, count to 10 and release your hands. Repeat this maneuver 10 to 20 times.
NB: Do not do this if you are bleeding or are pregnant. Also, if possible, visit a massage therapist who specializes in abdominal massage for best results.
8- Mugwort
Mugwort is a plant sometimes recommended to improve female fertility. It is also recommended for unblocking the fallopian tubes.
Mugwort has a long history of use for fertility in a number of different cultures. It has been used all over Europe and Asia for centuries. It is often used in Chinese medicine in the form of moxibustion, which involves burning mugwort above an acupressure point.
9- Green clay
The use of green clay to unclog the proboscis is very common in East Africa.
The blocked tubes are unblocked by the serious treatment of green clay and the follow-up of a feeding program made by a dietician or a naturotherapist.
OVARIAN CYST OPERATIONS AND NATURAL TREATMENT
What are Ovarian Cysts
The ovarian cysts are sacs filled with fluid that can develop in or on your ovaries. Most ovarian cysts are harmless and go away on their own. But you may need to have an operation to remove a cyst if it is causing you pain or discomfort or if there is a chance that it is cancer.
Ovarian cysts are usually removed using a surgical procedure called laparoscopy (a type of keyhole surgery), but sometimes open surgery is necessary. Your procedure will be performed by a gynecologist.
Dawasante's natural treatment for ovarian cyst
If you have polycystic ovary syndrome and are looking for a natural treatment that will cure you and prevent you from having the operation, this is the natural treatment for you. We offer you an all-natural treatment to cure your Ovarian Cysts. It is therefore made up of three elements: herbal teas, a poultice, and vaginal eggs. It is an effective, fast and long-lasting natural remedy that allows cysts to be permanently removed. All elements of our treatment are natural and herbal. Then trust us! So this is the secret to curing ovarian cysts without surgery.
This natural herbal treatment for ovarian cysts has proven its effectiveness with dozens of resolved cases. This herbal tea is the miracle solution to permanently cure ovarian cysts.
To discover our treatment for ovarian cysts, click on the image below
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
Prepare for the removal of the ovarian cyst
You will get information from your hospital on how to prepare for your operation. If you smoke, for example, you will be asked to quit. Smoking increases your risk of getting an infection after surgery, which can slow your recovery. It can also lead to complications.
Ovarian cysts are usually removed with keyhole surgery as a daily procedure. This means you can probably go home the same day, although sometimes it is necessary to stay overnight.
Before you start, ask a friend or family member to take you home after your procedure. And make sure there can be someone home with you for the first 24 hours.
The operation is performed under general anesthesia, so you will sleep during the operation. You will be prompted to follow the fasting instructions. This usually means not to eat or drink anything other than clear fluids about six hours before your surgery. You can usually drink water for up to two hours before your surgery, but not after. It is important to follow the advice given by your hospital.
You may be asked to wear compression stockings to help prevent blood clots from forming in the veins in the legs.
Your gynecologist will discuss with you what will happen before, during, and after your procedure, including any pain, you may be feeling. If you are unsure of something, don't be afraid to ask. No question is too short. It is important that you feel fully informed so that you can give your consent to the procedure. You may be asked to do so by signing a consent form.
What are the alternatives to ovarian cyst removal?
If an ovarian cyst is not causing you any symptoms, your gynecologist may simply suggest that you monitor it rather than undergo treatment. You will need to attend regular appointments for an ultrasound to check if the cyst is clearing or changing in size. If you are under 50, most ovarian cysts will go away on their own within two to three months.
What Happens During Ovarian Cyst Removal?

Removal of the ovarian cyst is usually done through keyhole surgery, but sometimes a larger cut is needed (open surgery). Your gynecologist will discuss with you the type of operation best suited to your situation.
Read: Ovarian cyst and ginger, natural treatment
Keyhole surgery (laparoscopy)
Simple or small cysts can usually be removed with surgery. If you are having keyhole surgery, your gynecologist will make two or three small cuts (between 5mm and 1cm long). One will be near your belly button and two will be lower, usually one on each side. They will pass small instruments and a tube-shaped telescopic camera (called a laparoscope) through the cuts. This procedure is called laparoscopy. Your gynecologist will then examine your ovaries and remove the cyst. The cuts on your skin are closed with glue or stitches.
Open surgery (laparotomy)
In some situations, your gynecologist may need to perform open surgery. This is when a smaller, larger cut is made in your lower abdomen (tummy) to reach your ovary. Your gynecologist may recommend that you have open surgery if the cyst is very large or if it is possible that it is cancerous. Or, they may need to change the laparoscopy to open the surgery during the procedure in order to safely remove your cyst. In some circumstances, it may be necessary to remove your entire ovary during the procedure.
What to expect after
After your laparoscopy, your nurse will make sure you are not in pain and let you rest for a few hours. They will offer you something to eat and drink. You can usually go later in the day when you feel ready. Someone should take you home, and a friend or family member should stay with you overnight.
Your nurse will give you advice on how to treat your injuries before you go home. They will probably want to check that you can urinate properly before you go home, and will also give you painkillers to take. You may be given a date for a follow-up appointment.
Having general anesthesia affects everyone differently. You may find that you are not as well coordinated or that it is difficult to think clearly. It should pass within 24 hours. In the meantime, don't drive, drink alcohol, operate machinery, or sign anything important. Always follow the advice given by your gynecologist or the hospital.
If your gynecologist used soluble stitches, these will go away on their own. The other stitches may need to be removed by your GP's office nurse. It will usually be around five to seven days after your operation.
Recovery from ovarian cyst removal
Your body needs time to heal after surgery. Everyone is different. You may feel tired and need to take a nap for a few days after you get home.
But it is also important for your recovery that you stand up. Try to take a few short walks (10-15 minutes) in the first few days, then increase gradually. One week after the operation, most women can walk slowly and steadily for 60 minutes. After about two weeks, they returned to their normal level of physical activity. You should avoid heavy lifting for four weeks.
You will likely be able to return to work a week after the procedure, but this may depend on the type of work you are doing. It may take a week or more. The time it takes to recover will also be affected by whether you've had keyhole or open surgery. It takes longer to recover from open surgery. If you have questions about your recovery or when you can resume particular activities, ask your gynecologist. It is important to follow their advice.
If you need pain relief, you can take over-the-counter pain relievers such as paracetamol or ibuprofen.
Side effects of ovarian cyst removal
After your surgery, you may have side effects. These should be mostly temporary and can include:
-Pain or discomfort in the lower abdomen for a few days after your operation;
-Pain in the shoulders;
-A small amount of vaginal bleeding for up to 48 hours;
-Feeling more tired than usual for a few days
Complications of ovarian cyst removal
Complications arise when more serious and unexpected problems occur during or after your procedure.
Most women recover well after the removal of the ovarian cyst. Keyhole surgery causes fewer complications and has a shorter recovery time than open surgery.
Possible complications from any type of surgery include bleeding or a blood clot, usually in a vein in the leg (deep vein thrombosis - DVT). You could also develop an infection.
Removing the cyst from the ovary can damage other organs, such as the bowel, ureters or bladder, but this is unusual.
Your ovaries produce important hormones and eggs, which can be fertilized. Your gynecologist will try to preserve your ovaries so that your hormones are not affected and you can still have children, but this may not always be possible. Before your procedure, your gynecologist should discuss with you the risk of losing an ovary during the operation.
If you have any of the following symptoms, you should contact the hospital where you had your operation:
-Stomach pain that gets worse
-A high temperature, especially if you have also lost your appetite or are ill;
-Red or sore skin around your scars;
-Burning or tingling sensation when you urinate more often, or that you cannot do so at all;
-Pain, swelling, redness, or a feeling of heat on the legs.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
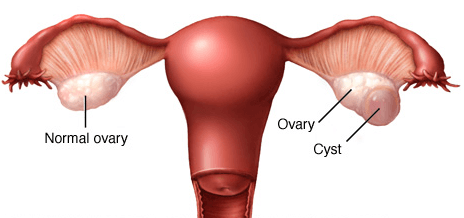
OVARIAN CYST AND PREGNANCY NATURAL TREATMENT
Ovarian cysts are sacs or pockets filled with fluid in an ovary or on its surface. Women have two ovaries; Each is the size and shape of an almond and is located on the side of the uterus. The ova (eggs), produced and ripe in the ovaries, are released in monthly cycles during fertile years.
Many women have ovarian cysts at some point. Most ovarian cysts do not present with much discomfort (or very little) and are not harmful. Most go away without treatment within a few months.
However, ovarian cysts (especially those that have ruptured) can cause severe symptoms. To protect your health, perform regular pelvic exams and familiarize yourself with symptoms that may indicate a problem that may be serious.
Dawasante's natural remedy for ovarian cysts
If you have polycystic ovary syndrome and are looking for a natural treatment that will cure you and prevent you from having the operation, this is the natural treatment for you. The herbal tea is made up of several herbs that regulate the hormone levels and the size of your cysts. Indeed, it contains several plants that will mimic the action of estrogen in your body. It is the best natural remedy for curing ovarian cysts. Usually, except when the diagnosis is too late, our natural treatment will cure ovarian cysts without side effects.
To discover our natural treatment for ovarian cysts, click here!!!
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
Symptoms that indicate an ovarian cyst
Most cysts don't cause any symptoms and go away on their own. However, a large ovarian cyst can cause:
-Pelvic pain: dull or severe pain in the lower abdomen on the side of the cyst;
-Feeling of fullness or heaviness in the abdomen;
-Swelling
The causes of ovarian cysts
Corpus luteum cyst
Most ovarian cysts occur after the menstrual cycle (functional cysts). Other types of cysts are much less common.
Functional cysts
Structures similar to cysts, called "follicles," usually develop every month. The follicles produce the hormones estrogen and progesterone and release an egg when you ovulate.
If a normal follicle continues to grow, it is called a “functional cyst”. There are two types of functional cysts:
· Follicular cyst Approximately in the middle of the menstrual cycle, an egg leaves its follicle and passes through the fallopian tube. A follicular cyst begins when the follicle does not break or release the egg, but continues to grow.
- Corpus luteum cyst. When a follicle releases the egg, it begins to produce estrogen and progesterone for conception. The follicle is now called the "corpus luteum". Sometimes fluid collects inside the follicle, which causes the corpus luteum to expand and a cyst to form.
Functional cysts are usually harmless, rarely cause pain, and usually go away on their own within two or three menstrual cycles.
Other cysts
Types of cysts that are not related to the normal functioning of the menstrual cycle are:
· Cyst dermoid. These cysts, also called "teratomas", can contain tissue, such as hair, skin or teeth, because they are formed from embryonic cells. They are usually not cancerous.
· Cystadenomas These form on the surface of an ovary and may be filled with a watery or mucous material.
· Endometriomas They are formed as a result of a disease in which uterine endometrial cells develop outside the uterus (endometriosis). Some tissue can adhere to the ovary and form a lump.
Dermoid cysts and cystadenomas may be enlarged, which can cause the ovary to move out of its position. This increases the possibility of a painful torsion of the ovary, called "ovarian torsion". Ovarian torsion can also cause blood flow to the ovary to decrease or stop. In fact, ovulation is the release of an egg from one of the ovaries. It usually occurs in the middle of the menstrual cycle, although the exact time may vary.
In preparation for ovulation, the uterine lining, or endometrium, thickens. The pituitary gland in the brain stimulates one of the ovaries to release an egg. The wall of the ovarian follicle breaks on the surface of the ovary. The egg is released.
Elongated structures called "fimbriae" carry the egg to the nearby fallopian tube. The egg travels through the fallopian tube, driven in part by contractions of the walls of the tube. Once in the fallopian tube, the egg can be fertilized by a sperm.
If the egg is fertilized, the egg and sperm join together and form a single-celled entity called a zygote. When the zygote moves down the fallopian tube into the uterus, it begins to divide rapidly and forms a group of cells called blastocysts, which looks like a small raspberry. When the zygote reaches the uterus, it is implanted in the uterine lining and pregnancy begins.
If the egg is not fertilized, the body simply reabsorbs it, perhaps even before reaching the uterus. About two weeks later, the lining of the uterus breaks off and is expelled through the vagina. This is called menstruation.
Risk factors
The risk of having an ovarian cyst increases due to:
· Hormonal problems: These include taking clomiphene (Clomid), a fertility medicine used to stimulate ovulation.
· Pregnancy: Sometimes the cyst that forms when you ovulate stays in the ovary throughout the pregnancy.
· Endometriosis: This condition causes uterine endometrial cells to grow outside the uterus. Some tissue can adhere to the ovary and form a lump.
· A severe pelvic infection: If the infection spreads to the ovaries, it can cause cysts to form.
· A previous ovarian cyst: If you have a cyst, you probably have more.
I have cysts and I'm pregnant… Is it time to panic?
Ovarian cysts are common in early pregnancy, even if you are not having your period. Usually, these cysts are harmless, just like most other ovarian cysts.
· However, if the cysts continue to grow throughout your pregnancy, there are a few possible problems. They can break, twist, or even cause problems during childbirth. This is one of the many reasons why it is important to stay under the care of an obstetrician/gynecologist during your pregnancy and throughout your life.
- If you have polycystic ovary syndrome you are at increased risk for gestational diabetes, pregnancy-induced high blood pressure, miscarriage or premature delivery.
· Talk to your OB / GYN about your risks and potential treatment options. She will provide you with a full set of options and recommend the best treatment to help you have the healthiest pregnancy possible.
Ovarian cysts: what consequences before pregnancy?
- Most of the time, having one or even more ovarian cysts does not prevent you from getting pregnant. Functional cysts do not really interfere with fertility (many women get pregnant naturally without even suspecting their presence) or only temporarily, while they resolve. For example, a follicular cyst can prevent ovulation during one cycle, but may not interfere with ovulation in the next cycle. In addition, if these cysts are slow to leave, hormonal treatment can accelerate their disappearance and return to a normal menstrual cycle with good ovulation.
- As for endometriosis and polycystic ovary syndrome, they can have a very small or greater impact on fertility depending on the severity of the disease: if necessary, treatment can be implemented to facilitate pregnancy. In general, large endometrial cysts are removed surgically while hormonal stimulation often helps to ovulate normally in polycystic ovary syndrome. Many women thus manage to become pregnant and carry on their pregnancy after these treatments.
Ovarian cysts: what consequences during pregnancy?
- It happens that an ovarian cyst is discovered accidentally, during a mandatory ultrasound during pregnancy. A small asymptomatic cyst often only requires simple monitoring, to make sure that it does not grow too large: normally, it will not interfere with the development of your future baby, or even your delivery.
- In the end, it is especially the cysts causing severe pain that must be removed surgically. The same can be said for very large ovarian cysts, which are often removed as a preventive measure (without treatment, a large cyst could trigger ovarian torsion). If this type of cyst is discovered during the very first months of your pregnancy, the operation will normally be postponed until the beginning of the second trimester: at this stage, it will no longer present any particular risks for your baby. In the meantime, the doctor may give you a rest.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527

OVARIAN CYSTS AND GINGER: Natural treatment
The ovarian cysts are sacs or fluid-filled sacs that develop in or on the surface of one or both ovaries of a woman. Most women will develop at least one cyst at some point in their life.
Dawasante's natural remedy for ovarian cyst
It is with the aim of remedying it and completely eradicating ovarian cysts that the health experts at Dawasante offer you natural herbal solutions. Click on the image below to discover this natural treatment. This natural herbal treatment for ovarian cysts has proven its effectiveness with dozens of resolved cases. This herbal tea is the miracle solution to permanently cure ovarian cysts. Indeed, it contains several plants that will mimic the action of estrogen in your body. Herbal tea is made up of several herbs that regulate the hormone levels and the size of your cysts. So this natural remedy will help you to relieve the pain of the menstrual cycle and regulate your cycle. The herbal tea will also expel waste from your uterus. Usually, except when the diagnosis is too late, our natural treatment will cure ovarian cysts without side effects.
To read more about our natural remedy and place an order, click here!
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
Symptoms of an ovarian cyst
Most ovarian cysts are considered functional, which means that they usually occur during the menstrual cycle and are not part of a disease process.
They are usually benign and for no apparent reason. Pathological cysts, on the other hand, can be either benign or cancerous.
Often people are unaware of ovarian cysts because they usually don't cause problems. However, in some cases, they can cause symptoms like abdominal bloating, pain during bowel movements, menstrual irregularities, pelvic pain before or during the menstrual cycle, pain during sex, pain in the lower back or thighs, pressure in the rectum or bladder, nausea, and vomiting. Certain types of ovarian cysts can also cause reduced fertility.
In many cases, ovarian cysts go away on their own within a few months. However, if they cause discomfort, there are many natural remedies that can help relieve symptoms and reduce the size of cysts.
Ginger and cysts
Ginger is a potent anti-inflammatory herb that reduces inflammation and relieves pain. Additionally, ginger increases heat in the body and induces menstruation.
Ginger juice still has its anti-inflammatory properties and it heals the joints. It reduces and with the passage of time the inflammation in the body completely ends. Small cysts can be removed completely with ginger juice.
Ginger tea is also a very effective natural remedy for natural relief of pain associated with ovarian cyst. It also has both antioxidant properties. Studies by Dawasante's experts have proven that ginger stops the growth of ovarian cysts.
How is it used? All you need to do is immerse the ginger tea bag in boiling water for a few minutes. If you don't like the taste, consider adding a squeeze of lemon.
How to make fresh ginger tea at home:

-Peel and cut a 2 inch piece of ginger.
-Boil the ginger in 2 cups of water for 10 minutes.
-Then remove from heat and add flavorings like lime juice and honey to taste.
Ginger has a strong aroma. This healthy herb can be used dried, powdered, fresh, in juice, oil or pickle form. Ginger has its own place in different cooking but apart from useful for dishes; it has many health benefits as well.
The health benefits of ginger
· Useful in suppressing allergic reaction.
· Useful in the treatment of stomach problems.
· Beneficial for treating loss of appetite.
· In the treatment of nausea useful caused by the treatment of cancer.
· Helps get rid of morning sickness.
· Useful in preventing vomiting and nausea after surgery.
· As well as beneficial in the treatment of stomach aches, colic, diarrhea and gas.
Nutritional values of ginger
Ginger is loaded with bioactive compounds and nutrients, which are very helpful for the brain and body. Ginger is rich sources of
· Beta carotene.
· Iron.
· Calcium.
· Silicon.
· Sodium.
· Magnesium.
· Potassium.
Vitamin A, B, E and B complex.
Here are some health benefits of ginger.
Certain conditions that ginger can help cure
Treat stomach pain
Ginger is rich in carminative properties which are really helpful in treating upset stomach. It helps prevent bloating and gas by relaxing the gastrointestinal muscles. It is well known for the treatment of diarrhea caused by bacteria. It is also useful in stomach alignment such as dyspepsia or colic. Dyspepsia is chronic in the digestion which results in feeling unwell in the upper part of the stomach.
It is therefore highly recommended to eat ginger after every meal in high quantity because studies reveal that ginger speeds up the process of emptying the stomach.
Helps prevent cancer
Cancer is a fatal disease resulting from the uncontrollable production of abnormal cells. Study reveals that ginger extract is considered an alternative treatment for different types of cancer. From colorectal cancer to ovarian cancer, ginger is very helpful.
The University of Minnesota study finds that ginger slows down the production of abnormal cells in colorectal cancer. Therefore prevent the nature cloning of cancer to produce abnormal cell to a large extent.
Ginger is also very useful in the treatment of skin, lungs, prostate, breast as well as pancreatic cancer.
Advice
· Adding ginger to your daily meal is a great way to keep cancer at bay.
Releasing Headaches
Ginger provides simple headache relief as well as migraine prevention through the synthesis of prostaglandin. Therefore helps to relieve pain in the blood vessels.
First method
· Take 3 tablespoons of powdered ginger.
· Add little water to make the paste.
· Apply the paste on the forehead.
· Repeat the steps whenever you feel headache and get relief.
Second method
· During the headache or migraine attack, having a cup of ginger tea would definitely minimize the pain.
InJoint pain relief from arthritis
Ginger has a rich property of anti-inflammatory so it revives in arthritis joint pain
First method
· Make a paste of turmeric and ginger powder.
· Apply to the affected area.
· Massage the area well.
· Follow this method twice a day.
Second method
· Apply a little ginger oil to the joints and muscles.
· Massage delicately.
· Add this method to your bath to relieve itchy joints and muscles.
Relieve menstrual pain
Ginger is a natural pain reliever. By eating ginger at the start of the menstrual period, women can feel relief from the symptoms of menstrual pain and difference.
First method
· Before the start of the menstrual period, at least four days before, add ginger to your daily meal.
Second method
· Take 1/4 piece of fresh ginger.
· Cut it into small slices.
· Boil a cup of water and add small slices of ginger in it.
· Boil for 2 minutes.
· Add a little honey or sugar.
· Switch off the stove.
· Drink ginger tea.
Third method
· Use ginger capsules.
These tested tips would be really helpful in relieving your menstrual period pain in women
Improve brain function and defend against Alzheimer's disease
Constant oxidative anxiety and inflammation can speed up the aging process. They are thought to be surrounded by the main drivers of Alzheimer's disease and age-related cognitive turn number down. Studies in animals have shown that the antioxidants and bioactive compound in ginger can slow down inflammatory reactions that take place in the brain. There are also some verifications that ginger can openly improve brain function. In a study of 60 middle-aged women, ginger extract was made public to gain better reaction time and functioning remembrance. There are also abundant studies in animals showing that ginger can save harm against age-related turn in the brain's role.
The vigorous ingredient in ginger can help fight infections
Gingerol, the bioactive material in fresh ginger, can be of help in reducing the threat of infections. In fact, ginger extract can curb the development of many different types of germs. It is very useful aligned with oral bacteria connected to inflammatory gum disease, the same as gingivitis and periodontitis. Brand new ginger can also be helpful in opposition to RSV virus, a regular cause of respiratory infections. Ginger helps perk up the immune structure. Consuming a small piece of ginger per day can help leaf possible danger of a stroke by retaining fatty deposit in the arteries. It also reduces bacterial infections in the abdomen, and helps fight a terrible cough and throat discomfort.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
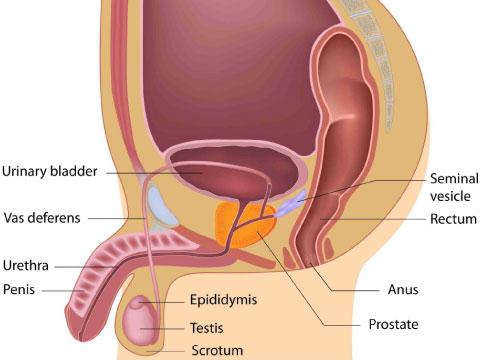
CHRONIC PROSTATITIS NATURAL TREATMENT
CHRONIC PROSTATITIS NATURAL TREATMENT
Infection of the prostate gland. Germs can come from outside through the urethra or come in through the blood. It can be due to endoscopic investigations, the introduction of instruments through the urethra to the bladder.
There is an acute form and a chronic form, with the presence of small abscesses, often due to an acute form that is poorly treated. Chronic prostatitis is not necessarily the sequel of acute prostatitis but of a recurrent urinary tract infection. Discover the natural treatment based on medicinal plants to cure prostatitis permanently without operation. Click on the image below to discover this natural treatment.
Our natural remedy is made of plants effective in treating prostatitis and some other male sexual problems. We have selected the best plants Africa had to offer to treat prostatitis.
To contact our experts please call or write to us on the following number, tel / WhatsApp
+22996374527
WE DELIVER ALL OVER THE WORLD
The functional disorders from there one would be defined by the term "prostatism" which includes: pollakiuria, dysuria, urgent urination.
If natural solutions exist, let's be clear: we are not kidding with prostate pathologies. Therefore, in cases of prostatic adenoma with acute urinary retention (RAU, in short, one can no longer urinate), or cancer of the gland, it is not allowed to stop allopathic treatment for natural therapeutic strategies. They can, however, be perfectly complementary.
Furthermore, we keep repeating it, self-treatment and self-medication are to be avoided. A true naturopath, or any health worker worthy of the name, is a professional who establishes sensitive protocols adapted to each case and each patient. However, the rules that we are going to advise you to follow our common sense and will give you an idea of the remarkable range that complementary medicines offer.
Some tips to get rid of prostatitis
Tobacco is taboo

First of all, it should be noted that losing weight is a prerequisite. As in many cases, being overweight weighs (no pun intended) on the health balance. A diet too high in calories increases all types of cancer, especially prostate cancer. Studies have shown that reducing calorie intake has a beneficial effect on prostate cancer.
Eliminating tobacco is also obvious. In smokers, prostate cancer - which is, as we have said, a slowly growing cancer - is more aggressive and more advanced than in non-smokers. Tobacco increases the risk of developing prostate cancer by 30%. In addition, smoking stimulates the growth of prostate cells. In question, the cadmium contained in the volutes.
Food

For effective food reform, the indications are often the same. It is therefore advisable to favor a balanced diet in proteins, carbohydrates and lipids, of organic quality, seasonal (and therefore adapted to each of them), and according to the needs of each one. Fruits and vegetables, therefore, rich in vitamins, minerals, and antioxidants, and fibers. If possible, we will prepare and consume these products as less cooked as possible to preserve the nutritional elements they contain and thus ensure optimal bio-assimilation. (except in certain cases, such as in people suffering from colitis, who will favor fruit or vegetable juices).
Avoid saturated animal fats and prefer unsaturated fats. We recommend consuming mackerel, sardines, herring, walnuts and first cold-pressed virgin and organic vegetable oils for the lipids essential to our cells. For zinc, opt for almonds and pumpkin or squash seeds, but also oysters and brewer's yeast. Zinc has the advantage of inhibiting the activity of the 5-alpha reductase enzyme which allows the transformation of testosterone into dihydrotestosterone, responsible for the enlargement of the prostate. Limit dairy products.
Herbs That Relieve Infectious Prostatitis
The many virtues of plants are often overlooked by patients who systematically go to a doctor at the first signs. In fact, it is possible to relieve yourself with plants when you have infectious prostatitis.
First make sure that there are lots of fruits and vegetables in your diet, especially:
> The broccoli, the cabbage flower or spinach.
> Apples, olives, black cherries, berries, citrus fruits, and grapes go a long way in reducing the signs of prostatitis, as these fruits are rich in quercitrin: an anti-inflammatory plant compound.
As far as plants are concerned, the seeds of squash have proved their worth in restoring hormonal balance through their action on the muscles of the bladder.
Palmetto plants in preparation reduce pain, while poplar regulates prostate, and penis gold regulates the kidneys.
Professionals also recommend nettle which helps to treat urinary tract dysfunctions: difficulty urinating, poor urine flow. The roots and leaves of nettle combined with opuntia and small-flowered fireweed flowers facilitate urination.
Hay flowers also have positive effects on the prostate.
To talk more about nettle:
Nettle roots

Stinging nettle or stinging nettle (Urtica dioica ) is often cited for its anti-inflammatory properties and for preventing the growth of prostate tissue. For this indication, it is the root that is used, especially at the beginning of the disorders, because it would make it possible to slow down the evolution of the adenoma and to reduce the frequency of urination. If the quality of scientific studies in this area is sometimes deemed insufficient, the European Commission, as well as the WHO (World Health Organization), nonetheless recognize as "clinically established" its use in "the treatment of urine emission problems associated with mild to moderate benign prostatic hypertrophy, when the absence of prostate cancer is proven". Doctor Jean-Michel Morel, who teaches herbal medicine at the faculty of Besançon, recommends nettle roots in the form of EPS (in pharmacies) at the rate of a teaspoon of 5 ml in the evening before meals in a glass of water. We can also consider consuming the roots in decoction (one teaspoon of dry roots per cup of water to boil for 5 minutes then let infuse 10 minutes, three times a day).
Saw palmetto and African plum

Frequently associated with nettle, saw palmetto or Florida palm ( Serenoa repens Small), formerly known as Sabal serrulata, is the other plant associated with the prostate and urination disorders in herbal medicine. It is the fruits of this small palm tree from the United States that are used and presented in the form of medicine. More than ten studies demonstrate its effects on the frequency of urination (and nocturnal awakenings). The bark of the African plum ( Prunus Africana ) has similar effectiveness, but this large tree native to Madagascar is said to be endangered, and for this reason, it is best to turn to Florida's palm.
Fireweed

This beautiful pink flower, common in the Alps, shows promise for treating an enlarged prostate. Dr. Kurt Hostettmann, a leading phytomedicine researcher, tells how he discovered their properties: "At the age of 65, my own father had problems with urination and he refused the prostate surgery he was offered. I had read that Maria Treben, an Austrian herbalist, recommended this plant, as she had observed in entrenched valleys of Austria. that it was consumed in herbal tea, as a tea substitute, and that prostate surgery was much less important there than elsewhere. It wasn't based on any scientific study, but I suggested my father try it. What he did. Morning and evening he took his fireweed infusion, and after three to four weeks his nighttime urination decreased markedly. He never had prostate problems again until his death nearly twenty-five years later. "On the strength of this first experience, Dr. Hostettmann then entrusted this subject of his doctoral thesis to one of his young collaborators. .
Fireweed was effectively effective in fighting prostate adenoma, limiting the number of urinations, strengthening the urinary stream and flow, by the same mechanism as that of current synthetic drugs (inhibition of 5-alpha reductase, the enzyme responsible for hypertrophy). The active ingredients of the plant are mainly present in the tannins, which are soluble in water. Hence its effectiveness in the form of herbal tea (for example 20 days per month). There are several varieties of fireweed, and the recommended ones are the fireweed ( Epilobium parviflorum Schreb) because they contain as many active ingredients, but less tannins, which could in the long run irritate the stomach. Some research suggests the usefulness of fireweed against prostate cancer cells, but this remains to be confirmed.
Pumpkin seeds

Finally, pumpkin seeds are also frequently cited to reduce the symptoms of benign prostate adenoma and are well known to Germans for this property. They are easily found in any store, and if their virtues on the prostate are not fully established, their richness in nutrients makes them an interesting health food to consume daily.
Against prostate cancer: coffee and tomatoes


No plant to date can accompany or cure prostate cancer. On the other hand, in prevention, a large study carried out among 48,000 people by the National Cancer Institute was able to establish that consumption of 6 cups of coffee per day reduced the risk of 60% of being affected by cancer of the prostate. Unfortunately, consuming so much coffee daily is not reasonable: in addition to a phenomenon of dependence, excess caffeine causes many side effects, such as nervousness, restlessness, anxiety, palpitations, insomnia, stomach irritation. , diarrhea ...
The good news, decaffeinated offers the same virtues. It is indeed the polyphenols in coffee, and not caffeine, which gives it these preventive properties. A similar study published by the same institute also showed that consuming cooked tomatoes two to three times a week reduces the risk of developing prostate cancer by a third (compared to occasional consumption). Finally, a healthy lifestyle remains effective prevention: avoiding exposure to toxic products, including pesticides (farmworkers are more exposed to this cancer), being active and limiting the consumption of red meat, cold meats, and cheeses, fatty, while favoring large rations of fruits, vegetables and fish.
Some other plants that help with prostate problems
- BUCHU: This plant comes from Africa and is considered a urinary antiseptic. It contains an oil that increases urine production
- Chamomile: An infusion or tea is believed to have calming effects on cramps or painful symptoms in the genitourinary system. Combines well with valerian and marshmallow.
- Garlic: Good for spasms and cramps. Combines well with Echinacea and Goldenseal to treat microbial activity.
- Cramp Bark: Bark Has antispasmodic, sedative, nervine and astringent properties. Designed to have potent antispasmodic effects on the genitourinary system in both men and women.
- Pumpkin Seeds: Pumpkin seeds are a natural source of zinc and linoleic acid (vitamin F). It is believed to play an important role in decongesting the prostate and reducing residual urine.
- Watermelon Seeds: Help prevent excessive urine buildup due to prostatitis and BPH. Works well with Uva Ursi and Buchu.
To contact our experts please call or write to us on the following number, tel / WhatsApp +22996374527
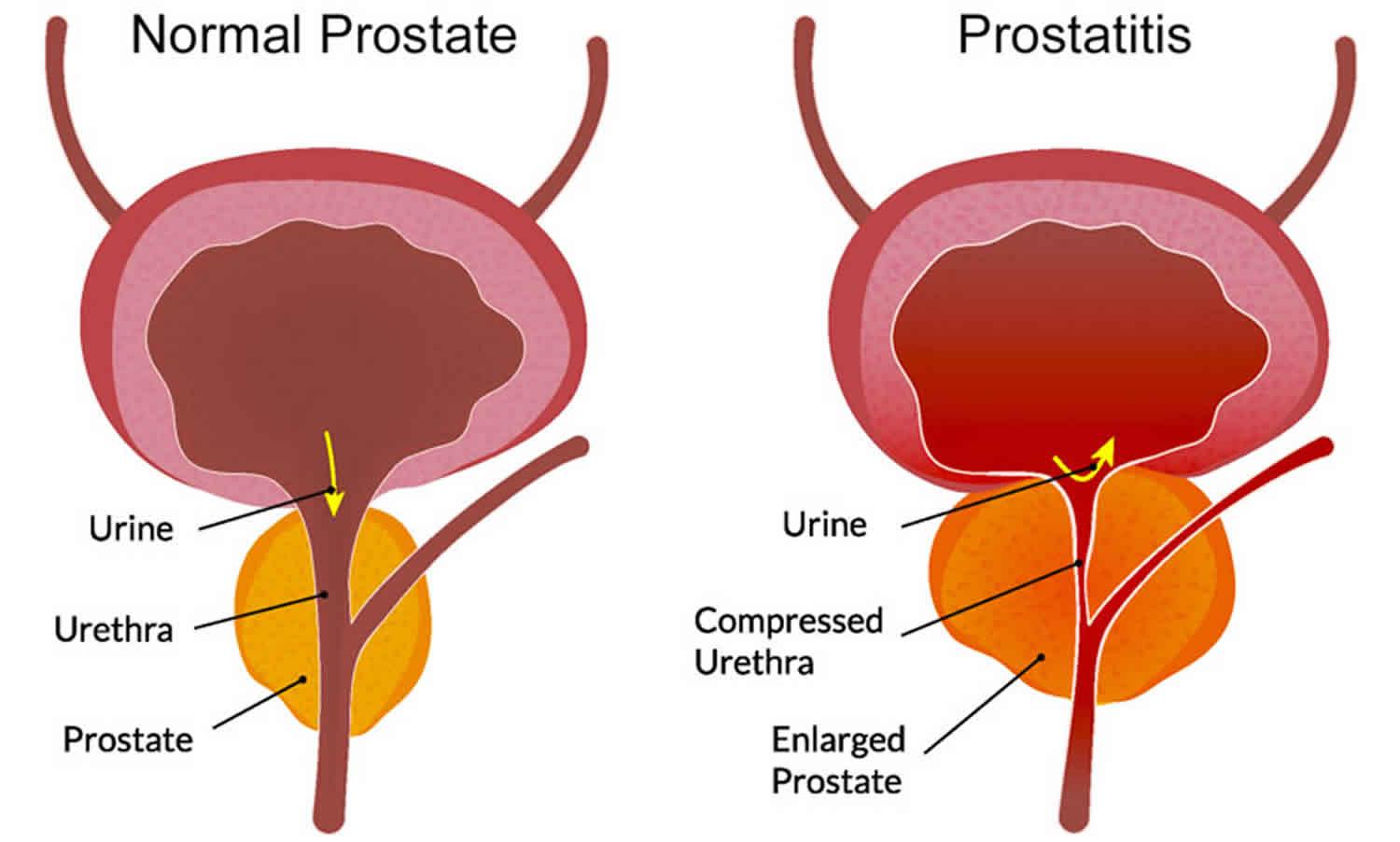
PROSTATITIS SYMPTOMS: Natural plant-based treatment
PROSTATITIS SYMPTOMS
Prostatitis is a painful inflammation of the prostate. It is a common condition that can affect men of all ages.
Dawasanté experts provide you with a natural treatment based on medicinal plants to cure prostatitis permanently.
HERBAL TREATMENT FOR PROSTATITIS
We have the right and ideal plants for healing prostatitis. They are used to slow the growth of the prostate, by reducing the "fuel" of prostate cells: benign prostatic hypertrophy and prostate cells work with the same factors and use the same "fuel".
These plants are also effective when the volume of the prostate is visible, above 40 m. Obtaining their relaxation and promoting the opening of the funnel of the neck of the bladder and the prostatic urethra. They thus improve the emptying of the bladder. These plants are the first phytotherapeutic approach to reduce the frequency of urination and improve the spray.
To discover our remedy to cure prostatitis, click here!
To contact our experts please call or write to us on the following number, tel / WhatsApp
: +229 51374202
Acute bacterial prostatitis
Acute bacterial prostatitis is caused by bacteria. It is said to be acute because its symptoms appear suddenly and can be severe. It is the least common type of prostatitis, but the easiest to treat.
Chronic bacterial prostatitis
Chronic (long-term) bacterial prostatitis is caused by bacteria and often persists for several months. Its symptoms are usually less severe than those caused by acute bacterial prostatitis and tend to go away and then come back. Chronic bacterial prostatitis can cause urinary symptoms like a burning sensation or pain during urination, but it does not cause fever or chills. It seems to occur more often in older men with benign prostatic hyperplasia.
This type of prostatitis is the most common. This is a chronic condition that is not caused by bacteria and causes pain or discomfort that may go away and return to the pelvis.
Asymptomatic inflammatory prostatitis
The prostatitis Asymptomatic inflammatory causes no symptoms and does not require treatment. Doctors often diagnose it when they do tests to check for other conditions, such as prostate cancer, or to determine the cause of infertility. To ask this
Prostatitis can cause the following signs and symptoms:
At first, prostate cancer does not cause any symptoms. Note that those shown below may be related to another prostate disease, such as benign prostatic hypertrophy.
- Difficulty urinating: difficulty starting to urinate or holding urine, inability to urinate, need to urinate frequently (especially at night), poor urine output, a burning sensation or pain when passing urine 'urinate.
- The blood in the urine or semen.
- Pain or frequent stiffness in the lower back, hips or upper thighs.
- Changes in urinary function: frequent urge, urge to urinate, need to push, urine retention, burning while urinating.
- Genital changes: painful ejaculations, or difficulty getting an erection. Predisposed people
Note that some " at-risk " men will never get prostate cancer. Several risk factors are being studied.
- Age. In North America, prostate cancer mainly affects men over the age of 60. The average age at diagnosis is 70 years, and 80 years at the time of death. Younger, only 0.5% of prostate cancers appear before age 50, and 22% between 55 and 64 ...
- Family history. The risks are higher when the father or a brother has already suffered from this disease, which suggests a genetic predisposition. This hypothesis is reinforced by the discovery that carriers of the BRCA1 and BRCA2 genes have an increased risk of prostate cancer.
- Ethnic origin. Men of African descent are more at risk than Caucasians, who are more at risk than Asians. It is estimated that Indians and Chinese are about 50 times less affected by prostate cancer than Westerners. However, when they migrate to countries where the disease is more common, their risk also increases. This suggests that factors not only related to genes but also to diet exert an influence.
- Obesity: A man who is significantly overweight has a higher risk of having prostate cancer detected at an advanced stage.
- Inflammation or infection of the prostate increases the risk of prostate cancer when it lasts a long time.
- Tall men have a higher risk of prostate cancer.
- Men who have been exposed to pesticides have a slightly higher risk of prostate cancer, especially if they have a history of prostate cancer in their family.
- Exposure to cadmium or rubber derivatives in the workplace also increases the risk of prostate cancer.
The prostatitis is sometimes the consequence of a sexual infection ( sexually transmitted disease ). But very often, no triggering factor is found.
In the elderly, prostatitis is frequently the consequence of a urinary infection, itself secondary to an enlarged prostate which promotes urinary stasis. We then speak of adenomitis
- presence of blood in the urine (hematuria) or semen
- burning sensation or pain during urination
- difficult or painful ejaculation
- urethral discharge
- pain or discomfort in the genitals, groin, lower abdomen, or lower back
- pain or feeling of pressure in the rectum
- need to urinate often (frequent urination)
- very urgent need to urinate (urgent urination)
- reduced urine stream
- difficulty urinating
- fever, chills, and muscle pain
- recurrent urinary tract infections
- sexual problems and loss of libido
.
More precisely:
- Fever over 38.5, chills, severe fatigue ;
- The patient complains of burning while urinating, of having difficulty urinating ( dysuria ), of urinating too often (pollakiuria);
- Sometimes there is a purulent discharge from the urinary meatus;
- Presence of blood in urine or semen;
- The urine may be cloudy and smelly.
Acute prostatitis can present with flu-like signs :
- Diffuse muscle pain, joint pain …;
- Rarely, a sensation of a foreign body in the anus is associated.
Still talking about this disease chronic prostatitis is characterized by chronic perineal pain, sometimes in the anal area. Voiding burns can evolve for several years.
Most often, prostate cancer does not have any symptoms; it is said to be "silent". It will be discovered by chance, following a blood test or during a routine prostate exam. In this case, the doctor will have performed a digital rectal examination, noted induration, and he will have sounded the alarm. This hardening is the most frequent clinical sign.
Similar symptoms when the urethra is compressed
Symptoms start to appear when the tumor grows and puts pressure on the urethra or when it is advanced. The symptoms are the same as for benign prostatic hypertrophy (BPH), because as we age the prostate increases in size and compresses the urethra. Prostatitis can also cause symptoms similar to prostate cancer. On the other hand, as mentioned earlier, the majority of patients with prostate cancer will have no clinical symptoms.
After the age of 40, it is important that people make sure not to confuse BPH, prostatitis and prostate cancer. The examination by a doctor therefore becomes more than important to be clear about it.
BPH or large prostate
The most common signs and symptoms
In the early stages of BPH, there are no signs and symptoms. These appear when the enlarged prostate puts pressure on the urethra and bladder. This can reduce the diameter of the urethra (compress it) or irritate the bladder, which can cause changes in urinary habits and difficulty passing urine. In some patients, symptoms may appear with minimal enlargement of the prostate.
BPH can cause the following symptoms:
- A need to urinate often day and night (frequent urination)
- An urgent need to urinate (urgent urination)
- Difficulty starting or stopping urinating
- A weak or slow urine stream
- A stream of urine that stops
- A feeling of not emptying your bladder
- Difficulty controlling your bladder (urine leakage)
- Pain or burning sensation when urinating
- Difficult or painful ejaculation
- Presence of blood in urine or semen (rare)
Prostatitis or inflammation of the prostate
The most common signs and symptoms
Prostatitis can cause a wide range of symptoms that vary from one man to another. They can be similar to those caused by benign prostatic hyperplasia (BPH) and prostate cancer. On the other hand, it is distinguished by the presence of pain in the pelvic region and so acute, by high fever and chills.
Prostatitis can be caused by an acute urinary tract infection (bacterial prostatitis) or by chronic inflammation / chronic tenderness.
Prostatitis can cause the following symptoms:
- A need to urinate often day and night (frequent urination)
- An urgent need to urinate (urgent urination)
- Difficulty starting or stopping urinating
- A weak or slow urine stream
- A stream of urine that stops
- A feeling of not emptying your bladder
- Pain or burning sensation when urinating
- Pain in the pelvis area (genitals, groin, lower abdomen or lower back)
- Difficult or painful ejaculation
- Fever and chills if the prostatitis is acute
- Recurrent urinary tract infections
- Presence of blood in urine or semen (rare)
BPH and prostatitis do not equate to prostate cancer. They are among the most common diseases related to the prostate.
Localized cancer
Signs and symptoms of localized cancer
The most common signs and symptoms
It is common for prostate cancer in its very early stages to not cause any symptoms due to its generally slow development. Symptoms can appear if the tumor grows and compresses your urethra - causing changes in your urinary habits or other problems - or if your cancer is advanced. The tumor does not usually cause pain in the prostate itself.
As mentioned above, it should be remembered that all of these symptoms are usually caused by benign enlargement of the prostate that occurs with age and not by prostate cancer. They can also be caused by other problems related to the urinary tract, including bacterial or infectious prostatitis, among others.
Cancer can cause the following symptoms (most often there are no symptoms ):
- A need to urinate often day and night (frequent urination)
- An urgent need to urinate (urgent urination)
- Difficulty starting or stopping urinating
- A weak or slow urine stream
- A stream of urine that stops
- A feeling of not emptying your bladder
- Difficulty controlling your bladder (urine leakage)
- Pain or burning sensation when urinating
- Difficult or painful ejaculation
- Presence of blood in urine or semen (rare)
Signs and symptoms of advanced cancer
Signs and symptoms when it spreads outside the prostate
Cancer that started in the prostate then spreads to the pelvic nodes (these are not the same nodes as those in the groin, which are noticeable: the pelvic nodes are found deep in the belly, near the prostate; do not see them and we do not feel them). This is called lymph node metastasis. These lymph node metastases do not cause pain, but can occasionally cause edema (swelling) of the feet and ankles (see why below).
In the even more advanced stage of the disease, cancer cells have usually migrated to the bones, especially those of the pelvis and spine (these are bone metastases).
If the metastases are large enough, then the following symptoms may appear:
- Pain in the lower back or hips
- Numbness or paralysis of the lower extremities (in the spine, metastases can compress the spinal cord)
- Edema (swelling) of the feet and ankles (lymph node metastases can cause poor lymphatic drainage in the lower limbs)
- Weight loss and impairment of general condition (we do not feel well)
- Constant fatigue and pallor (bone metastases can cause anemia)
To contact our experts please call or write to us on the following number, tel / WhatsApp
: +229 51374202
ALL ABOUT SPERMATOZOIDS: Bark, Roots, Herbal Teas, Plants
ALL ABOUT SPERMATOZOIDS: Bark, Roots, Herbal Teas, Plants
A spermatozoon is a mobile male reproductive cell (or gamete) involved in sexual reproduction. During fertilization, the sperm unites with an egg or an oocyte (female gamete) to form an egg cell, which will then develop into an embryo to give a new individual. This is how the Dawasanté experts provide you with a natural treatment to treat your problems with sperm abnormalities (oligospermia, necrospermia, asthenospermia, teratospermia, azoospermia, etc.).
Click on the image below to discover this natural treatment
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
The possible link between male infertility and chromosomal abnormalities in spermatozoa has been explored in several studies, since the advent of the technique of fluorescence in situ hybridization (FISH).
INTRODUCTION
Chromosomal abnormalities in humans may be responsible for infertility. In fact, the prevalence of abnormalities detected in the blood karyotype is ten times higher in infertile men than in the general population, ie around 5.3%, versus 0.6%. Numerical and structural abnormalities of the sex chromosomes are found with a high frequency, especially in men with severe azoospermia or oligo-astheno-teratospermia (OAT). The treatment of choice to remedy male infertility with OAT is Medically Assisted Reproduction (PMA) by Intra Cytoplasmic Sperm Injection (ICSI). However, it has been reported in recent years that the rate
of aneuploidy (abnormal number of chromosomes) of the sex chromosomes and de novo structural chromosomal abnormalities of paternal origin is higher in the offspring of these men. The risk of transmission of a chromosomal abnormality to offspring as the natural process of sperm selection is bypassed by the ICSI procedure should therefore be carefully considered and evaluated.
SPERMATOZOID CARYOTYPE AND FISH
Karyotypic analysis of spermatozoa makes it possible to determine in what proportion the gametes themselves are carriers of chromosomal abnormalities, in particular in infertile men.
In 1978, Rudak et al. described a technique for the karyotypic analysis of spermatozoa, based on the in vitro penetration of the latter into hamster oocytes. This technically heavy and delicate technique was only successfully practiced by a dozen laboratories around the world.
The technique of FISH (Fluorescence In Situ Hybridization) and its developments now make it possible to perform the chromosomal study of spermatozoa and analyze a large number of cells, using chromosome-specific probes that hybridize to particular regions of the DNA and can then be detected visually using a fluorescence microscope. For the FISH study, sperm from an ejaculate is spread on slides and undergo a chemical treatment resulting in the decondensation of their heads, while maintaining the structure that distinguishes them from other cells that may be in the ejaculate. Spermatozoa are also distinguished by the fact that they present signals corresponding to haploid and non-diploid cells. intact with clear hybridization signals are counted
MORPHOLOGICALLY NORMAL SPERMATOZOIDS
Morphology and motility are currently the parameters used to identify the sperm that will be microinjected as part of an ICSI procedure. Spermatozoa with an abnormal morphology are also more likely to present aneuploidy, but this risk has not been clearly quantified.
Ryu et al. studied the frequency of aneuploidy in sperm of normal morphology in infertile patients who are candidates for ICSI and all carriers of a normal blood karyotype compared to fertile patients. The morphology criterion used was that of Kruger. FISH analysis of chromosomes 18, X and Y were performed. In the group of infertile patients, and aneuploidy rate was found varying from 1.8% to 5.5% compared to 0% to 2.6% in the control patients. This result shows that the morphology of the spermatozoa is not an absolute criterion for the selection of a genetically normal spermatozoon.
Note that the different reported figures of sperm aneuploidy in men without fertility problems vary between 0 and 5% depending on the studies, differences which may be due to the use of probes with variable hybridization efficiency or to the visual interpretation of signals.
CHROMOSOMIC ANOMALIES, SPERMOGRAM AND LIFESTYLE
In a recent review, the sperm karyotypes of men without spermogram abnormalities were analyzed, with the aim of looking for possible correlations with age and lifestyle. The results of some fifty studies combining data from sperm analysis by FISH from 500 men (more than 5 million spermatozoa) were compiled. The results are an average reported rate of abnormality of 0.15% for each chromosome and 0.26% for sex chromosomes. The majority of chromosomes had an even distribution of abnormalities, with the exception of chromosomes 21, 22 and sex in which the frequencies of abnormalities were significantly higher. Trisomies 21 and 22 are also the most frequently found in the products of spontaneous miscarriages, showing the link between chromosomal abnormalities in spermatozoa and abnormalities found in the embryo. This work also demonstrated a slight increase in the frequency of disomies with paternal age, mainly for the sex chromosomes, but no effect of smoking, alcohol and caffeine consumption.
INFERTILITY AND KYOTYPES OF SPERMATOZOIDS
It is reported that 23% of men with azoospermia and 5-10% of men with OAT have an abnormal blood karyotype, resulting in a high likelihood of producing aneuploid gametes. It is known, for example, that the proportion of gametes with a chromosomal imbalance can be as high as 50% in men carrying a reciprocal translocation. However, a normal blood karyotype does not exclude the production of aneuploid gametes. An abnormal intra-testicular environment can affect spermatogenesis, in particular by disrupting the mechanisms controlling chromosome segregation during cell division.
A defect in spermatogenesis can have many origins such as systemic disease, malnutrition, endocrine disorders, obstructive pathologies and genetic defects. Indeed, a large number of severe OATs and azoospermia have genetic etiologies, including microdeletions at the level of the Y chromosome, abnormalities of meiosis, and mutations in the cystic fibrosis gene. However, “idiopathic” OAT remains the diagnosis most often retained in male infertility, despite extensive investigations to try to determine its origin. The main interest in identifying an etiology with OAT lies in the evaluation of the prognosis and the risk of producing embryos with chromosomal abnormalities.
A large study is now the source of much controversy over the relationship between spermogram abnormalities and potential risks of chromosomal abnormalities in ICSI. Fertilization and pregnancy rates obtained in relation to parameters of sperm number, mobility and morphology of infertile men were retrospectively analyzed in 966 cycles of ART with ICSI. The results showed comparable ICSI successes independent of the magnitude of OAT parameters. They concluded that in the extreme, only a living sperm in ejaculate can be sufficient for ICSI to be successful. While this study was therefore very reassuring, it does not
In order to study the etiology of “unlabelled” OATs, Calogero et al. used the FISH technique to explore the rate of aneuploidy in sperm chromosomes 8, 12, 18, X and Y in one group of patients with teratospermia, another with OAT and a control group. They observed similarly increased rates of aneuploidy in the first two groups, which suggested that teratospermia may be the critical endpoint associated with aneuploidy. The authors, therefore, recommended that a FISH analysis be performed in cases of teratospermia, before any attempt at ICSI. These same authors performed another study to try to relate the rate of sperm aneuploidy in eighteen men with OAT and the results of ICSI in affected couples. For these cases of OAT, and overall fertilization rate of 95% and a pregnancy of 39% was obtained. Very curiously, this pregnancy rate was significantly higher than reported by multiple centers practicing the ICSI technique (the generally accepted average rate is around 25%), which the authors of the article do not discuss. The rate of oocyte fertilization by ICSI was independent of the rate of aneuploidy. On the other hand, the patients who had not had a pregnancy (91%) had significantly higher aneuploidy rates than those of the controls.
Bernardini et al. also analyzed by FISH the rate of aneuploidy of the spermatozoa for chromosomes 1, 17, X, and Y, on a series of twenty-two cases of infertile men compared to fertile controls. A significantly higher rate of aneuploidy was found in men with OAT (18%) compared to controls (2.28%).
In the case of azoospermia patients, it is now sometimes possible to perform ICSI after a testicular biopsy in which sperm is found. The reported numbers of chromosomal abnormalities are impressive: indeed, one study estimated the proportion of chromosomal abnormalities at 19.6% in a group of patients with non-obstructive azoospermia and 8.2% in those with obstructive azoospermia. Here again, the link between gonadal insufficiency and the presence of chromosomal aneuploidies is well demonstrated.
It can be concluded from these data that a high rate of aneuploidy in spermatozoa is associated with a low rate of pregnancy and therefore less success through assisted reproduction by ICSI. However, the rate of fertilization of the oocytes does not seem to depend on the rate of aneuploidy, which means that the transferred embryos are more often carriers of aneuploidies and that on the other hand, their implantation would be disadvantaged. In this context, genetic counseling following a FISH analysis of the sperm would be highly desirable, before a couple begins a long and difficult procedure of assisted reproduction by ICSI.
SPERMATOZOID ANEUPLOIDS AND GENE FACTORS
A particularly important point of these studies is that they make it possible to explain certain male infertilities so far called “idiopathic”. In fact, disturbances of meiosis or premeiotic mitosis during spermatogenesis could predispose to the non-chromosomal disjunctions that are observed. The next step would consist in identifying which are the genetic factors at the origin of these disorders of meiosis and mitosis and to characterize them to have one more diagnostic means available in idiopathic male infertility. If gene abnormalities predisposing to non-disjunctions were detected, this diagnostic tool would be available and the possible transmission in the offspring of this pathology would be evaluable. And then supported by numerous studies. We now know that at least thirty genes are involved in the control of meiotic and mitotic divisions. For example, the role of HspA2, a “chaperone” protein with a specific testicular expression that is thought to be involved in the synaptonemal complex has recently been demonstrated. The role of genes of the MAD (Mitotic Arrest Deficiency) family involved in premeiotic mitotic control is also discussed.
There is a case, recently reported in the literature, where FISH analysis of spermatozoa made it possible to pose a contraindication to ART. In the study in question patients with different types of absolute teratospermia (100%) were studied. One of them had a sperm morphological abnormality consisting of macrocephaly and multiple flagella. In this patient, 90% of the sperm analyzed by FISH presented aneuploidy. This result was considered to be a contraindication to ICSI.
FEASIBILITY
In these various studies, between 3000 and 10,000 sperm per patient are analyzed. This represents a significant investment of time, considering that for FISH analysis on amniocytes, there are routinely between 50 and 100 cells. It is estimated that to detect significant levels of aneuploidy in sperm, an analysis of around 1000 cells may be sufficient. The method of collection is no different from that for a spermogram, and only a small fraction of ejaculate is used to smear onto slides for chemical treatment of the sample prior to FISH.
CONCLUSION
While the use of FISH on spermatozoa in male infertility appears undoubtedly valuable and contributory in the context of a pre-ART workup, or after repeated ART failures, the formal indications for this analysis have not yet been clearly established. established. One of the first uses of this approach could be to give couples undergoing a pre-ICSI procedure for OAT or azoospermia a more detailed indication of the chances of success and risks of miscarriages due to chromosomal abnormalities potentially present in the sperm. This information should then be communicated to patients within the framework of genetic counseling, taking into account the psychological repercussions of a possible poor prognosis of success.
Some authors also consider that this technique can be used in the event of miscarriages with repetitions of undetermined etiology beyond the framework of male infertility. Indeed, if 60% of the miscarriages of the first trimester are due to chromosomal abnormalities and a majority are of maternal origin, the FISH technique on the spermatozoa has shown a paternal origin in 8 to 12% of cases, corresponding to a greater incidence of chromosomal abnormalities in their gametes.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
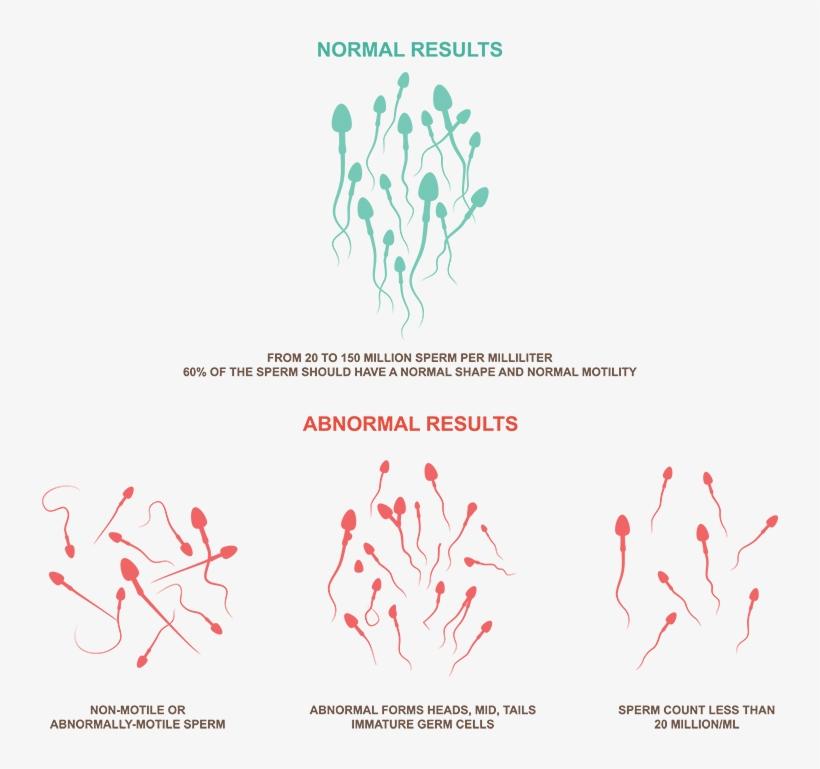
TYPES OF TERATOSPERMIA: mild, moderate, and severe
The teratospermia (or teratozoospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. This is how the Dawasanté experts provide you with a natural treatment to treat all your fertility problems related to the quality and quantity of your sperm.
Click HERE or on the image below to discover this natural treatment
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Teratozoospermia or teratospermia is a seminal alteration that involves a high percentage of abnormally shaped sperm.
It is a cause of male infertility, the severity of which will depend on the greater or lesser number of amorphous sperm cells in the semen.
According to the different criteria used to assess the degree of teratozoospermia, we can distinguish 3 types: mild, moderate, or severe.
1-Classification of teratozoospermia
When a man performs a spermogram to assess the quality of his sperm, in the results report, he will obtain the values of all seminal parameters, including sperm morphology.
A man is considered to have teratozoospermia when the percentage of sperm with normal morphology in his seminogram is less than 4%, according to criteria established by the World Health Organization (WHO) in 2010.
On the other hand, some labs also use Kruger's strict criteria to diagnose teratozoospermia. According to Kruger, a man suffers from teratozoospermia when less than 15% of his sperm has a normal form.
Percentage of normal sperm
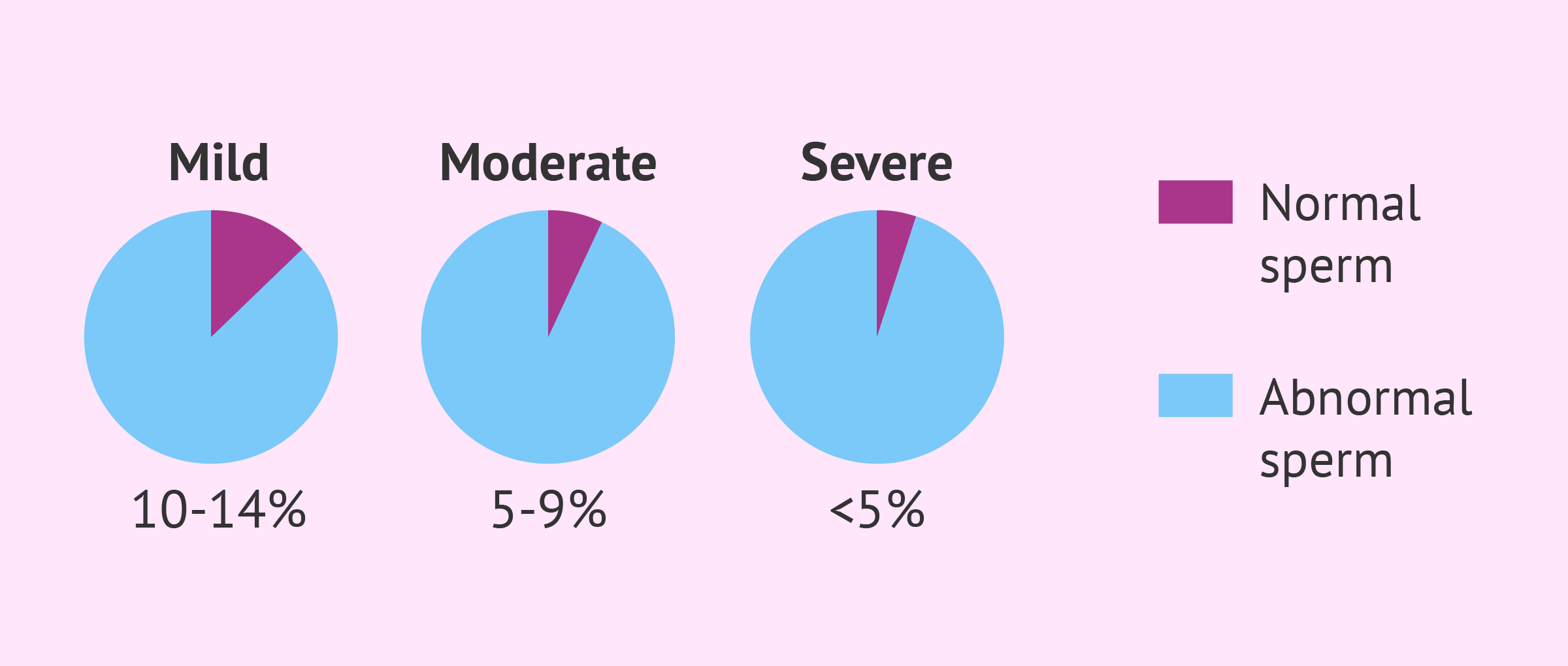
Since the WHO benchmark is so low, there is no point in talking about types of teratozoospermia based on the number of normal sperm. Therefore, for the classification of spermatozoa in this sense, it is better to use Kruger's criterion, which is stricter than the previous one.
1-1 Mild teratozoospermia
A man suffers from mild teratozoospermia when the number of normal sperm in his spermogram ranges from 14% to 10%.
The rest of the sperm will have an abnormality in their head, neck or tail. Despite this, men with mild teratospermia do not have a bad prognosis for having children.
If assisted reproduction techniques are necessary to achieve pregnancy, artificial insemination (AI) and in vitro fertilization ( IVF ) may be performed, depending on the concentration and mobility of the sperm.
The shape of the sperm is important for the fertilization of the egg. However, men with mild teratozoospermia can achieve a natural pregnancy.
In addition, there are various dietary supplements that contain vitamins and antioxidants that help in the maturation of sperm and can improve their morphology.
If you are interested in this topic, you can read the following article: Treatment of teratozoospermia.
1-2 Moderate teratozoospermia
Moderate or severe teratozoospermia is diagnosed when sperm results show that only 9-5% of sperm have a normal shape.
With this diagnosis, it is quite complicated to have children naturally. To achieve a pregnancy with moderate teratozoospermia, an in vitro fertilization technique such as ICSI will most likely be necessary.
The ICSI (Intracytoplasmic Sperm Injection) is based on the selection of spermatozoa under a microscope and their direct injection into each egg and fertilization.
PMA, like any medical treatment, requires that you trust the professionalism of the doctors and clinic you have chosen. Obviously, not all are the same. The Fertility Report selects the most advantageous clinics for you based on our rigorous quality criteria. In addition, the system performs a comparison of prices and conditions offered by different clinics to facilitate your decision making.
1-3 Severe teratozoospermia
When the spermogram morphology test shows a normal sperm value of less than 5%, the man has severe or severe teratozoospermia.
Sperm with good morphology is therefore very few in number and, therefore, the possibility of achieving natural pregnancy is very low.
Spermatozoa with alterations in their morphology have problems progressing gradually, they have more difficulty reaching the egg, penetrating its thick pellucid layer and also fusing its male nucleus with the female one. The consequence of all this is that they can lead to fertilization failures.
Teratozoospermia and fertilization failure

The most suitable assisted reproduction technique for extreme teratozoospermia is ICSI or its improved variant: IMSI.
The IMSI is the same as intracytoplasmic sperm injection, but with the use of a microscope magnification of 6300, so it is possible to get very close to the sperm morphology and make a better selection.
2-Your frequently asked questions
2-1 Can we cure severe teratozoospermia?
If a man has less than 5% of sperm with normal morphology, it is very difficult to regain a normal value with natural or pharmacological treatment. Improvement can be seen over time, especially if the man maintains a healthy lifestyle.
On the other hand, if the teratozoospermia appears associated with another pathology such as, for example, varicocele, it is possible that the spermogram improves its parameters during a surgical intervention to eliminate the varicocele.
2-2 What is isolated teratozoospermia?
Discrete teratozoospermia means that the affected parameter, in this case, the morphology of the sperm, does not have a value much lower than the reference value. Therefore, it would be a mild teratozoospermia.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
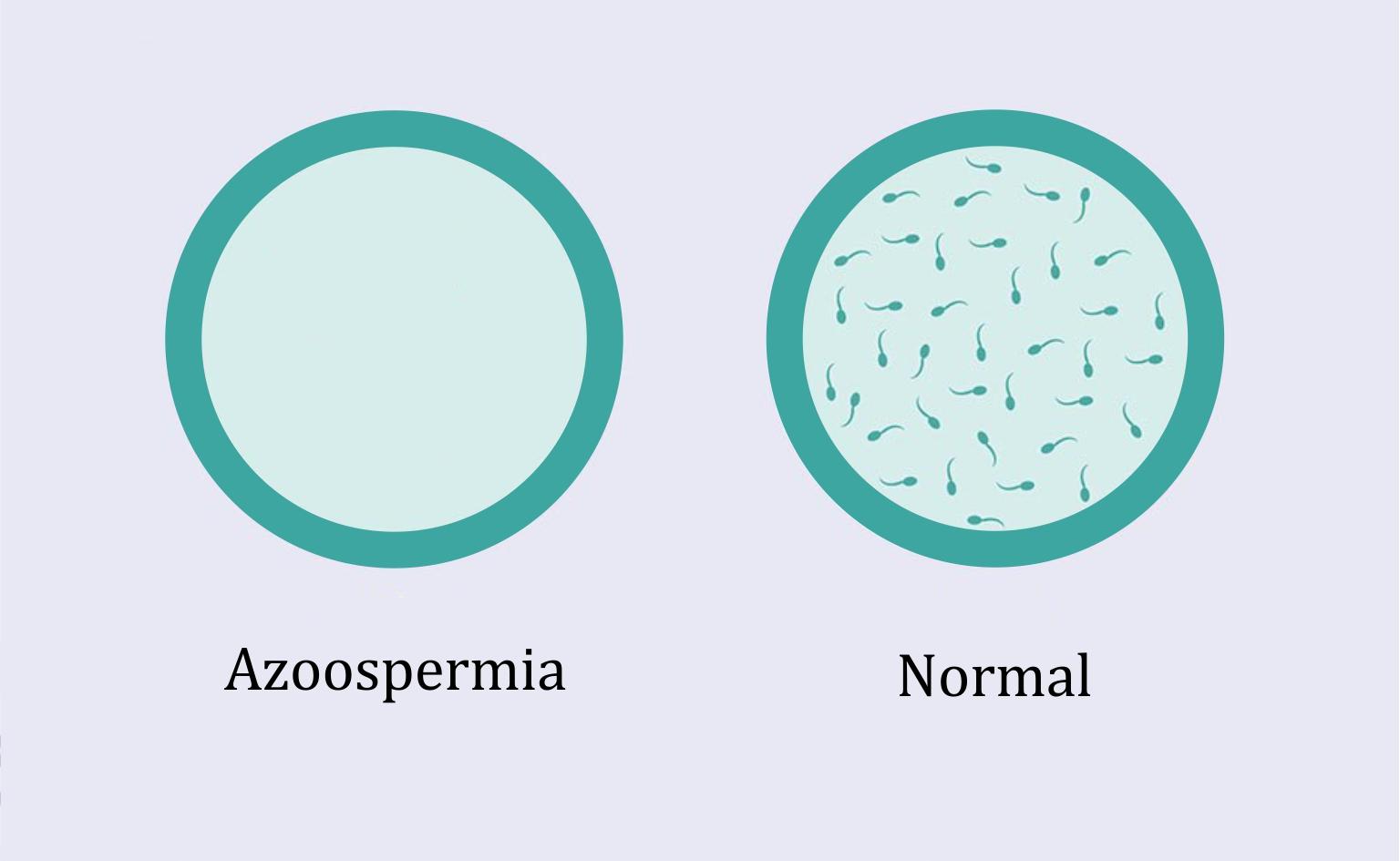
AZOOSPERMIA AND PREGNANCY: Natural treatment
Natural pregnancy in a woman whose partner has secretory or obstructive azoospermia is not possible. However, when the treatments applied do not solve the problem, Dawasanté experts offer you a natural herbal treatment to cure your azoospermia and allow your partner to quickly get pregnant.
Click here or on the image below to discover this natural treatment .
To discover our natural solution to treat azoospermia click here!
Contact our experts, tel / WhatsApp: +22990312738
1: Aspiration of sperm
In men with obstructive azoospermia , no sperm is seen in the ejaculate, but sperm is produced in the testis.
One option is to extract the sperm directly from the testis or epididymis. In this way, it is possible to obtain sperm, but in low quantity and of poor quality in relation to mobility and morphology.
For this reason, in the event of obtaining sperm by aspiration, it will be necessary to resort to the technique of ICSI (intracytoplasmic sperm micro-injection). ICSI is the ideal in vitro fertilization technique because only one sperm is needed for each egg to be fertilized. In addition, in this process, it is the specialist himself who introduces the sperm into the egg.
There are several procedures for extracting sperm, and their names come from the acronyms in English:
1.1: MESA
Corresponds to the term: microsurgical epididymal sperm aspiration , i.e., microsurgical aspiration of epididymal sperm. It is used in patients with obstruction of the genital tract. This involves making a small incision in the epididymis and extracting the sperm from inside the epididymis.
It is a complicated operation and the costs are high. For this reason, although it allows to collect more sperm than with a PESA, it is not the most chosen technique.
1.1.1: PESA
It is the percutaneous aspiration of epididymal sperm ( percutaneous epididymal sperm aspiration ). This is a simpler and less invasive procedure than the previous one and does not require as many skills on the part of the doctor. It is performed under sedation, so that the patient does not feel any pain.
A needle is inserted through the skin of the scrotum to reach the epididymis. The downside is that the needle is inserted blind, and although this is unusual, it is possible that no sperm will be aspirated.
1.1.2: TESA
Its English name is: testicular sperm aspiration , and it is referred to as the aspiration of sperm from the testis. It is also performed percutaneously, just like PESA. The difference is that the aspiration is done from the testes and not from the epididymis.
This type of aspiration is usually performed when the other options (MESA and PESA) are not applicable due to changes such as absence or obstruction of the epididymis.
2: Testicular biopsy
Also known as TESE ( testicular sperm extraction ). It is performed under local anesthesia and consists of the following elements:
- The specialist opens the different testicular layers using a scalpel or a laser until it reaches the testicle, from which he will extract small pieces. About 2-3 cm of testicular layers are opened. They will then be closed with one or two stitches.
- After the biopsy is performed or at the same time as the biopsy, the tissues are analyzed under a microscope for sperm, which will then be used in the ICSI technique in the hope of pregnancy.
- Although it is indicated in patients with obstructive azoospermia , it is also applied in certain situations of secretory azoospermia. In many of these cases, although no sperm is produced in the testes, foci of spermatogenesis can be found, that is, if you search exhaustively, it is possible to find a sperm.
- In any case, the possibility of achieving pregnancy by applying ICSI with the few sperm found after testicular biopsy of patients with secretory azoospermia is low.
3: Sperm donation
The above procedures may be effective for obstructive azoospermia , but they are not usually applied to secretory azoospermia. In patients with this alteration, where no treatment is able to reverse spermatogenesis, it is recommended to resort to sperm donation .
This is artificial insemination or in vitro fertilization with sperm donated by a healthy young man . This donor is subjected to a series of physical and psychological examinations to verify his good state of health and to confirm the safety of the use of his sperm.
The choice of one or the other reproductive technique will depend on certain qualities of the woman such as her age, the patency of the fallopian tubes, etc.
This is an alternative with a high probability of success . However, it has a major drawback: humans give up transmitting their genetic heritage. This means that the children born will not be the biological children of their father, since they will inherit the traits of the donor who gave the sperm.
4: Your frequently asked questions
If my husband has total azoospermia, should we consider donating sperm as the only option so that I can get pregnant?
If as total azoospermia you hear irreparable secretory azoospermia, yes, sperm donation is the best option for you to achieve pregnancy.
In severe cases of secretory azoospermia, it is very difficult to obtain viable sperm with fertilizing ability, so it is necessary to resort to sperm donation.
After 11 years of vasectomy, will I be able to have children if I have a testicular biopsy?
A testicular biopsy is used to obtain sperm directly from the testis, which is the place of production. However, after so long a time of voluntary obstruction, that is, after preventing the produced sperm from coming out, it is possible that the organism itself has reduced production. However, since only one sperm per egg is needed for ICSI treatment, you may be able to achieve pregnancy in your partner from the sperm found during the biopsy.
In any case, you should be aware that it is quite possible that no viable sperm will be found after the biopsy.
Pregnancy was detected by measuring serum HCG on two independent occasions, at least 15 days after the embryo replacement. Clinical pregnancy was determined by observing a gestational sac with a fetal heartbeat on a transvaginal ultrasound at 6–7 weeks gestation. The clinical embryo implantation rate was defined as the number of gestational sacs seen during ultrasound screening at 6-7 weeks gestation divided by the number of embryos transferred.
To discover our natural solution to treat azoospermia click here!
Contact our experts, tel / WhatsApp: +22990312738
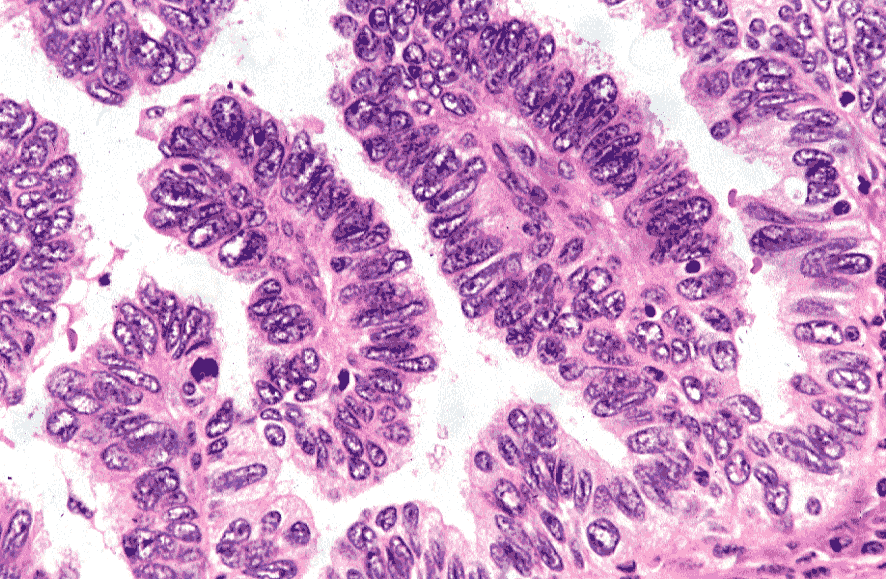
CAUSES OF VERGE ADENOCARCINOMA: NATURAL TREATMENT
CAUSES ADENOCARCINOMA THE VERGE: NATURAL TREATMENT
The adenocarcinoma verge or penile cancer is a disease in which malignant (cancer) cells form in the tissues of the penis.
Adenocarcinoma of the penis or cancer of the penis is usually found on the glans or foreskin of the penis, but can also occur on the shaft of the penis. Almost all penile cancers start in the skin of the penis.
The cancer of the penis or the penis is rare cancer in France.
But before going any further in our writing, and in case you are concerned by this condition and want to avoid surgery at all costs, the health experts at DAWABIO after much research offer you a very effective solution based on herbal remedies for adenocarcinoma of the penis or cancer of the penis. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Different types of cancer
Penile cancer can develop at the expense of the skin or the internal tissues of the penis: it is called squamous cell carcinoma.
More rarely, it can be low cell carcinoma, melanoma.
Causes of adenocarcinoma of the penis
Certain factors predispose to the development of penile cancer or adenocarcinoma of the penis :
The lack of hygiene, aggravated by the existence of phimosis (affection of the penis) preventing any removal of coring, increases the risk of penile cancer. "Indeed, microbial development can lead to inflammation involved in the development of cancer, explains Dr. Ludovic Ferretti, member of the committee of andrology and sexual medicine of the French Association of Urology. Thus, we recommend a classic cleaning to water and soap after scalping (without forcing), then drying. And after urinating, wipe the glans well so as not to let acid urine infiltrate under the foreskin, which would promote inflammation.
· Phimosis (phimosis corresponds to a narrowing of the tip of the foreskin which prevents pull the foreskin);
· Dermatological disease of the glans or the foreskin which can become secondarily cancerous, like a mole for example;
The causes and risk factors of developing penile cancer include the infection with the human papillomavirus ( HPV )
The use of regular hygiene care, with systematic removal of the cores, remains the best prevention.
The dupenis cancer or carcinoma of the penis is a disease in which malignant (cancer) cells form in the tissues of the penis.
The penis is a rod-shaped male reproductive organ that transmits semen and urine from the body. It contains two types of erectile tissue (spongy tissue with blood vessels that fill with blood to make an erection):
Corpora cavernosa: The two columns of erectile tissue that make up most of the penis.
Corpus spongiosum: The single column of erectile tissue that forms a small part of the penis. The spongy body surrounds the urethra (the tube through which urine and sperm pass from the body).
Erectile tissue is wrapped in connective tissue and covered with skin. The glans (head of the penis) is covered with loose skin called the foreskin.
Infection with human papillomavirus can increase the risk of developing penile cancer.
Anything that increases your chances of getting a disease is called a risk factor. Having a risk factor doesn't mean you'll get cancer; not having risk factors doesn't mean you won't get cancer. Talk to your doctor if you think you are at risk. The risk factors for penile cancer or adenocarcinoma of the penis are as follows:
Circumcision can help prevent infection with the human papillomavirus ( HPV ). A circumcision is an operation in which the doctor removes part or all of the foreskin from the penis. Many boys are circumcised soon after birth. Men who were not circumcised at birth may have a higher risk of developing penile cancer.
The other risk factors for penile cancer are:
Be 60 years of age or older.
Have phimosis (a condition in which the foreskin of the penis cannot be pulled over the glans).
Have poor personal hygiene.
Having many sexual partners.
Use of tobacco products.
Symptoms
Changes in the skin of the penis are the most common symptom of penile cancer. They can appear on the foreskin of uncircumcised men, or on the tip of the penis (the glans) or the shaft.
Warning signs of the disease may include:
- Changes in skin thickness or color on the penis
- A bump on it
- A rash or small “crusty” bumps on it; it may look like an unhealed scab.
- Growths on the penis that appear bluish-brown
- A smelly discharge under the foreskin
- A sore on the penis, which may bleed
- Swelling at the tip of the penis
- Lumps under the skin in the groin area
Most men with these symptoms do not have penile cancer. Rather, it is an infection or an allergic reaction. Nonetheless, it's important to check for any unusual symptoms on or near your penis immediately. Early treatment is preferable.
Men at risk
There is convincing evidence that there are certain factors that increase the risk of penile cancer. Among them :
Chronic inflammation of the penis due to poor genital hygiene;
Human papillomavirus ( HPV ) infection ;
A narrowing of the foreskin, also called phimosis: this condition prevents the foreskin from retracting to reveal the glans, which makes genital hygiene more difficult and may mask a skin lesion;
· Smoking;
Precancerous lesions such as Queyrat erythroplakia or Bowen's disease.
Signs of penile cancer include sores, discharge, and bleeding.
These signs and others can be caused by penile cancer or adenocarcinoma of the penis or by other conditions. Check with your doctor if you have any of the following:
Redness, irritation or sore on the penis.
A lump on the penis.
Penile cancer and circumcision
In contrast, a circumcision performed in childhood provides some protection against cancer of the penis. HPV vaccination can also decrease the risk of developing the disease.
Usually, follow-up visits are first semiannual and then decrease in frequency over time. The duration of follow-up is in all cases a minimum of 5 years because 90% of recurrences are in the first 5 years, 75% of which are in the first 2 years.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
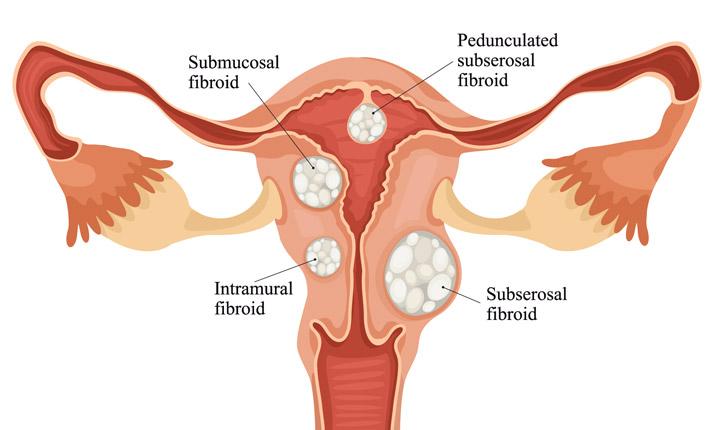
7 natural remedies to get rid of cysts and fibroids in an easy way
|
Many women are most often faced with serious situations of fibroids and uterine cysts, especially during the pregnancy years. Usually, these conditions do not cause discomfort, although, for some women, hormonal fluctuations can cause pain and swelling. The fibroids, also called myomas, are benign non-cancerous tumors that grow on the uterine wall. The ovarian cysts, including polycystic ovary syndrome, are fluid-filled cysts appear in the ovaries and are quite common. We are going to tell you in this article about the best herbal remedies to treat fibroids and ovarian cysts.
Dawasante's herbal treatment for cysts and fibroidsDawasanté experts provide you with a natural herbal-based treatment to permanently cure cysts and fibroids without operation. Click on the image below to discover this natural treatment. To contact our experts please call or write to us on the following number, tel / WhatsApp WE DELIVER ALL OVER THE WORLD
The Best Herbs For Treating FibroidsIf you have fibroids and are looking for a natural alternative to avoid the operation, you have come to the right place. Here is the best natural remedy in the world to make your fibroids disappear naturally and get pregnant fast. It is composed of several herbal teas made from the best plants in the world to remove all your fibroids, make the pain disappear and expel all waste contained in your uterus. How does it work?Herbal tea works by preventing the action of progesterone on the endometrium (lining of the uterus) and keeping estrogen levels within normal limits. This will have the effect of the permanent disappearance of fibroids and your pain. Thus, the heavy menstrual bleeding will be completely stopped at the end of the treatment. To discover our natural remedy for: -Eliminate fibroids, click here -To get pregnant quickly, click here The best herbal remedies to treat ovarian cystsHere is the best natural remedy in the world to make ovarian cysts go away. This natural remedy is made from the best herbal remedies for treating ovarian cysts. He will heal you and you will avoid the operation. Herbal tea is made up of several herbs that regulate the hormone levels and the size of your cysts. It will help you relieve the pain of the menstrual cycle and regularize your cycle. The herbal tea will also expel waste from your uterus. Usually, except when the diagnosis is too late, our natural treatment will cure ovarian cysts without side effects.
Some other natural remedies |
Ginger
Ginger root is very effective in reducing pain and improving blood circulation. You can make tea by adding fresh ginger roots to a glass of boiling water. Filter the tea and drink it several times a day. Ginger root also helps reduce inflammation in the ovaries and uterus.
Olive oil
One of the natural remedies for fibroids is olive oil. It is known to block estrogen. Olive oil is known to block estrogen. When the estrogen level is within the desired range, there is no risk of bromine. It is obtained by taking a tablespoon of olive oil with a little lemon juice on an empty stomach in the morning. You can also prepare olive tea from the fermentation of olive leaves which help strengthen the immune system.
Epsom Bath Salts
Bathing with Epsom salts will greatly reduce pain and other symptoms associated with ovarian cysts. The content of magnesium sulfate present in Epsom salt acts as a muscle relaxant which in turn soothes pain.
Lemon juice
One of the other natural remedies for treating fibroids is lemon juice. Add two teaspoons of lemon juice and one teaspoon of baking soda to a glass of water. Shake the solution well and drink. To reduce the symptoms of fibroids, drink this solution regularly.
Beetroot
Beetroot contains a compound known as betacyanin that boosts the liver's ability to flush toxins from your system. Plus, the alkaline nature of beets helps balance your body's acidity. This in turn reduces the severity of the symptoms of the ovarian cyst.
Take 1 liter of beet juice
1/2 liter of pure honey
Put all the ingredients in the blender and mix them for a few seconds.
Mode of consumption:
Drink 3 glasses every day
1 glass after breakfast
1 glass after having lunch
1 glass after having dinner
NB: follow this treatment for at least 2 months.
Flaxseed
It helps to balance the percentage of estrogen with progesterone in the body. This will help shrink the cysts. Additionally, flax seeds are high in fiber, which helps the body flush out harmful toxins, cholesterol, and other wastes processed by the liver.
Ingredients:
300 g of vinaigrette leaves
500 g of honey
Preparation method:
chop the leaves of the vinaigrette and add the honey. Leave it there for 2-3 days, until they are thoroughly soaked.
How to use:
It is advisable to consume this first remedy in the morning, on an empty stomach, and you should not eat anything for at least 2 hours. This remedy is extremely helpful in boosting the metabolism and cleansing the body of toxins, which makes it really effective especially during the winter months.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
NABOTH CYST AND INFERTILITY: Natural treatment
NABOTH'S CYSTS FOR INFERTILITY
The Naboth cysts are tiny cysts that form on the surface of your cervix. Your cervix connects your vagina to your uterus. It is sometimes called the cervical canal. Naboth's cysts are filled with mucus which is secreted by the cervical glands. Sometimes the small bumps are called cervical cysts, mucinous retention cysts, or epithelial cysts. Naboth's cysts are quite common. They do not pose a threat to your health and are not a sign of cervical cancer.
If you are looking for a natural treatment to fight Naboth cysts, the experts at Dawasanté have the solution for you. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
NATURAL TREATMENT
The natural treatment that we offer to cure Naboth cysts is essentially made from natural herbal teas. Herbal tea is made up of plants whose active ingredients are able to suppress the symptoms that you feel and allow you to have a total recovery. This is the solution to find a normal life.
To discover our natural remedy to cure Naboth cysts, click here
The causes
The cervix is the tissue that connects the uterus to the vagina. The cervix has two distinct parts lined up in two different types of cells:
- Glandular cells, which line the area of the cervix closest to the uterus
- · Squamous cells, which line the part of the cervix closest to the vagina
Glandular and squamous cells meet to form an area called the transformation zone. This area undergoes many changes over the course of a woman's life, especially during pregnancy and childbirth.
Cells in the transformation zone are constantly changing, making this zone very susceptible to abnormal cell growth.
A number of conditions can cause a lump on the cervix and are described in the following sections.
Cervical polyps
A cervical polyp is a bulb-shaped, non-cancerous growth that develops on the cervix. The appearance, size and color of polyps can vary widely. It is not known why cervical polyps develop, but some of the possible causes of these polyps can include:
- High estrogen levels
- Inflammation of the cervix
- Blocked blood vessels
In most cases, cervical polyps are benign, with only 1 in 1,000 being cancerous. The doctor can remove the cervical polyps in a simple procedure.
Pregnant women can develop small white bumps called Naboth's cysts. They can form when excess skin cells block the mucous glands lining the cervix. Women may not know they have a Nabothian cyst until their doctor finds one during a routine pregnancy check-up. Although Naboth's cysts usually don't cause symptoms, they can rupture and release a foul-smelling discharge or blood.
Cervical fibroids
Fibroids, or myomas, are non-cancerous tumors that usually grow in muscle tissue in the uterus. Although rare, fibroids can also grow in the cervix.
Fibroids can vary in size and some can grow large enough to cause weight gain and swelling of the lower abdomen. Fibroids are almost always benign. Cancerous fibroids are rare and occur in less than 1 in 1,000 cases.
Cervical cancer
A lump on the cervix may indicate cervical cancer. Early Stage Cervical Cancer May Not Cause Symptoms Reliable Source. Cervical cancer can affect one or both types of cells that line the cervix.
Symptoms
Naboth cysts can cause a variety of symptoms if any. They can cause the following symptoms:
- Heavy or painful periods
- Bleeding between periods
- Foul-smelling vaginal discharge
- Pressure or swelling of the lower abdomen
- Frequent need to urinate
- Pain in the lower back, pelvis or legs
- Pain during intercourse
To diagnose the underlying cause of a lump on the cervix, the doctor will collect the following information:
- Family history
- · medical background
- Current drugs
They may also perform a physical exam and other diagnostic tests:
· Ultrasound tests use sound waves to create images of structures inside the abdomen and pelvis.
· MRI scans use a strong magnetic field and radio waves to create detailed images of the tissues inside the body.
· Hysteroscopy can help diagnose conditions affecting the uterus. During the procedure, a healthcare professional will guide a thin tubular device called a hysteroscope through the vagina and uterus. The hysteroscope captures images inside the uterus and transmits them to a computer.
· Laparoscopy uses a camera attached to the end of a thin tube to examine female reproductive organs.
· Biopsies are small samples of tissue from the lining of the cervix. After removal, the doctor will send the sample to a laboratory for analysis. Biopsies can detect the presence of precancerous or cancerous cells.
Complications
Usually, fibroids do not cause serious complications. However, untreated fibroids can increase the risk of infertility and cause problems during pregnancy, such as:
- Placental ablation
- · premature delivery
- · miscarriage
Having fibroids does not increase the risk of developing cancerous fibroids. Naboth's cysts rarely cause serious complications and often go away without treatment.
However, large Naboth cysts can distort the shape of the cervix. These cysts may require excision or surgical removal.
Medical treatments
Benign growths, such as cervical polyps and Naboth's cysts, often do not require treatment.
However, even benign growths can cause problems. Cysts and polyps can grow large enough to distort the shape of the cervix and may require surgical removal or drainage.
Treatment options for bumps on the cervix may include:
Surgery
Here are examples of surgical treatments for bumps on the cervix:
· Polypectomy: this method is to remove a polyp of the cervix with forceps or a string. This procedure usually takes place in an outpatient clinic.
· Electro-coagulation ablation: This method uses the heat of an electric current to remove a cervical cyst.
· Myomectomy: During this procedure, a surgeon will remove the fibroids through a small incision in the lower abdomen.
Medication
Gonadotropin-releasing drugs (GnRH) agonists and antagonists can treat symptomatic cervical fibroids.
GnRH drugs cause the body to make less estrogen and progesterone, which effectively reduces the size of fibroids without harming fertility.
Taking over-the-counter pain relievers, such as ibuprofen and acetaminophen, may help reduce cramps and lower back pain associated with the cervical lump.
Risk factors
It is not known exactly what causes the bumps on the cervix. However, there are certain factors that can increase the risk of developing a lump on the cervix.
Risk factors for cervical lumps include:
- Taking birth control pills containing estrogen
- Having a family history of fibroids, polyps, cysts or cervical cancer
- Inflammation of the cervix due to infections such as HPV, herpes, or yeast infections
- Be overweight or obese
- Having a weakened immune system
Prevention
Maintaining a healthy weight and controlling hormone levels can help reduce the risk of developing a lump on the cervix.
However, leading a healthy lifestyle does not guarantee complete protection against conditions that can cause a lump on the cervix. Participating in routine pelvic exams and Pap smears can help detect cervical abnormalities at an early stage.
The widespread use of regular Pap smears over the past decades has resulted in a significant reduction in the rates of cervical cancer deaths and diagnoses.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.