the secret to curing sickle cell anemia
Blog / 252 results found
Hepatitis B - natural treatments and recommended diets
The hepatitis B virus (HBV) is an infectious disease caused by the hepatitis virus B, transmitted most frequently parenterally (digestive), manifested clinically by various developments, porters, and mild to severe forms with a potential passage in chronic condition. The incubation period of the disease lasts 45 - 120 - 180 days.
What if I have hepatitis?
If you have hepatitis a, b, c, don't panic! Dawabio experts offer you here a very effective natural remedy to destroy the hepatitis virus in a maximum of 2 months. The natural treatment we offer you to cure hepatitis is entirely made up of medicinal plants. Unlike drugs that only fight the symptoms of hepatitis, it completely destroys the virus. It also helps to cleanse the liver. How does it work?
The tea has anti-inflammatory properties and antioxidants, which help in the treatment and prevention of problems hépatiques.C'est so the best remedy natural cure for hepatitis A, B, and C. It also fights against the viruses responsible for hepatitis. It also provides antioxidants that help maintain the overall health of the liver. Simply put, it helps the body fight viral infections and cleanse the liver.
It is the miracle solution to cure hepatitis.
To contact our experts please call or write to us on the following number, tel / WhatsApp: 0022996374527
How does viral hepatitis B manifest?
The disease can have different manifestations from one case to another. There may be people with the virus who have manifestations of the disease and others who are carriers of the virus but who do not have any symptoms.
For the first case (in which there are manifestations), the onset of the disease is slow, with loss of appetite, nausea, vomiting, liver pain, fatigue, headache, general weakness, and joint pain. Less frequently (30 to 40% of cases), a fever that lasts several days, sometimes even longer. During this period, itchy skin may also occur. One of the first signs of the disease is a change in the color of the urine, which turns ash brown like beer. After 1-2 days after finding that the urine has changed color. Jaundice appears (yellowing of the skin and mucous membranes), the stools may turn gray, rashes appear on the skin and the liver increases in size.
In the second case, there is a form of hepatic B virus infection in which carriers of the virus show no signs of illness. These are the so-called “healthy carriers”. To come back to your question, our response is that there is a national hepatitis B treatment program, but that it is strictly for patients with manifestations and not for healthy carriers. In your case, what you need to do is to follow a proper diet as well as careful liver care with liver protection products.
In the following, we will describe in detail the foods that are indicated for liver disease, as well as those that are prohibited. When it comes to the possibility of having children, if their mother is not a carrier of a liver virus, there is a 50% chance that they will be born healthy.
Here are the natural treatments for the symptoms of hepatitis B:
1. A healthy and balanced menu
One of the main factors influencing the course of the virus is the daily menu. It is very important to consume only natural unprocessed foods in an anti-inflammatory diet, it is also helpful to consume foods containing chlorophyll to reduce oxidative stress and harmful effects on the liver.

Eat the following foods as often as possible:
- green leafy vegetables such as spinach, arugula or green salad;
- broccoli, cauliflower and Brussels sprouts;
- carrots, sweet potatoes and beets;
- fresh fruits, in particular blueberries, strawberries and citrus fruits;
- lean meat and fatty fish;
- chicken or beef liver;
- natural sources of probiotics such as yogurt, kefir and cheese;
- basil, parsley, oregano and ginger;
- nuts and seeds, in particular chia seeds, flax and raw nuts;
- coconut oil and extra virgin olive oil.
To reduce nausea, it helps to eat a hearty breakfast, and for lunch and dinner choose light foods. You can also add 1 to 2 drops of peppermint essential oil in a glass of water to quickly eliminate nausea and dizziness.
2. Avoid foods with inflammatory potential

In order to prevent the virus from spreading in the body and making symptoms worse, it is ideal to eliminate foods that promote inflammation. You will need to forgo sugar, hydrogenated oils, refined carbohydrates, and any non-organic dairy products.Do not use semi-processed foods, drink alcohol or use medications that contain acetaminophen. , a substance which may make side effects on the liver worse.
3. Maintains optimal hydration

Vomiting is a common symptom of hepatitis B and promotes dehydration. It is very important to drink enough water throughout the day, both during meals and in the intervals between them.Drink 8-10 glasses of water a day, plus fruit juices or smoothies for an extra dose of vitamins and minerals. Avoid carbonated juices or sports drinks as they are high in sugar and will increase dehydration. Even coffee or tea is only occasionally beneficial. Also try coconut water, which restores the body's electrolyte balance.
4. Reduce stress

To reduce the severity of symptoms, you need to learn to relax and deal with stressful times effectively. Get enough rest, practice yoga, read a book you like, use aromatic oils to freshen the air, or meditate.
Do not be affected by anxiety or worry because you will feel worse if you can relax you will find easier solutions and enjoy special moments with your loved ones. It creates a balance between personal life and career, doesn't get overwhelmed by small events and find something positive in everything that happens to you.
5. Try silymarin

This plant protects the liver and stimulates the elimination of toxins from the body. It acts as an antioxidant, neutralizing the harmful effects of free radicals and reducing oxidative stress. According to studies, silymarin is useful for both acute and chronic hepatitis B.
To contact our experts please call or write to us on the following number, tel / WhatsApp: 0022996374527
WE DELIVER ALL OVER THE WORLD
Did this article answer all of your questions?
Leave us a comment or contact us via WhatsApp at: 0022996374527 for more information
8 complications of Parkinson's disease and natural treatment
Parkinson's disease is a disease that can interfere with people activities because it affects the function of body movements. Some of the main symptoms of Parkinson's disease are tremors, slow body movements, and stiffness in the limbs.
Also, Parkinson's disease can lead to several complications, which you have to know.
Natural alternative to Parkinson's disease
If you have Parkinson's disease, or if you have a loved one who suffers from Parkinson's disease, here is a natural, effective remedy with no side effects that will allow you to cure the disease away of all these heavy chemical drugs. This natural treatment is best for treating Parkinson's disease. It stands out because it is entirely herbal and we take the patient and family as a whole. Trust us! It’s the quick fix to naturally cure Parkinson’s disease.
This herbal tea that we offer, by its antioxidant action, slows the progression of the handicap of people affected by Parkinson's disease. It is made up of plants that are an adequate source of levodopa, the precursor to dopamine, a neurotransmitter that patients with Parkinson's lack. It is an excellent remedy that promotes cognitive improvement, mood, and memory of the patient. This natural treatment also reduces the amount of iron in the brain without causing an iron deficit in order to perform other functions in the body. It’s the perfect natural remedy for Parkinson’s. It will allow the patient to return to normal life.
To discover our natural remedy to cure Parkinson's disease, click here
NB: In the case of Parkinson's disease, In addition to the natural remedy, we also offer psychological support to the patient. You and your family will be in daily contact with a psychologist who will guide and assist you daily.
Parkinson's complications to watch for
The complications of Parkinson's disease are not just physical disorders, such as those related to blood pressure and digestive disorders. Patients with this disease are also at risk of suffering from mental disorders, such as depression. They can also suffer from sleep problems, such as apnea and insomnia.
The following is an explanation of some complications of Parkinson's disease, which should be noted.
- Depression
Mental disorders due to the diagnosis of a chronic illness such as Parkinson's disease are very natural. Besides, chemical changes in the brain can also cause depression. Parkinson's disease can cause depression through changes in the hormone serotonin, which regulates mood.
It is noted that half of the people with Parkinson's disease experience clinical depression at some point in their lives.
- Difficulty speaking and chewing
Talking can be difficult for people with Parkinson's over time. As this disease affects the muscles, the patient's words become difficult to understand. Changes in thinking skills make communication complicated.
As the muscles in the jaw and mouth become weak, the victim has difficulty chewing. Difficulty chewing and swallowing can create a blockage of food in the esophagus and potentially food entering the lungs, which can cause pneumonia.
- Dementia
Parkinson's disease is a disorder that mainly affects the movements of the body. Even so, this disease can also disrupt the part of the brain, which controls thoughts and memories.
In 50 to 80% of people with Parkinson's disease, there is an abnormal build-up of alpha-synuclein proteins in the brain. This protein heap is also found in people with dementia with Lewy bodies.
- Bowel and bladder disorders
The other complications of Parkinson's disease are bowel and bladder disorders. This happens due to interference in the transmission of messages from the brain to the bladder and the intestines.
Bowel and bladder disorders as a complication of Parkinson's disease include frequent urination, bedwetting (while laughing, exercising or sneezing) and poor urine flow. Besides, people with Parkinson's disease can also be affected by diarrhea, constipation, and accidental stool discharge.
- Sleeping troubles
People who suffer from Parkinson's disease also suffer from more pronounced sleep disorders, compared to those of the same age who do not suffer from this disease.
Some sleep disturbances in people with Parkinson's disease are insomnia, nightmares, drowsiness during the day, and difficulty breathing while sleeping (apnea). Talking while sleeping and constantly going to the bathroom can also be felt.
- Blood pressure problems
Parkinson's disease affects the performance of the autonomic nervous system, which is responsible for controlling blood flow and pressure. The system being disrupted, people with Parkinson's disease also experience interference with their blood pressure, both low blood pressure and high blood pressure, such as orthostatic hypertension.
In addition, blood pressure disorders in people with Parkinson's disease can also cause heart problems.
- Sexual dysfunction
Complications of Parkinson's disease can also be sexual. Sexual dysfunction can be characterized by low libido, difficulty reaching orgasm, erectile dysfunction or impotence in men or vaginal dryness in women.
A decrease in arousal and sexual function may occur due to a decrease in the neurotransmitter that is dopamine. Dopamine is a brain chemical, the role of which is to generate pleasure. Male erectile function is controlled by the autonomic nervous system, the job of which is to tell blood vessels to expand when there is excitement to allow an erection. A dysfunction in the process can hamper your ability to get an erection, and such a dysfunction is also common in Parkinson's disease. Another cause is the low testosterone level. You need enough hormones to get good erectile function. And low testosterone levels often occur in Parkinson's patients.
Depression and anxiety disorders can also be a trigger for sexual dysfunction in people with Parkinson's disease.
Olfactory sense
The reduced sensitivity of smell in Parkinson's disease is often overlooked. According to experts, desensitization of smell can occur, due to an accumulation of abnormal proteins, called alpha-synuclein. Protein builds up in the part of the brain that controls the ability of the human smell.
PARKINSON'S DISEASE: DANGEROUS OR NOT
One of the diseases linked to the nerves is Parkinson's disease. This disease is most often seen in the elderly. However, do you know if this disease can strike anyone at any age? Is Parkinson's disease dangerous then? Get that information in my explanations below.
Dawasante's experts have gone to great lengths to find the best treatment for Parkinson's disease.
What you need to know about Parkinson's disease, a neurological disorder
Parkinson's disease is a progressive neurological disorder. In other words, this disease will develop and become more serious over time. Usually, as people with Parkinson's disease age, the rate of Parkinson's disease gets worse.
Parkinson's disease is often considered a dangerous disease. However, this disease is mainly caused by one thing. The cause of Parkinson's disease is an imbalance of chemicals in the brain corresponding to a lower amount of dopamine compared to acetylcholine.
Normally, the amount of dopamine and that of acetylcholine in the brain are the same or balanced. However, in people with Parkinson's disease, the amount of dopamine is less than that of acetylcholine, which causes an imbalance that triggers this disease.
Parkinson's disease is generally characterized by a group of symptoms called TSAP. TSAP means trembling or trembling of the hands, stiffness or stiffness, akinesia or slowing of movement, and postural imbalance or loss of balance.
However, if a person has any of these symptoms, it does not mean that they have Parkinson's disease, which is considered dangerous. The point is that if these symptoms do not appear because of an imbalance, it cannot be called Parkinson's disease.
Natural Treatment
Our herbal remedy is the best herbal medicine recommended by health experts because it has powerful and natural properties to cure various diseases. Dawasante's herbal medicine is made from natural herbal ingredients that are selected and reviewed by health experts. This natural remedy far surpasses conventional drugs as it directly combats the causes of Parkinson's disease. The natural remedy for curing Parkinson's disease that we offer is composed of natural herbal teas. Our herbal tea, by its powerful antioxidant action allows a marked slowdown in the progression of the handicap of patients with Parkinson's disease. It is made up of plants that are an adequate source of levodopa, the precursor of dopamine, which parkinsonian patients lack. It is an excellent remedy that promotes cognitive improvement, mood, and memory of the patient. This natural remedy is the secret to cure Parkinson's disease, thanks to plants. Natural treatment reduces the amount of iron in the brain without causing too much iron deficiency so that to perform other functions in the body. It’s the perfect natural remedy for Parkinson’s. It will allow the patient to return to normal life. In addition, natural herbal teas have no side effects, unlike drugs on the market which can have devastating side effects (hypersexuality, compulsive shopping, perversions etc ...). The value of prescribing these drugs is still controversial, even in the medical community. As they are natural herb-based products, our herbal teas have no side effects, either on the body or on health. Our natural treatment is not dangerous for the patient. To discover this miracle cure, click here.
Parkinson's disease is a dangerous disease
Parkinson's disease is a disease that can reduce the quality of life. This disease is not fatal, but when someone has their quality of life diminished, they cannot do daily activities like people in general.
For example, those who are in good health can button their own clothes. Meanwhile, patients with the disease find it difficult to do so. In fact, buttoning clothes is not a difficult question. Especially compared to other daily activities such as cooking, etc.
Therefore, Parkinson's disease can be considered dangerous because it can develop over time and slowly "eat away" at the lives of those affected. In a sense, this disease will gradually hamper the lives of the sick more and more. People with Parkinson's disease will inevitably experience a decline in quality of life without adequate treatment.
In addition, this dangerous condition can also cause other illnesses, including Parkinson's dementia. When a person suffers from Parkinson's dementia, it is not only their body movements that undergo changes, but it also attacks memory and causes changes in behavior and emotions.
Evolution of the disease
Parkinson's disease is a neurological disease that progressively worsens and affects the part of the brain that works to coordinate body movements. As a result, people with disorders find it difficult to regulate body movements, including speaking, walking, and writing.
As said before, this disease gradually worsens over time, and is divided into 5 stages as described below:
Stage 1: In stage 1, the first unilateral signs appear. The symptoms of Parkinson's disease are mild and do not interfere with the patient's activity. They do not disturb the daily life of the patient.
Stage 2: The duration of the development of Parkinson's disease from stage 1 to stage 2 is different for each patient. It can take place in a few months or years. At this point, symptoms begin to appear. Discomfort begins to be felt by the patient.
Stage 3: Stage 3 of Parkinson's disease is characterized by increasingly apparent symptoms. There are bilateral signs. Body movements begin to slow down and disrupt the activities of those affected. The patient's posture begins to change at this level. There is no real serious handicap and the patient retains full autonomy.
Stage 4: At this stage, people have difficulty standing or walking. Walking is still possible tho. Patients' body movements will slow more and more, their autonomy being limited, they, therefore, need the help of others to support their activities.
Stage 5: Stage 5 Parkinson's disease can prevent people from getting up. Patients may also experience delusions (delusions) and hallucinations. They therefore lose their autonomy.
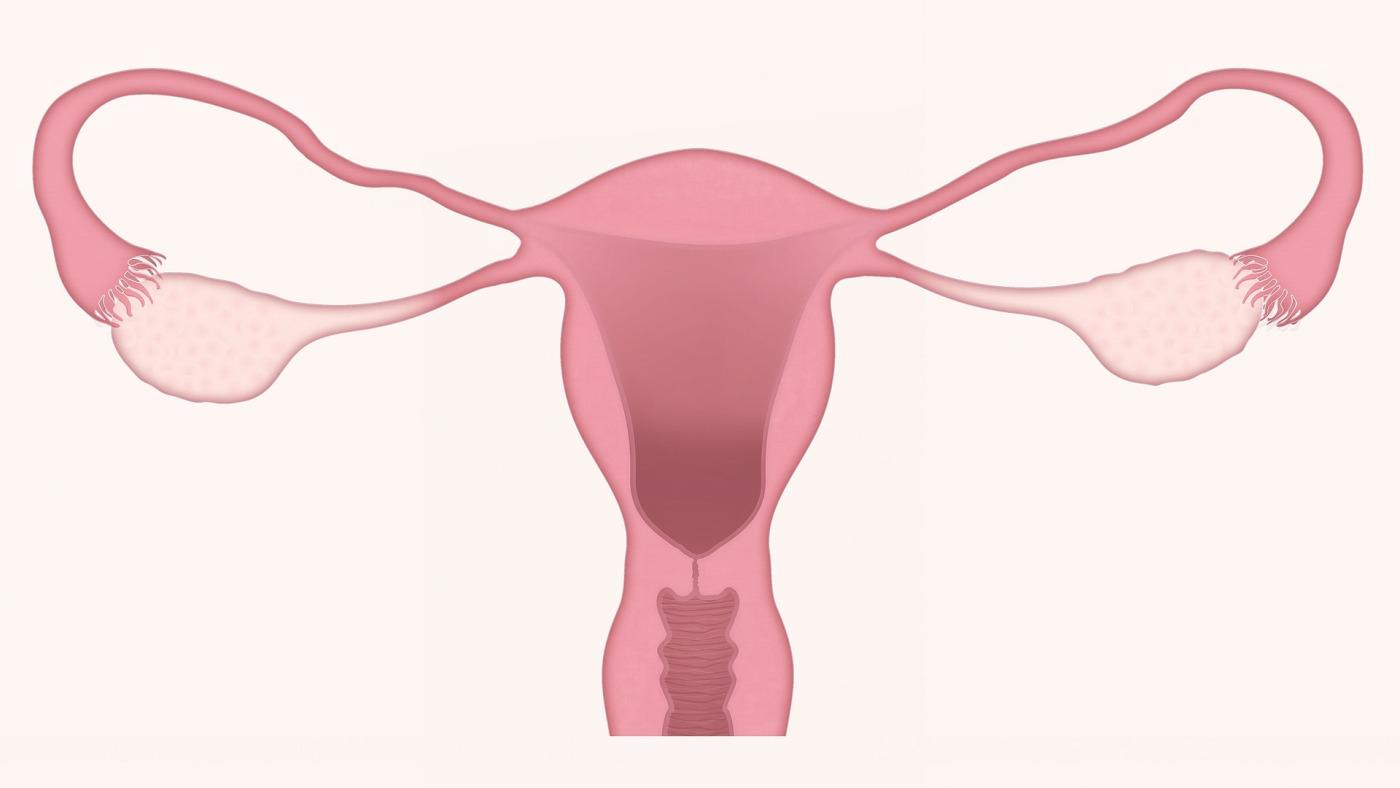
CLOGGED FALLOPIAN TUBES: What you need to know
The infertility is not only related to ovulation problems. Problems can also arise with the tubes when they are blocked or damaged. The egg and the sperm just can't seem to meet. However, Dawasanté experts provide you with a natural herbal treatment to unblock your tubes permanently without side effects and without surgery.
Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
What are the tubes?
- The uterine tubes or fallopian tubes are part of the genital system. There are two, which are on either side of the uterus. They connect the ovaries and the uterus via the pinna.
- The tube-shaped uterine tubes are used to receive the oocytes released every month from the ovaries and to transport them to the uterus. When the egg is expelled by the ovaries during ovulation, it is sucked in through the pinna of the tube. Fertilization (meeting between the egg and the sperm ) takes place in the tubes, during the journey from the egg to the uterus.
- For a woman to get pregnant and have a baby, the tubes must be functioning normally and be intact (at least one!). In 15% of cases of fertility disorders, the causes are linked to an abnormality of the tubes.
Tubal obstruction: what is happening?
- When the tubes are blocked , it will interfere with the movement and progression of the egg and sperm. Either the egg cannot meet the sperm (and there is no fertilization) or there is fertilization, but the egg cannot progress to the uterus.
- When fertilization does not take place or remains impossible, the egg is automatically lost in the abdominal cavity. We are talking about tubal sterility.
- If the blockage is not complete, the fertilized egg will be able to circulate, but will have difficulty making its way to the uterus. The egg will then implant in the tube and evolve into an ectopic pregnancy. At some point, the tube will rupture, causing internal bleeding.
Tubal abnormalities: what are the causes?
Many conditions can lead to blockages in the tubes and cause infertility. This anomaly is linked to genital infections, endometriosis or a sequel to surgery (adhesion for example).
Genital infections
- Genital infections are most often the result of sexually transmitted diseases that affect the tubes.
- Salpingitis is an inflammation of the tubes due to a genital infection. It can be acute (that is, the infection is recent) or chronic (the infection has occurred in the past and still persists) and causes obstruction of the tubes. Infections associated with salpingitis are usually caused by Chlamydia, mycoplasmas or gonococci. These are the germs responsible for sexually transmitted diseases, but which often go unnoticed.
- To prevent these infections, it is recommended to protect yourself during sexual intercourse (especially in the case of multiple or occasional partners) and regular monitoring by your gynecologist is necessary.
Other infections
- Other infections can infect the tubes. In case of peritonitis (an infection of the peritoneum) for example, following a complicated appendicitis, the tube can be infected.
- Uterine infections can also block the tubes. In the event of a history of abortion or miscarriage, tissue scars after these events will develop and form obstacles in the tubes. This is also the case with one or more history of ectopic pregnancy.
Endometriosis
- The Endometriosis is a gynecological condition in which the endometrial tissue which normally covers the uterine wall, is found in the fallopian tubes. The abnormal presence of this uterine lining in the tubes will block the progression of spermatozoa to the egg and prevent fertilization.
Surgical sequelae
- We talk about adhesion when the walls of the tubes stick together, preventing the movement of the egg and sperm. These adhesions are sometimes post-operative complications. They can form following an appendectomy or surgery of the ovaries or uterus. These post-operative complications are rare today because they are easily controlled.
How do you know if the tubes are blocked?
-
The obstruction in the tubes is often difficult to detect because there are few symptoms (possibly some abdominal pain or more abundant vaginal discharge). Consultations and analyzes are only carried out during the infertility assessment carried out when the woman who wants a child cannot get pregnant, after having had regular and unprotected sex for 1 year. During this assessment, in addition to the questioning and clinical examinations, the doctor will have to prescribe several examinations and analyzes to identify the problem.
- The specific test to detect an abnormality in the patency of the tubes is hysterosalpingography. It consists of injecting opaque product from the cervix and following the progress of this product in the tubes by an x-ray.
- In addition to the hysterosalpingography, the doctor may need to perform a hysteroscopy, an examination which allows the uterine cavity to be visualized using an endoscope (an optical fiber) through natural channels.
- A laparoscopy can also be considered: under general anesthesia, it allows the tubes to be examined from "inside" with an optical device after having made a small incision at the navel.
Tubal abnormalities, what treatment?
- Treatment will depend on the cause of the obstruction. Only the doctor is able to prescribe the appropriate drugs or treatment methods. The need for treatment depends mainly on the state of patency of the tubes, the state of the genitals and the state of health in general. You are free to discuss all the treatment options that may be available to you to find the most suitable for you.
- The doctor may indicate laparoscopic surgery (laparoscopy), if your state of health allows it and according to certain parameters evaluated by the doctor. It is a surgical procedure performed under general anesthesia.
- Depending on the state of the patency of the tubes, the doctor may suggest a salpingectomy, a surgical procedure that involves removing the blocked and diseased tube, especially in the case of a hydrosalpinx (the tube is full of liquid). You can then be a candidate for in vitro fertilization.
- Tubal cannulation is a less burdensome surgical procedure than laparoscopic surgery, performed when the obstruction is located closer to the uterus. The operation consists of introducing a cannula through the uterus to unblock the tube.
Good to know: if only one of your tubes is blocked, treatment is not always mandatory, pregnancy is possible. If both are blocked, there are other options available to help you get pregnant, especially if the methods of treating blocked tubes remains thin. The IVF is now the oldest method, but the most appropriate for getting pregnant if tubes plugged.
If your fallopian tubes are blocked, it will cause temporary infertility since the meeting between the sperm and your oocyte cannot take place. What are the causes of blocked tubes ? Are there any treatments to remedy blocked tubes
The uterine or fallopian tubes are an integral part of the female genital system . These tubes, since there are two, play an essential role in reproduction: they connect the ovaries and the uterus by the pinna. Their main objective is to receive the eggs released every month during the period of ovulation and to lead them to the uterus. The phenomenon of fertilization occurs in the tubes during the path between the egg and the uterus. In order to get pregnant, the tubes have to work properly. Indeed, this would prevent the meeting between the male and female gametes. Note that 15% of infertility cases result precisely from this style of abnormality in the tubes .
The causes
There are many reasons for the blocked fallopian phenomenon . First of all, there is salpingitis which is an inflammation of the tubes. Then comes the case of genital infections , usually caused by sexually transmitted diseases. That's why doctors recommend protecting yourself with each intercourse , especially in the case of multiple partners. This can indeed lead to infertility in some cases. The endometriosis is itself a disease that can also affect the fallopian tubes. It can interfere with the path of sperm to the oocyte feminine. Inflammation of the small pelvis can affect and obstruct the upper part of the reproductive organs. As for abnormalities affecting the vagina and uterus , they can also be a source of possible infertility . Myomas, which are usually benign growths, can also come into a tube and block it. Finally, certain surgical sequelae can play a role in the malfunction of the tubes .
Tubal obstruction and treatment
Obstruction in detail
First of all, you must first be sure that your tubes are well blocked. The symptoms are not necessarily obvious to detect because the pain is minimal. It is when you go for analyzes (such as during the infertility assessment ) that we can see if this is the case or not. This very specific examination consists of injecting a product from your cervix and following its progress to the tubes using an X-ray. The blocked tubes can also be detected in other tests such as hysteroscopy and laparoscopy. If your fallopian tubes are indeed blocked, it will upset or simply make fertilization impossible. When this is impossible, we speak of tubal sterility. If the obstruction is not complete, the fertilized egg will implant in the tube before creating a uterine pregnancy, possibly causing internal bleeding if the tube ruptures.
Possible treatments
The treatment of this pathology will depend both on the nature and on the cause of the obstruction. You will need to go through stimulation of ovulation by administering drugs in order to produce eggs in each cycle . The intervention is recommended for women with both tubes blocked, but it is not always enough to improve fertility . In some cases, women will then use IVF to get pregnant.
When the fallopian tubes are blocked, the meeting between a sperm and an oocyte cannot occur. This obstruction therefore constitutes a temporary cause of infertility or, in the most severe cases, of sterility. There are many reasons for the obstruction of one or both uterine ducts. What are they ? What are the possible treatments? Response elements.
What are the fallopian tubes used for?
Better known as the uterine tubes , the fallopian tubes are an integral part of the female genital system. Thus, the two tubes play a major role in the process of human reproduction since they connect the ovaries and the uterus. It is in them that the oocyte, resulting from the ovary, transits and can be fertilized by a sperm. In some cases, these uterine tubes can become blocked, preventing the meeting of male and female gametes.
Blocked fallopian tubes: what are the causes?
There are many possible reasons for the obstruction of one or both fallopian tubes :
- the PID : it corresponds to inflammation of the fallopian tubes. It is mainly caused by bacteria from the Chlamydiae family , although in some cases gonococci or mycoplasmas can be responsible.
- genital infections: these are often caused by sexually transmitted infections (STIs). It can lead to cases of infertility or sterility.
- the Endometriosis : This disorder is due to an abnormal proliferation of endometrial tissue outside the uterine cavity. This gynecological pathology can affect the fallopian tubes and hinder the progression of sperm to the oocyte.
- inflammation of the small pelvis: this is an upper genital infection (IGH), that is to say of the upper part of the reproductive organs.
- congenital anomalies of the uterus or vagina: these so-called "Mullerian" anomalies can reduce a woman's chances of getting pregnant.
- the myomas : these benign growths can be housed in a trunk and obstruct the passage.
Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
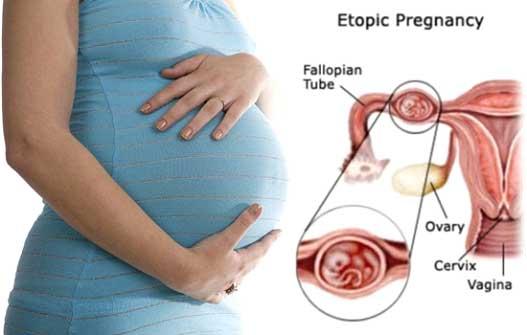
PREGNANCY WITH A SINGLE FALLOPIAN TUBE: natural treatment
Pregnancy is the condition of a pregnant woman. The question is whether a woman can get pregnant with just one fallopian tube. Obviously YES. Dawasanté experts offer you a natural treatment to unblock your tubes and allow you to quickly get pregnant. Click on the image below to discover this natural treatment
PREGNANCY WITH A SINGLE BLOCKED FALLOPIAN TUBE
Is it possible for me to get pregnant if I only have one fallopian tube?
Uterine tubes (or fallopian tubes) are muscle tubes leading from the ovaries to the uterus. The uterine tubes are responsible for collecting the egg each month. The fusion between the egg and the sperm (fertilization) also takes place inside the egg. The resulting embryo is taken to the uterus where the pregnancy will progress. Obviously, the fallopian tubes play an essential role in natural reproduction linked to ovulation, fertilization and pregnancy. Diseases or abnormalities of the uterine tubes are responsible for up to 30% of infertility cases.
What if I have blocked tubes and want to get pregnant?
Here is the best African herbal remedy to unblock the tubes and get pregnant quickly. These herbs are very effective in unblocking the fallopian tubes. They have already enabled many women around the world who had blocked tubes to regain their fertility without operations. If you have blocked tubes, here are the medicinal plants that will allow you to experience the joy of being a mother.
To discover our natural remedy to unblock the tubes and get pregnant quickly, Click on the image
The anatomical integrity of the fallopian tubes is essential for natural fertility. Many health conditions can affect the fallopian tubes. For example, an ectopic pregnancy (pregnancy outside the womb in one of the fallopian tubes). Surgery and removal of the affected tube are often necessary for such conditions for these to be properly thinned. Questions arise after surgery: Will I be able to get pregnant naturally if I only have one fallopian tube? The answer is yes, although the chances of conceiving naturally decrease slightly. Some research estimates this decrease between 15 and 45%.
There are other diseases, as well as ectopic pregnancies, which can damage one or both fallopian tubes. For example, endometriosis, sexually transmitted diseases and abdominal surgery (appendicitis and peritonitis, among others). If both tubes are affected (or if they have been removed), natural conception is highly unlikely and appropriate treatment will include assisted reproduction therapy through in vitro fertilization in order to achieve pregnancy.
Have only one fallopian tube. Is it possible for me to get pregnant?
Yes. The fallopian tubes are a pair of tubes through which eggs pass from the ovaries to the uterus. Each month, in a process called ovulation, one of the ovaries releases an egg that travels to one of the fallopian tubes, where it may or may not be fertilized by a sperm.
You may only have one fallopian tube if you've had pelvic surgery for an infection, tumor, or ectopic pregnancy. Sometimes some women are born with just one tube. However, you can still be pregnant with just one tube if:
You have at least one working ovary
You have monthly menstrual cycles (ovulation)
Your remaining fallopian tube is healthy
If you are unable to get pregnant after trying to conceive or have a known history of fallopian tube problems, see your gynecologist or reproductive endocrinologist for evaluation.
HERE ARE SOME TIPS TO FIGHT AGAINST CLOUDY TRUMPS
1-Turmeric
Turmeric is a natural anti-inflammatory. It can be very effective in unblocking the fallopian tubes. Curcumin, the active ingredient in turmeric, is very effective in reducing inflammation. You can consume curcumin in supplement form, add turmeric to your food, or drink a glass of turmeric.
Turmeric has no known side effects when taken in small doses. However, at doses of more than 8 grams per day, it can have unwanted effects. Make sure you take the correct dosage of turmeric or, better yet, add the spice to your cooking.
2-Garlic
Garlic is a great way to improve fertility and unclog fallopian tubes. Garlic has always been consumed for its many health benefits as the aphrodisiac properties present in garlic help in improving blood circulation in the body. Eating raw garlic every day on an empty stomach helps fight infertility in women, lowers blood pressure and cholesterol.
3-Vitamin C
Vitamin C is an antioxidant that can reduce inflammation by helping your immune system to function better. For this reason, it is ideal for healing scars and may have a positive effect on the fallopian tubes.
If you suspect that the cause of the blocked fallopian tubes is an infection, vitamin C can help you overcome it. To unclog your tubes, we recommend that you use natural vitamin C. It's easy to get vitamin C from food sources, especially when you like citrus fruits. Eat as many oranges, lemons, and grapefruit as possible. Aside from, you can try strawberries, broccoli, and green peppers to cure yourself with good vitamin C.
4- Castor oil
Castor oil has been used for centuries to improve fertility in women, and more specifically to unblock the fallopian tubes. How is it used?
- dipped a rag in castor oil
-Place this cloth on the skin on the lower abdomen. This will improve circulation and promote healing of the tissues and organs under the skin. Castor oil therapy helps the fallopian tubes by softening tissue and improving circulation in the pelvic area.
5- Apple cider vinegar
Apple cider vinegar is a fermentation product that produces yeasts and bacteria that are beneficial for unblocking the tubes. This is because vinegar contains a number of vitamins and minerals, including magnesium, potassium, copper, group B vitamins and vitamin C. Taken daily, it can help unblock the fallopian tubes by balancing hormones and shrinking fibroids.
Manual:
-Mix 2 tablespoons of apple cider vinegar in 1 glass of water
-You can add a touch of honey or molasses to sweeten the mixture.
-You can drink the mixture right away or sip it for 30 minutes.
6-Meditation
Meditating daily will help lower stress levels and promote general healing. However, reducing stress reduces deterioration and inflammation of the fallopian tubes.
As an additional tip, don't forget to start meditating with a short session consisting of breathing exercises and relaxation techniques. Even if you only do it for a few minutes, meditation will provide you with positive energy to start your day and reduce your stress.
Because of the high number of eggs that just one of your ovaries can make, your chances of getting pregnant again are almost as great as before this procedure. The only problem is that there may be a small anomaly in the second proboscis. It may therefore be necessary to do some examinations to check that it is perfectly permeable. Your gynecologist will tell you if he deems these exams necessary. But whatever your situation, technical advancements in this area suggest that your chances of becoming a mother in the future remain intact.
NATURAL TREATMENT FOR CLOGGED FALLOPIAN: TESTIMONIAL
BLOCKED FALLOPIAN TUBE NATURAL TREATMENT TESTIMONIAL
I, MUKABE Jennifer, suffered for more than 05 years from obstruction of the fallopian tubes. Both my tubes were blocked, so it was impossible for me to get pregnant naturally. If you suffer from blocked fallopian tubes click here.
I want to share with you the best solution to unclog fallopian tubes. This is a natural treatment based on medicinal plants which allow the tubes to unclog, this natural treatment is a real miracle after 06 weeks of treatment I went back to my doctor to see the condition of my tubes and indeed we noticed that there was an improvement and that the liquid could pass. After 02 months of full treatment, we tried to have a child and by the grace of GOD after the 05 long waits and search, we found the solution. Today we have our daughter GRACE who is already 08 months old and in great shape. It is beautiful and very possible to unclog the fallopian tubes and to get pregnant naturally, the experts at DAWASANTE allowed us to have our child without having to undergo IVF.
What if I have blocked tubes and want to get pregnant?
Here is the best African herbal remedy for unblocking the tubes and getting pregnant quickly. These herbs are very effective in unblocking the fallopian tubes. They have already enabled many women around the world who had blocked tubes to regain their fertility without operations. If you have blocked tubes, here are the medicinal plants that will allow you to experience the joy of being a mother.
To discover our natural remedy for unblocking the tubes and getting pregnant quickly, click here
Natural herbal treatment is the best way to naturally unblock the fallopian tubes, become fertile, and have children. Luciole had testified last year, asking our opinion on his situation. As I explained to him in my answer, with the baby tests, you never know how it will be, and especially how long it will take. And indeed, after more than a year, the doctors realized that Luciolehad blocked tubes that would not allow her to get pregnant naturally. Here is his testimony.
{TESTIMONIAL} 16 MONTHS OF BABY TESTING… TO FIND OUT THAT I WON'T GET PREGNANT NATURALLY!
Hello,
I asked you for a little help a few months ago because I wanted to have a baby.
You answered me and I thank you. So I chose to continue with the baby tests.
As a reminder, at the time, I had cancerous lesions on the cervix (therefore rigorous monitoring) and polycystic ovaries. We were already in average dispositions, but super confident in nature, and in life. Guest gifts wedding dresses classes dance wedding catering wedding stationery.
The only indication of the gynecologist "come see me in a year if you are not pregnant".
So we went head-to-head and took our practical work seriously.
I saw my gynecologist no less 3-4 times in these 12 months, for different follow-ups. Pain in the ovaries, lesion checks, and of course the ovaries. Nothing to report, we continue the tests without pressure, without a schedule, just because we like to train!
WE WERE AGAIN IN HIS PRACTICE IN THE 13TH MONTH OF BABY TRIAL
Still nothing on the horizon.
He then talks to us about infertility, treatment protocols, reimbursements, and assisted reproduction. The famous words that scare. My partner and I are a little shaken up, even if we suspected it (and yes I tend to dig a subject long, wide, and across…).
We each pass our many exams (supposed to be 100% refunded, but we still have to move forward ... in a month anyway! Yes that they do not say!).
My last meeting is a hystero (tube radio using a contrast liquid). Normally it doesn't hurt, but opinions differ on this.
For me, it was very painful.
My two tubes are blocked, the liquid does not pass, and forces entry. After the 4th test, the doctor decides to stop forcing and hurting me. But she has this little phrase "damn it was just starting to pass."
So I only listen to my courage and tell him to make one last try to unblock the tubes. It hurts horribly, but the wicked eventually opens, and the liquid passes.
When I get home, I'm completely confused.
Blocked TUBE? Why ? Where is that from?
I inquire and see that I do not fit into any category of pre-arrangements with blocked tubes ...
I even contacted my mum saying "you're sure I didn't have appendicitis, eh ?? ". I knew the answer, of course, but at least that could explain everything that was on my mind.
I NEEDED TO UNDERSTAND WHY ALL THIS HAPPENED TO ME
Why the cancerous lesions due to the papillomavirus when I had always protected myself?
Why the polycystic ovaries, when I had ultrasounds of the ovaries younger?
Why are the tubes blocked, and how did we miss it?
Right now I feel super angry.
Against the medical world, against life a lot too. But above all, I do not understand why all this has never been seen or considered important enough to inform me.
When I was 17, I did this famous ultrasound of the ovaries. I was told, "you have cysts, it's nothing, we put you on the pill that will go away". I have been on the pill for 11 years. They didn't go away, and I gave my body 11 years of hormones without ever knowing it wouldn't change a thing. Without ever knowing that maybe it will be a little difficult to have a baby.
And today, it took a painful and "exceptional" examination to discover that the months of testing had been wasted, it was unlikely to pass. With a diagnosis that says "we don't always know where it comes from, it's probably an old infection that has degenerated, often there are no symptoms."
So yes, why do a test without symptoms? To avoid learning at 29 that it was screwed up anyway (naturally).
I really wonder how can we miss all of this, and if we could have done something, anything to reduce the bill.
If you suffer from blocked fallopian tubes click here.
Today I can respond to Luciole and all the other women who suffer from blocked fallopian tubes. In all sincerity and with all my certainty, having the tubes blocked is not inevitable. The solution to naturally unblocking the fallopian tubes and having children exists and it is very effective. Health experts from Africa have developed a natural herbal treatment that helps to naturally unblock the fallopian tubes and get pregnant naturally.
I take this opportunity to express my eternal gratitude to the experts at Dawasanté
To discover our natural remedy for unblocking the tubes and getting pregnant quickly, click here
Contact our experts, tel / whatsapp: +33644661758 / +22990312738

ENDOMETRIOSIS AND WEIGHT GAIN: Natural treatment
Endometriosis causes the endometrial tissue, which usually lines the uterus, to grow outside the uterus. It can cause chronic pain, heavy or irregular periods, and infertility. Some people also report weight gain and bloating.
Here is the natural treatment to cure the weight gain caused by endometriosis and itself.
Click on the image below to discover this natural treatment.
Little research has explored why endometriosis could lead to weight gain. People with endometriosis who suspect that the disease is causing weight gain or preventing them from losing weight should talk to a doctor.
Sometimes other conditions such as polycystic ovary syndrome (PCOS) can mimic the symptoms of endometriosis.
In this article, we take a look at how endometriosis can lead to weight gain, and how to achieve and maintain a healthy weight.
To discover the natural solution against endometriosis, click here
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
Does Endometriosis Cause Weight Gain?
Although there is a lot of anecdotal evidence that has linked endometriosis to weight gain, scientific research does not yet prove it.
Qualitative research A reliable source from 2014, some women feel that endometriosis contributes to weight gain and poor body image.
Endometriosis can cause weight gain in at least four ways.
Bloating
Bloating and fluid retention are common symptoms of endometriosis. Although bloating does not cause fat, it can feel heavier and thicker.
Bloating can also change the way clothes fit. Many people notice that bloating is worse immediately before or during their period.
Estrogen
Endometriosis is an estrogen-related disease, which means that symptoms worsen when estrogen levels are higher.
Some people believe that estrogen dominance leads to weight gain. It happens when the body produces too much estrogen, exceeding progesterone.
Drugs to treat endometriosis
Many studies show that treatments for endometriosis can lead to weight gain.
One of the most effective treatments for endometriosis is a synthetic form of the hormone progesterone. Progesterone slows the growth of endometrial tissue.
However, many women experience weight gain with progesterone. According to a 2010 Trusted Source study, 40 to 50% of women gain weight or retain water with progesterone treatment.
Pain
Endometriosis is painful. For some people, the pain is severe enough to make it difficult to exercise and keep active. Over time, this can lead to weight gain.
Some symptoms of endometriosis can make a person look or feel heavy. These symptoms can include:
- Bloating
- Constipation
- Water retention
- Endometrial tissue masses in the pelvic region
Other symptoms of endometriosis can include:
- Severe cramps during periods
- Pelvic pain between periods
- Pain during intercourse
- Difficulty getting pregnant
- Bladder pain
- Strong urge to urinate
- Incontinence
- Pain during bowel movements or urination
- Unexplained pain in the stomach
The severity of symptoms does not necessarily indicate the extent of adhesions in endometriosis. Some people with severe endometriosis have no symptoms. People with mild endometriosis can have severe symptoms.
How to lose weight with endometriosis
Many natural and alternative health sites promise to help people with endometriosis lose weight by following a specific diet. However, there is no clinical evidence to suggest that a diet specific for endometriosis can contribute to weight gain or reduce symptoms of endometriosis.
Having surgery to remove endometrial tissue that is growing outside the uterus can help relieve pain and may reduce bloating. This, in turn, can help a person lose weight or appear slimmer.
To lose weight in any situation, a person must burn more calories than they consume. Some strategies that can support this goal include:

- Increase physical activity. Walk as often as possible and take regular breaks after long periods of sitting. The 2015-2020 Physical Activity Guidelines for Americans Trusted Source advise getting 150-300 minutes of moderate-intensity cardio or 75-150 minutes of high-intensity cardio per week. They also advise strength training at least 2 days a week.
- Eat a variety of filling and lower calorie foods. Avoiding sugary snacks, sodas, and other sugary drinks in excess can also help.
- Eat more protein. Protein can improve metabolism and help a person feel fuller for longer. This reduces the desire to eat high calorie snacks.
People with endometriosis should talk to a doctor about weight loss strategies, especially if they have other conditions such as PCOS.
PCOS has symptoms similar to endometriosis. PCOS is caused by hormonal imbalance and, like endometriosis, can cause painful periods.
Other symptoms of PCOS include:
- Irregular or absent periods
- Excessive hair
- Unexplained weight gain
- Difficulty getting pregnant
- Insulin resistance or diabetes
People with endometriosis can also get PCOS. For this reason, it is important that people with irregular periods, painful periods, or fertility problems seek testing for both of these conditions.
PCOS can cause weight gain, often due to insulin resistance. A low glycemic index diet may contribute to weight gain associated with PCOS. Some people also find hormonal birth control pills to relieve symptoms.
Endometriosis is a chronic disease. However, a number of management strategies, including hormone therapy and surgery, can help reduce symptoms.
Many women with endometriosis feel frustrated with the little research available on weight gain related to endometriosis. A doctor who listens and takes a person's symptoms seriously is the key to finding effective treatment.
By discussing weight gain with their doctor, patients can gain personalized weight loss strategies and support for dealing with the challenges of living with endometriosis.
To discover the natural solution against endometriosis, click here
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
Did this article answer all of your questions?
Leave us a comment or contact us via WhatsApp at: 0022996374527 for more information
HERBAL REMEDY FOR UTERINE POLYPS : Dawasanté experts
UTERINE POLYP: HERBAL REMEDY
The Uterine polyps are benign and are formed on the surface of the endometrium, which is located within the uterine cavity. They can be simple and multiple. In some cases, polyps at the offset neck. Neoplasm has a body and a leg, which is attached through the endometrium. Numerous medical observations suggest that polyps are most often found at the bottom of the uterus or its walls. Here is a herbal remedy that the experts at Dawasanté put at your disposal to treat uterine polyps. Click on the image below to discover this herbal treatment for uterine polyps.
The causes of this disease can be different, and tumors appear in young girls and older women. If the doctor put such a diagnosis - do not despair. There are ways not only with medication, you can still treat uterine polyps with an herbal remedy. Both methods are effective in killing polyps and preventing new ones. A woman can choose the most suitable treatment option for yourself, depending on the characteristics of her body.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: https://wa.me/22996374527
Signs and symptoms of uterine polyps

Pronounced symptoms of uterine polyps are few, their presence is easily confused with symptoms of other diseases. The main symptom that should alert a woman - profuse vaginal discharge.
During the early development of the disease, uterine bleeding and failure of the menstrual cycle can occur. A polyp tends to increase. This process leads to involuntary contractions of the uterus, the cervix by which it is relaxed and pushed into the vagina neoplasm. Women may, therefore, feel pain and cramping, vaginal discharge is observed as ichor.
Asymptomatic illness contributes to the fact that patients in the early stages do not pay much attention to minor signals from the body, resulting in seeking medical assistance too late.
Polyps are especially dangerous for pregnant women. In such cases, treatment is only possible with the use of homeopathy and traditional medicine.
To get rid of polyps, use some folk remedies only after histological analysis, which will help determine the exact nature of the polyp. These tumors are glandular, fibrioznymi glandular, fibrioznymi, and adenomatous. Adenomatous polyps - the most dangerous, as they are the main irreversible changes at the cellular level. These tumors are signs of a precancerous condition in the lining of the uterus.
Celandine for the treatment of uterine polyps

To achieve good results from the treatment of uterine polyps herbal remedy can be at an early stage when the disease is only just beginning to develop. Also, folk remedies are often used as prophylaxis before or after drug treatment. But regardless of the folk method, women need to be sure to see your doctor.
Most often, to get rid of polyps in the uterus, used celandine. It is recognized as the most effective and popular way. It is necessary to take and use for douching.
To prepare the healing infusion to collect the fresh celandine cabbage and fill their glass jar, then pour boiling water. In addition, the bank should close the lid, wrap with a blanket or a towel, and infuse it in this way for 12 hours.
The ready infusion should be taken three times a day. The initial dose should be 1 st. g., which should be gradually increased by 100 ml at a time. In this way, the treatment of uterine polyps should be carried out for two weeks after which requires a break - three weeks. In addition, the course must be repeated.
Back to summary
Herbal and berry extracts to deal with polyps
Useful and effective extracts that are able to overcome the disease, usually prepared from rose hips, berries, cranberries, nettle. This type of treatment is considered to be one of the most benign, which traditional medicine offers.
To prepare the infusion of the healing need:
- cranberries
- chopped nettles
- hips
All the ingredients should be mixed together and the mixture pour a glass of hot water. Soak the infusion should be in a closed container for 4 hours. Means should be taken twice a day for 250 ml.
Equally effective is accounted for on the basis of the tincture of golden whiskers. To make this folk remedy, you need to:
- 50 golden mustache seals;
- 500 ml of vodka.
The plant should be crushed and pour vodka, then let it brew for 10 days. The ready infusion should be taken twice a day in the diluted form: a third of a cup of water add 20 drops of medicated liquid. The use of these drugs is necessary before meals. Treatment should be carried out for a month, then take a break for 10 days. Expect full recovery from uterine polyps to be possible only after five treatments.
Pumpkin seeds and garlic as a remedy for polyps

Garlic since ancient times is considered an excellent remedy for a variety of ailments. List of public methods can beat uterine polyps, also it includes this herbal medicine. Based on this, it is possible to make their own medical rod.
This will require a large clove of garlic, crushed and carefully wrapped the entire mass resulting in a two-layer gauze, then tightly bandage. The ready compress should be careful at night to enter as deep as possible into the vagina and pull it out in the morning. To remedy such manipulation of polyps should be repeated for a month every night.

For an indoor reception, it is possible to prepare another useful folk medicine on the basis of pumpkin seeds. Require:
- 7 hard pieces of egg yolks;
- fresh pumpkin seeds;
- 2 cups of vegetable oil.
The seeds should be well ground and add the yolks carefully mashed. Then the resulting mixture should be mixed with vegetable oil, optionally to form a homogeneous paste. This is followed by a mass placed for 30 minutes in a water bath. When the means ready to cool down, it is necessary to take a teaspoon of fasting for five days, then take a break for the same period of time. The repetition rate required to complete recovery. The mixture should be refrigerated, tamped.
Douching using an herbal decoction

In the arsenal of folk remedies are the very popular treatment showers. To combat this way of uterine polyps is used quite often. Typically, douching should be used if the woman against the background of the disease is observed vaginal bleach.
To prepare the solution for irrigation will need:
- yarrow
- rosemary leaves
- Sage leaves
- oak bark
All the ingredients must be crushed and mixed in an enamel container, then pour 2, 5 l of boiling water. Then the mixture should be put on the fire and bring to a boil. Boil the broth and simmer for half an hour should be. When it is ready, it is necessary to cool it to room temperature. Then you need to empty the infusion using a cheesecloth or fine strainer.
The lukewarm solution is used for douching twice a day every day to get rid of the disease.
Medicinal herbal teas based on nettle and knotweed

To cook another decoction for douching can use these herbs:
- nettle
- knotweed grass
- pharmacy chamomile - 1 tbsp.
Herbs need to grind and mix. The resulting mixture should be put in an enamel saucepan and pour boiling water 1 liter. Boil the followed broth for 5 minutes over medium heat and then allow to cool to room temperature.
Strained broth Ready to use for douching. Treatment is effective, it is desirable to carry out the procedure at least twice a day for 2 weeks.
Always remember that the reproductive function is one of the most important for a woman, so in case of alarming symptoms must necessarily be examined by a doctor. It is useful in visits to the doctor and as a prophylactic measure. If the disease is detected and treatment is still necessary to start the independent thoughtless application of various folk remedies is not necessary. It is necessary to consult a gynecologist, who will choose the most suitable and safe way.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: https://wa.me/22996374527
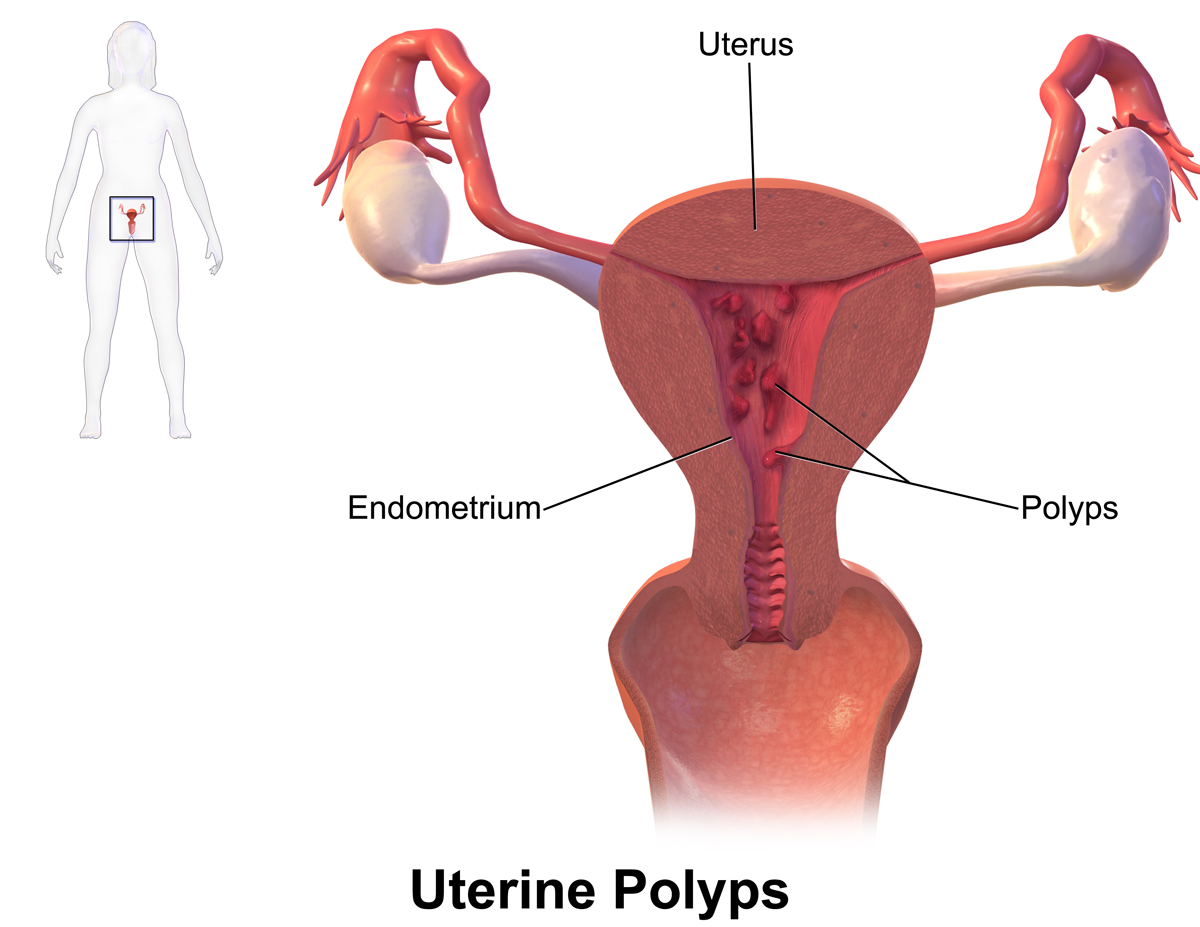
UTERINE POLYPS AND CANCER: Natural treatment
UTERINE POLYPS AND CANCER
A polyp can sometimes seem like a fibroid uterus ( polyp fibrous) or cancer endometrial ( polyp atypical, irregular). Conversely, cancer endometrial can sometimes look like a polyp. The combination of a polyp to cancer endometrial is more common after menopause. However, Dawasanté experts provide you with a natural treatment to cure uterine polyp cancer. Click on the image below to discover this natural treatment.
To contact our experts please call or write to us on the following number, tel / WhatsApp: https://wa.me/22996374527
The uterine polyps are growths that develop at the expense of the lining of the uterus (endometrium), or at the expense of the lining of the cervix (endocervical).
These growths are benign tumors. They can be single or multiple. A polyp can be "pedicle" (comprising an insertion foot) or sessile (broad implantation base). It can be "fibrous" or "mucous". By definition, the development of a polyp occurs at the expense of a mucous membrane. This is why, in addition to the uterus, certain organs or areas of the human body can be invaded by this type of tumor such as the bladder, colon, stomach, vagina, etc.
The uterine polyps are outgrowths attached to the inner wall of the uterus which extends into the uterine cavity. Cellular proliferation in the lining of the womb (endometrium) results in the formation of uterine polyps, also called endometrial polyps. These polyps are usually non-cancerous (benign), although some can be cancerous or turn into cancer (precancerous polyps).
A uterine polyp can look like a fibroid or a cancerous tumor, so be careful not to get the wrong diagnosis. Cancerization of the polyp is possible.
All examinations performed should show whether the uterine polyps are benign or not. Thus, after removing these growths, a complete analysis of them is required. Postmenopausal women are prone to endometrial cancer combined with uterine polyps.
Two forms of treatment are possible to treat polyps, the choice is based on their benignity, size, appearance, etc. Those that are small and less worrying may go away as a result of hormonal drug therapy. With this treatment, the patient takes progestins. In most cases, operative hysteroscopy is necessary, it consists of the removal of the polyps. This form of treatment should be carried out with great care, especially in women who wish to have children later. For postmenopausal women, the risk of recurrence being high, endarterectomy is recommended.
Endometrial cancer is a cancer of the inside of the uterus, where the endometrium is the lining that lines the inside of the uterus. In women with cancer at this level, endometrial cells multiply abnormally. Endometrial cancer usually occurs after menopause, but 10 to 15% of cases affect premenopausal women, including 2 to 5% of women under 40 years old.
A significant proportion of endometrial cancer is thought to be attributable to an excess of estrogenic hormones produced by the ovaries or supplied by the outside. The ovaries produce 2 types of hormones during the female cycle: estrogen and progesterone. These hormones act on the endometrium throughout the cycle, stimulating its growth and then its expulsion during menstruation. An excess of estrogen hormones would create an imbalance conducive to the poorly controlled growth of endometrial cells.
Several factors can increase estrogen levels, such as obesity or hormone therapy with estrogen alone. This type of hormone therapy is therefore reserved for women who have had the uterus removed or hysterectomy who are no longer at risk of endometrial cancer. For more information, see the People at risk and Risk factors sections.
For some women, however, endometrial cancer does not appear to be caused by a higher level of estrogen.
Other causes are involved in endometrial cancer, such as advanced age, overweight or obesity, genetics, hypertension, etc.
Sometimes cancer occurs without a risk factor being identified.
Like any mucous membrane, the endometrium is made up of surface cells called “epithelial” and supporting tissue, the “chorion”. More than 90% of endometrial tumors develop at the expense of the epithelium. This category includes cancerous lesions such as adenocarcinomas and carcinosarcomas, pre-cancerous lesions such as atypical hyperplasias, endometrial polyps, and lesions induced by tamoxifen. Adenocarcinomas, the most common form, are developed from "glandular" type epithelial cells.
Other metabolic factors: diabetes and glycemic load
Diabetes is a risk factor for endometrial cancer. The risk of developing this cancer is twice as high (significant relative risk) in diabetic patients than in people without diabetes (Larsson, 2006).
It is the development of insulin resistance that is responsible for the increased risk of cancer. Insulin is then in large quantities in the blood and will be able to stimulate growth factors acting on the endometrium. The precise mechanisms are not well known. This is confirmed in the 2013 WCRF / AIRC report. This same international report also found that increased glycemic load (which estimates the ability of foods eaten to increase blood glucose) is a risk factor for endometrial cancer with a probable level of scientific evidence to account. based on current scientific data; these are not as convincing as for obesity.
Early puberty and late menopause
Age at puberty determines when the ovaries start producing estrogen, and menopause determines when they stop producing estrogen. Earlier puberty or late menopause, therefore, exposes a woman to estrogen for a longer period of her life and therefore represents a risk factor.
Not having had a child (nulliparity)
The menstrual cycle of women experiences a period during which the functional area of the endometrium collapses. In order to accommodate the future fertilized egg, the endometrium must regenerate. For this, estrogen plays a role in stimulating cell growth in the endometrium.
During pregnancy, there is no ovulation for 9 months. The estrogen stimulation does not stop, however, but is much less than if there had been 9 ovarian cycles. Thus, women without children are exposed to greater amounts of estrogen: this is considered a risk factor for the development of endometrial cancer (Lochen, 1997).
This is sort of how polyp can be the root cause of cancer or various tumors.
To contact our experts please call or write to us on the following number, tel / WhatsApp: https://wa.me/22996374527
UTERINE POLYPS AND OPERATIONS: Natural treatment
UTERINE POLYPS AND OPERATION
First of all, remember that the reproductive function - one of the most important in a person's life, so there should be no treatment of uterine polyps folk remedies without consulting a gynecologist. Only then can it be used in a variety of recipes. If necessary, you can combine treatment folk remedies homeopathy. And some of the most actively advertised drugs, given the rich list of contraindications, usually better not to use. It has been proven that herbal treatment is much more effective and safer in terms of side effects and adverse effects from the use of many homeopathic remedies at the same time. Later in the article, we are going to discuss the different possible operations performed for uterine polyps.
What is a uterine polyp?
The uterine polyps are outgrowths attached to the inner wall of the uterus which extend into the uterine cavity. Cellular proliferation in the lining of the womb (endometrium) results in the formation of uterine polyps, also called endometrial polyps. These polyps are usually non-cancerous, although some can be cancerous or turn into cancer (precancerous polyps). Here is the natural herbal treatment to cure uterine polyps. Click on the image below to discover this natural treatment .
Usually, unless you are diagnosed with uterine polyp late, our natural treatment will heal uterine polyps and have no side effects. Trust us! It is the miracle solution to permanently cure uterine polyps and avoid the operation thanks to the plants. The treatment we offer you to cure Uterine Polyps, which is 100% herbal, will also suppress the symptoms you are experiencing. If you suffer from uterine polyps and want a quick and complete cure, click here. The dawabio experts have the solution for you!
HOW CAN AN UTERINE POLYP BE?
Uterine polyps vary in size from a few millimeters (no larger than a sesame seed) to several centimeters (the size of a golf ball). They attach to the uterine wall by a large base or thin rod.
You may have one or more uterine polyps. They usually stay contained in your uterus, but occasionally they slide down through the opening of the uterus (cervix) into your vagina. Uterine polyps most often occur in women who have gone through menopause or have completed, although younger women can suffer from them as well.
Symptoms
Signs and symptoms of uterine polyps include:
- Irregular menstrual bleeding - for example, having frequent, unpredictable periods of varying length and heaviness
- Bleeding between periods
- Excessively heavy periods
- Vaginal bleeding after menopause
- Infertility
Some women have only bleeding or light bleeding; others are symptom-free.
The causes
Hormonal factors seem to play a role. Uterine polyps are sensitive to estrogen, which means that they develop in response to circulating estrogen.
Risk factors
Risk factors for developing uterine polyps include:
- Being perimenopausal or menopausal
- Have high blood pressure (hypertension)
- Being obese
Complications
The uterine polyps may be associated with infertility. If you have uterine polyps and cannot have children, removing them may allow you to get pregnant, but the data is inconclusive.
Diagnostic
If your doctor suspects that you have uterine polyps, he may do any of the following:
- Transvaginal ultrasound . A thin, wand-like device placed in your vagina emits sound waves and creates a picture of your uterus, including its interior. Your doctor will be able to detect clearly present polyp or identify a uterine polyp as an area of thickened endometrial tissue.
A related procedure, called a hysterosonography also called sonohysterography, involves injecting saltwater (saline solution) into your uterus through a small tube inserted into your vagina and cervix. The saline dilates your uterine cavity, giving the doctor a clearer view of the inside of your uterus during the ultrasound.
- Hysteroscopy. Your doctor inserts a thin, flexible, lighted scope (hysteroscope) into your vagina and your cervix into your uterus. The hysteroscopy allows your doctor to examine the inside of your uterus.
- Endometrial biopsy. Your doctor may use a suction catheter inside the uterus to collect a sample for a lab test. Uterine polyps can be confirmed by an endometrial biopsy, but the biopsy can also miss the polyp.
Most uterine polyps are non-cancerous (benign). However, some precancerous changes in the uterus (endometrial hyperplasia) or cancers of the uterus (endometrial carcinomas) appear as uterine polyps. Your doctor will likely recommend the removal of the polyp and send a tissue sample for lab analysis to make sure you don't have uterine cancer.
Medical treatments
For uterine polyps, your doctor may recommend:
- Watchful waiting. Small polyps without symptoms can resolve on their own. Treating small polyps is unnecessary unless you are at risk for uterine cancer.
- Medicines. Certain hormonal drugs, including progestins and gonadotropin-releasing hormone agonists, can alleviate symptoms of the polyp. But taking such medications is usually a short-term solution at best - symptoms usually return once you stop taking the medication.
- Surgical removal. It is a surgical intervention which allows one to treat certain pathologies of the uterine cavity by natural means. The operation is carried out using a camera called a hysteroscope (measuring 10 mm in diameter), into which the surgical instruments are inserted. This intervention is performed in the operating room, under general anesthesia or under locoregional anesthesia (epidural analgesia or spinal anesthesia).
As part of an infertility assessment or treatment, laparoscopy may be combined with operative hysteroscopy. It allows the exploration of the entire female pelvis, the verification of the patency of the uterine tubes and the performance of other possible associated procedures.
When is an operative hysteroscopy performed?
The intervention is performed outside of the period, in the first part of the cycle. In a premenopausal woman, the ideal time is between D-8 and D-13 of the cycle (D-1 being the first day on which the rules begin). This is the only time when we are sure that there is no early pregnancy. In this phase of the cycle, the endometrium is thin and the lesion is better visible. In postmenopausal women, the operation can be performed at any time, preferably outside the bleeding period and sometimes after prior preparation with estrogen for 10 days or with prostaglandins, in order to facilitate the dilation of the cervix. There is no other special preparation before the operative hysteroscopy.
How is an operative hysteroscopy performed?
An operative hysteroscopy can be performed under locoregional anesthesia (epidural or spinal anesthesia) or under general anesthesia. The choice of the type of anesthesia is fixed in a pre-anesthetic consultation. An operative hysteroscopy is usually done on an “outpatient” basis. The patient returns in the morning, on an empty stomach, then leaves accompanied a few hours after the end of the operation. In some cases, hospitalization of 24 to 48 hours is necessary. The intervention is performed by a gynecologist-surgeon. It is carried out by natural means. There is therefore no visible external scar. The operation itself begins with progressive dilation of the uterine cervix using metal candles (prior treatment with tablets administered vaginally is often prescribed to facilitate this gesture).
The hysteroscope is introduced into the uterine cavity. Permanent irrigation throughout the operation with a special liquid (Glycocolle) allows the distension and visualization of the uterine cavity. A special system allows the control of the pressures and a balance of the inputs and outputs of the liquid. The hysteroscope is connected to a video screen that the surgeon observes throughout the operation in order to adapt his gestures. Surgical instruments are introduced into the hysteroscope tube (scissors, resection loop, section hook, ball, etc.).
When an intrauterine lesion is removed, the resection shavings are sent to the pathology laboratory for histological tissue analysis. The results are communicated to the patient by the gynecologist during a post-operative consultation, at the same time as the operative report.
What are the risks?
Like every surgical procedure, operative hysteroscopy involves certain risks:
- Persistence of small bleeding for several days is usual;
- Risk of hemorrhage, occurring immediately postoperatively or remotely (in the days following the operation). It may be related to a tear in the cervix or a uterine perforation. The occurrence of bleeding may require further intervention;
- Risk of infection, manifested by smelly vaginal discharge, pelvic pain and fever, urinary tract infection;
- Failure of the operation following a false route of the path of the hysteroscope against indicating the continuation of the operation;
- Very rarely, an operative hysteroscopy can cause infertility by obstruction of the uterine cervix (stenosis) or by the occurrence of postoperative synechia;
- Absence of periods, by stenosis (obstruction) of the uterine cervix or by the appearance of a synechia, which may require dilation or reoperation;
- Cervico-isthmic open bite linked to the dilation of the uterine cervix;
- Risks associated with anesthesia: allergy, infection…;
- Exceptionally, an intestinal or urinary system wound, linked to a uterine perforation;
- Neurological damage linked to an important intravascular passage of the irrigation liquid (Glycocolle): headaches, visual disturbances, respiratory and cardiovascular disorders, hyponatremia, and hemodilution.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: https://wa.me/22996374527
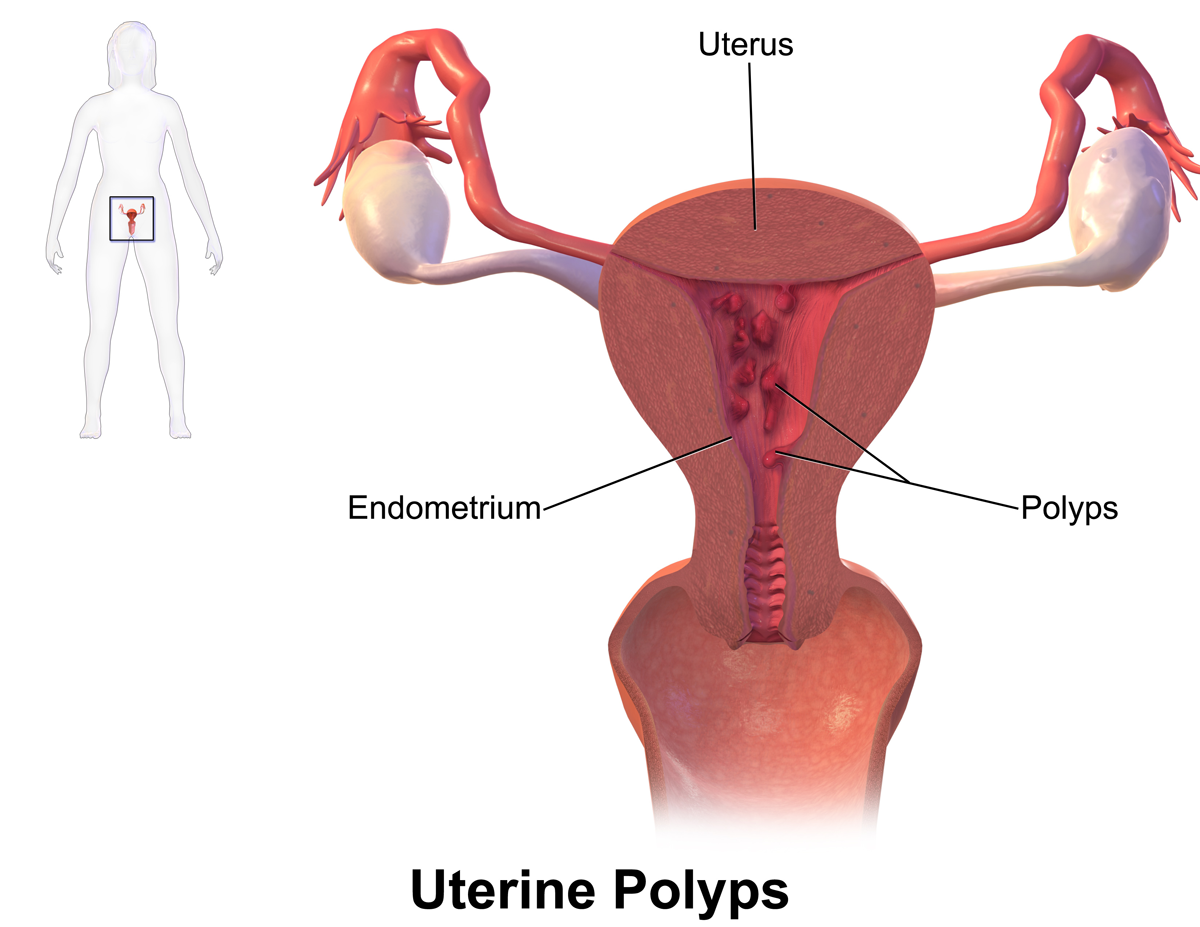
SYMPTOMS OF UTERINE POLYPs: Natural treatment
WHAT ARE THE SIGNS OF UTERINE POLYPS?

Uterine polyps are stressful news for any woman. They can cause a negative experience and discomfort. They are not cancerous, at least for the most part they are not. To what extent they still endanger health is a question whose exact answer can only be heard in the doctor's office.
Uterine polyps come in different sizes and are attached to the wall of the uterus. They are single or in a group of several. They are likely to occur at a young age but are more common in women before and during menopause.
Uterine growths are sensitive to estrogen and the most likely causes are hormonal changes. Among the risk factors for them are overweight, high blood pressure, and some drugs for breast cancer.
HERBAL TREATMENT FOR UTERINE POLYPS
The causes of this disease can be different, and tumors appear in young girls and older women. If the doctor put such a diagnosis - do not despair. There are ways not only with medication, you can still treat uterine polyps with an herbal remedy. Both methods are effective in killing polyps and preventing new ones. A woman can choose the most suitable treatment option for yourself, depending on the characteristics of her body.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: https://wa.me/22996374527
Symptoms of uterine polyps
The truth is that they are mostly found during random examinations by a gynecologist. This is not due to negligence or ignorance on the part of the ladies, but only because these polyps form asymptomatically. Doubt about their locality is caused mainly by:
- Irregular menstrual flows. They appear at no time and last indefinitely.
- Spots between periods. They are not exactly a monthly flow, but rather spots left by one.
- Prolonged menstruation. Significant lengthening of the menses for no apparent reason.
The most popular recipes against uterine polyps

Consider effective and easy-to-prepare folk remedies that will help treat uterine polyps without surgery and without significant obstruction to the body.
Herbal extract for regular intake
To prepare the soup, you will need 1 teaspoon black currant fruit, 3 teaspoons cinnamon wild rose fruit, 2 teaspoons of dioica nettle leaves.
Currants, rose hips, and nettle bloomery should be mixed and grind well.
Then take a tablespoon of the resulting mixture and pour two cups of boiling water.
Giving to run for an hour and filter through cheesecloth (during which time the infusion will gain almost room temperature).
If the taste is too bitter, you can add a little sugar - it does not affect the properties of the soup. It should be taken 4 times a day at any time by drinking half a glass. This recipe is a great help in treating cervical polyp.
Herbal decoction for douching
Endometrial surface polyps arise for various reasons, one of which is a violation of the natural hormonal balance against the background of nutrient deficiency. It is this situation that can be corrected by applying a decoction.
Should be used if there are vaginal cords.
To prepare the need: 2 tablespoons herb yarrow ordinary, 2 tablespoons rosemary leaves, 2 tablespoons sage leaves drug, 4 tablespoons plain oak bark.
All these components should be well ground and mixed in an enamel bowl. Then, pour boiling water volume of 2.5 liters and bring it to a boil.
Boil the broth need about half an hour, then cool - always at room temperature. When the broth itself reaches room temperature, it is necessary to filter through a fine sieve or gauze. Then it can be used for vaginal douching, the procedure is repeated twice a day. also the effective herbal treatment of uterine fibroids - Another annoying problem.
Effective folk remedy against uterine polyps
For the treatment of uterine polyps folk remedies it is possible as an operative or homeopathic way, and with the help of folk remedies, even if the symptoms are strong enough. Use this decoction should be in the presence of heavy and persistent vaginal cords.
To prepare the decoction, you will need to collect: 3 tablespoons of dioica nettle leaves, 5 tablespoons herb knotweed, 1 tablespoon chamomile, 1 tablespoon of ordinary oak bark.
You need to carefully grind and mix well all the ingredients. Then take two tablespoons of the resulting mixture, put in an enamel pan, and fill it with 1 liter of boiling water.
Decoction boil for 5 minutes on low heat, then leaves to cool to room temperature.
When the broth has cooled, strain it through a fine sieve or cheesecloth. The resulting mixture can be used for vaginal douching. For effective enough to use it at least twice a day.
Experience has shown that the use of this decoction can eliminate endometrial polyp without surgery.
Recipe based on celandine
Particularly effective since ancient times is considered the treatment of uterine polyps greater celandine. The more you can use it not only for sprintsevalnyh solutions but also for oral administration.
However, it should be remembered that before taking such funds it is necessary to consult with your doctor.
The same recipe is very simple.
We need to a quart a jar and fill it with fresh grass celandine.
Then you need to pour boiling water over the grass.
The bank is not broken, it is best to warm up before preparing the solution.
Cover the dish with a warm scarf and it will leave in a few hours.
Then, the mixture is ready, and it can be used for regular swallowing.
It should be taken three times a day. We must start with very small portions (about 1 teaspoon) and then gradually increase the dose by the end of the second week from one serving to 100 milliliters.
A two-week course can be effective enough to eliminate appearing polyp in the uterus.
Sometimes, of course, it is not enough, and you will have to repeat it. But before the infusion of celandine again, you need to rest for not less than two weeks.
It is also useful for uterine propolis, for example, candles for uterine fibroids from propolis are useful for healing.
As is the case with other folk remedies for the treatment of uterine polyps, be sure to remember that the infusion of celandine - is not a cure. And polyps, regardless of their origin, require medical supervision. However, to engage with homeopathy, and especially immediately agree to surgery should not be in any case - because your body must protect itself and carry out its treatment should be as painless as possible means.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: https://wa.me/22996374527
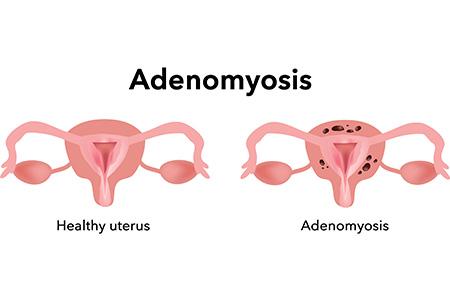
ADENOMYOSIS NATURAL TREATMENT
We talk about adenomyosis when the tissue that normally lines the uterus (the endometrium) grows in the muscular wall of the uterus. Adenomyosis can cause menstrual cramps, low abdominal pressure, and bloating before your period and can lead to heavy periods. It is even responsible in some cases of infertility in women. Here is the natural herbal treatment from Dawasanté experts to treat adenomyosis. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Adenomyosis is most common in women who have had several children.
If you have adenomyosis and want to avoid the operation at all costs, you have come to the right place. Here we offer you a natural remedy made from medicinal plants very effective to permanently cure adenomyosis. It is specially designed for patients who do not want to have surgery because every operation carries a risk.
Natural treatment
The natural treatment that we offer to cure adenomyosis consists mainly of natural herbal teas. This natural herbal treatment for adenomyosis will remove the pain you feel during your period and allow you to have normal cycles. It outperforms conventional treatments that relieve pain, but don't get to the root of the pain. Our herbal tea contains plants that reduce the estrogen level in the blood. This helps block the proliferation and bleeding of adenomyosis lesions. These herbal remedies are rich in an antioxidant that inhibits the enzymes that lead to pro-inflammatory prostaglandins. These are nutrients in high doses anti-inflammatory. This will definitely put an end to the pain you feel during your period. We know that many of you have had adenomyosis treatment or surgery, but the pain returned years later. No panics ladies! With us, no recurrence, no side effects. You will be permanently cured of adenomyosis.
This natural herbal tea also facilitates cell multiplication relating to fertility, growth, healing and immunity; to the synthesis and secretion of many hormones. Thanks to these medicinal plants, you will avoid miscarriages. It is nature's secret to cure adenomyosis and get pregnant quickly.
Our natural remedy to treat adenomyosis very often gives positive results and acts significantly on the reduction of the pain felt. It has an efficiency rate of 98%. Trust us ladies and you will get pregnant once more.
To discover our natural remedy to cure Naboth cysts, click here
Symptoms
Sometimes adenomyosis does not cause any signs or symptoms or causes only mild discomfort. However, adenomyosis can cause:
-
Heavy or prolonged menstrual bleeding
-
Severe cramping or sharp, knife-like pelvic pain during menstruation (dysmenorrhea)
-
Chronic pelvic pain
The causes
The cause of adenomyosis is not known. There have been a lot of theories, including:
· Invasive tissue growth. Some experts believe that adenomyosis results from the direct invasion of endometrial cells through the lining of the uterus into the muscle that forms the walls of the uterus. Uterine incisions made during an operation such as a cesarean section could promote the direct invasion of endometrial cells into the lining of the uterus.
· Developmental origins. Other experts suspect that adenomyosis originates in the uterine muscle from endometrial tissue deposited there during the formation of the uterus in the fetus.
· Inflammation uterine is related to childbirth. Another theory suggests a link between adenomyosis and childbirth. Inflammation of the lining of the uterus during the postpartum period can cause the normal boundary of the cells that line the uterus to rupture. Surgery on the uterus can have a similar effect.
· Origin of stem cells. A recent theory suggests that stem cells from the bone marrow could invade the uterine muscle, causing adenomyosis.
Regardless of the course of adenomyosis, its growth depends on the circulation of estrogen in the female body.
Risk factors
Risk factors for adenomyosis include:
-
Previous uterine surgery, such as cesarean or fibroid removal
-
Childbirth
-
Middle Ages
Most cases of adenomyosis occur in women between the ages of 40 and 50. Adenomyosis in these women could be linked to longer exposure to estrogen compared to that in younger women. However, current research suggests that the condition might be common in younger women.
Complications
If you often have heavy and prolonged bleeding during your period, you can develop chronic anemia, which can lead to fatigue and other health problems.
While not harmful, the pain and excessive bleeding associated with adenomyosis can disrupt your lifestyle. You may be avoiding activities that you have done in the past because you are in pain or are worried about bleeding.
Diagnostic
Your doctor may suspect adenomyosis based on:
-
Signs and symptoms
-
A pelvic exam that reveals an enlarged and tender uterus
-
Ultrasound of the uterus
-
Magnetic resonance imaging (MRI) of the uterus
In some cases, your doctor may take a sample of uterine tissue (endometrial biopsy) to check that your abnormal uterine bleeding is not associated with another serious condition. But an endometrial biopsy will not help your doctor confirm the diagnosis of adenomyosis.
The only way to confirm adenomyosis is to examine the uterus after a hysterectomy. However, pelvic imaging such as ultrasound and MRI can detect signs of it.
Other uterine diseases can cause signs and symptoms similar to adenomyosis, making adenomyosis difficult to diagnose. The conditions include fibroids (leiomyomas), uterine cells growing outside the uterus (endometriosis), and growths in the lining of the womb (endometrial polyps).
Your doctor may conclude that you only have adenomyosis if you have chosen other possible causes of your signs and symptoms.
Medical treatments
Adenomyosis often goes away after menopause, so treatment may depend on how close you are to this stage of life.
Treatment options for adenomyosis include:
· Anti-inflammatory. Your doctor may recommend anti-inflammatory drugs, such as ibuprofen, to control the pain. By starting an anti-inflammatory medication one to two days before your period starts and taking it during your period, you can reduce menstrual blood flow and help relieve pain.
· Hormonal Drugs. Birth control pills that combine estrogen and progestins, patches containing hormones, or vaginal rings can reduce the heavy bleeding and pain associated with adenomyosis. Progestin-only contraception, such as an intrauterine device, or continuous-use birth control pills often lead to amenorrhea - the absence of periods - which may provide some relief.
· Hysterectomy. If your pain is severe and no other treatment has worked, your doctor may suggest surgery to remove your uterus. Removing your ovaries is not necessary to control adenomyosis.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
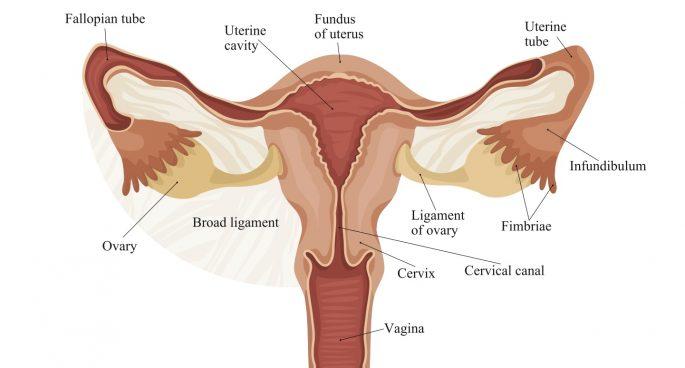
OBSTRUCTION OF FALLOPIAN TUBE: Natural treatment
Endometriosis is a common and painful disease that affects thousands of women around the world in North America as in Africa and South, other continent and is one of the three main causes of infertility in women.
During a normal menstrual cycle, the lining of your uterus - called the endometrium - begins to thicken before you become pregnant. If you don't get pregnant that month, your body loses its endometrium during your period and the process starts all over again. In endometriosis, for reasons that researchers don't fully understand, tissue very similar to the endometrium begins to grow outside the uterus in various places that it shouldn't. It can appear in or on the ovaries, fallopian tubes, the various structures that support the uterus and the lining of the pelvic cavity. Sometimes it is also found in other places, including the cervix, vagina, rectum, bladder, bowel and elsewhere.
The problem is, this tissue behaves like normal endometrial tissue - it builds up and breaks down with your menstrual cycle - but it can't shed like normal endometrial tissue during your period. As a result, unwanted tissue causes irritation and inflammation. This build-up of tissue can prevent the eggs from leaving the ovaries or from being fertilized by the sperm. It can also leave scars and block the fallopian tubes, preventing the meeting between the egg and the sperm.
Finally, endometriosis problems can be the cause of tubal obstruction. This is because pieces of the uterine lining can end up in the tubes or on the ovaries and block the progression of sperm to the egg, thus preventing fertilization. Dawasanté experts provide you with a natural herbal treatment to unblock your tubes and allow you to quickly get pregnant.
Click on the image below to discover this natural treatment.
However, obstruction of the fallopian tubes is a major cause of female infertility. The blocked fallopian tubes do not allow the egg and sperm to converge, making fertilization impossible. The fallopian tubes are also called oviducts, uterine tubes, and salpines (singular salpinx).
Tubal obstruction
About 20% of female infertility can be attributed to the causes of the tubes. occlusion of the distal tubes (affecting the tip towards the ovary) is usually associated with the formation of hydrosalpinx and is often caused by Chlamydia trachomatis. Pelvic adhesions can be associated with such an infection. In less severe forms, the fimbriae may be clumped and damaged, but some permeability may still be preserved. Tubal obstruction in the middle of the segment may be due to tubal ligation procedures, as this part of the tube is a common target for sterilization procedures. Proximal tubal occlusion can occur after infection, such as. In addition, some tubal sterilization procedures such as the Essure procedure target the part of the tube near the uterus.
A blockage of the uterine tubes can be caused by various disorders, and in some rare cases even be present from birth without causing symptoms until the desire to conceive a child. Obstruction of the fallopian tubes is very often involved in cases of female infertility.
There are various causes of obstruction, or even lesions, of the tubes:
- Pelvic infections;
- Use of an intrauterine device;
- Rupture of the appendix;
- Pelvic or lower abdominal surgery;
- Certain pathologies, for example, tuberculosis;
- Ectopic pregnancy in the fallopian tubes;
- Congenital malformations of the tubes;
- Uterine fibroma ;
- Endometriosis ;
- Asherman's syndrome (lesions or infections during surgery).
We speak of proximal tubal obstruction when the tubal isthmus is involved. It can follow an abortion, miscarriage, cesarean section, pelvic inflammatory disease or the contraceptive pill.
If the distal tubes are blocked, it is the end of the tube on the side of the ovary that is affected. This type of obstruction is often associated with a "hydrosalpinx" which refers to the abnormal presence of a pocket of fluid in the fallopian tube. Usually, hydrosalpinx is caused by infection with Chlamydia trachomatis (sexually transmitted infection).
In other cases, the ovarian fringes, which have an important role in the conduction of the oocyte in the tubes, are damaged or stick together.
Several elements are at the origin of this obstruction
GENITAL INFECTIONS
The majority of the causes of obstruction are infections of the genital tract, especially of the tubes ( salpingitis ) which have occurred in the past. Most of the time, they are due to sexually transmitted diseases (such as chlamydia), which may have gone unnoticed. Nevertheless, they were sufficient to block the proboscis and make it waterproof. This is why it is important for all women to prevent the risk of STDs, in particular through safe sex with occasional partners and regular gynecological monitoring.
MEMBERSHIP
Aside from infections, adhesions, where the two sides of the tube wall stick together, can also be present.
ENDOMETRIOSIS
Endometriosis problems may be the cause of obstruction of the fallopian tubes. This is because pieces of the uterine lining can end up in the tubes or on the ovaries and block the progression of sperm to the egg, thus preventing fertilization.
Most often, a catheter can become blocked due to an infection such as pelvic inflammatory disease (PID). The tubal infertility rate would be 12% after one, 23% after two and 53% after three episodes of PID. The fallopian tubes can also be blocked or disabled by endometritis, infections after childbirth, and intra-abdominal infections, including appendicitis and peritonitis. The formation of adhesions may not block a fallopian tube, but make it dysfunctional by deforming it or separating it from the ovary. It has been reported that women with distal tubal occlusion have a higher rate of HIV infection.
The fallopian tubes can be blocked as a method of birth control. In these situations, the tubes tend to be healthy and, in general, patients requesting the procedure had children. Tubal ligation is considered a permanent procedure.

NATURAL TREATMENT FOR CLOGGED FALLOPIAN TUBES
The fallopian tubes are muscle tubes lined with delicate hair-like structures. These “hairs” work in both directions; help egg travel from the ovaries to the uterus and help sperm come up from the uterus.
Each fallopian tube ends in fimbriae, which are finger-like structures. Fimbriae grab and guide an egg when the ovary releases it.
The fallopian tubes play an important role in conception because they are the place where most of the eggs are fertilized. If part of the fallopian tube is damaged, for example by surgery or an infection, it may be blocked with scar tissue.
The fallopian tubes blocked are one of the possible causes of female infertility. Usually, there are no symptoms, but certain risk factors can increase the risk of developing the disease. The medical term for a blocked fallopian tube is tubal occlusion. However, Dawasanté experts provide you with a natural herbal treatment to unblock the tubes without surgery, allowing you to quickly get pregnant.
Dawasante's natural treatment to unclog blocked fallopian tubes

What if I have blocked tubes and want to get pregnant?
Here is the best African herbal remedy for unblocking the tubes and getting pregnant quickly . These herbs are very effective at unblocking the fallopian tubes. They have already enabled many women around the world who had blocked tubes to regain their fertility without operations. If you have blocked tubes, here are the medicinal plants that will allow you to experience the joy of being a mother
Click on the image below to discover this natural treatment.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
What are the best natural treatment for unclogging your tubes?
Thanks to our research, we have identified several effective homemade natural remedies to unblock the tubes and get pregnant quickly in addition we have:
11 remèdes naturels contre les trompes bouchées
1-Turmeric

Turmeric is a natural anti-inflammatory. It can be very effective in unblocking the fallopian tubes. Curcumin, the active ingredient in turmeric is very effective in reducing inflammation. You can consume curcumin in supplement form, add turmeric to your food, or drink a glass of turmeric.
Turmeric has no known side effects when taken in small doses. However, at doses of more than 8 grams per day, it can have unwanted effects. Make sure you take the correct dosage of turmeric or, better yet, add the spice to your cooking.
2-Garlic

Garlic is a great way to improve fertility and unclog the fallopian tubes. Garlic has always been consumed for its many health benefits as the aphrodisiac properties present in garlic help to improve blood circulation in the body. Eating raw garlic daily on an empty stomach helps fight infertility in women, lowers blood pressure and cholesterol
3- Cleansing with a fertility diet

The fertility diet helps cleanse the entire reproductive system and increase blood flow to the reproductive organs. The herbs in this cleansing regimen are absorbed by the body and will work where they are needed. The fertility cleanse creates a "clean slate" in the body which helps the body respond better and use other natural remedies.
This fertility diet cleans up the food waste that you need to avoid and synthesizes more that you need. Foods that you should avoid are alcohol, cigarettes, non-organic meats and dairy products, processed foods, processed white seeds, white sugar, fried foods, soy foods.
When it comes to what you should eat, the following should be suitable for fertility cleansing:
- Eat all organic vegetables.
- Eat low amounts of dairy products and make sure the ones you eat are organic.
- Eat fish at least three times a week.
- All types of red meats are recommended.
- Avoid chicken or chicken products.
- Seeds are also highly recommended
- Consume foods with high enzymatic proportions
- Avoid all refined sugars or fruit juices (unless it is freshly squeezed).
- Drink plenty of clean water.
4- Castor oil

the castor oil has been used for centuries to enhance fertility in women, and in particular to unblock fallopian tubes. How is it used?
-dip a cloth in castor oil
-Place this cloth on the skin on the lower abdomen. This will improve circulation and promote healing of the tissues and organs under the skin. Castor oil therapy helps the fallopian tubes by softening tissue and improving circulation in the pelvic area.
5- Apple cider vinegar

Apple cider vinegar is a fermentation product that produces yeasts and bacteria that are beneficial for unblocking the tubes. This is because vinegar contains a number of vitamins and minerals, including magnesium, potassium, copper, group B vitamins, and vitamin C. Taken daily, it can help unblock the fallopian tubes by balancing hormones and shrinking fibroids.
Instructions for use:
-Mix 2 tablespoons of apple cider vinegar in 1 glass of water
-You can add a touch of honey or molasses to soften the mixture.
-You can drink the mixture right away or sip it for 30 minutes.
6-Meditation

Meditating daily will help lower stress levels and promote general healing. However, reducing stress reduces deterioration and inflammation of the fallopian tubes.
As an additional tip, don't forget to start meditating with a short session consisting of breathing exercises and relaxation techniques. Even if you only do it for a few minutes, meditation will provide you with positive energy to start your day and reduce your stress.
7- Fertility massage

Some alternative medicine practitioners suggest fertility massages to unblock the fallopian tubes. These usually involve hot oil massages on the abdominal area. How to do a fertility massage?
- Lie down on an exercise mat with your face up and a pillow under your lower back.
-Relax and apply almond, olive, or lavender oil to your hands and apply by massaging your pubic bone, as the uterus is below this bone.
-Gently massage from bottom to bottom and pull your abdominal wall towards the navel. Maintain this position, count to 10 and release your hands. Repeat this maneuver 10 to 20 times.
NB: Do not do this if you are bleeding or are pregnant. Also, if possible, visit a massage therapist who specializes in abdominal massage for best results.
8- Mugwort

Mugwort is a plant sometimes recommended to improve female fertility. It is also recommended for unblocking the fallopian tubes.
Mugwort has a long history of use for fertility in a number of different cultures. It has been used all over Europe and Asia for centuries. It is often used in Chinese medicine in the form of moxibustion, which involves burning a mugwort above an acupressure point.
9- Green clay

The use of green clay to unclog the proboscis is very common in East Africa.
The blocked tubes are released by the serious treatment of green clay and the follow-up of a feeding program made by a dietician or a naturotherapist.
10- Foods with antioxidants

Try to avoid things like meat from animals as they contain hormones that can affect a woman's hormones like estrogen. Replace them with foods rich in antioxidants to promote wound healing. Foods rich in antioxidants are:
- Fresh fruits, vegetables (all kinds)
- Vegetable oils like sunflower oil, coconut oil, olive oil.
- Tea, chocolate, soy, coffee, and cinnamon are high in flavonoids (a type of antioxidant).
- Carotenoids are plant enzymes that have antioxidant activity and can reduce the build-up of free radicals in the body. Carotenoids can be stored by consuming eggs, fruits and red-yellow vegetables like carrots, mangoes, peppers, papayas, citrus fruits, spinach, etc.
11-Stop drinking and smoking

The blockage of the fallopian tubes most often occurs when you are under excessive stress. So, you need to improve the quality of your life to be on track to naturally unblock the fallopian tubes.
Alcohol and smoking are considered to be primary factors for such illnesses and are important for relief by permanently giving up these habits. Not only will this action improve the conditions of the fallopian tubes, it will also improve the health of your body, nails, hair, teeth and even your skin.
If you are a regular smoker or an alcoholic, now is the time to start working out and quit altogether.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
CLOGGED FALLOPIAN TUBES AND FIBROIDS: Natural treatment
The fibroid uterine cancer are not common tumors (benign) of the uterus and are the most common reason for recommending a hysterectomy. They grow from the muscle wall of the uterus and are made up of muscle and fibrous tissue. Many women over the age of 35 have fibroids but usually have no symptoms. Fibroids can be the cause of blocked tubes. Here is a treatment to cure fibroids naturally and prevent blocked tubes. Click on the image below to discover this natural treatment.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
In some women, however, fibroids (myomas) can cause heavy bleeding, pelvic discomfort and pain, and occasionally put pressure on other organs. These symptoms may require treatment. Treatment may take the form of drugs to control pain and bleeding, hormone therapy to shrink the tumor, surgery to remove the tumor, or a hysterectomy. There are promising new investigational drugs that can temporarily shrink tumors. These drugs can have serious side effects and are usually very expensive. These treatments may be sufficient or provide temporary relief and allow a woman to delay a hysterectomy, especially if she still wants to have children. In more severe cases, a hysterectomy may be recommended.
Some women choose to do nothing because fibroids will often shrink in size as a woman goes through menopause.
As for the fallopian tubes, they are an essential organ of the female reproductive system. Measuring about ten centimeters each, these two ducts formed by smooth muscles and covered by the peritoneum connect the ovaries to the uterus. During ovulation, the oocyte expelled by the ovary is captured in the pinna, the terminal part of the proboscis, and moved to the ampulla, the central part of the duct. This is where fertilization by a sperm can take place. Then, for 3 to 4 days, the embryo develops in the tube, the time necessary for its transport to the uterine cavity.
There is a link between blocked tubes and fibroids
First of all, in case of blocked or damaged tubes, know that there are three reviews to explore their functionality.
- Hysterosalpingography
- Laparoscopy
- Fertiloscopy
Many interventions, however banal, can damage the tubes: an appendectomy, a gynecological surgery on the ovaries or the operation of a uterine fibroid.
It is indeed essential that the uterine cavity is strictly normal in order to restore fertility. When fibroids are in the uterine cavity, they should be removed by hysteroscopic resection. A 5 mm or more conventionally 9 mm resectoscope is used to cut them chip by chip. Fibroids located far from the uterine cavity are rarely responsible for infertility and do not require surgery. In case of blocked tubes, they will also have to be removed by an operating technique identical to that used for fibroids.
Also depending on the extent of the tumor and its location, uterine fibroids can put fertility at risk.
This is because the tumor can block the fallopian tubes, deform the uterine cavity, and prevent the implantation of the embryo. Under these conditions, a uterine fibroid makes pregnancy impossible.
Fibroids , being a benign tumor, the size of which can sometimes lead to complications during pregnancy. Perhaps the cause of the obstruction of the fallopian tubes
which can occur after salpingitis (inflammation of the tubes of infectious origin), and can prevent sperm from coming into contact with oocytes.
It is important to remember that the advantages of operative laparoscopy over conventional surgery are numerous. It makes it possible to avoid the opening of the abdominal cavity and therefore results in the absence of postoperative scar, with an obvious aesthetic interest for the woman.
In addition, the duration of hospitalization is shorter than in the context of conventional surgery. Finally, the postoperative period is more comfortable for the patient, and there is a faster resumption of activity with a lower number of postoperative sequelae.
Finally, it should be noted that certain surgical indications may be justified even when the couple also has recourse to In Vitro Fertilization (IVF) or IVF with ICSI (Intra Cytoplasmic Sperm Injection), in order to improve the chances of pregnancy.
The tube-shaped uterine tubes are used to receive the oocytes released every month from the ovaries and to transport them to the uterus. When the egg is expelled by the ovaries during ovulation, it is sucked in through the pinna of the tube. Fertilization (meeting between the egg and the sperm) takes place in the tubes, during the journey from the egg to the uterus. In order for a woman to get pregnant and have a baby, the tubes must be functioning normally and be intact (at least one!). In 15% of cases of fertility disorders, the causes are linked to an abnormality of the tubes.
The exact reasons why some women develop fibroids are unknown. Fibroids tend to grow in families, and affected women often have a family history of fibroids. Women of African descent are two to three times more likely to develop fibroids than women of other races.
The fibroids develop in response to stimulation by the hormone estrogen produced naturally in the body and are sometimes the cause of wrong bite thus preventing fertilization. These growths can appear as early as age 20 but tend to decrease after menopause when the body stops making large amounts of estrogen.
Fibroids can be tiny and not a problem, or they can weigh several pounds. Fibroids generally tend to grow slowly.
The following factors have been associated with the presence of fibroids:
- Being overweight, obese
- Never having given birth to a child (called nulliparity)
- The onset of menstruation before the age of 10
How do I know if my tubes are blocked
The obstruction in the tubes is often difficult to detect because there are few symptoms (possibly some abdominal pain or more abundant vaginal secretions). Consultations and analyzes are only carried out during the infertility assessment carried out when the woman who wants a child cannot get pregnant, after having had regular and unprotected sex for 1 year.
When the tubes are blocked, it will interfere with the movement and progression of the egg and sperm. Either the egg cannot meet the sperm (and there is no fertilization) or there is fertilization, but the egg cannot progress to the uterus.
When fertilization does not take place or remains impossible, the egg is automatically lost in the abdominal cavity. We are talking about tubal sterility.
If the obstruction is not complete, the fertilized egg will be able to circulate, but will have difficulty making its way to the uterus. The egg will then implant itself in the tube and develop into an ectopic pregnancy. At some point, the tube will rupture, causing internal bleeding.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
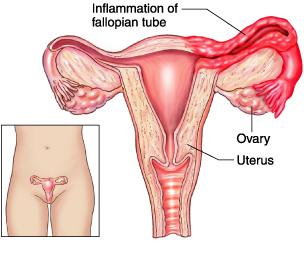
SALPINGITIS NATURAL TREATMENT
Salpingitis, what is this?
A PID is an infection of one or both fallopian tubes. A germ of sexually transmitted diseases is always responsible for the primary infection (gonococci and chlamydia especially), the infection by other pathogenic bacteria occurring only secondarily through the vaginal, blood, lymphatic or peritoneal route. However, Dawasanté experts have a natural herbal treatment for a tubal infection. Click on the image below to discover this natural treatment.
Thanks to our research, we have identified several natural home remedies that are very effective in unblocking the tubes and getting pregnant quickly. It is:
Turmeric is a natural anti-inflammatory. It can be very effective in unblocking the fallopian tubes. Curcumin, the active ingredient in turmeric, is very effective in reducing inflammation. You can consume curcumin in supplement form, add turmeric to your food, or drink a glass of turmeric.
Turmeric has no known side effects when taken in small doses. However, at doses of more than 8 grams per day, it can have unwanted effects. Make sure you take the correct dosage of turmeric or, better yet, add the spice to your cooking.
2-Garlic
Garlic is a great way to improve fertility and unclog fallopian tubes. Garlic has always been consumed for its many health benefits as the aphrodisiac properties present in garlic help in improving blood circulation in the body. Eating raw garlic every day on an empty stomach helps fight infertility in women, lowers blood pressure and cholesterol.
3- Vitamin C
Vitamin C is an antioxidant that can reduce inflammation by helping your immune system to function better. For this reason, it is ideal for healing scars and may have a positive effect on the fallopian tubes.
If you suspect that the cause of the blocked fallopian tubes is an infection, vitamin C can help you overcome it. To unclog your tubes, we recommend that you use natural vitamin C. It's easy to get vitamin C from food sources, especially when you like citrus fruits. Eat as many oranges, lemons, and grapefruit as possible. Aside from, you can try strawberries, broccoli and green peppers to heal yourself with a good vitamin C.
4- Castor
oil Castor oil has been used for centuries to improve fertility in women, and more especially to unblock the fallopian tubes. How is it used?
- dipped a rag in castor oil
-Place this cloth on the skin on the lower abdomen. This will improve circulation and promote healing of the tissues and organs under the skin. Castor oil therapy helps the fallopian tubes by softening tissue and improving circulation in the pelvic area.
5- Apple cider
vinegar Apple cider vinegar is a fermentation product that produces yeasts and bacteria that are beneficial for unblocking the tubes. This is because vinegar contains a number of vitamins and minerals, including magnesium, potassium, copper, group B vitamins, and vitamin C. Taken daily, it can help unblock the fallopian tubes by balancing hormones and shrinking fibroids.
Directions:
-Mix 2 tablespoons of apple cider vinegar in 1 glass of water
-You can add a touch of honey or molasses to soften the mixture.
-You can drink the mixture right away or sip it for 30 minutes.
6-Meditation
Meditating daily will help you decrease stress levels and promote general healing. However, reducing stress reduces deterioration and inflammation of the fallopian tubes.
As an additional tip, don't forget to start meditating with a short session consisting of breathing exercises and relaxation techniques. Even if you only do it for a few minutes, meditation will provide you with positive energy to start your day and reduce your stress.
7- Fertility massage
Some practitioners of alternative medicine suggest fertility massages unblock the fallopian tubes. These usually involve hot oil massages in the abdominal area. How to do a fertility massage?
- Lie down on an exercise mat with your face up and a pillow under your lower back.
-Relax and apply almond, olive, or lavender oil to your hands and apply by massaging your pubic bone, as the uterus is below this bone.
-Gently massage from bottom to bottom and pull your abdominal wall towards the navel. Maintain this position, count to 10 and release your hands. Repeat this maneuver 10 to 20 times.
NB: Do not do this if you are bleeding or are pregnant. Also, if possible, visit a massage therapist who specializes in abdominal massage for best results.
8- Mugwort
Mugwort is a plant sometimes recommended to improve female fertility. It is also recommended for unblocking the fallopian tubes.
Mugwort has a long history of use for fertility in a number of different cultures. It has been used all over Europe and Asia for centuries. It is often used in Chinese medicine in the form of moxibustion, which involves burning mugwort above an acupressure point.
9- Green clay
The use of green clay to unclog the proboscis is very common in East Africa.
The blocked tubes are unblocked by the serious treatment of green clay and the follow-up of a feeding program made by a dietician or a naturotherapist.
OVARIAN CYST OPERATIONS AND NATURAL TREATMENT
What are Ovarian Cysts
The ovarian cysts are sacs filled with fluid that can develop in or on your ovaries. Most ovarian cysts are harmless and go away on their own. But you may need to have an operation to remove a cyst if it is causing you pain or discomfort or if there is a chance that it is cancer.
Ovarian cysts are usually removed using a surgical procedure called laparoscopy (a type of keyhole surgery), but sometimes open surgery is necessary. Your procedure will be performed by a gynecologist.
Dawasante's natural treatment for ovarian cyst
If you have polycystic ovary syndrome and are looking for a natural treatment that will cure you and prevent you from having the operation, this is the natural treatment for you. We offer you an all-natural treatment to cure your Ovarian Cysts. It is therefore made up of three elements: herbal teas, a poultice, and vaginal eggs. It is an effective, fast and long-lasting natural remedy that allows cysts to be permanently removed. All elements of our treatment are natural and herbal. Then trust us! So this is the secret to curing ovarian cysts without surgery.
This natural herbal treatment for ovarian cysts has proven its effectiveness with dozens of resolved cases. This herbal tea is the miracle solution to permanently cure ovarian cysts.
To discover our treatment for ovarian cysts, click on the image below
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
Prepare for the removal of the ovarian cyst
You will get information from your hospital on how to prepare for your operation. If you smoke, for example, you will be asked to quit. Smoking increases your risk of getting an infection after surgery, which can slow your recovery. It can also lead to complications.
Ovarian cysts are usually removed with keyhole surgery as a daily procedure. This means you can probably go home the same day, although sometimes it is necessary to stay overnight.
Before you start, ask a friend or family member to take you home after your procedure. And make sure there can be someone home with you for the first 24 hours.
The operation is performed under general anesthesia, so you will sleep during the operation. You will be prompted to follow the fasting instructions. This usually means not to eat or drink anything other than clear fluids about six hours before your surgery. You can usually drink water for up to two hours before your surgery, but not after. It is important to follow the advice given by your hospital.
You may be asked to wear compression stockings to help prevent blood clots from forming in the veins in the legs.
Your gynecologist will discuss with you what will happen before, during, and after your procedure, including any pain, you may be feeling. If you are unsure of something, don't be afraid to ask. No question is too short. It is important that you feel fully informed so that you can give your consent to the procedure. You may be asked to do so by signing a consent form.
What are the alternatives to ovarian cyst removal?
If an ovarian cyst is not causing you any symptoms, your gynecologist may simply suggest that you monitor it rather than undergo treatment. You will need to attend regular appointments for an ultrasound to check if the cyst is clearing or changing in size. If you are under 50, most ovarian cysts will go away on their own within two to three months.
What Happens During Ovarian Cyst Removal?

Removal of the ovarian cyst is usually done through keyhole surgery, but sometimes a larger cut is needed (open surgery). Your gynecologist will discuss with you the type of operation best suited to your situation.
Read: Ovarian cyst and ginger, natural treatment
Keyhole surgery (laparoscopy)
Simple or small cysts can usually be removed with surgery. If you are having keyhole surgery, your gynecologist will make two or three small cuts (between 5mm and 1cm long). One will be near your belly button and two will be lower, usually one on each side. They will pass small instruments and a tube-shaped telescopic camera (called a laparoscope) through the cuts. This procedure is called laparoscopy. Your gynecologist will then examine your ovaries and remove the cyst. The cuts on your skin are closed with glue or stitches.
Open surgery (laparotomy)
In some situations, your gynecologist may need to perform open surgery. This is when a smaller, larger cut is made in your lower abdomen (tummy) to reach your ovary. Your gynecologist may recommend that you have open surgery if the cyst is very large or if it is possible that it is cancerous. Or, they may need to change the laparoscopy to open the surgery during the procedure in order to safely remove your cyst. In some circumstances, it may be necessary to remove your entire ovary during the procedure.
What to expect after
After your laparoscopy, your nurse will make sure you are not in pain and let you rest for a few hours. They will offer you something to eat and drink. You can usually go later in the day when you feel ready. Someone should take you home, and a friend or family member should stay with you overnight.
Your nurse will give you advice on how to treat your injuries before you go home. They will probably want to check that you can urinate properly before you go home, and will also give you painkillers to take. You may be given a date for a follow-up appointment.
Having general anesthesia affects everyone differently. You may find that you are not as well coordinated or that it is difficult to think clearly. It should pass within 24 hours. In the meantime, don't drive, drink alcohol, operate machinery, or sign anything important. Always follow the advice given by your gynecologist or the hospital.
If your gynecologist used soluble stitches, these will go away on their own. The other stitches may need to be removed by your GP's office nurse. It will usually be around five to seven days after your operation.
Recovery from ovarian cyst removal
Your body needs time to heal after surgery. Everyone is different. You may feel tired and need to take a nap for a few days after you get home.
But it is also important for your recovery that you stand up. Try to take a few short walks (10-15 minutes) in the first few days, then increase gradually. One week after the operation, most women can walk slowly and steadily for 60 minutes. After about two weeks, they returned to their normal level of physical activity. You should avoid heavy lifting for four weeks.
You will likely be able to return to work a week after the procedure, but this may depend on the type of work you are doing. It may take a week or more. The time it takes to recover will also be affected by whether you've had keyhole or open surgery. It takes longer to recover from open surgery. If you have questions about your recovery or when you can resume particular activities, ask your gynecologist. It is important to follow their advice.
If you need pain relief, you can take over-the-counter pain relievers such as paracetamol or ibuprofen.
Side effects of ovarian cyst removal
After your surgery, you may have side effects. These should be mostly temporary and can include:
-Pain or discomfort in the lower abdomen for a few days after your operation;
-Pain in the shoulders;
-A small amount of vaginal bleeding for up to 48 hours;
-Feeling more tired than usual for a few days
Complications of ovarian cyst removal
Complications arise when more serious and unexpected problems occur during or after your procedure.
Most women recover well after the removal of the ovarian cyst. Keyhole surgery causes fewer complications and has a shorter recovery time than open surgery.
Possible complications from any type of surgery include bleeding or a blood clot, usually in a vein in the leg (deep vein thrombosis - DVT). You could also develop an infection.
Removing the cyst from the ovary can damage other organs, such as the bowel, ureters or bladder, but this is unusual.
Your ovaries produce important hormones and eggs, which can be fertilized. Your gynecologist will try to preserve your ovaries so that your hormones are not affected and you can still have children, but this may not always be possible. Before your procedure, your gynecologist should discuss with you the risk of losing an ovary during the operation.
If you have any of the following symptoms, you should contact the hospital where you had your operation:
-Stomach pain that gets worse
-A high temperature, especially if you have also lost your appetite or are ill;
-Red or sore skin around your scars;
-Burning or tingling sensation when you urinate more often, or that you cannot do so at all;
-Pain, swelling, redness, or a feeling of heat on the legs.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
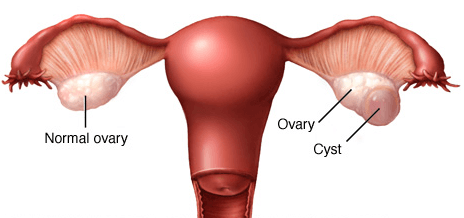
OVARIAN CYST AND PREGNANCY NATURAL TREATMENT
Ovarian cysts are sacs or pockets filled with fluid in an ovary or on its surface. Women have two ovaries; Each is the size and shape of an almond and is located on the side of the uterus. The ova (eggs), produced and ripe in the ovaries, are released in monthly cycles during fertile years.
Many women have ovarian cysts at some point. Most ovarian cysts do not present with much discomfort (or very little) and are not harmful. Most go away without treatment within a few months.
However, ovarian cysts (especially those that have ruptured) can cause severe symptoms. To protect your health, perform regular pelvic exams and familiarize yourself with symptoms that may indicate a problem that may be serious.
Dawasante's natural remedy for ovarian cysts
If you have polycystic ovary syndrome and are looking for a natural treatment that will cure you and prevent you from having the operation, this is the natural treatment for you. The herbal tea is made up of several herbs that regulate the hormone levels and the size of your cysts. Indeed, it contains several plants that will mimic the action of estrogen in your body. It is the best natural remedy for curing ovarian cysts. Usually, except when the diagnosis is too late, our natural treatment will cure ovarian cysts without side effects.
To discover our natural treatment for ovarian cysts, click here!!!
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
Symptoms that indicate an ovarian cyst
Most cysts don't cause any symptoms and go away on their own. However, a large ovarian cyst can cause:
-Pelvic pain: dull or severe pain in the lower abdomen on the side of the cyst;
-Feeling of fullness or heaviness in the abdomen;
-Swelling
The causes of ovarian cysts
Corpus luteum cyst
Most ovarian cysts occur after the menstrual cycle (functional cysts). Other types of cysts are much less common.
Functional cysts
Structures similar to cysts, called "follicles," usually develop every month. The follicles produce the hormones estrogen and progesterone and release an egg when you ovulate.
If a normal follicle continues to grow, it is called a “functional cyst”. There are two types of functional cysts:
· Follicular cyst Approximately in the middle of the menstrual cycle, an egg leaves its follicle and passes through the fallopian tube. A follicular cyst begins when the follicle does not break or release the egg, but continues to grow.
- Corpus luteum cyst. When a follicle releases the egg, it begins to produce estrogen and progesterone for conception. The follicle is now called the "corpus luteum". Sometimes fluid collects inside the follicle, which causes the corpus luteum to expand and a cyst to form.
Functional cysts are usually harmless, rarely cause pain, and usually go away on their own within two or three menstrual cycles.
Other cysts
Types of cysts that are not related to the normal functioning of the menstrual cycle are:
· Cyst dermoid. These cysts, also called "teratomas", can contain tissue, such as hair, skin or teeth, because they are formed from embryonic cells. They are usually not cancerous.
· Cystadenomas These form on the surface of an ovary and may be filled with a watery or mucous material.
· Endometriomas They are formed as a result of a disease in which uterine endometrial cells develop outside the uterus (endometriosis). Some tissue can adhere to the ovary and form a lump.
Dermoid cysts and cystadenomas may be enlarged, which can cause the ovary to move out of its position. This increases the possibility of a painful torsion of the ovary, called "ovarian torsion". Ovarian torsion can also cause blood flow to the ovary to decrease or stop. In fact, ovulation is the release of an egg from one of the ovaries. It usually occurs in the middle of the menstrual cycle, although the exact time may vary.
In preparation for ovulation, the uterine lining, or endometrium, thickens. The pituitary gland in the brain stimulates one of the ovaries to release an egg. The wall of the ovarian follicle breaks on the surface of the ovary. The egg is released.
Elongated structures called "fimbriae" carry the egg to the nearby fallopian tube. The egg travels through the fallopian tube, driven in part by contractions of the walls of the tube. Once in the fallopian tube, the egg can be fertilized by a sperm.
If the egg is fertilized, the egg and sperm join together and form a single-celled entity called a zygote. When the zygote moves down the fallopian tube into the uterus, it begins to divide rapidly and forms a group of cells called blastocysts, which looks like a small raspberry. When the zygote reaches the uterus, it is implanted in the uterine lining and pregnancy begins.
If the egg is not fertilized, the body simply reabsorbs it, perhaps even before reaching the uterus. About two weeks later, the lining of the uterus breaks off and is expelled through the vagina. This is called menstruation.
Risk factors
The risk of having an ovarian cyst increases due to:
· Hormonal problems: These include taking clomiphene (Clomid), a fertility medicine used to stimulate ovulation.
· Pregnancy: Sometimes the cyst that forms when you ovulate stays in the ovary throughout the pregnancy.
· Endometriosis: This condition causes uterine endometrial cells to grow outside the uterus. Some tissue can adhere to the ovary and form a lump.
· A severe pelvic infection: If the infection spreads to the ovaries, it can cause cysts to form.
· A previous ovarian cyst: If you have a cyst, you probably have more.
I have cysts and I'm pregnant… Is it time to panic?
Ovarian cysts are common in early pregnancy, even if you are not having your period. Usually, these cysts are harmless, just like most other ovarian cysts.
· However, if the cysts continue to grow throughout your pregnancy, there are a few possible problems. They can break, twist, or even cause problems during childbirth. This is one of the many reasons why it is important to stay under the care of an obstetrician/gynecologist during your pregnancy and throughout your life.
- If you have polycystic ovary syndrome you are at increased risk for gestational diabetes, pregnancy-induced high blood pressure, miscarriage or premature delivery.
· Talk to your OB / GYN about your risks and potential treatment options. She will provide you with a full set of options and recommend the best treatment to help you have the healthiest pregnancy possible.
Ovarian cysts: what consequences before pregnancy?
- Most of the time, having one or even more ovarian cysts does not prevent you from getting pregnant. Functional cysts do not really interfere with fertility (many women get pregnant naturally without even suspecting their presence) or only temporarily, while they resolve. For example, a follicular cyst can prevent ovulation during one cycle, but may not interfere with ovulation in the next cycle. In addition, if these cysts are slow to leave, hormonal treatment can accelerate their disappearance and return to a normal menstrual cycle with good ovulation.
- As for endometriosis and polycystic ovary syndrome, they can have a very small or greater impact on fertility depending on the severity of the disease: if necessary, treatment can be implemented to facilitate pregnancy. In general, large endometrial cysts are removed surgically while hormonal stimulation often helps to ovulate normally in polycystic ovary syndrome. Many women thus manage to become pregnant and carry on their pregnancy after these treatments.
Ovarian cysts: what consequences during pregnancy?
- It happens that an ovarian cyst is discovered accidentally, during a mandatory ultrasound during pregnancy. A small asymptomatic cyst often only requires simple monitoring, to make sure that it does not grow too large: normally, it will not interfere with the development of your future baby, or even your delivery.
- In the end, it is especially the cysts causing severe pain that must be removed surgically. The same can be said for very large ovarian cysts, which are often removed as a preventive measure (without treatment, a large cyst could trigger ovarian torsion). If this type of cyst is discovered during the very first months of your pregnancy, the operation will normally be postponed until the beginning of the second trimester: at this stage, it will no longer present any particular risks for your baby. In the meantime, the doctor may give you a rest.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527

OVARIAN CYSTS AND GINGER: Natural treatment
The ovarian cysts are sacs or fluid-filled sacs that develop in or on the surface of one or both ovaries of a woman. Most women will develop at least one cyst at some point in their life.
Dawasante's natural remedy for ovarian cyst
It is with the aim of remedying it and completely eradicating ovarian cysts that the health experts at Dawasante offer you natural herbal solutions. Click on the image below to discover this natural treatment. This natural herbal treatment for ovarian cysts has proven its effectiveness with dozens of resolved cases. This herbal tea is the miracle solution to permanently cure ovarian cysts. Indeed, it contains several plants that will mimic the action of estrogen in your body. Herbal tea is made up of several herbs that regulate the hormone levels and the size of your cysts. So this natural remedy will help you to relieve the pain of the menstrual cycle and regulate your cycle. The herbal tea will also expel waste from your uterus. Usually, except when the diagnosis is too late, our natural treatment will cure ovarian cysts without side effects.
To read more about our natural remedy and place an order, click here!
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
Symptoms of an ovarian cyst
Most ovarian cysts are considered functional, which means that they usually occur during the menstrual cycle and are not part of a disease process.
They are usually benign and for no apparent reason. Pathological cysts, on the other hand, can be either benign or cancerous.
Often people are unaware of ovarian cysts because they usually don't cause problems. However, in some cases, they can cause symptoms like abdominal bloating, pain during bowel movements, menstrual irregularities, pelvic pain before or during the menstrual cycle, pain during sex, pain in the lower back or thighs, pressure in the rectum or bladder, nausea, and vomiting. Certain types of ovarian cysts can also cause reduced fertility.
In many cases, ovarian cysts go away on their own within a few months. However, if they cause discomfort, there are many natural remedies that can help relieve symptoms and reduce the size of cysts.
Ginger and cysts
Ginger is a potent anti-inflammatory herb that reduces inflammation and relieves pain. Additionally, ginger increases heat in the body and induces menstruation.
Ginger juice still has its anti-inflammatory properties and it heals the joints. It reduces and with the passage of time the inflammation in the body completely ends. Small cysts can be removed completely with ginger juice.
Ginger tea is also a very effective natural remedy for natural relief of pain associated with ovarian cyst. It also has both antioxidant properties. Studies by Dawasante's experts have proven that ginger stops the growth of ovarian cysts.
How is it used? All you need to do is immerse the ginger tea bag in boiling water for a few minutes. If you don't like the taste, consider adding a squeeze of lemon.
How to make fresh ginger tea at home:

-Peel and cut a 2 inch piece of ginger.
-Boil the ginger in 2 cups of water for 10 minutes.
-Then remove from heat and add flavorings like lime juice and honey to taste.
Ginger has a strong aroma. This healthy herb can be used dried, powdered, fresh, in juice, oil or pickle form. Ginger has its own place in different cooking but apart from useful for dishes; it has many health benefits as well.
The health benefits of ginger
· Useful in suppressing allergic reaction.
· Useful in the treatment of stomach problems.
· Beneficial for treating loss of appetite.
· In the treatment of nausea useful caused by the treatment of cancer.
· Helps get rid of morning sickness.
· Useful in preventing vomiting and nausea after surgery.
· As well as beneficial in the treatment of stomach aches, colic, diarrhea and gas.
Nutritional values of ginger
Ginger is loaded with bioactive compounds and nutrients, which are very helpful for the brain and body. Ginger is rich sources of
· Beta carotene.
· Iron.
· Calcium.
· Silicon.
· Sodium.
· Magnesium.
· Potassium.
Vitamin A, B, E and B complex.
Here are some health benefits of ginger.
Certain conditions that ginger can help cure
Treat stomach pain
Ginger is rich in carminative properties which are really helpful in treating upset stomach. It helps prevent bloating and gas by relaxing the gastrointestinal muscles. It is well known for the treatment of diarrhea caused by bacteria. It is also useful in stomach alignment such as dyspepsia or colic. Dyspepsia is chronic in the digestion which results in feeling unwell in the upper part of the stomach.
It is therefore highly recommended to eat ginger after every meal in high quantity because studies reveal that ginger speeds up the process of emptying the stomach.
Helps prevent cancer
Cancer is a fatal disease resulting from the uncontrollable production of abnormal cells. Study reveals that ginger extract is considered an alternative treatment for different types of cancer. From colorectal cancer to ovarian cancer, ginger is very helpful.
The University of Minnesota study finds that ginger slows down the production of abnormal cells in colorectal cancer. Therefore prevent the nature cloning of cancer to produce abnormal cell to a large extent.
Ginger is also very useful in the treatment of skin, lungs, prostate, breast as well as pancreatic cancer.
Advice
· Adding ginger to your daily meal is a great way to keep cancer at bay.
Releasing Headaches
Ginger provides simple headache relief as well as migraine prevention through the synthesis of prostaglandin. Therefore helps to relieve pain in the blood vessels.
First method
· Take 3 tablespoons of powdered ginger.
· Add little water to make the paste.
· Apply the paste on the forehead.
· Repeat the steps whenever you feel headache and get relief.
Second method
· During the headache or migraine attack, having a cup of ginger tea would definitely minimize the pain.
InJoint pain relief from arthritis
Ginger has a rich property of anti-inflammatory so it revives in arthritis joint pain
First method
· Make a paste of turmeric and ginger powder.
· Apply to the affected area.
· Massage the area well.
· Follow this method twice a day.
Second method
· Apply a little ginger oil to the joints and muscles.
· Massage delicately.
· Add this method to your bath to relieve itchy joints and muscles.
Relieve menstrual pain
Ginger is a natural pain reliever. By eating ginger at the start of the menstrual period, women can feel relief from the symptoms of menstrual pain and difference.
First method
· Before the start of the menstrual period, at least four days before, add ginger to your daily meal.
Second method
· Take 1/4 piece of fresh ginger.
· Cut it into small slices.
· Boil a cup of water and add small slices of ginger in it.
· Boil for 2 minutes.
· Add a little honey or sugar.
· Switch off the stove.
· Drink ginger tea.
Third method
· Use ginger capsules.
These tested tips would be really helpful in relieving your menstrual period pain in women
Improve brain function and defend against Alzheimer's disease
Constant oxidative anxiety and inflammation can speed up the aging process. They are thought to be surrounded by the main drivers of Alzheimer's disease and age-related cognitive turn number down. Studies in animals have shown that the antioxidants and bioactive compound in ginger can slow down inflammatory reactions that take place in the brain. There are also some verifications that ginger can openly improve brain function. In a study of 60 middle-aged women, ginger extract was made public to gain better reaction time and functioning remembrance. There are also abundant studies in animals showing that ginger can save harm against age-related turn in the brain's role.
The vigorous ingredient in ginger can help fight infections
Gingerol, the bioactive material in fresh ginger, can be of help in reducing the threat of infections. In fact, ginger extract can curb the development of many different types of germs. It is very useful aligned with oral bacteria connected to inflammatory gum disease, the same as gingivitis and periodontitis. Brand new ginger can also be helpful in opposition to RSV virus, a regular cause of respiratory infections. Ginger helps perk up the immune structure. Consuming a small piece of ginger per day can help leaf possible danger of a stroke by retaining fatty deposit in the arteries. It also reduces bacterial infections in the abdomen, and helps fight a terrible cough and throat discomfort.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
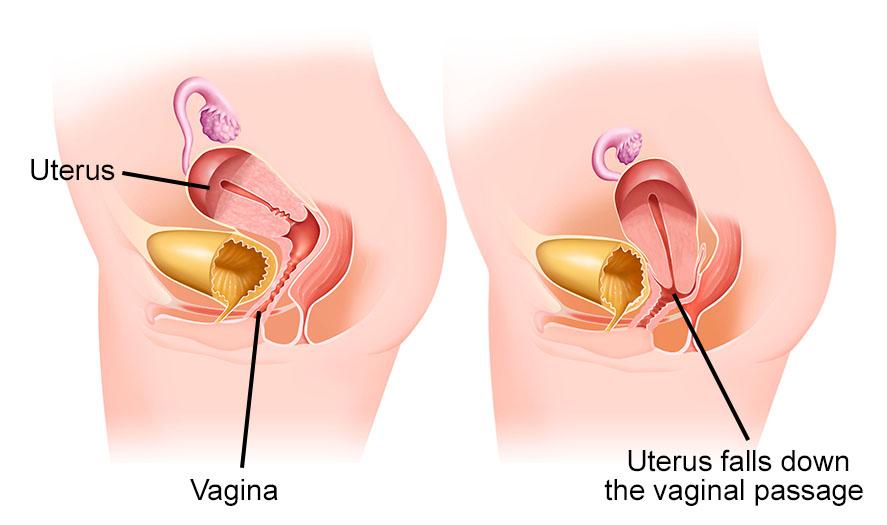
PROLAPSUS AND FOOD: The experts at Dawasanté