cure varicocele permanently
Blog / 94 results found
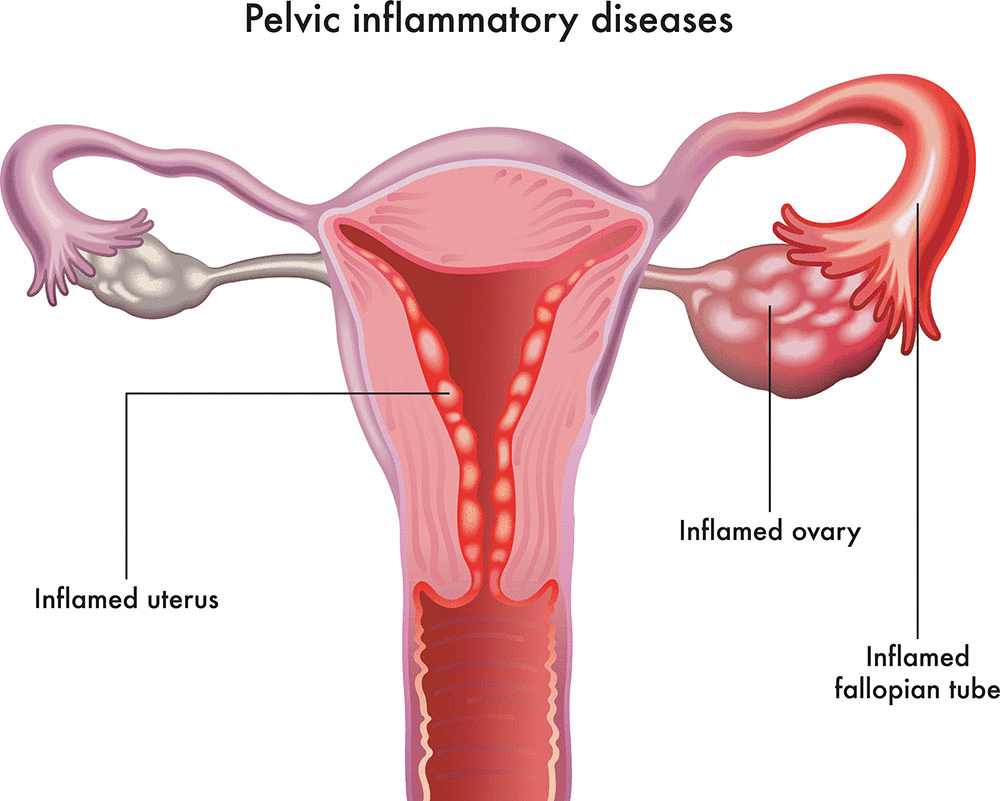
PELVIC INFLAMMATORY DISEASE
The pelvic inflammatory disease , or PID, is the term used for generalized inside infection of the uterus, fallopian tubes and ovaries. Symptoms of PID can include vaginal discharge, chronic pelvic pain, and fever. However, Dawasanté experts have available a treatment to remedy this disease. Click on the image below to discover this natural treatment
PELVIC INFLAMMATORY DISEASE
GENERALITY
Inflamed pelvic inflammatory disease fallopian tubes
Pelvic inflammatory disease (PID) is an infection of the reproductive organs of women. This usually happens when sexually transmitted bacteria spread from the vagina to the uterus, fallopian tubes, or ovaries.
If you suffer from pelvic inflammatory disease click here
Pelvic inflammatory disease often does not cause any signs or symptoms. As a result, you may not realize that you have the disease and get the treatment you need. The condition can be detected later if you are having trouble getting pregnant or if you develop chronic pelvic pain.
What if I have blocked tubes or PID and want to get pregnant?
Symptoms
The signs and symptoms of pelvic inflammatory disease can include:
Pain in the lower abdomen and pelvis
Heavy vaginal discharge with an unpleasant odor
Abnormal uterine bleeding, especially during or after sex, or between menstrual cycles
Pain or bleeding during sex
Fever, sometimes with chills
Painful or difficult urination
The MIP can cause only mild signs and symptoms, if any. When severe, PID can cause fever, chills, severe abdominal or pelvic pain - especially during a pelvic exam - and bowel discomfort.
When to see a doctor
See your doctor or seek urgent medical attention if you have:
Severe pain in the abdomen
Nausea and vomiting, with an inability to keep anything
Fever, with a temperature over 101 F (38.3 C)
Vaginal discharge
If your signs and symptoms persist but are not serious, see your doctor as soon as possible. A discharge from the vagina with an odor, painful urination, or bleeding between menstrual cycles may be associated with a sexually transmitted infection (STI). If these signs and symptoms appear, stop having sex and see your doctor soon. Prompt treatment of an STI can help prevent PIDs.
The causes
Many types of bacteria can cause PIDs , but gonorrhea or chlamydia infections are the most common. These bacteria are usually acquired through unprotected sex. Less commonly, bacteria can enter your reproductive tract whenever the normal barrier created by the cervix is disrupted. This can happen after childbirth, miscarriage, or abortion.
Risk factors
A number of factors can increase your risk for pelvic inflammatory disease, including:
Be a sexually active woman under 25
Having multiple sexual partners
Being in a sexual relationship with someone who has more than one sexual partner
Having sex without a condom
Showering regularly, which upsets the balance of beneficial and harmful bacteria in the vagina and may mask symptoms
Having a history of pelvic inflammatory disease or sexually transmitted infection
Most experts now agree that an inserted intrauterine device (IUD) does not increase the risk of pelvic inflammatory disease. Any potential risk is usually within the first three weeks after insertion.
Complications
Untreated pelvic inflammatory disease can cause scar tissue. You could also develop collections of infected fluid (abscess) in the fallopian tubes, which could damage your reproductive organs.
Other complications can include:
Ectopic pregnancy. The PID is a major cause of tubal pregnancy (ectopic). In an ectopic pregnancy, the scar tissue from the PID prevents the fertilized egg from making its way through the fallopian tube to implant in the uterus. Ectopic pregnancies can cause massive, life-threatening bleeding, and require urgent medical attention.
Infertility. PID can damage your reproductive organs and cause infertility - the inability to get pregnant. The more PID you have had, the greater your risk of infertility. Delaying treatment for PIDs also greatly increases your risk of infertility.
Chronic pelvic pain. Pelvic inflammatory disease can cause pelvic pain that can last for months or even years. The scarring in the fallopian tubes and other pelvic organs can cause pain during intercourse and ovulation.
Tubo-ovarian abscess. The MIP can cause the formation of an abscess - a collection of pus - in the fallopian tube and ovaries. If left untreated, you could develop a life-threatening infection.
Prevention
To reduce your risk of pelvic inflammatory disease:
Practice safe sex. Use condoms every time you have sex, limit the number of partners, and ask about a potential partner's sexual history.
Talk to your doctor about contraception. Many forms of contraception do not protect against the development of PID . Using barrier methods, such as a condom, can help reduce your risk. Even if you are taking birth control pills, it is still important to use a condom every time you have sex to protect yourself from STIs.
Have it tested. If you're at risk of getting an STI, such as chlamydia, make an appointment with your doctor for a screening test. Establish a regular screening schedule with your doctor if necessary. Treating an STI early gives you the best chance of avoiding PID.
Request that your partner be tested. If you have pelvic inflammatory disease or an STI, ask your partner for a screening test and, if necessary, treatment. This can prevent the spread of STIs and the possible recurrence of PIDs .
Pelvic inflammatory disease is a polymicrobial infection of the female genital tract: cervix, uterus, fallopian tubes, and ovaries; an abscess can form. Pelvic inflammatory disease can be sexually transmitted. Symptoms usually include abdominopelvic pain, cervical discharge, and irregular bleeding. Long-term complications include infertility, chronic pelvic pain, and ectopic pregnancy. Diagnosis is made by PCR of cervical swabs for Neisseria gonorrhoeae and Chlamydia, microscopic examination of cervical discharge (usually), and ultrasound or laparoscopy (sometimes). Treatment is based on antibiotics.
Pelvic inflammatory disease can affect the cervix, uterus, fallopian tubes, and / or ovaries. Infection of the cervix ( cervicitis ) causes mucopurulent discharge. Infections of the fallopian tubes (salpingitis), uterus (endometritis), and ovaries (oophoritis) tend to occur at the same time. If severe, the infection can spread to the ovaries (oophoritis) and then to the peritoneum (peritonitis). Salpingitis with endometritis and oophoritis, with or without peritonitis, is often called salpingitis, although other structures are involved. Pus may collect in the tubes (pyosalpinx) and an abscess may form (tubo-ovarian abscess).
Etiology
Pelvic inflammatory disease is caused by an overgrowth of organisms that originate from the vagina and cervix and travel up into the uterus and fallopian tubes. Neisseria gonorrhoeae and Chlamydia trachomatis are common causes of pelvic inflammatory disease; they are sexually transmitted. Mycoplasma genitalium , which is also transmitted sexually, can also cause or contribute to pelvic inflammatory disease. The incidence of sexually transmitted inflammatory pelvic disease is decreasing; to <50% of patients who have a positive acute pelvic inflammatory disease test for gonorrhea or chlamydia infection.
Pelvic inflammatory disease usually also involves other aerobic and anaerobic bacteria, including bacterial vaginitis pathogens . Vaginal organisms such as Haemophilus influenzae , Streptococcus agalactiae , enteric gram-negative bacilli may be involved in pelvic inflammatory disease, as well as Ureaplasma sp. Vaginal inflammation and bacterial vaginosis contribute to the upward spread of vaginal organisms.
Risk factors
Pelvic inflammatory disease is seen in women <35 years old. It is rare before the first period, after menopause and during pregnancy.
Risk factors include
-
History of pelvic inflammatory disease
-
Presence of bacterial vaginitis or any sexually transmitted infection
Other risk factors, especially for pelvic inflammatory gonococcal disease or Chlamydia, include
-
Young age
-
Non-white race
-
Low socioeconomic status
-
Multiple or new sex partners
-
Vaginal irrigations
Symptomatology
Abdomino-pelvic pain, fever, leucorrhoea and functional menometrorrhagia are common, especially during or after menstruation.
Cervicitis
In cervicitis, the cervix is red and bleeds easily. Mucopurulent leucorrhoea are frequent; usually they are yellow-green and can be seen draining from the endocervical canal.
Acute salpingitis
Abdomino-pelvic pain is usually present and bilateral but can be unilateral, even if both tubes are affected. Pain can also be felt in the upper abdomen. Nausea and vomiting are common when the pain is severe. Metrorrhagia (caused by endometritis) and fever appear in up to 1/3 of patients.
In the early stages, symptoms may be mild or absent. Later, sensitivity to cervical mobilization, muscle defense and increased decompression pain are common.
Sometimes dyspareunia or dysuria are observed.
Many women with inflammation severe enough to cause scarring have little or no symptoms.
Pelvic inflammatory disease caused by N. gonorrhoeae is usually more acute and causes more severe symptoms than that caused by C. trachomatis , which can be indolent. Pelvic inflammatory disease caused by M. genitalium , like that caused by C. trachomatis , is also mild and should be considered in women who do not respond to first-line therapy for pelvic inflammatory disease.
Complications
The Fitz-Hugh-Curtis syndrome (périhépatite causing pain right upper quadrant) can result from pelvic inflammatory disease gonorrhea or chlamydia. The infection can become chronic, with exacerbations and intermittent remissions.
A tubo-ovarian abscess (collection of pus in the appendages) develops in about 15% of women who have salpingitis. It can accompany an acute or chronic infection and is more likely in the event of treatment delay or incomplete treatment. Pain, fever, and peritoneal symptoms are usually present and can be severe. An adnexal mass may be palpable, although extreme pain may limit the possibilities for examination. The abscess can rupture, causing progressively severe symptoms and sometimes septic shock.
The hydrosalpinges (distension fluid by tubal obstruction flag of tubes) is usually asymptomatic, but may be responsible for pelvic gravity, chronic pelvic pain or dyspareunia and / or infertility.
Salpingitis can lead to scarring and adhesion of the tubes, which often results in chronic pelvic pain, infertility, and an increased risk of ectopic pregnancy.
Diagnostic
-
Strong suspicion
-
PCB
-
Pregnancy test
Pelvic inflammatory disease is suspected when women of childbearing age, especially those with risk factors, have lower abdominal pain or unexplained cervical or vaginal discharge. Pelvic inflammatory disease is suggested when irregular bleeding, dyspareunia, or dysuria remains unexplained. Pelvic inflammatory disease is more likely in cases of abdomino-pelvic pain, unilateral or bilateral adnexal pain, and pain when the cervix is mobilized. A palpable adnexal mass suggests a tubo-ovarian abscess. A pauci-symptomatic infection can leave serious consequences, caution must be exercised.
If pelvic inflammatory disease is suspected, cervical swabs analyzed by PCR for N. gonorrhoeae and C. trachomatis (with sensitivity and specificity of approximately 99%) and a pregnancy test is performed. If PCR is not available, cultures are performed. However, infection of the upper tract is possible even with negative cervical swabs. At this time, the cervical discharge is usually examined to confirm the presence of pus; a Gram stain or an examination on a wet mount under physiological serum is carried out but these examinations are neither sensitive nor specific.
If a patient cannot be seen because of pain, an ultrasound is done as soon as possible.
The white blood cell count may be high but is not helpful for diagnosis.
If the pregnancy test is positive, an ectopic pregnancy, which may cause similar symptoms, should be considered.
Other common causes of pelvic pain include endometriosis, adnexal torsion, ruptured ovarian cyst, and appendicitis. The signs that differentiate these disorders are discussed elsewhere ( Pelvic pain ).
Fitz-Hugh-Curtis syndrome can resemble acute cholecystitis but can usually be differentiated by finding salpingitis during pelvic examination and, if necessary, on ultrasound.
If an adnexal or pelvic mass is suspected clinically or if a patient does not respond to antibiotics within 48 to 72 h, ultrasound is done as soon as possible to rule out tubo-ovarian abscess, pyosalpinx and unrelated disorders. pelvic inflammatory disease (eg, ectopic pregnancy , adnexal torsion ).
If the diagnosis is uncertain after ultrasound, a laparoscopy should be performed; purulent peritoneal fluid observed laparoscopically is the gold standard for diagnosis.
Treatment
-
Antibiotics to cover N. gonorrhoeae , C. trachomatis , and sometimes other organisms
Antibiotics are administered empirically to cover N. gonorrhoeae and C. trachomatis and are secondarily adjusted to the results of the antibiogram. Empiric treatment is necessary whenever the diagnosis is in question for several reasons:
-
Tests (especially bedside tests) are inconclusive.
-
Diagnosis based on clinical criteria may be imprecise.
-
Failure to treat mildly symptomatic pelvic inflammatory disease can lead to serious complications.
Hospitalization of the patient with cervicitis or clinically mild to moderate pelvic inflammatory disease is not necessary. The outpatient treatment protocol aims ( Protocols for the treatment of pelvic inflammatory diseases * ) usually also to eradicate bacterial vaginitis , which often coexists.
Sexual partners of patients infected with N. gonorrhoeae or C. trachomatis should be treated.
If patients do not improve after treatment that covers the usual pathogens, pelvic inflammatory disease due to M. genitalium should be considered. Patients can be treated empirically with moxifloxacin 400 mg po once / day for 7 to 14 days (eg, for 10 days).
Women with pelvic inflammatory disease are usually hospitalized if any of the following signs are present:
-
Uncertain diagnosis, with inability to rule out a disorder requiring surgical treatment (eg, appendicitis)
-
Pregnancy
-
Severe symptoms or a high fever
-
Tubo-ovarian abscess
-
Inability to tolerate or follow outpatient treatment (eg, due to vomiting)
-
Lack of response to outpatient (oral) treatment
In these cases, IV antibiotics ( Treatment protocols for pelvic inflammatory diseases * ) are started as soon as the bacteriological samples are taken and are continued until the patient is afebrile for 24 h.
The tubo-ovarian abscess may require a more prolonged IV antibiotic therapy. Treatment with transvaginal or percutaneous drainage guided by ultrasound ultrasound or CT may be considered if the response to antibiotics alone is incomplete. Sometimes a laparoscopy or a laparotomy is necessary for drainage. If a ruptured tubo-ovarian abscess is suspected, immediate laparotomy is necessary. In women of childbearing age, surgery should be aimed at preserving the pelvic organs (in the hope of preserving fertility).
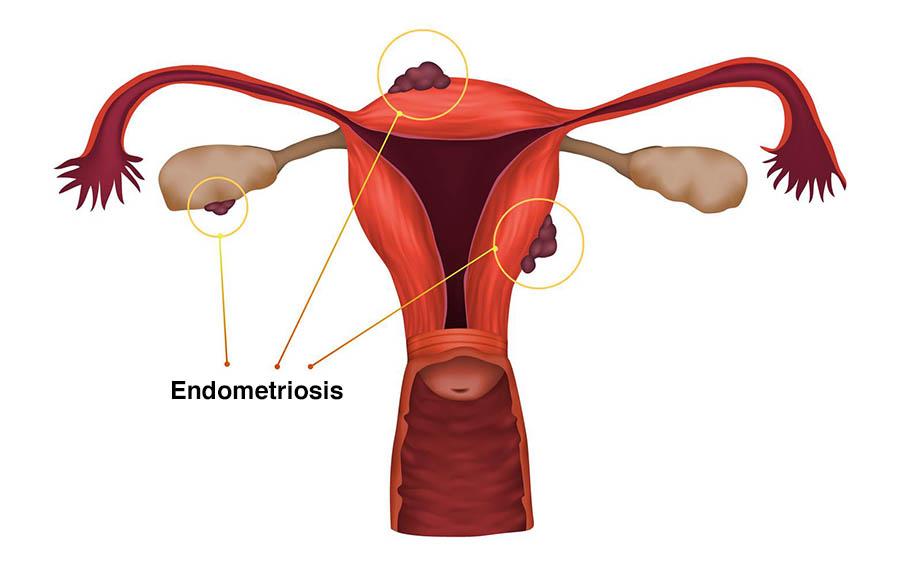
ENDOMETRIOSIS TREATMENT REGIME: Natural treatment
Endometriosis is a gynecological disease that affects one woman out of 10. It is characterized by the development, outside the uterine cavity, similar fabric to that of the lining of the uterus (called the endometrium). It potentially affects all regulated women.
One of the body's defenses, when it is attacked, is to trigger acute inflammation, the first characteristic symptom of which is pain. However, Dawasanté experts provide you with a natural herbal treatment to treat your endometriosis. and allow you to quickly design. Click on the image below to discover this natural treatment.
The inflammation is in this case the consequence of an attack on the organism. In the case of chronic inflammation, inflammation is a disease in itself, which can occur in any organ of the body and which is the cause of pathologies such as endometriosis.
What is endometriosis?
Endometriosis is a chronic inflammatory disease characterized by severe pain and bleeding outside the uterus during menstruation. This bleeding will be the cause of the inflammation. The more endometrial tissue spreads to other organs, the more inflammation spreads. The complexity of this disease is that it is multifactorial. But if it is impossible to know the precise causes, the factors that maintain it are known. They are present everywhere, and sometimes constitute the daily life of those affected, fueling the inflammation. Due to its location, the digestive system, and more particularly the intestines, are frequently affected by this inflammation. However, certain foods can contribute to inflammation, they are said to be "pro-inflammatory", while others can on the contrary calm it.
Foods to avoid and foods to adopt to better manage the disease
To avoid
Foods high in saturated fat like butter, cream, cheese, red meat, cold meats, and sweets as they contain pro-inflammatory components.
Foods containing additives (E), a large part of which is classified as carcinogenic.
Ultra-processed foods contain refined sugars, excess salt, saturated fat, additives, preservatives, colorings, flavor enhancers and poor quality ingredients, they do not provide any nutrients they often are. at high caloric density, these are "empty" calories. In this category, we find all industrial foods (spread, breakfast cereals, pastries, cakes, sweets, ready-made dishes such as quiches, pizzas, fast food, etc.).
Gluten because it contributes to intestinal hyperpermeability, which allows toxins to pass into the blood.
To adopt
You will need to provide your body with foods rich in antioxidant and anti-inflammatory properties. Foods of plant origin should constitute a major part of the diet.
To fill up on omega 3:
- Oilseeds (almonds, walnuts, hazelnuts), 30g per day.
- Hemp seeds, chia seeds, 15g per day.
- Oily fish such as sardines, herring or mackerel, twice a week.
- Vegetable oils such as hemp or camelina oil, one tablespoon per day.
To fill up on vitamins:
- Between 1 to 3 fruits per day.
- At least 400g of vegetables daily. Favor organic products to avoid bringing toxins to your body (pesticide residues and other chemicals).
- If you can't do without dairy products, those low in fat and lactose can be saved, such as yogurt. They are to be chosen from organic origin only and from goats or sheep.
Although the anti-inflammatory diet alone cannot reduce chronic inflammation, it is nonetheless an ally in regulating the disease and especially in preventing a worsening of symptoms.
Choosing the right dietary fat
Several studies have shown a relationship between certain fats and the incidence of endometriosis or the severity of symptoms. Omega-3s appear to be protective while omega-6s should be reduced. In addition, you must be careful with trans fatty acids.
A 2010 study of 71,000 women showed that women who have the highest intake of omega-3 fatty acids have a 22% lower risk of developing endometriosis. On the contrary, a diet rich in trans fatty acids would increase the risk by 48%. Finally, studies show that animal fats increase the risk of endometriosis.
Besides, the results of studies suggest that the intake of omega-6 - which has a pro-inflammatory action when they are more than omega-3 - should be reduced. Increasing the intake of omega-3 makes it possible to decrease the production of pro-inflammatory prostaglandins from omega-6, thus reducing inflammation and probably pain. Several studies show that lowering the omega-6 / omega-3 ratio reduces the risk of endometriosis and / or the severity of symptoms. A diet rich in omega-3s could therefore help reduce the risk of developing endometriosis or even reduce the disease.
In practice
The omega-6 / omega-3 ratio should ideally be between 1/1 and 5/1. To achieve it, you must reduce omega-6 (sunflower oil, grape seed oil, peanut, etc.) and increase omega-3. The best sources of omega-3 are fatty fish such as salmon, sardines, mackerel, herring, trout. For vegetarians/vegans, it is advisable to increase the intake of precursor foods such as nuts, flax seeds, vegetable oils rich in alpha-linolenic acid.
Regarding trans fatty acids, manufacturers have made real progress in recent years but there are still products with hydrogenated or partially hydrogenated oils that it is better to avoid.
Limit red meat
High consumption of red meat would increase the risk of endometriosis. It should therefore be avoided, just like cold cuts.
Women who eat 7 servings of red meat per week are twice as likely to suffer from endometriosis as women who eat less than 3 per week according to an Italian study. The same study reports that women who eat ham 3 times a week increased their risk of endometriosis by 80% compared to those who ate it less than once a week.
Among the possible explanations, the iron content of red meat. Researchers indeed show the implication of iron in endometriosis. On the other hand, excessive consumption of red meat causes both inflammation and oxidative stress, especially if it is eaten grilled.
A study published in the American Journal of Obstetrics and Gynecology in June 2018 confirms these results. The researchers analyzed the eating habits of 81,908 participants (Nurses' Health Study II) followed for 22 years. During this period, 3,800 cases of endometriosis were diagnosed. The results show that women who eat more than 2 servings of red meat per day have a 56% increased risk of suffering from endometriosis compared to those who do not eat red meat more than once a week. This association was stronger with unprocessed red meats. On the other hand, the researchers did not find any impact of the consumption of poultry, fish, shellfish and eggs on the risk of endometriosis.
In practice
Limit or even avoid the consumption of red meat. If you eat a little, do not overcook or broil it, the glycation products formed during these high-temperature cooking increases oxidative stress and inflammation.
More tips in The best way to eat meat (subscribers)
Eat lots of fresh vegetables and fruits
By pooling the results of two case-control studies involving more than 1,000 women in total, Italian researchers have shown that those who consume the greenest vegetables and fresh fruits have a significantly lower risk of suffering from endometriosis.
Green vegetables are particularly rich in folate, methionine and vitamin B6, nutrients that can influence the expression of certain genes, DNA methylation and prevent epigenetic alterations. All of these phenomena could be involved in endometriosis.
In a 2018 study, researchers used data from 70,835 women in the Nurses' Health Study II (8). Their results show the beneficial effect of high fruit consumption, particularly citrus, on the risk of endometriosis. Indeed, women who consume at least one serving of citrus fruits per day have a 22% lower risk of suffering from endometriosis, compared to women who consume less than one serving per week. The beneficial effect of citrus fruits could be explained by their high content of β-cryptoxanthin, a powerful antioxidant and a precursor of vitamin A.
The data obtained are however variable depending on the studies.
In practice
Give pride of place to green vegetables (spinach, green beans, broccoli, salads, Swiss chard, etc.), at least once a day, and eat fresh fruit, favoring grapefruit, orange, clementines. To get the most of their benefits, fruits and vegetables should preferably be chosen organic.
Avoid gluten?
A small study of 207 women with severe endometriosis reports that after 12 months of a gluten-free diet, 75% of women noticed an improvement in their symptoms, including a decrease in pain. But there are too few studies on the effect of a gluten-free diet on endometriosis to be able to draw any conclusions.
There are, however, several studies that have looked at the potential link between endometriosis and celiac disease... These two diseases indeed share some common points such as the involvement of oxidative stress and inflammation. The frequency of celiac disease is also thought to be higher in women with endometriosis. A study of 11,000 women shows that having celiac disease increases the risk of endometriosis by 39%.
In practice
Scientific evidence is lacking on the effectiveness of a gluten-free diet in improving the symptoms of endometriosis. But testimonials from women report that switching to gluten-free has been effective for them. You can do your experiment and eliminate gluten for a month and see if your symptoms improve.
- 7 keys to going gluten-free
- The gluten-free casein-free diet in practice
The case of soybeans
A few studies have been done to assess the effect of soy consumption on endometriosis. Japanese researchers have shown in a study of 138 women that those who have the highest levels of genistein and daidzein - the isoflavones in soy - in their urine have a lower risk of developing endometriosis in an advanced stage. Another study conducted on rats shows that soy isoflavones can regress endometriosis thanks to their role as hormone modulators. In another study, mice with endometriosis received varying doses (50 to 500 mg/day) of genistein for 14 days. The researchers noticed that the endometriosis lesions decreased, regardless of the dose of genistein received. Genistein is therefore capable of inhibiting the proliferation or of causing apoptosis of cells involved in endometriosis. For the moment, studies are few and do not allow to conclude as to the effect of soy in women with endometriosis.
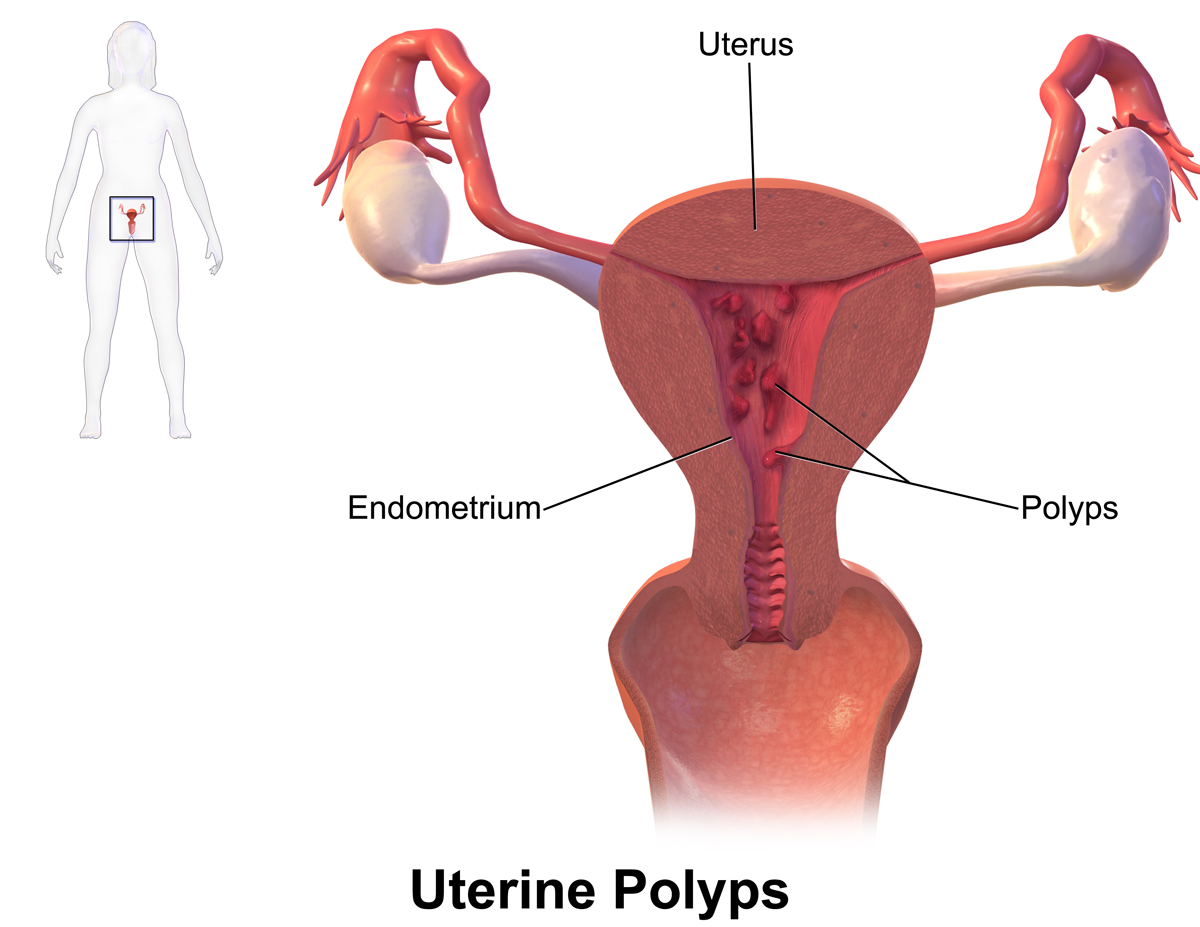
UTERINE POLYPS AND CANCER: Natural treatment
UTERINE POLYPS AND CANCER
A polyp can sometimes seem like a fibroid uterus ( polyp fibrous) or cancer endometrial ( polyp atypical, irregular). Conversely, cancer endometrial can sometimes look like a polyp. The combination of a polyp to cancer endometrial is more common after menopause. However, Dawasanté experts provide you with a natural treatment to cure uterine polyp cancer. Click on the image below to discover this natural treatment.
To contact our experts please call or write to us on the following number, tel / WhatsApp: https://wa.me/22996374527
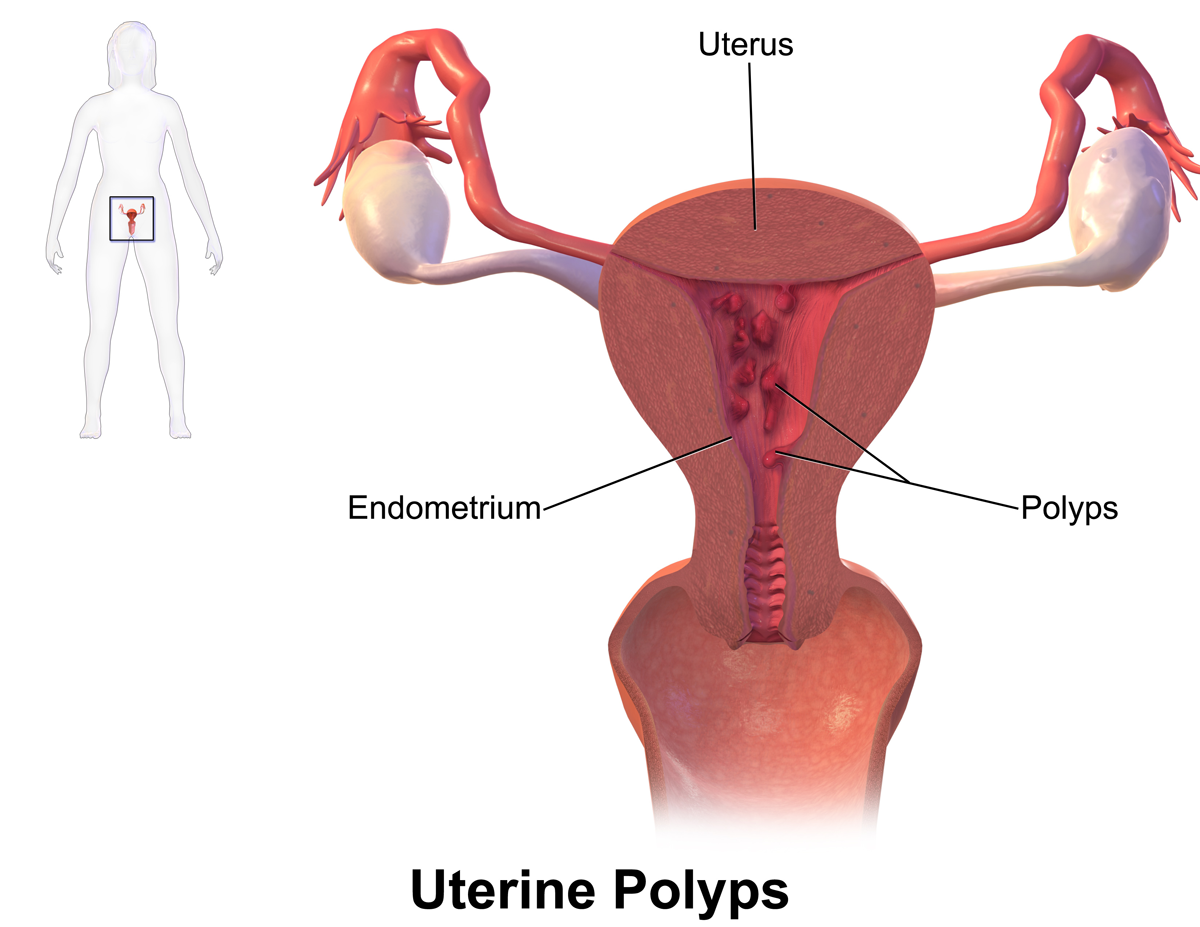
The uterine polyps are growths that develop at the expense of the lining of the uterus (endometrium), or at the expense of the lining of the cervix (endocervical).
These growths are benign tumors. They can be single or multiple. A polyp can be "pedicle" (comprising an insertion foot) or sessile (broad implantation base). It can be "fibrous" or "mucous". By definition, the development of a polyp occurs at the expense of a mucous membrane. This is why, in addition to the uterus, certain organs or areas of the human body can be invaded by this type of tumor such as the bladder, colon, stomach, vagina, etc.
The uterine polyps are outgrowths attached to the inner wall of the uterus which extends into the uterine cavity. Cellular proliferation in the lining of the womb (endometrium) results in the formation of uterine polyps, also called endometrial polyps. These polyps are usually non-cancerous (benign), although some can be cancerous or turn into cancer (precancerous polyps).
A uterine polyp can look like a fibroid or a cancerous tumor, so be careful not to get the wrong diagnosis. Cancerization of the polyp is possible.
All examinations performed should show whether the uterine polyps are benign or not. Thus, after removing these growths, a complete analysis of them is required. Postmenopausal women are prone to endometrial cancer combined with uterine polyps.
Two forms of treatment are possible to treat polyps, the choice is based on their benignity, size, appearance, etc. Those that are small and less worrying may go away as a result of hormonal drug therapy. With this treatment, the patient takes progestins. In most cases, operative hysteroscopy is necessary, it consists of the removal of the polyps. This form of treatment should be carried out with great care, especially in women who wish to have children later. For postmenopausal women, the risk of recurrence being high, endarterectomy is recommended.
Endometrial cancer is a cancer of the inside of the uterus, where the endometrium is the lining that lines the inside of the uterus. In women with cancer at this level, endometrial cells multiply abnormally. Endometrial cancer usually occurs after menopause, but 10 to 15% of cases affect premenopausal women, including 2 to 5% of women under 40 years old.
A significant proportion of endometrial cancer is thought to be attributable to an excess of estrogenic hormones produced by the ovaries or supplied by the outside. The ovaries produce 2 types of hormones during the female cycle: estrogen and progesterone. These hormones act on the endometrium throughout the cycle, stimulating its growth and then its expulsion during menstruation. An excess of estrogen hormones would create an imbalance conducive to the poorly controlled growth of endometrial cells.
Several factors can increase estrogen levels, such as obesity or hormone therapy with estrogen alone. This type of hormone therapy is therefore reserved for women who have had the uterus removed or hysterectomy who are no longer at risk of endometrial cancer. For more information, see the People at risk and Risk factors sections.
For some women, however, endometrial cancer does not appear to be caused by a higher level of estrogen.
Other causes are involved in endometrial cancer, such as advanced age, overweight or obesity, genetics, hypertension, etc.
Sometimes cancer occurs without a risk factor being identified.
Like any mucous membrane, the endometrium is made up of surface cells called “epithelial” and supporting tissue, the “chorion”. More than 90% of endometrial tumors develop at the expense of the epithelium. This category includes cancerous lesions such as adenocarcinomas and carcinosarcomas, pre-cancerous lesions such as atypical hyperplasias, endometrial polyps, and lesions induced by tamoxifen. Adenocarcinomas, the most common form, are developed from "glandular" type epithelial cells.
Other metabolic factors: diabetes and glycemic load
Diabetes is a risk factor for endometrial cancer. The risk of developing this cancer is twice as high (significant relative risk) in diabetic patients than in people without diabetes (Larsson, 2006).
It is the development of insulin resistance that is responsible for the increased risk of cancer. Insulin is then in large quantities in the blood and will be able to stimulate growth factors acting on the endometrium. The precise mechanisms are not well known. This is confirmed in the 2013 WCRF / AIRC report. This same international report also found that increased glycemic load (which estimates the ability of foods eaten to increase blood glucose) is a risk factor for endometrial cancer with a probable level of scientific evidence to account. based on current scientific data; these are not as convincing as for obesity.
Early puberty and late menopause
Age at puberty determines when the ovaries start producing estrogen, and menopause determines when they stop producing estrogen. Earlier puberty or late menopause, therefore, exposes a woman to estrogen for a longer period of her life and therefore represents a risk factor.
Not having had a child (nulliparity)
The menstrual cycle of women experiences a period during which the functional area of the endometrium collapses. In order to accommodate the future fertilized egg, the endometrium must regenerate. For this, estrogen plays a role in stimulating cell growth in the endometrium.
During pregnancy, there is no ovulation for 9 months. The estrogen stimulation does not stop, however, but is much less than if there had been 9 ovarian cycles. Thus, women without children are exposed to greater amounts of estrogen: this is considered a risk factor for the development of endometrial cancer (Lochen, 1997).
This is sort of how polyp can be the root cause of cancer or various tumors.
To contact our experts please call or write to us on the following number, tel / WhatsApp: https://wa.me/22996374527
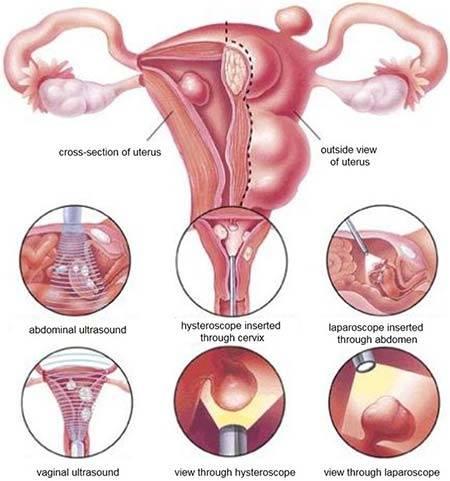
HYSTEROSCOPY UTERINE POLYPES CURETTING: Natural treatment
UTERINE HYSTEROSCOPY POLYPES CURETTING
Uterine curettage is an operation that involves removing the internal tissue of the uterus called the endometrium.
This curettage is carried out using a curette (a small "spoon"). Here is the natural treatment to cure uterine polyps without curettage. Click on the image below to discover this natural treatment.
Curettage is most often performed in conjunction with hysteroscopy.
Previously the polyps were removed by an intervention called: Curettage, today this intervention has become obsolete and out of fashion because blind and often incomplete.
Hysteroscopic resection of polyps: consists under visual control (thanks to the endoscope placed in the cavity) in electively (precisely) removing the polyp without touching the rest of the cavity, so as not to damage it (this intervention must replace the classic “curettage” which is now somewhat obsolete because it is blind and often incomplete). This new way of approaching the procedure (the use of an endoscopic camera) is more precise and does not risk impairing subsequent fertility. If the polyps are multiple or numerous, this method makes it possible to list them and remove them all with precision (each will be analyzed separately).
After menopause, or when the patient no longer wishes to become pregnant, it can be combined with an endarterectomy (intervention which consists in removing the endometrium: the mucous membrane that lines the uterus) in order to prevent new polyps from growing nearby. of those who have been withdrawn; this intervention (endarterectomy) clearly improves the results of this type of intervention.
In patients of childbearing age, the operative hysteroscopy should be checked by a new diagnostic hysteroscopic check (done in consultation) one to two months after the operation in order to check the integrity of the cavity and the good healing.
Treatment may not be necessary if the polyps are not causing any symptoms. However, polyps should be treated if they cause heavy bleeding during menstruation or if they are suspected of being precancerous or cancerous. They should be removed if they cause problems during pregnancy, such as miscarriage, or result in infertility in women who wish to become pregnant. If a polyp is discovered after menopause, it should be removed.
The treatment methods include the following:
- Medicines: Medicines that help regulate hormonal balance, such as progestins or gonadotropin-releasing hormone agonists, can be used temporarily. These drugs help relieve symptoms. However, symptoms will usually return after you stop taking the medication.
- Hysteroscopy: (see above) This can also be used as a method of treatment. In treatment, the doctor inserts surgical instruments into the hysteroscope to remove the detected polyps.
- Curettage: (see above) It can be performed at the same time as a hysteroscopy. While using the hysteroscope to examine the inside of the uterus, the doctor uses a curette to scrape the lining and remove polyps. Polyps can be sent to a lab to determine if they are benign or cancerous. This technique is effective for small polyps.
- Additional surgery may be needed if a polyp cannot be removed by other methods or if the polyps are cancerous. A hysterectomy, a surgical procedure that removes the entire uterus, may be needed in cases where cancer cells are found in uterine polyps.
Operative hysteroscopy is the treatment of excellence for the uterine polyp.
The surgical procedure will remove the polyp in its entirety including the area on which the uterine polyp is implanted. Sometimes the adjacent mucosa will also be removed during the same operation, when it is too thick, especially when the patient is postmenopausal. An endometrial resection or endarterectomy will then be performed. When performing a therapeutic curettage, the doctor removes the contents of your uterus, not just a small sample of tissue. Your doctor can do this for:
- Cleanse the tissues that remain in the uterus after a miscarriage or abortion to prevent infection or heavy bleeding
- Remove a molar pregnancy, in which a tumor forms instead of a normal pregnancy
- Treat excessive bleeding after childbirth by clearing the placenta from the uterus
- Remove cervical or uterine polyps, which are usually non-cancerous (benign)
Curettage with another procedure called a hysteroscopy. During a hysteroscopy, thin with a light and a camera at the end into your vagina, through your cervix, and into your uterus.
The doctor then views the lining of your uterus on a screen, noting any areas that appear abnormal, checking for polyps, and taking tissue samples, if necessary. During a hysteroscopy, your doctor may also remove uterine polyps and fibroids.
This polyp will be sent to the laboratory which will analyze it; in a few days, the result will be available. But the surgeon is most often able to guide the diagnosis and reassure the patient at the simple macroscopic view during the operation (i.e. with the simple eye) of the nature of this polyp
For dilation and curettage, you will be given anesthesia. The choice of anesthesia depends on the reason for curettage and your medical history.
General anesthesia makes you unconscious and unable to feel pain. Other forms of anesthesia provide light sedation or injections to numb only a small area (local anesthesia) or a larger area (regional anesthesia) of your body.
During the procedure:
- Your doctor inserts an instrument called a speculum into your vagina, like during a Pap test, to see your cervix.
- Your doctor inserts a series of thicker and thicker sticks into your cervix to slowly dilate your cervix until it is properly opened.
- Your doctor removes the dilation rods and inserts a spoon-shaped instrument with a sharp edge or suction device, then removes the uterine tissue.
Because you are unconscious or sedated during D&C, you should not experience any discomfort.
After the procedure
You can spend a few hours in a recovery room after the D&C so your doctor can monitor you for heavy bleeding or other complications. It also gives you time to recover from the effects of the anesthesia.
If you had general anesthesia, you might feel nauseous or vomit, or you might have a sore throat if a tube was placed in your windpipe to help you breathe. With general anesthesia or light sedation, you may feel drowsy for several hours.
The normal side effects of a D&C can last for a few days and include:
- Slight cramps
- Spotting or light
- Postoperative check-up: very rarely, a new diagnostic hysteroscopy will be performed after surgery to assess the state of the uterine cavity. Most often no examination is necessary following the removal of a polyp by operative hysteroscopy.
Of course, if the results of the polyp analysis are worrying, a new medical and surgical strategy will be considered.

NABOTH CAUSE CYST: Natural treatment
NABOTH CAUSE CYST
A cyst Nabothian (or egg Naboth ) is a cyst mucous that develops at the neck of the uterus; it is due to the obliteration of the excretory ducts of the glands of the uterine cervix. Here is the natural herbal treatment to cure Naboth cysts. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
This is the accumulation of mucus produced by the glands of the endocervix (columnar epithelium) which cannot be evacuated due to the physiological covering of the gland by squamous epithelium (a phenomenon of repair). These cysts are most often visible at the level of the ectocervix, presenting on colposcopy as a translucent cyst whose wall is covered with vessels. They can also sit in the endocervix and be visible on ultrasound.
Causes of Naboth's cyst
The Naboth cysts are formed:
- Either because there is a development of the tissue of the cervix (following childbirth for example).
- Either in older women, because the natural secretions are retained in the thinned tissue of the cervix.
The cause of the appearance of a Nabothian cyst is the obstruction of the ducts carrying the secretions from the mucus glands. It is a common phenomenon in a woman after childbirth, the lining of the cervix develops, or in postmenopausal women, in whom the lining of the uterus becomes thinner.
The cysts of Naboth often appear after repair ectropion: epithelium squamous metaplasia (newly formed) covers the glandular endocervical crypts, without colonizing, and locked glands continue to secrete, which is responsible for their expansion; the glands then form small cysts which protrude under the squamous epithelium.
These retentional glandular cysts are visible on the ectocervix.
Nabothian cysts form when the mucus-producing glands in your cervix become covered with skin cells and become blocked. The skin cells clog the glands, causing mucus to build up. This causes a cyst to form on the neck that looks like a small white bump.
Childbirth and physical trauma to the cervix can cause Nabothian Trusted Source cysts in some women. During childbirth, excess skin cells can grow on the mucous gland and trap the mucus, causing cysts to form. Physical trauma around the cervix can cause excess tissue on top of the mucous glands during the healing process and trap mucus, which can also cause these cysts to appear. Cysts caused by physical trauma are especially common during recovery from chronic cervicitis, in which cervical tissue is inflamed.
You are more likely to develop these cysts if you are pregnant or of childbearing age. Childbearing age lasts from puberty until the onset of menopause, which can sometimes reach 40 or 50 years.
You might also be at risk of developing similar cysts if you have a disorder called malignant adenoma. This condition is a type of neoplasia that affects the production of mucus in the cervix of your uterus. These cysts are often identical to Naboth's cysts. Talk to your doctor about screening for malignant adenoma if you are concerned that your Naboth cyst is the result of this condition rather than other causes.
In most cases, Nabothian cysts appear when new tissue grows back on the cervix after childbirth. This new tissue blocks the openings of the nabothian glands in the cervix, trapping their mucous secretion in tiny pockets under the skin. Nabothian cysts are a normal finding on the cervix of women who have had children. They are also seen in postmenopausal women whose cervical skin has thinned with age. Less often, nabothian cysts are linked to chronic cervicitis, long-term infection of the cervix.
The mucus-producing gland in the cervix is covered with cells and skin clogs. Physical trauma and childbirth cause additional skin cells to grow in the mucous gland and trap the mucus, resulting in the cyst forming.
Infection: The cervical glands produce large amounts of mucus to protect the area from all kinds of infections and inflammation. This process can be understood as the body's natural way to wash away foreign objects that can cause health problems.
As the level of mucus production increases, there will obviously be an increased risk of blockage and cyst formation. Therefore, infections and inflammation can cause the growth of Naboth cysts.
Hormonal changes: the changes hormonal play a direct role in the formation of such cysts. For example, menopause is a stage in which a woman may experience thinning of the skin of the cervix. It causes inflammation of the cervix causing cervical infection.
The cervix connects the two most important parts of the female reproductive system. Therefore, hormonal changes will have a direct effect on him.
These cysts mainly develop during pregnancy, childbirth or menopause. Therefore, the development of these cysts could be the result of changes in hormone levels.
Trauma: Injury or scarring of the tissues lining the cervix could lead to the formation of Naboth's cysts. The body tries to grow new tissue to repair and heal the injured area, but sometimes there can be an overgrowth of the tissue.
Pregnancy: Normally, the cervix remains open to allow the movement of semen from the vagina to the uterus and the flow of menstrual fluid from the uterus to the vagina.
However, during pregnancy, the body's mechanism closes the cervix to ensure the development of the fetus in the womb. New tissue grows on the mucous gland after childbirth due to the process of metaplasia.
If these tissues grow excessively, they could block the glands and prevent mucus from draining out, leading to the development of Naboth cysts.
Neck Problems: Postmenopausal women may experience thinning of the skin of the cervix. Inflammation of the cervix is a common effect of cervicitis.
These problems, along with other sexually transmitted infections of the cervix, could lead to the development of cysts on the surface of the cervix.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
SYMPTOMS OF UTERINE POLYPs: Natural treatment
WHAT ARE THE SIGNS OF UTERINE POLYPS?

Uterine polyps are stressful news for any woman. They can cause a negative experience and discomfort. They are not cancerous, at least for the most part they are not. To what extent they still endanger health is a question whose exact answer can only be heard in the doctor's office.
Uterine polyps come in different sizes and are attached to the wall of the uterus. They are single or in a group of several. They are likely to occur at a young age but are more common in women before and during menopause.
Uterine growths are sensitive to estrogen and the most likely causes are hormonal changes. Among the risk factors for them are overweight, high blood pressure, and some drugs for breast cancer.
HERBAL TREATMENT FOR UTERINE POLYPS
The causes of this disease can be different, and tumors appear in young girls and older women. If the doctor put such a diagnosis - do not despair. There are ways not only with medication, you can still treat uterine polyps with an herbal remedy. Both methods are effective in killing polyps and preventing new ones. A woman can choose the most suitable treatment option for yourself, depending on the characteristics of her body.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: https://wa.me/22996374527
Symptoms of uterine polyps
The truth is that they are mostly found during random examinations by a gynecologist. This is not due to negligence or ignorance on the part of the ladies, but only because these polyps form asymptomatically. Doubt about their locality is caused mainly by:
- Irregular menstrual flows. They appear at no time and last indefinitely.
- Spots between periods. They are not exactly a monthly flow, but rather spots left by one.
- Prolonged menstruation. Significant lengthening of the menses for no apparent reason.
The most popular recipes against uterine polyps

Consider effective and easy-to-prepare folk remedies that will help treat uterine polyps without surgery and without significant obstruction to the body.
Herbal extract for regular intake
To prepare the soup, you will need 1 teaspoon black currant fruit, 3 teaspoons cinnamon wild rose fruit, 2 teaspoons of dioica nettle leaves.
Currants, rose hips, and nettle bloomery should be mixed and grind well.
Then take a tablespoon of the resulting mixture and pour two cups of boiling water.
Giving to run for an hour and filter through cheesecloth (during which time the infusion will gain almost room temperature).
If the taste is too bitter, you can add a little sugar - it does not affect the properties of the soup. It should be taken 4 times a day at any time by drinking half a glass. This recipe is a great help in treating cervical polyp.
Herbal decoction for douching
Endometrial surface polyps arise for various reasons, one of which is a violation of the natural hormonal balance against the background of nutrient deficiency. It is this situation that can be corrected by applying a decoction.
Should be used if there are vaginal cords.
To prepare the need: 2 tablespoons herb yarrow ordinary, 2 tablespoons rosemary leaves, 2 tablespoons sage leaves drug, 4 tablespoons plain oak bark.
All these components should be well ground and mixed in an enamel bowl. Then, pour boiling water volume of 2.5 liters and bring it to a boil.
Boil the broth need about half an hour, then cool - always at room temperature. When the broth itself reaches room temperature, it is necessary to filter through a fine sieve or gauze. Then it can be used for vaginal douching, the procedure is repeated twice a day. also the effective herbal treatment of uterine fibroids - Another annoying problem.
Effective folk remedy against uterine polyps
For the treatment of uterine polyps folk remedies it is possible as an operative or homeopathic way, and with the help of folk remedies, even if the symptoms are strong enough. Use this decoction should be in the presence of heavy and persistent vaginal cords.
To prepare the decoction, you will need to collect: 3 tablespoons of dioica nettle leaves, 5 tablespoons herb knotweed, 1 tablespoon chamomile, 1 tablespoon of ordinary oak bark.
You need to carefully grind and mix well all the ingredients. Then take two tablespoons of the resulting mixture, put in an enamel pan, and fill it with 1 liter of boiling water.
Decoction boil for 5 minutes on low heat, then leaves to cool to room temperature.
When the broth has cooled, strain it through a fine sieve or cheesecloth. The resulting mixture can be used for vaginal douching. For effective enough to use it at least twice a day.
Experience has shown that the use of this decoction can eliminate endometrial polyp without surgery.
Recipe based on celandine
Particularly effective since ancient times is considered the treatment of uterine polyps greater celandine. The more you can use it not only for sprintsevalnyh solutions but also for oral administration.
However, it should be remembered that before taking such funds it is necessary to consult with your doctor.
The same recipe is very simple.
We need to a quart a jar and fill it with fresh grass celandine.
Then you need to pour boiling water over the grass.
The bank is not broken, it is best to warm up before preparing the solution.
Cover the dish with a warm scarf and it will leave in a few hours.
Then, the mixture is ready, and it can be used for regular swallowing.
It should be taken three times a day. We must start with very small portions (about 1 teaspoon) and then gradually increase the dose by the end of the second week from one serving to 100 milliliters.
A two-week course can be effective enough to eliminate appearing polyp in the uterus.
Sometimes, of course, it is not enough, and you will have to repeat it. But before the infusion of celandine again, you need to rest for not less than two weeks.
It is also useful for uterine propolis, for example, candles for uterine fibroids from propolis are useful for healing.
As is the case with other folk remedies for the treatment of uterine polyps, be sure to remember that the infusion of celandine - is not a cure. And polyps, regardless of their origin, require medical supervision. However, to engage with homeopathy, and especially immediately agree to surgery should not be in any case - because your body must protect itself and carry out its treatment should be as painless as possible means.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: https://wa.me/22996374527
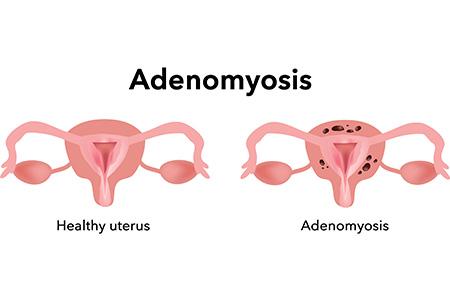
ADENOMYOSIS NATURAL TREATMENT
We talk about adenomyosis when the tissue that normally lines the uterus (the endometrium) grows in the muscular wall of the uterus. Adenomyosis can cause menstrual cramps, low abdominal pressure, and bloating before your period and can lead to heavy periods. It is even responsible in some cases of infertility in women. Here is the natural herbal treatment from Dawasanté experts to treat adenomyosis. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Adenomyosis is most common in women who have had several children.
If you have adenomyosis and want to avoid the operation at all costs, you have come to the right place. Here we offer you a natural remedy made from medicinal plants very effective to permanently cure adenomyosis. It is specially designed for patients who do not want to have surgery because every operation carries a risk.
Natural treatment
The natural treatment that we offer to cure adenomyosis consists mainly of natural herbal teas. This natural herbal treatment for adenomyosis will remove the pain you feel during your period and allow you to have normal cycles. It outperforms conventional treatments that relieve pain, but don't get to the root of the pain. Our herbal tea contains plants that reduce the estrogen level in the blood. This helps block the proliferation and bleeding of adenomyosis lesions. These herbal remedies are rich in an antioxidant that inhibits the enzymes that lead to pro-inflammatory prostaglandins. These are nutrients in high doses anti-inflammatory. This will definitely put an end to the pain you feel during your period. We know that many of you have had adenomyosis treatment or surgery, but the pain returned years later. No panics ladies! With us, no recurrence, no side effects. You will be permanently cured of adenomyosis.
This natural herbal tea also facilitates cell multiplication relating to fertility, growth, healing and immunity; to the synthesis and secretion of many hormones. Thanks to these medicinal plants, you will avoid miscarriages. It is nature's secret to cure adenomyosis and get pregnant quickly.
Our natural remedy to treat adenomyosis very often gives positive results and acts significantly on the reduction of the pain felt. It has an efficiency rate of 98%. Trust us ladies and you will get pregnant once more.
To discover our natural remedy to cure Naboth cysts, click here
Symptoms
Sometimes adenomyosis does not cause any signs or symptoms or causes only mild discomfort. However, adenomyosis can cause:
-
Heavy or prolonged menstrual bleeding
-
Severe cramping or sharp, knife-like pelvic pain during menstruation (dysmenorrhea)
-
Chronic pelvic pain
The causes
The cause of adenomyosis is not known. There have been a lot of theories, including:
· Invasive tissue growth. Some experts believe that adenomyosis results from the direct invasion of endometrial cells through the lining of the uterus into the muscle that forms the walls of the uterus. Uterine incisions made during an operation such as a cesarean section could promote the direct invasion of endometrial cells into the lining of the uterus.
· Developmental origins. Other experts suspect that adenomyosis originates in the uterine muscle from endometrial tissue deposited there during the formation of the uterus in the fetus.
· Inflammation uterine is related to childbirth. Another theory suggests a link between adenomyosis and childbirth. Inflammation of the lining of the uterus during the postpartum period can cause the normal boundary of the cells that line the uterus to rupture. Surgery on the uterus can have a similar effect.
· Origin of stem cells. A recent theory suggests that stem cells from the bone marrow could invade the uterine muscle, causing adenomyosis.
Regardless of the course of adenomyosis, its growth depends on the circulation of estrogen in the female body.
Risk factors
Risk factors for adenomyosis include:
-
Previous uterine surgery, such as cesarean or fibroid removal
-
Childbirth
-
Middle Ages
Most cases of adenomyosis occur in women between the ages of 40 and 50. Adenomyosis in these women could be linked to longer exposure to estrogen compared to that in younger women. However, current research suggests that the condition might be common in younger women.
Complications
If you often have heavy and prolonged bleeding during your period, you can develop chronic anemia, which can lead to fatigue and other health problems.
While not harmful, the pain and excessive bleeding associated with adenomyosis can disrupt your lifestyle. You may be avoiding activities that you have done in the past because you are in pain or are worried about bleeding.
Diagnostic
Your doctor may suspect adenomyosis based on:
-
Signs and symptoms
-
A pelvic exam that reveals an enlarged and tender uterus
-
Ultrasound of the uterus
-
Magnetic resonance imaging (MRI) of the uterus
In some cases, your doctor may take a sample of uterine tissue (endometrial biopsy) to check that your abnormal uterine bleeding is not associated with another serious condition. But an endometrial biopsy will not help your doctor confirm the diagnosis of adenomyosis.
The only way to confirm adenomyosis is to examine the uterus after a hysterectomy. However, pelvic imaging such as ultrasound and MRI can detect signs of it.
Other uterine diseases can cause signs and symptoms similar to adenomyosis, making adenomyosis difficult to diagnose. The conditions include fibroids (leiomyomas), uterine cells growing outside the uterus (endometriosis), and growths in the lining of the womb (endometrial polyps).
Your doctor may conclude that you only have adenomyosis if you have chosen other possible causes of your signs and symptoms.
Medical treatments
Adenomyosis often goes away after menopause, so treatment may depend on how close you are to this stage of life.
Treatment options for adenomyosis include:
· Anti-inflammatory. Your doctor may recommend anti-inflammatory drugs, such as ibuprofen, to control the pain. By starting an anti-inflammatory medication one to two days before your period starts and taking it during your period, you can reduce menstrual blood flow and help relieve pain.
· Hormonal Drugs. Birth control pills that combine estrogen and progestins, patches containing hormones, or vaginal rings can reduce the heavy bleeding and pain associated with adenomyosis. Progestin-only contraception, such as an intrauterine device, or continuous-use birth control pills often lead to amenorrhea - the absence of periods - which may provide some relief.
· Hysterectomy. If your pain is severe and no other treatment has worked, your doctor may suggest surgery to remove your uterus. Removing your ovaries is not necessary to control adenomyosis.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
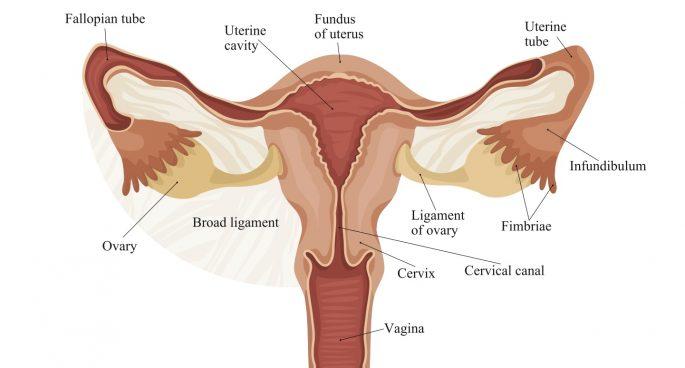
OBSTRUCTION OF FALLOPIAN TUBE: Natural treatment
Endometriosis is a common and painful disease that affects thousands of women around the world in North America as in Africa and South, other continent and is one of the three main causes of infertility in women.
During a normal menstrual cycle, the lining of your uterus - called the endometrium - begins to thicken before you become pregnant. If you don't get pregnant that month, your body loses its endometrium during your period and the process starts all over again. In endometriosis, for reasons that researchers don't fully understand, tissue very similar to the endometrium begins to grow outside the uterus in various places that it shouldn't. It can appear in or on the ovaries, fallopian tubes, the various structures that support the uterus and the lining of the pelvic cavity. Sometimes it is also found in other places, including the cervix, vagina, rectum, bladder, bowel and elsewhere.
The problem is, this tissue behaves like normal endometrial tissue - it builds up and breaks down with your menstrual cycle - but it can't shed like normal endometrial tissue during your period. As a result, unwanted tissue causes irritation and inflammation. This build-up of tissue can prevent the eggs from leaving the ovaries or from being fertilized by the sperm. It can also leave scars and block the fallopian tubes, preventing the meeting between the egg and the sperm.
Finally, endometriosis problems can be the cause of tubal obstruction. This is because pieces of the uterine lining can end up in the tubes or on the ovaries and block the progression of sperm to the egg, thus preventing fertilization. Dawasanté experts provide you with a natural herbal treatment to unblock your tubes and allow you to quickly get pregnant.
Click on the image below to discover this natural treatment.
However, obstruction of the fallopian tubes is a major cause of female infertility. The blocked fallopian tubes do not allow the egg and sperm to converge, making fertilization impossible. The fallopian tubes are also called oviducts, uterine tubes, and salpines (singular salpinx).
Tubal obstruction
About 20% of female infertility can be attributed to the causes of the tubes. occlusion of the distal tubes (affecting the tip towards the ovary) is usually associated with the formation of hydrosalpinx and is often caused by Chlamydia trachomatis. Pelvic adhesions can be associated with such an infection. In less severe forms, the fimbriae may be clumped and damaged, but some permeability may still be preserved. Tubal obstruction in the middle of the segment may be due to tubal ligation procedures, as this part of the tube is a common target for sterilization procedures. Proximal tubal occlusion can occur after infection, such as. In addition, some tubal sterilization procedures such as the Essure procedure target the part of the tube near the uterus.
A blockage of the uterine tubes can be caused by various disorders, and in some rare cases even be present from birth without causing symptoms until the desire to conceive a child. Obstruction of the fallopian tubes is very often involved in cases of female infertility.
There are various causes of obstruction, or even lesions, of the tubes:
- Pelvic infections;
- Use of an intrauterine device;
- Rupture of the appendix;
- Pelvic or lower abdominal surgery;
- Certain pathologies, for example, tuberculosis;
- Ectopic pregnancy in the fallopian tubes;
- Congenital malformations of the tubes;
- Uterine fibroma ;
- Endometriosis ;
- Asherman's syndrome (lesions or infections during surgery).
We speak of proximal tubal obstruction when the tubal isthmus is involved. It can follow an abortion, miscarriage, cesarean section, pelvic inflammatory disease or the contraceptive pill.
If the distal tubes are blocked, it is the end of the tube on the side of the ovary that is affected. This type of obstruction is often associated with a "hydrosalpinx" which refers to the abnormal presence of a pocket of fluid in the fallopian tube. Usually, hydrosalpinx is caused by infection with Chlamydia trachomatis (sexually transmitted infection).
In other cases, the ovarian fringes, which have an important role in the conduction of the oocyte in the tubes, are damaged or stick together.
Several elements are at the origin of this obstruction
GENITAL INFECTIONS
The majority of the causes of obstruction are infections of the genital tract, especially of the tubes ( salpingitis ) which have occurred in the past. Most of the time, they are due to sexually transmitted diseases (such as chlamydia), which may have gone unnoticed. Nevertheless, they were sufficient to block the proboscis and make it waterproof. This is why it is important for all women to prevent the risk of STDs, in particular through safe sex with occasional partners and regular gynecological monitoring.
MEMBERSHIP
Aside from infections, adhesions, where the two sides of the tube wall stick together, can also be present.
ENDOMETRIOSIS
Endometriosis problems may be the cause of obstruction of the fallopian tubes. This is because pieces of the uterine lining can end up in the tubes or on the ovaries and block the progression of sperm to the egg, thus preventing fertilization.
Most often, a catheter can become blocked due to an infection such as pelvic inflammatory disease (PID). The tubal infertility rate would be 12% after one, 23% after two and 53% after three episodes of PID. The fallopian tubes can also be blocked or disabled by endometritis, infections after childbirth, and intra-abdominal infections, including appendicitis and peritonitis. The formation of adhesions may not block a fallopian tube, but make it dysfunctional by deforming it or separating it from the ovary. It has been reported that women with distal tubal occlusion have a higher rate of HIV infection.
The fallopian tubes can be blocked as a method of birth control. In these situations, the tubes tend to be healthy and, in general, patients requesting the procedure had children. Tubal ligation is considered a permanent procedure.
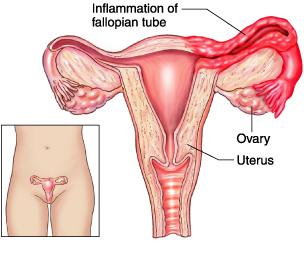
SALPINGITIS NATURAL TREATMENT
Salpingitis, what is this?
A PID is an infection of one or both fallopian tubes. A germ of sexually transmitted diseases is always responsible for the primary infection (gonococci and chlamydia especially), the infection by other pathogenic bacteria occurring only secondarily through the vaginal, blood, lymphatic or peritoneal route. However, Dawasanté experts have a natural herbal treatment for a tubal infection. Click on the image below to discover this natural treatment.
Thanks to our research, we have identified several natural home remedies that are very effective in unblocking the tubes and getting pregnant quickly. It is:
Turmeric is a natural anti-inflammatory. It can be very effective in unblocking the fallopian tubes. Curcumin, the active ingredient in turmeric, is very effective in reducing inflammation. You can consume curcumin in supplement form, add turmeric to your food, or drink a glass of turmeric.
Turmeric has no known side effects when taken in small doses. However, at doses of more than 8 grams per day, it can have unwanted effects. Make sure you take the correct dosage of turmeric or, better yet, add the spice to your cooking.
2-Garlic
Garlic is a great way to improve fertility and unclog fallopian tubes. Garlic has always been consumed for its many health benefits as the aphrodisiac properties present in garlic help in improving blood circulation in the body. Eating raw garlic every day on an empty stomach helps fight infertility in women, lowers blood pressure and cholesterol.
3- Vitamin C
Vitamin C is an antioxidant that can reduce inflammation by helping your immune system to function better. For this reason, it is ideal for healing scars and may have a positive effect on the fallopian tubes.
If you suspect that the cause of the blocked fallopian tubes is an infection, vitamin C can help you overcome it. To unclog your tubes, we recommend that you use natural vitamin C. It's easy to get vitamin C from food sources, especially when you like citrus fruits. Eat as many oranges, lemons, and grapefruit as possible. Aside from, you can try strawberries, broccoli and green peppers to heal yourself with a good vitamin C.
4- Castor
oil Castor oil has been used for centuries to improve fertility in women, and more especially to unblock the fallopian tubes. How is it used?
- dipped a rag in castor oil
-Place this cloth on the skin on the lower abdomen. This will improve circulation and promote healing of the tissues and organs under the skin. Castor oil therapy helps the fallopian tubes by softening tissue and improving circulation in the pelvic area.
5- Apple cider
vinegar Apple cider vinegar is a fermentation product that produces yeasts and bacteria that are beneficial for unblocking the tubes. This is because vinegar contains a number of vitamins and minerals, including magnesium, potassium, copper, group B vitamins, and vitamin C. Taken daily, it can help unblock the fallopian tubes by balancing hormones and shrinking fibroids.
Directions:
-Mix 2 tablespoons of apple cider vinegar in 1 glass of water
-You can add a touch of honey or molasses to soften the mixture.
-You can drink the mixture right away or sip it for 30 minutes.
6-Meditation
Meditating daily will help you decrease stress levels and promote general healing. However, reducing stress reduces deterioration and inflammation of the fallopian tubes.
As an additional tip, don't forget to start meditating with a short session consisting of breathing exercises and relaxation techniques. Even if you only do it for a few minutes, meditation will provide you with positive energy to start your day and reduce your stress.
7- Fertility massage
Some practitioners of alternative medicine suggest fertility massages unblock the fallopian tubes. These usually involve hot oil massages in the abdominal area. How to do a fertility massage?
- Lie down on an exercise mat with your face up and a pillow under your lower back.
-Relax and apply almond, olive, or lavender oil to your hands and apply by massaging your pubic bone, as the uterus is below this bone.
-Gently massage from bottom to bottom and pull your abdominal wall towards the navel. Maintain this position, count to 10 and release your hands. Repeat this maneuver 10 to 20 times.
NB: Do not do this if you are bleeding or are pregnant. Also, if possible, visit a massage therapist who specializes in abdominal massage for best results.
8- Mugwort
Mugwort is a plant sometimes recommended to improve female fertility. It is also recommended for unblocking the fallopian tubes.
Mugwort has a long history of use for fertility in a number of different cultures. It has been used all over Europe and Asia for centuries. It is often used in Chinese medicine in the form of moxibustion, which involves burning mugwort above an acupressure point.
9- Green clay
The use of green clay to unclog the proboscis is very common in East Africa.
The blocked tubes are unblocked by the serious treatment of green clay and the follow-up of a feeding program made by a dietician or a naturotherapist.
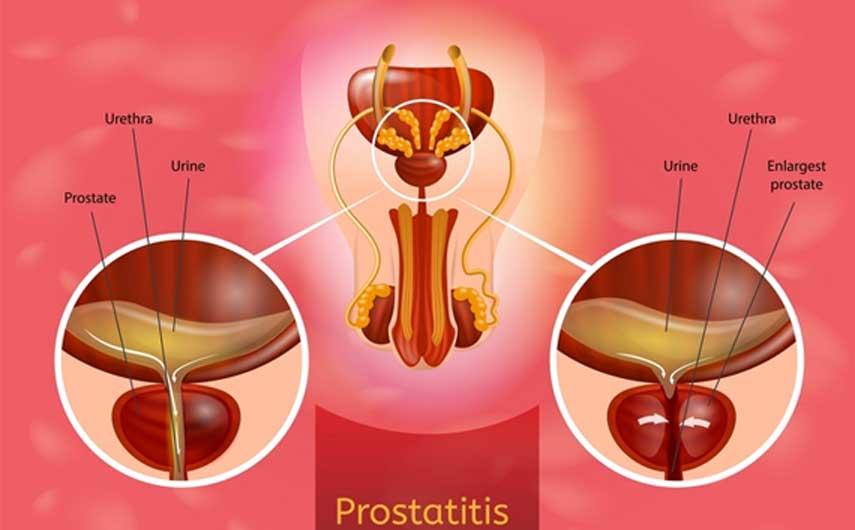
CAUSES OF PROSTATITIS : Natural treatment
WHAT BRINGS ABOUT PROSTATITIS?
The prostate is a walnut-sized gland that all men have. It is located under your bladder and in front of your rectum. The job of the prostate is to make a fluid that contains semen. This fluid protects the sperm as they travel to a woman's egg.
If your prostate becomes swollen, painful, and inflamed, you have a condition called prostatitis.
The Prostatitis is the infection, acute or chronic, prostate (gland located below the bladder, found only in humans). In some cases of chronic prostatitis, no causal germ is found on examinations. This is called chronic non-bacterial prostatitis. Any urinary tract infection accompanied by fever in men is prostatitis, except pyelonephritis (kidney infections).
The chronic prostatitis is the result of urinary tract infections repeated. The prostate is an anatomical crossroads between the urinary tract and the male genital tract. Any prostatitis can therefore be the consequence of bacterial contamination of the urethra, but also of an infection of the entire urinary tract (bladder, ureters, kidneys).
The most common prostate diseases are cancer, adenoma (benign enlargement of the gland) and prostatitis. This is characterized by acute or chronic infection of the prostate. It can affect men of all ages, with a predominance around 30 or 40 years old, unlike cancer or adenoma that affects older men.
It's not cancer, and it's different from an enlarged prostate. Here is the natural herbal treatment to cure prostatitis and increase fertility.
NATURAL TREATMENT FOR PROSTATITIS
This natural treatment to permanently and quickly cure prostatitis that we offer is composed of two elements: a herbal tea and an ointment. It also helps relieve urinary symptoms, including those caused by an enlarged prostate without having to have an operation. It works in particular by reducing the swelling of the prostate gland and providing immense relief. The natural treatment also helps cure urination difficulties and it restores sexual balance. So this is the secret to cure prostatitis by plants without surgery and without side effects.
CLICK HERE TO GET THIS PRODUCT!!
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
So in the rest of this article we will list the causes of this condition.
Prostatitis is a group of diseases affecting the prostate that present with similar symptoms such as pain or discomfort in the perineal region and genitourinary tract.
The condition is not always caused by an infection and there is not necessarily inflammation of the prostate. Prostatitis can be divided into four categories:
- Acute bacterial prostatitis : This is an acute infection of the prostate.
- Chronic bacterial prostatitis : This is due to poorly treated acute prostatitis or recurrent urinary tract infection.
- Chronic non-bacterial prostatitis or chronic pelvic pain syndrome : Symptoms of prostatitis are present, but infection is not the cause. It can be taken with or without inflammation.
- Asymptomatic inflammatory prostatitis : Infection and inflammation occur, but there are no symptoms.
In cases where prostatitis is caused by bacterial infection, the diagnosis is simple, and in its acute form, treatment is effective. However, in chronic non-bacterial forms, the origin is not entirely clear, so diagnosis and treatment are complicated.
Prostatitis can cause problems with sexual activity and infertility in men.
Causes and risk factors of prostatitis :

Different factors may be involved: food, urine, sex, influence of stress, sports practice including cycling ... Chronic bacterial prostatitis is the most common cause of recurrent urinary tract infection in men and 5 to 10 % of all prostatitis.
Prostatitis is sometimes the consequence of sexual contamination (sexually transmitted disease). But very often, no triggering factor is found.
In the elderly, prostatitis is frequently the consequence of a urinary infection , itself secondary to an enlarged prostate which promotes urinary stasis. We then speak of adenomitis.
To be more specific Prostatitis can affect men of all ages, but it is more common in young and middle-aged men. Other risk factors for the development of prostatitis are:
- History of prostatitis
- Have a recent urinary tract infection
- Recent use of a urinary catheter or recent urologic procedure
- Enlarged prostate gland
- Having rectal sex
- Structural or functional abnormality of the urinary tract
- Dehydration (not enough fluid)
- Trauma or injury to the local pelvis such as cycling or horseback riding
Acute prostatitis is caused by bacterial damage. Chronic prostatitis can be bacterial or non-bacterial, inflammatory or non-inflammatory. Different factors may be involved: food, urine, sex, influence of stress, sports practice including cycling ... Chronic bacterial prostatitis is the most common cause of recurrent urinary tract infection in men and 5 to 10 % of all prostatitis. Chronic non-bacterial prostatitis is the most common prostatitis. Although other, rarer problems can affect the prostate, the most common are prostatitis, benign prostatic hyperplasia, and cancer.
Prostatitis is inflammation of the prostate, often due to a bacterial infection. Most often, it is the E. Coli bacteria that is involved (more than 80% of cases).
Most of the time, acute prostatitis is due to a bacterial infection of urinary origin. The most frequently encountered germ is the bacterium Escherichia coli. The contamination can be sexual, but this is infrequent. Infection can also appear when urine is stagnant in the bladder due to the presence of an adenoma that blocks the complete emptying of the bladder. More rarely, an infection can occur following the insertion of a urinary catheter or a prostate biopsy (removal of a fragment of the prostate to analyze it). Chronic prostatitis (which lasts at least 3 months), which corresponds to a significant inflammation of the prostate, often results from acute prostatitis that is poorly treated or recurrent. Acute bacterial prostatitis is often caused by common bacterial strains. The infection can start when bacteria in the urine get into your prostate. Antibiotics are used to treat the infection. If they do not kill bacteria, prostatitis may recur or be difficult to treat (chronic bacterial prostatitis).
Nerve damage in the lower urinary tract, which can be caused by surgery or trauma to the area, could contribute to prostatitis not caused by bacterial infection. In many cases of prostatitis, the cause is not identified.
Prostatitis being a seminal infection; the latter are invasions of pathogenic microorganisms that occur somewhere in the male reproductive and urinary tract, so that they may be present in seminal fluid. They can affect the testes, causing orchitis, the epididymis causing epididymitis, or prostatitis if it occurs in the prostate.
In the path that sperm and seminal fluid must follow to go outward, contact with the infected area will take place, which can impair the ability of the sperm to fertilize the egg. Inflammation from the infection can cause a blockage and prevent semen or ejaculate from coming out.
Likewise, It can also result from various sexually transmitted organisms such as Neisseria gonorrhea, Chlamydia trachomatis or HIV (learn how to eat right with AIDS). The other organisms responsible for the infection are the same as those most often found in urinary tract infections, such as Escherichia coli. In many cases (especially in the chronic form of prostatitis), no specific cause for prostatitis can be found.
CLICK HERE TO GET THIS PRODUCT!!
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
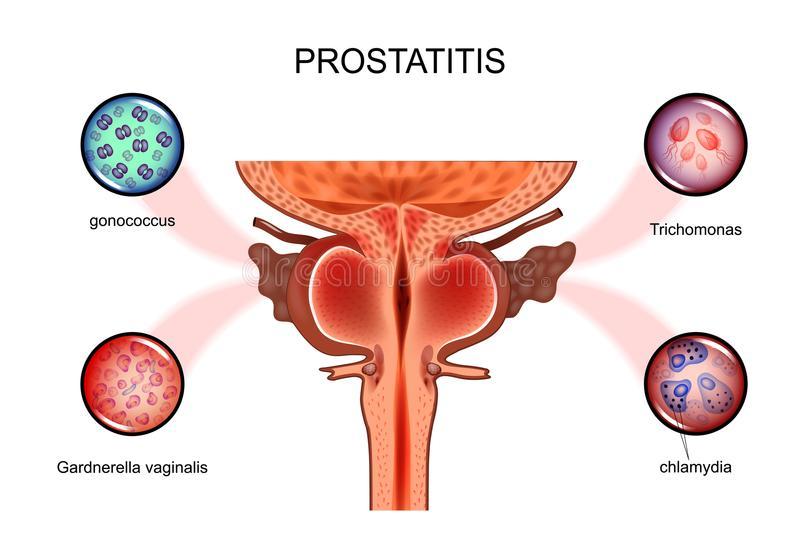
RELATIONSHIP BETWEEN PROSTATITIS AND CHLAMYDIA: Natural treatment
Relationship Between Prostatitis and Chlamydia
Some people with chlamydia have difficulty getting or keeping an erection, which is commonly called erectile dysfunction. This difficulty arises when chlamydia infects the prostate and resulting in prostatitis. Here is a natural treatment of herbal medicine to permanently cure prostatitis. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
What is Prostatitis?
Prostatitis chronic bacterial is a rare disorder that causes recurrent infection in the prostate and causes swelling, inflammation and infections frequent urinary tract. The prostate is a small gland located directly below the bladder in men.
Even with prolonged antibiotic treatment, bacteria can still survive in the prostate, and symptoms often return.
Treatment
If you suffer from prostate problems (inability to urinate, urination disorders, erectile dysfunction, premature ejaculation, lower back pain and penile pain, etc.), this is the miracle solution that will help you cure or prevent your prostatitis. The natural remedy to cure prostatitis permanently and quickly that we offer is composed of two elements: a herbal tea and an ointment. Generally, with the exception of the diagnosis too late, our natural treatment makes it possible to treat prostatitis quite easily and does not leave any sequelae. So trust us! This natural treatment is the secret to cure prostatitis without operation, without side effects thanks to plants.
Herbal tea is made from plants that have anti-inflammatory, astringent, antibacterial and calming properties. It works in particular by reducing the swelling of the prostate gland and providing immense relief. This natural remedy also contains several natural anti-inflammatory compounds that inhibit the inflammatory process that triggers inflammation and pain in the prostate gland. It also helps relieve urinary symptoms, including those caused by an excessively large prostate without having to have an operation. The natural remedy also helps in curing difficulty in urinating and it restores sexual balance. So this is the secret to cure prostatitis with plants.
First, the pain in your lower back and in your penis will gradually disappear. You will no longer have difficulty urinating and your erection will gradually return to normal. The use of herbal products to cure prostatitis gives excellent results. Our therapy to cure prostatitis that we offer is effective, fast, long-lasting. So; it will save you from having to go through an operation. Herbal tea to treat prostatitis has no side effects, either on the body or on health. Our natural treatment is secure. So this is the secret to cure prostatitis without operation and without side effects.
To discover our natural remedy to cure prostatitis, click here
What is Chlamydia?
Chlamydia is a sexually transmitted infection (STI) that can cause long-term health problems. Many people with chlamydia have no symptoms and are unaware that they are infected.
If left untreated, chlamydia can lead to:
Chronic prostatitis in men causing pain and erectile dysfunction
An increased risk of contracting HIV
Permanent infertility in women and a painful condition called pelvic inflammatory disease
Does chlamydia cause prostatitis?
Chlamydia can infect the prostate, causing a complication called prostatitis, which can lead to ED.
If chlamydia gets into the genital tract, it can spread to nearby organs. In men, the Chlamydia bacteria can infect the urethra, the tube that carries semen out of the body. Over time, bacteria can travel through the urethra to the prostate.
If the prostate becomes infected and inflamed, blood flow to the penis may be restricted, which can make it difficult to get or maintain an erection.
Symptoms of chlamydia
Chlamydia often does not cause any symptoms. In some people, symptoms appear several weeks after the initial infection, and then one person may have passed on chlamydia to another person.
When chlamydia causes symptoms, they can include:
A burning sensation when urinating
Discharge from the penis or vagina
Pain or swelling in the testicles, which is less common
Symptoms of prostatitis
Prostatitis can cause the following signs and symptoms:
Presence of blood in the urine (hematuria) or semen
Burning sensation or pain during urination
Difficult or painful ejaculation
Urethral discharge
Pain or discomfort in the genitals, groin, lower abdomen or lower back
Pain or feeling of pressure in the rectum
Need to urinate often (frequent urination)
Very urgent need to urinate (urgent urination)
Reduced urine stream
Difficulty urinating
Fever, chills and muscle pain
Recurrent urinary tract infections
Sexual problems and loss of libido
How is prostatitis diagnosed?
To make a diagnosis, your doctor will take your medical history and do a physical exam to look for swollen lymph nodes near the groin or for fluid discharge from the urethra.
Your doctor will also do a rectal exam to examine the prostate. During this test, your doctor will insert a lubricated, gloved finger into your rectum to look for signs of infection, such as a soft prostate or an enlarged prostate.
Your doctor may also perform the following tests:
• test urethral fluid for bacteria
• tests to rule out a sexually transmitted infection
• urine test
Medical treatment
Antibiotics are the main treatment for this condition. They are usually taken for four to six weeks. However, as the infection may come back, you may need to take antibiotics for 12 weeks or more. Your doctor will arrange for a follow-up after treatment to make sure the infection is completely gone.
It can take six months to a year for symptoms to go away completely. In the meantime, some home remedies may be able to ease your symptoms. Home remedies include:
• hot baths
• drink 64 to 128 ounces of water per day
• use fabric softeners to avoid constipation
• avoid alcohol, caffeine, citrus juices and hot and spicy dishes
• medicines to treat pain
Additional treatment may be necessary in the following rare cases:
• If you cannot pass urine, a health care provider will insert a tube called a catheter to empty your bladder.
• If you have an abscess, your doctor will drain it.
• If you develop sepsis, you will receive intensive antibiotic therapy and will have to stay in hospital.
• If you have stones or mineral deposits in your prostate, your doctor may need to remove your prostate. It's very rare.
Tips to follow if you have prostate cancer
When you are suffering from chronic bacterial prostatitis, certain lifestyle changes can be of great help. Here are the tips to follow:
–Drink plenty of water. Ideally, you should drink at least 1.5 liters of water per day. Fluid intake helps the metabolic process to function well.
-Avoid excessive consumption of alcohol and tobacco. They can irritate your bladder and especially make your symptoms worse.
-Eat healthily, especially avoid foods that are too sweet and fats. Eat lots of fruits and vegetables
-Avoid sitting in a sitting position for too long. But in the event that this is unavoidable, favor a comfortable seat
-Regular moments of relaxation and sufficient sleep are also essential.
-Avoid any other activity that generates pressure on the perineum that accentuates symptoms, for example, cycling.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
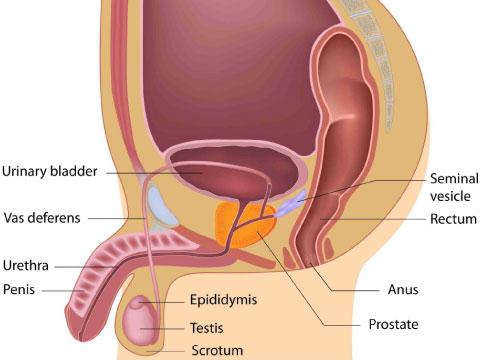
CHRONIC PROSTATITIS NATURAL TREATMENT
CHRONIC PROSTATITIS NATURAL TREATMENT
Infection of the prostate gland. Germs can come from outside through the urethra or come in through the blood. It can be due to endoscopic investigations, the introduction of instruments through the urethra to the bladder.
There is an acute form and a chronic form, with the presence of small abscesses, often due to an acute form that is poorly treated. Chronic prostatitis is not necessarily the sequel of acute prostatitis but of a recurrent urinary tract infection. Discover the natural treatment based on medicinal plants to cure prostatitis permanently without operation. Click on the image below to discover this natural treatment.
Our natural remedy is made of plants effective in treating prostatitis and some other male sexual problems. We have selected the best plants Africa had to offer to treat prostatitis.
To contact our experts please call or write to us on the following number, tel / WhatsApp
+22996374527
WE DELIVER ALL OVER THE WORLD
The functional disorders from there one would be defined by the term "prostatism" which includes: pollakiuria, dysuria, urgent urination.
If natural solutions exist, let's be clear: we are not kidding with prostate pathologies. Therefore, in cases of prostatic adenoma with acute urinary retention (RAU, in short, one can no longer urinate), or cancer of the gland, it is not allowed to stop allopathic treatment for natural therapeutic strategies. They can, however, be perfectly complementary.
Furthermore, we keep repeating it, self-treatment and self-medication are to be avoided. A true naturopath, or any health worker worthy of the name, is a professional who establishes sensitive protocols adapted to each case and each patient. However, the rules that we are going to advise you to follow our common sense and will give you an idea of the remarkable range that complementary medicines offer.
Some tips to get rid of prostatitis
Tobacco is taboo

First of all, it should be noted that losing weight is a prerequisite. As in many cases, being overweight weighs (no pun intended) on the health balance. A diet too high in calories increases all types of cancer, especially prostate cancer. Studies have shown that reducing calorie intake has a beneficial effect on prostate cancer.
Eliminating tobacco is also obvious. In smokers, prostate cancer - which is, as we have said, a slowly growing cancer - is more aggressive and more advanced than in non-smokers. Tobacco increases the risk of developing prostate cancer by 30%. In addition, smoking stimulates the growth of prostate cells. In question, the cadmium contained in the volutes.
Food

For effective food reform, the indications are often the same. It is therefore advisable to favor a balanced diet in proteins, carbohydrates and lipids, of organic quality, seasonal (and therefore adapted to each of them), and according to the needs of each one. Fruits and vegetables, therefore, rich in vitamins, minerals, and antioxidants, and fibers. If possible, we will prepare and consume these products as less cooked as possible to preserve the nutritional elements they contain and thus ensure optimal bio-assimilation. (except in certain cases, such as in people suffering from colitis, who will favor fruit or vegetable juices).
Avoid saturated animal fats and prefer unsaturated fats. We recommend consuming mackerel, sardines, herring, walnuts and first cold-pressed virgin and organic vegetable oils for the lipids essential to our cells. For zinc, opt for almonds and pumpkin or squash seeds, but also oysters and brewer's yeast. Zinc has the advantage of inhibiting the activity of the 5-alpha reductase enzyme which allows the transformation of testosterone into dihydrotestosterone, responsible for the enlargement of the prostate. Limit dairy products.
Herbs That Relieve Infectious Prostatitis
The many virtues of plants are often overlooked by patients who systematically go to a doctor at the first signs. In fact, it is possible to relieve yourself with plants when you have infectious prostatitis.
First make sure that there are lots of fruits and vegetables in your diet, especially:
> The broccoli, the cabbage flower or spinach.
> Apples, olives, black cherries, berries, citrus fruits, and grapes go a long way in reducing the signs of prostatitis, as these fruits are rich in quercitrin: an anti-inflammatory plant compound.
As far as plants are concerned, the seeds of squash have proved their worth in restoring hormonal balance through their action on the muscles of the bladder.
Palmetto plants in preparation reduce pain, while poplar regulates prostate, and penis gold regulates the kidneys.
Professionals also recommend nettle which helps to treat urinary tract dysfunctions: difficulty urinating, poor urine flow. The roots and leaves of nettle combined with opuntia and small-flowered fireweed flowers facilitate urination.
Hay flowers also have positive effects on the prostate.
To talk more about nettle:
Nettle roots

Stinging nettle or stinging nettle (Urtica dioica ) is often cited for its anti-inflammatory properties and for preventing the growth of prostate tissue. For this indication, it is the root that is used, especially at the beginning of the disorders, because it would make it possible to slow down the evolution of the adenoma and to reduce the frequency of urination. If the quality of scientific studies in this area is sometimes deemed insufficient, the European Commission, as well as the WHO (World Health Organization), nonetheless recognize as "clinically established" its use in "the treatment of urine emission problems associated with mild to moderate benign prostatic hypertrophy, when the absence of prostate cancer is proven". Doctor Jean-Michel Morel, who teaches herbal medicine at the faculty of Besançon, recommends nettle roots in the form of EPS (in pharmacies) at the rate of a teaspoon of 5 ml in the evening before meals in a glass of water. We can also consider consuming the roots in decoction (one teaspoon of dry roots per cup of water to boil for 5 minutes then let infuse 10 minutes, three times a day).
Saw palmetto and African plum

Frequently associated with nettle, saw palmetto or Florida palm ( Serenoa repens Small), formerly known as Sabal serrulata, is the other plant associated with the prostate and urination disorders in herbal medicine. It is the fruits of this small palm tree from the United States that are used and presented in the form of medicine. More than ten studies demonstrate its effects on the frequency of urination (and nocturnal awakenings). The bark of the African plum ( Prunus Africana ) has similar effectiveness, but this large tree native to Madagascar is said to be endangered, and for this reason, it is best to turn to Florida's palm.
Fireweed

This beautiful pink flower, common in the Alps, shows promise for treating an enlarged prostate. Dr. Kurt Hostettmann, a leading phytomedicine researcher, tells how he discovered their properties: "At the age of 65, my own father had problems with urination and he refused the prostate surgery he was offered. I had read that Maria Treben, an Austrian herbalist, recommended this plant, as she had observed in entrenched valleys of Austria. that it was consumed in herbal tea, as a tea substitute, and that prostate surgery was much less important there than elsewhere. It wasn't based on any scientific study, but I suggested my father try it. What he did. Morning and evening he took his fireweed infusion, and after three to four weeks his nighttime urination decreased markedly. He never had prostate problems again until his death nearly twenty-five years later. "On the strength of this first experience, Dr. Hostettmann then entrusted this subject of his doctoral thesis to one of his young collaborators. .
Fireweed was effectively effective in fighting prostate adenoma, limiting the number of urinations, strengthening the urinary stream and flow, by the same mechanism as that of current synthetic drugs (inhibition of 5-alpha reductase, the enzyme responsible for hypertrophy). The active ingredients of the plant are mainly present in the tannins, which are soluble in water. Hence its effectiveness in the form of herbal tea (for example 20 days per month). There are several varieties of fireweed, and the recommended ones are the fireweed ( Epilobium parviflorum Schreb) because they contain as many active ingredients, but less tannins, which could in the long run irritate the stomach. Some research suggests the usefulness of fireweed against prostate cancer cells, but this remains to be confirmed.
Pumpkin seeds

Finally, pumpkin seeds are also frequently cited to reduce the symptoms of benign prostate adenoma and are well known to Germans for this property. They are easily found in any store, and if their virtues on the prostate are not fully established, their richness in nutrients makes them an interesting health food to consume daily.
Against prostate cancer: coffee and tomatoes


No plant to date can accompany or cure prostate cancer. On the other hand, in prevention, a large study carried out among 48,000 people by the National Cancer Institute was able to establish that consumption of 6 cups of coffee per day reduced the risk of 60% of being affected by cancer of the prostate. Unfortunately, consuming so much coffee daily is not reasonable: in addition to a phenomenon of dependence, excess caffeine causes many side effects, such as nervousness, restlessness, anxiety, palpitations, insomnia, stomach irritation. , diarrhea ...
The good news, decaffeinated offers the same virtues. It is indeed the polyphenols in coffee, and not caffeine, which gives it these preventive properties. A similar study published by the same institute also showed that consuming cooked tomatoes two to three times a week reduces the risk of developing prostate cancer by a third (compared to occasional consumption). Finally, a healthy lifestyle remains effective prevention: avoiding exposure to toxic products, including pesticides (farmworkers are more exposed to this cancer), being active and limiting the consumption of red meat, cold meats, and cheeses, fatty, while favoring large rations of fruits, vegetables and fish.
Some other plants that help with prostate problems
- BUCHU: This plant comes from Africa and is considered a urinary antiseptic. It contains an oil that increases urine production
- Chamomile: An infusion or tea is believed to have calming effects on cramps or painful symptoms in the genitourinary system. Combines well with valerian and marshmallow.
- Garlic: Good for spasms and cramps. Combines well with Echinacea and Goldenseal to treat microbial activity.
- Cramp Bark: Bark Has antispasmodic, sedative, nervine and astringent properties. Designed to have potent antispasmodic effects on the genitourinary system in both men and women.
- Pumpkin Seeds: Pumpkin seeds are a natural source of zinc and linoleic acid (vitamin F). It is believed to play an important role in decongesting the prostate and reducing residual urine.
- Watermelon Seeds: Help prevent excessive urine buildup due to prostatitis and BPH. Works well with Uva Ursi and Buchu.
To contact our experts please call or write to us on the following number, tel / WhatsApp +22996374527
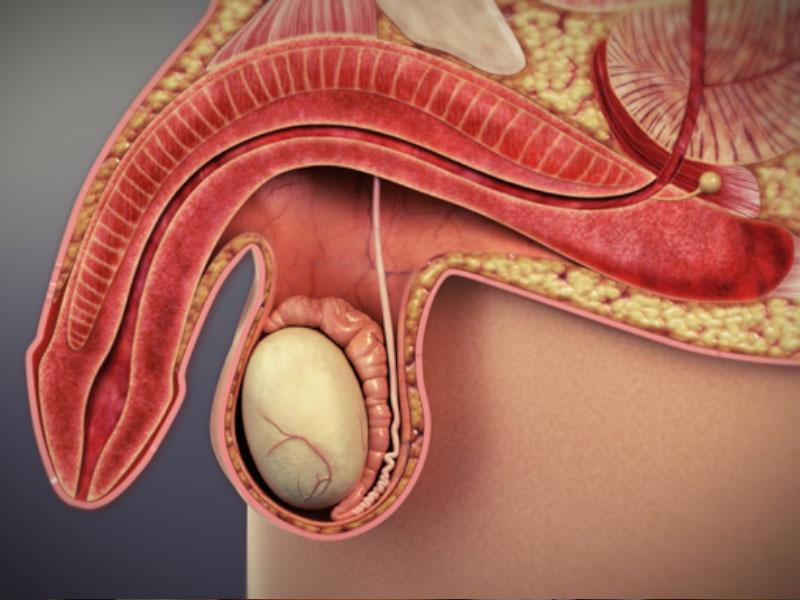
SOFT ERECTION NATURAL TREATMENT
ERECTION MOLLE NATURAL TREATMENT
When it comes to soft erection There are many causes that can lead to the inability of the penis to erect normally such as serious illnesses and psychological factors. All men with a weak erection problem show different causes and it is important to identify them correctly in order to apply the right treatment.
Therefore and in order to help you and completely eradicate these genes, the Health experts of Dawabio after much research offers you a very effective solution based on medicinal plants to treat a soft erection. Click on the image below to discover this natural treatment

We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
RECALL :
It is very important for men with impotence and other health problems to consult a doctor first to know the real state of your health and what will be the most appropriate treatments.
Usually, a flabby penis occurs in older men as they tend to have serious conditions like diabetes, kidney failure, high blood pressure, atherosclerosis, cardiovascular disease, and multiple sclerosis.
These diseases affect the nerves and also the circulation of blood to the penis. That is why, when you visit a doctor to discuss an impotence problem, he will ask you to examine your general health, as any of the slightly higher diseases can cause this sexual problem.
In the rest of our article we will outline some natural soft erection treatment.
1: Red vine, ginseng
If the erection gradually becomes poorer, without there necessarily being a drop in libido, and if the spontaneous erections in the morning or at night disappear, this often indicates a vascular cause. In this case, we can bet on circulatory plants such as sweet clover, red vine, witch hazel, horse chestnut ... We use them alone or in synergy (Quatuor Circulation, Super Diet; Nat & Form, etc.). 6 capsules per day or 5 ml of glycerine macerate (Phytostandard, Phytoprevent) morning and evening, for at least a month to treat sexual weakness or soft erection.
2: The "vegetable Viagra"
Tribulus Terrestris (also called " vegetable viagra ") and mucuna are two plants that act on the erection by promoting the production of testosterone. "This association is useful in the event of significant erectile problems associated with a decrease in libido", specifies the specialist.
Dosage: To be taken in the form of a glycerine macerate, 5 ml morning and evening as a minimum 3-month cure to see results.
3: Patchouli or pine essential oils
Essential oils with vasodilating virtues (pistachio lentisk, patchouli, palmarosa ...) can promote erection. Other oils with testosteronergic action can also help restart the machine if the problem is accompanied by a drop in libido: Scots pine, cumbawa, black spruce, Siam wood ... Aromatherapy can help. elsewhere be associated with herbal medicine to cure sexual weakness or soft erection.
4: A dietary supplement based on amino acids and vitamin B3
The combination of amino acids (l-arginine and l-carnitine) and vitamin B3 increases the production of nitrogen monoxide, thus promoting the vasodilation necessary for an erection. "The advantage is that you can take this dietary supplement continuously, to cure sexual weakness or soft erection. There is no need to plan the intake before sex, which helps keep sexual spontaneity This is interesting for those who experience a small decrease in libido which is accompanied by a decrease in erectile capacity but do not want or cannot take drugs such as Viagra, Cialis ... for medical reasons ", summarizes Annabelle Pongratz Muller-Vitu. It is in the form of sachets of powder to be diluted in water (Ezerex), in a cure of a one-month minimum.
5: An ylang-ylang massage
The psychic aspect of the erection is not to be neglected. "Tenderness, touch, caresses ... and the atmosphere of relationships are very important to restore dialogue and trust within the couple," recalls the sex therapist. To create favorable conditions, we can for example try to be massaged by (and massaged) his partner with a vegetable oil in which we dilute a few drops of essential oil, to be chosen for its fragrance, according to the smell that we feel. "talks" the most. Some ready-made massage oils (Light of Love massage oil, Essential Elements; Sensory Awakening massage oil, Puressentiel) contain essential oils known for their intoxicating and aphrodisiac fragrances: sandalwood, ylang-ylang, ... On the other hand, the essential oil will have no real therapeutic action by the cutaneous route.
6: A good workout
Sport is the number one ally of erection: it promotes good vascular health, improves self-esteem and endurance, lowers stress, helps fight against abdominal obesity which is very bad for the body. 'erection ", notes the specialist. No need to do much: 30 minutes 3 times a week already allow good maintenance at the cardiovascular level, which can only have a positive impact on the erection. help quickly find solutions to sexual weakness or your soft erection.
In general, a healthy lifestyle promotes a good erection and certain "enemies" should be avoided: alcohol, tobacco, cannabis.
Also to finish here are some foods that help treat erectile dysfunction :
· Dark chocolate: Yes, you read that right! Dark chocolate is an aphrodisiac and has many health benefits. It helps lower levels of the stress hormone cortisol and contains high levels of phenethylamine, a relaxing chemical that can also increase sexual pleasure. If all that wasn't enough, dark chocolate cocoa is rich in flavonoids; vasodilators that facilitate blood flow to the penis, and thus improve sexual weakness or soft erection.
· Bananas: Often embarrassing when eaten in public due to their resemblance to an erect penis! The fruit is very rich in potassium which is very beneficial for the heart and maintains good blood circulation, which is obviously essential for a strong erection. Potassium will also help maintain normal sodium levels and reduce the risk of high blood pressure. Bananas are also an excellent source of vitamin B and thus maintain your energy level and testosterone production, leading to higher libido.
· Chillies: Keep the heat with the chili in your sex life! Have you ever felt a rush of blood in your face and redness of the skin while eating chili peppers? This is because they work effectively to dilate blood vessels, and luckily not just on your face. When it comes to sex, they also do wonders by pumping more blood into the penis, and they work very quickly. However, it doesn't over-consume it, as it can irritate your stomach and intestines.
· Salmon: This is a fantastic food for weight loss because the fish generally do not contain carbohydrates and are perfect when combined with vegetables. Salmon is also good for the penis and thus may improve sexual weakness or flabby erection. Omega-3 fatty acids in oily fish help improve the functioning of your nervous system and promote healthy heart and blood circulation. towards the penis because of the enormous cardiovascular benefits they provide.
· Watermelon: This fruit has been shown to be a natural food similar to Viagra. The drug Viagra works by helping to relax and widen the blood vessels in the penis, allowing an easier erection when you are sexually aroused. Many experts claim that watermelon (or watermelon) works in a similar way due to the presence of "citrulline". Citrulline stimulates the production of arginine, an amino acid that helps relax and dilate blood vessels, thus improving blood circulation just like Viagra does.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
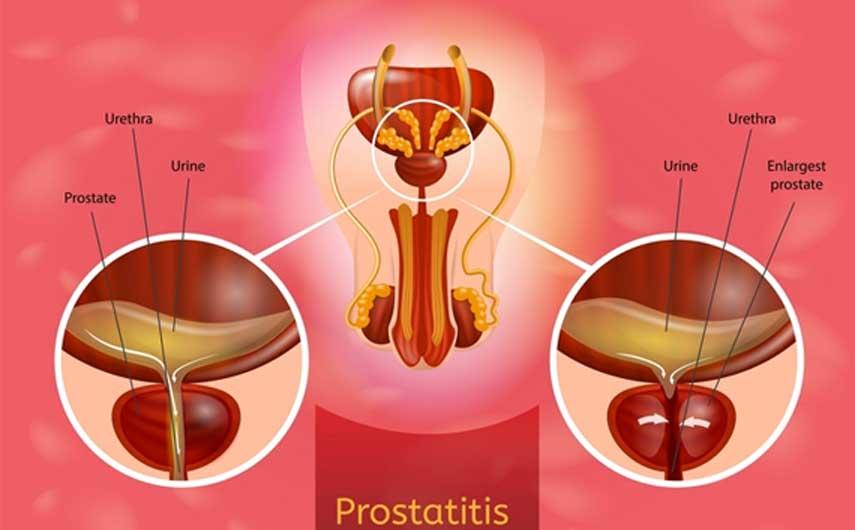
GRAND MOTHER'S PROSTATITIS REMEDY: Natural treatment
GRAND MOTHER'S PROSTATITIS
Prostate cancer occurs in the later stages of inflammation of the prostate, a common result after untreated prostatitis. Men who ignore prostatitis are actually risking their lives. If you want to live long and be healthy, if you need an erection and a normal libido, you must treat the inflammation of the prostate. And it should be done as soon as possible. Here is the natural treatment from the experts at Dawasanté to cure prostatitis permanently. Click on the image below to discover this natural treatment.
It should be understood that prostatitis is a fatal disease that can escalate and lead to a cancerous tumor. The untreated and misdiagnosed disease develops rapidly and can lead to cancer in just 1 to 2 years and often leads to the death of the sufferer
The bad news is that in 96.7% of cases, men who suffer from prostatitis suffer from sexual weakness sooner or later.
Now let's look specifically at the most effective natural treatments for treating prostatitis and for prostate health in general.
Natural remedies, easy to find and use, effective not only because they reduce inflammation, but also because they are able to " deflate the prostate ", thus countering the problem of benign prostatic hypertrophy. , significantly improving urine flow and thus facilitating urination.
Some of these remedies are therefore also useful for the strong antibacterial and immunostimulating properties, which are very useful in cases of prostatitis of bacterial origin.
These remedies can be taken alone or all together.
If you are already taking medication for prostatitis (or other illnesses), before taking any of these herbs, or any supplement, I strongly advise you to consult your doctor.
To remedy this we offer you some solution related to certain plants and your food
1 - aloe juice
Aloe, from a phytotherapeutic point of view, is without a doubt one of the most complete and effective natural remedies, so much so that it can be used to treat and prevent an endless number of diseases. Prostatitis is no exception.
Due to its rich assets (vitamins, minerals, flavonoids, amino acids, anthraquinones, polysaccharides, etc.), Aloe has antimoral, immunostimulatory, anti-inflammatory, antibacterial, antifungal and antiviral properties.
Oral consumption of aloe juice helps reduce inflammation of the prostate and bladder, shrinks the size of the prostate, and effectively neutralizes bacterial infections.
There are several varieties of Aloe, the one with the most active ingredients is definitely Aloe Arborescent (not Aloe Vera!).
This plant uses leaves which, after removing the thorns, must be mixed with honey and a little grappa (or other distillate). The result is a greenish and frothy juice, slightly bitter and rich in healthy properties.
2 – Epilobium
Epilobium is the quintessential prostate herb, as it has been used for over a century in traditional medicine to specifically treat all diseases that affect this gland, such as prostatitis and prostatic hyperplasia. Indeed, soon after its consumption, the effects already begin to be felt, with greater ease to urinate and completely empty the bladder. Indeed, Epilobium exerts a rapid and effective anti-inflammatory action against the bladder and the prostate, while reducing the size of the prostate.
3 - Bee pollen
Bee pollen is a treasure trove of nutritious and healthy substances.
In fact, it contains 35% protein, 21 amino acids of 23, 35% carbohydrate, 5% fat (mostly unsaturated aids), all vitamins (except vitamins B4 and F), minerals and flavonoids. In fact, several studies confirm that consuming bee pollen is effective in fighting prostatitis and enlarged prostate, as it reduces pain and inflammation and inhibits the proliferation of prostate tissue.
4 - Root and nettle leaves
Nettle (Utica dioica) is another natural remedy commonly used in the treatment of prostatitis.
A study was recently published in 100 patients with benign prostatic hyperplasia, where the effects of nettle on reducing the size of the prostate are confirmed. The leaves of root and nettle are used to treat prostate problems. With the leaves, you prepare an herbal tea (simply let the leaves infuse for 10 minutes in hot water then filter). The root is used as a decoction instead. Nettle root is sometimes used in conjunction with saw palmetto. To further determine its effectiveness
5 - Pumpkin seeds
Pumpkin seeds have a long tradition in traditional medicine, in the treatment of intestinal worms as well as in the treatment of prostate disorders.
This is thanks to the very high zinc content.
In fact, zinc affects androgen metabolism by inhibiting the activity of the enzyme that converts testosterone to DHT, 5alpha-reductase. It is an androgenic hormone that is fundamental for the development and normal growth of the prostate. Nevertheless, it is also recognized that it is the cause of hyperplastic nodules of the gland, which can eventually lead to benign prostatic hyperplasia (BPH).
In addition, zinc reduces the secretion of prolactin, a hormone that activates a testosterone booster in the prostate. The higher the testosterone, the higher the production of DHT. By reducing the synthesis of prolactin, zinc also ensures lower DHT.
The seeds of pumpkin contain beta-sitosterol, a compound similar to cholesterol and present in some plants. Preliminary studies have shown that beta-sitosterol can improve urine flow and reduce the amount of urine left in the bladder after urination.
Some studies recommend taking 10 g of pumpkin seed extract per day for symptoms of BPH.
6. Pygeum (African plum extract)
Pygeum has also been shown to contain a wide range of fatty acids, alcohols and sterols, such as beta-sitosterol, which have an antioxidant and anti-inflammatory effect on the urogenital tract.
A few studies indicate that consuming 100 to 200 mg of Pygeum extract daily or splitting it into two doses of 50 mg twice daily may help reduce symptoms of BPH.
7. Saw Palmetto
Saw palmetto is one of the most studied and widely used herbal supplements to treat BPH.
Several studies have linked saw palmetto to reduced symptoms of BPH. This is probably due to the fact that it inhibits the production of testosterone and reduces the size of the inner wall of the prostate.
However, other studies have not been able to establish whether the use of a saw palmetto supplement has an impact on BPH symptoms compared to a placebo.
8. Zi-Shen Pill (ZSP)
The Zi-Shen (ZSP) pill contains a blend of three herbs, including Chinese cinnamon.
The formula comes from ancient Chinese medicine dating back to the 13th century. Trusted Source researchers showed that rats given the Zi-Shen formula exhibited reduced levels of BPH.
More research is needed in humans to determine its effectiveness.
9. Cernilton
Some people use herbal supplements made from rye pollen to treat symptoms of BPH. These bothersome symptoms may include the inability to empty the bladder completely and the need to urinate frequently at night.
Under the Cernilton brand, rye pollen is included in the formulation of several registered pharmaceutical supplements intended to alleviate the symptoms of BPH.
Despite its popularity, it has never been shown Cernilton had an impact on symptoms of BPH as part of scientific studies on a large scale. However, some indicate that it can help reduce the overall size of the prostate.
More research is needed to determine if it works or not.
10. Orbignya speciosa (babassu)
Babassu or Orbignya speciosa is a species of palm native to Brazil. Several indigenous Brazilian tribes and communities use the dried or ground kernels from the tree to treat urogenital symptoms and conditions.
Babassu nut oil has also been shown to be a source for inhibiting testosterone production, while other parts of the nut contain compounds with anti-inflammatory and antioxidant properties.
11. lycopene
Lycopene is a natural pigment found in many fruits and vegetables. One study has shown that it may help slow the progression of BPH.
Tomatoes are the richest source of lycopene available to most people. But a few other fruits and vegetables contain lower levels of this antioxidant.
Usually, the more pink or red the fruit or vegetable, the higher its lycopene content.
Other sources of lycopene include:
- Papaya
- pink grapefruit
- watermelon
- goyave
- carrots
- Red peppers
- apricots
- Red cabbage
12. Zinc
l has been shown that chronic zinc deficiency potentially increasing the likelihood of developing BPH. Taking zinc supplements or increasing dietary zinc intake can help reduce urinary symptoms associated with an enlarged prostate.
Zinc is found in poultry, seafood, and several types of seeds and nuts, such as sesame and pumpkin.
13. green tea
Green tea contains many antioxidants called catechins, which strengthens the immune system and possibly slow the progression of cancer the prostate.
It is important to keep in mind that green tea contains caffeine. Caffeine can stimulate the bladder and cause a sudden urge to urinate which can worsen the symptoms of BPH.
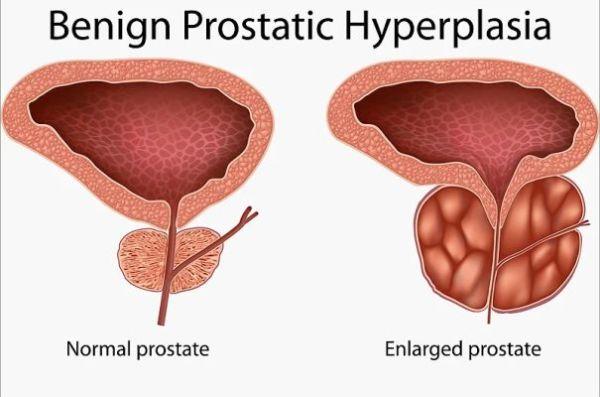
PROSTATIC HYPERTROPHY: Natural treatment
PROSTATIC HYPERTROPHY
An enlarged prostate is a common condition in men. An enlarged prostate can cause unpleasant urinary symptoms, such as blocking the flow of urine out of the bladder. It can also cause bladder, urinary tract, or kidney problems.
There are several effective treatments for prostate enlargement, including medications, minimally invasive therapies, and surgery. To choose the best option, you and your doctor will consider your symptoms, the size of your prostate, other health concerns, and your preferences. Visit the natural herbal treatment of Dawasanté experts to definitively cure the enlarged prostate. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Treatment
If you suffer from an enlarged prostate, here is the miracle solution that will allow you to naturally cure or prevent your enlarged prostate. The natural remedy to permanently and quickly cure the enlarged prostate that we offer is composed of two elements: an herbal tea and an ointment. Generally, with the exception of the diagnosis too late, our natural treatment makes it possible to cure the enlarged prostate quite easily and does not leave any sequelae. So trust us! This natural treatment is the secret to treating an enlarged prostate without operation, without side effects thanks to plants.
Herbal tea is made from plants that have anti-inflammatory, astringent, antibacterial and calming properties. It works in particular by reducing the swelling of the prostate gland and providing immense relief. This natural remedy also contains several natural anti-inflammatory compounds that inhibit the inflammatory process that triggers inflammation and pain in the prostate gland. It also helps relieve urinary symptoms, including those caused by an overly large prostate without having to have an operation. The natural remedy also helps in curing difficulty in urinating and it restores sexual balance. It is therefore the secret to cure hypertrophy of the prostate with plants.
First, the pain in your lower back and in your penis will gradually disappear. You will no longer have difficulty urinating and your erection will gradually return to normal. The use of herbal products to treat an enlarged prostate gives excellent results. Our therapy to cure the enlarged prostate that we offer is effective, fast, long-lasting. So; it will save you from having to go through an operation. Herbal tea to treat an enlarged prostate has no side effects, either on the body or on health. Our natural treatment is secure. So this is the secret to cure enlarged prostate without surgery and without side effects.
To discover our natural remedy to cure an enlarged prostate, click here
Symptoms
The severity of symptoms in people with an enlarged prostate varies, but symptoms tend to gradually worsen over time. Common signs and symptoms of an enlarged prostate include:
Frequent or urgent need to urinate
Increased frequency of nighttime urination ( nocturia )
Difficulty starting to urinate
Weak urine flow or flow that stops and starts
Dribble at the end of urination
Inability to completely empty the bladder
Less common signs and symptoms include:
Urinary tract infection
Inability to urinate
Blood in the urine
The size of your prostate doesn't necessarily determine the severity of your symptoms. Some men whose prostate is only slightly dilated may have severe symptoms, while others in those with a severely enlarged prostate may only have minor urinary symptoms.
In some men, symptoms eventually stabilize and may even improve over time.
The causes
The prostate is located below the bladder. The tube that carries urine from the bladder out of your penis ( urethra ) goes through the center of the prostate. When the prostate gets bigger, it begins to block the flow of urine.
Most men have continued to grow prostate in their lifetime. In many men, this continued growth enlarges the prostate enough to cause urinary symptoms or significantly block urine flow.
The cause of prostate enlargement is not entirely clear. However, it could be due to changes in the balance of sex hormones as men get older.
Risk factors
Risk factors for prostate enlargement include:
· Aging. An enlarged prostate rarely causes signs and symptoms in men under the age of 40. About a third of men have moderate to severe symptoms by age 60 and about half by age 80.
· Family history. Having a blood relative, like a father or sibling, with prostate issues means you're more likely to have issues.
· Diabetes and heart disease. Studies show that diabetes, along with heart disease and the use of beta-blockers, may increase the risk of an enlarged prostate.
· Way of life. Obesity increases the risk of an enlarged prostate, while exercise can lower your risk.
Complications
Complications of an enlarged prostate can include:
· Sudden inability to urinate (urinary retention). You may need to insert a tube (catheter) into your bladder to drain urine. Some men with enlarged prostate need surgery to relieve urinary retention.
· Urinary tract infections (UTI). The inability to completely empty the bladder can increase the risk of urinary tract infection. If UTIs occur frequently, you may need to have surgery to remove part of the prostate.
· Bladder stones. These are usually caused by an inability to completely empty the bladder. Bladder stones can cause infection, irritation of the bladder, blood in the urine and obstruction of its flow.
· Damage to the bladder. A bladder that has not completely emptied can stretch and weaken over time. As a result, the muscle wall of the bladder no longer contracts properly, making it more difficult for your bladder to empty completely.
- Renal lesions. The pressure of urinary retention in the bladder can directly damage the kidneys or allow bladder infections to reach the kidneys.
Most men with an enlarged prostate do not develop these complications. However, acute urinary retention and kidney damage can pose serious health threats.
Having an enlarged prostate is not thought to increase the risk of prostate cancer.
Diagnostic
Your doctor will start by asking you detailed questions about your symptoms and giving you a physical exam. This initial examination is likely to include:
· Digital rectal examination. The doctor inserts a finger into your rectum to check your prostate for enlargement.
· Test of urine. Testing a sample of your urine can help rule out infection or other conditions that can cause similar symptoms.
· Blood test. The results may indicate kidney problems.
· Blood test with prostate-specific antigen (PSA). PSA is a substance produced in your prostate. PSA levels increase when the prostate is enlarged. However, high levels of PSA can also be due to recent procedures, infection, surgery, or prostate cancer.
Transrectal ultrasound. An ultrasound probe is inserted into your rectum to measure and assess your prostate.
· Prostate biopsy. Transrectal ultrasound guides the needles used to take tissue samples (biopsies) from the prostate. Examining the tissue can help your doctor diagnose or rule out prostate cancer.
· Urodynamic and pressure-flow studies. A catheter is inserted into your bladder through your urethra. Water - or, less frequently, air - is slowly injected into your bladder. Your doctor can then measure the bladder pressure and determine how your bladder muscles are working. These studies are typically only used in men with suspected neurological problems and in men who have had a previous prostate procedure and still have symptoms.
· Cystoscopy A flexible, lighted instrument (cystoscope) is inserted into your urethra, allowing your doctor to see inside your urethra and bladder. You will be given a local anesthetic before this test.
Medical treatment
A wide variety of treatments are available for an enlarged prostate, including medications, minimally invasive therapies, and surgery. The best choice of treatment depends on several factors, including:
The size of your prostate
· Your age
Your overall health
The amount of discomfort or discomfort you feel
If your symptoms are tolerable, you may decide to defer treatment and just watch your symptoms. For some men, symptoms may improve without treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
PROSTATITIS FOODS: Natural treatment
PROSTATITIS FOODS
Prostate degeneration: a scourge for men
The cancer prostate is the most common cancer in men in Western countries. Each year, more than 40,000 cases are diagnosed in France. In addition, numerous studies carried out since the seventies lead to think that food is involved for 30 to 40% in the genesis of cancers in general. At the same time, and still in France, 70,000 men each year undergo an operation linked to benign prostatic hypertrophy.
Knowing that a number of dietary factors are involved in degenerative prostate disease, it is important for men to be vigilant about the contents of their plate. However, Dawasanté experts provide you with a natural herbal treatment to cure prostatitis.
NATURAL TREATMENT FOR PROSTATITIS
This natural treatment to permanently and quickly cure prostatitis that we offer is composed of two elements: a herbal tea and an ointment. It also helps relieve urinary symptoms, including those caused by an enlarged prostate without having to have an operation. It works in particular by reducing the swelling of the prostate gland and providing immense relief. The natural treatment also helps cure urination difficulties and it restores sexual balance. So this is the secret to cure prostatitis by plants without surgery and without side effects.
CLICK HERE TO GET THIS PRODUCT!!
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
The current literature abounds in articles on the relationship between certain foods and the occurrence of prostate cancer. Even more in the field of nutrition than in others, separating the chaff from the wheat is not easy. Knowing this, and although we can not confirm anything in the face of data which are still mostly at the research stage, it seemed useful to us to carefully list the foods most often incriminated today in degenerative disease. prostate.
Gentlemen, take care of your prostate
From 10 to 20% of prostate cancers could be prevented with a balanced diet. Extenso reviews with you the content of your plate ...
Foods to choose
Vegetables, more vegetables!
It's an indisputable fact: vegetables play a major role in cancer prevention. To enjoy their benefits, fill half your plate with vegetables. Vary the colors to take advantage of the different compounds they offer.
Also, although they are not all particularly colorful, vegetables belonging to the cruciferous family, such as cauliflower, broccoli, bok choy and Brussels sprouts also have anti-cancer properties. Consuming it at least 5 times a week could decrease the risk of developing prostate cancer.
Vitamin E and selenium

Selenium, which is found in rice, wheat, and Brazil nuts, would provide a protective effect. However, its effect would be seen especially in men who have low amounts of selenium in their blood.
Vitamin E, found in almonds, flax seeds, hazelnuts, safflower, corn and soybean oil would also be beneficial in prevention. Its role would be particularly effective in smokers and in those who have low amounts of vitamin E in the blood.
Broccoli, and more broadly vegetables from the cruciferous family, help prevent the onset of certain cancers including prostate cancer.

The broccoli isothiocyanates including sulforaphane, and ibérine that appear to act on the expression of genes (6). According to some authors, when a person develops cancer, certain genes are activated and others repressed in particular, and other crucifers such as Brussels sprouts contain; However, broccoli seems to stimulate genes that prevent cancer and slow down genes that facilitate its growth, by chemical modification of ligands.
- It is recommended to drink green tea daily. Its benefits are manifold. It contains catechins, an antioxidant substance that is said to help limit the development of tumors.
Other foods contain less lycopene: pink grapefruit, watermelon, papaya, guava, dried apricots, for example.
- The pomegranate. "It is less known but pomegranate juice is a real ally for the health of his prostate. You can drink a glass every day," says Professor Zerbib. The antioxidants present in the pomegranate fruit are said to be responsible for these benefits.
- Curcumin. Several studies have shown that curcumin has anti-tumor effects. "Consumption once or twice a week is sufficient," advises Professor Zerbib.
Regarding alcohol, it is better to be careful of white alcohols such as white wine, champagne and beer which promote urinary disorders and infections but have no direct effect on tumor growth.
The best prevention is early detection of prostate cancer for men who have risk factors, including family history.
Lycopene
Lycopene is a substance from the carotenoid family. It is a powerful antioxidant. The tomatoes are rich in lycopene. This lycopene is better assimilated in cooked tomatoes (tomato sauces, coulis, purées) than in raw tomatoes, except tomato juice which also offers good availability of lycopene.
But don't we say that cooking deteriorates certain food components, such as vitamins for example?
Certainly yes. Nevertheless, cooking seems rather beneficial to the antioxidant score, at least concerning the tomato.
Thus, its vitamin C content effectively decreases by cooking, but its concentration of phenols increases, so that the water-soluble anti-radical capacity increases.
Without being specific to prostate cancer, let us also point out a meta-analysis published in the Journal of the National Cancer Institute on 2/17/99, which shows that men consuming more than 10 times a week of tomato products have a 33 % lower risk of developing cancer compared to those who consume less than twice a week.
It is interesting to consume lycopene almost daily, in the form of vegetables and fruits.
Isothiocyanates
Polyphenols
Polyphenols are what give food color.
The polyphenols in tea would protect against prostate cancer, and in particular green tea, the daily consumption of which could reduce the occurrence of prostate cancer by around two thirds.
Certain authors nevertheless emphasize the fact of consuming preferably teas resulting from a culture free from phytosanitary products such as pesticides or heavy metals. It also seems logical to extrapolate this remark to all of our nutrients.
A recent study conducted by NutriNet-Santé cites coffee as a major source of beneficial polyphenols among the French.
The red wine is rich in Resveratrol is a polyphenol. The rougher the wine, the more resveratrol it contains. This substance is antioxidant, anti-inflammatory, and would have an estrogenic effect (inhibiting testosterone, a male hormone which has a proliferative action on the prostate). 4 glasses of red wine per week would slow the progression of the disease by 41%
Consuming 250 ml of pomegranate juice every day would reduce the occurrence of prostate cancer by 60%.
The fruits and vegetables are rich in polyphenols cancer-protective, but not specific for prostate cancer. It is from this observation, among other things, that the National Health Nutrition Plan recommended 5 fruits and vegetables per day.
A diet rich in soy would reduce PSA levels by 14%.
Soy contains polyphenols (genistein, family of isoflavones) which have an antioxidant and estrogenic role. Tofu, soy drinks and yogurts are rich in it. Although it is not a phenol, it is interesting to know that soybeans contain saponins, which are anti-inflammatory but above all anti-proliferation of tumor cells. Remember, however, as said above that the consumption of soy can have drawbacks (drop-in sperm, among others).
Omega 3
Omega 3s have an anti-inflammatory role. They also control testosterone. They are present in fatty fish, which by the way, also contain more vitamin D, which is also beneficial for the prostate, the more fatty they are.
The flaxseed oil, rich in omega 3 is currently under study. Flaxseed oil also contains lignans which give rise to phytoestrogens.
A study presented in June 2007 in Chicago on the occasion of the 43rd annual meeting of the American Society of Clinical Oncology showed a decrease in the proliferation of prostate cancer cells by 30 to 40% in men undergoing prostate removal in due to cancer and having previously consumed flax seeds.
The rapeseed oil has been the subject of controversy especially following an epidemiological study conducted at Harvard on a group of 50,000 physicians health professionals. According to this study, participants who consumed the most omega 3 had a higher risk of prostate cancer than those who consumed little!
While other studies say the opposite. For example, a large American prospective study conducted by the NIH (equivalent to Inserm) was published in August 2006. It involved 30,000 volunteers. She didn't find that men who consumed the most ALA (alpha-linolenic acid, omega 3) had more cancer.
Also contain omega 3: rapeseed, walnut, wheat germ oils.
Monounsaturated fatty acids
These good fats would be favorable to prostate tissue. It is about olive oil , peanuts, hazelnuts but also almonds and avocados as well as goose fat, duck.
Vitamin D
Men with above-average plasma vitamin D levels have a 45% lower risk of developing aggressive prostate cancer, according to a study by the American Society of Clinical Oncology. As a reminder, 90% of vitamin D is synthesized in our skin following sun exposure, the remaining 10% being found in our food of animal origin (eggs, non-skimmed dairy products, fatty fish, etc.).
On the other hand, we will see later that one should not abuse too fatty products.
Selenium
Selenium is a powerful antioxidant. 200 micrograms of selenium reduce the incidence of prostate cancer by 63%. But 400 micrograms of selenium have a reverse action by pro-oxidant effect!
The Brazil nut contains a lot of selenium. The garlic and broccoli are also well provided. The red onions also contain enough. Onion is a very interesting food against the occurrence of prostate cancer and other cancers, in particular by its content of phenols and flavonoids.
Lutein
Lutein is a carotenoid with antioxidant properties and capable of promoting apoptosis (programmed cell death, 100 times more common for tumor cells than for healthy cells).
The lawyer is particularly well endowed with it. It is in any case a food to recommend. An acetone extract of avocado inhibits the in vitro growth of both androgen-dependent and androgen-independent prostate cancer cells.
Consuming 50 grams of avocado per day would reduce prostate cancer mortality by 40%.
Other hypothetical protectors
Pumpkin seed oil is also sometimes cited still for its antioxidant action. It can be used mixed with other edible oils to season dishes.
Dietary factors that attack the prostate
The alcohol
The alcohol should be consumed in moderation. Alcohol seems to be involved in many cancers (16).
Fats
Industrialized products containing hydrogenated lipids should be consumed in moderation.
Products containing saturated and trans fatty acids should also be consumed in moderation.
Among the foods containing trans fatty acids, we can mention margarines , cookies , pastries , fried foods .
The red meats and cold cuts are often stigmatized by their intake of saturated fatty acids. However, red meats are not necessarily very high in fat. However, according to a study conducted in 2000, it still takes a daily fat consumption corresponding to more than 33% of the calories of the day to multiply by 3 the risk of prostate cancer.
While it is true that omega 3s are considered favorable to the prostate, it is accepted that omega 6s ( corn oil , walnuts, grape seed, sunflower, etc.) generally attack this prostate tissue.
It should be noted that obesity must be fought here as in the fight against other cancers: the risk of death from prostate cancer is doubled with a body mass index exceeding 30. The prostate is larger on average by 32% in the obese. In the same vein, and to fight cancer in general, you must avoid a sedentary lifestyle. A low calorie diet and moderate physical activity (30 minutes of walking per day) would reduce mortality by 10 to 30%. Be careful, however, not to overdo it: more than 2 hours a day has a pro oxidizing effect
Food supplements
According to some authors, the excess intake of antioxidants eliminates too many free radicals.
Free radicals are certainly responsible for the occurrence of cancer, but their presence is also useful in the elimination of cancer cells which are rich in them and which can be self-destroyed by this auto-intoxication. According to these authors, it is therefore necessary to avoid industrial antioxidant supplements, to stick to a good diet sufficiently supplying natural antioxidants. So be careful with "food supplements".
Preparation methods
The acrylamide promotes the onset of prostate cancer. This substance is found in crisps and breakfast cereals . This is linked to the cooking method.
The polyamines found in cold cuts in the form of nitrosamines during salting and smoking seem to promote prostate cancer.
In particular, it is known that polyamines increase PSA and bone pain from prostate metastases.
Overcooking, leading to the presence of polycyclic aromatic substances can be carcinogenic. Example with the blackening of overcooked meats.
Beware of excess!
It is likely that selenium and vitamin E taken in too much can have harmful effects on your health. It is therefore preferable to include foods that contain them in your diet rather than consuming them in the form of supplements. In fact, supplements have not been shown to help prevent prostate cancer.
Foods to eat in moderation
Fatty substances
A diet high in fat, especially animal fat, would increase the risk of developing prostate cancer. In addition, excess fat in the diet could lead to excess weight. Since excessive calorie consumption and obesity are two factors linked to a greater risk of prostate cancer, it is best to ensure that you meet your energy needs, without exceeding them.
Tips to limit harmful fats:
· Prefer cooking with steam, in the oven or on the grill rather than deep frying;
· Reduce your consumption of pastries and baked goods (croissants, commercial muffins, donuts, etc.).
· Decrease your consumption of animal fat, by varying your sources of protein: include fish and legumes more often in your menu;
· Favor non-hydrogenated oils and margarine over animal fats;
· Choose leaner cuts of meat;
· Switch to low fat milk and alternatives.
Red meat and cold cuts
Red meats, mainly those that are grilled, could promote the appearance of certain cancers, including that of the prostate. Processed meats (ham, bacon, cold meats and cold cuts) could also play a harmful role.
At lunchtime, choose canned fish, chickpea or tofu spreads and leftover roasts rather than the traditional slices of ham, salami or "baloney".
Calcium and dairy products
Although calcium is an absolutely essential nutrient for the development and maintenance of bone health, it seems that excessive consumption may be linked to a greater risk of developing prostate cancer. To enjoy the benefits of calcium without risking the disadvantages as well, it is recommended that you do not take calcium supplements that provide more than 1000 mg.
High consumption of whole, partially skimmed, or fat-free dairy products has been linked to an increased risk of developing prostate cancer. This link is not clear and more studies still need to be done.
Canada's Food Guide classifies dairy products as a protein food. They therefore have their place in your diet, without having to give them a disproportionate importance.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: 0022996374527
WE DELIVER ALL OVER THE WORLD
PROSTATITIS TREATMENT BY PHYTOTHERAPY
DEFINITION
The prostatitis is an inflammation caused by a bacterial infection of the prostate.
This organ is an endocrine gland in the male genital system which has the function of producing the seminal fluid necessary for the development and mobility of sperm.
Conventional care for prostatitis requires the use of a cytobacteriological examination of the urine to identify the pathogen responsible for the disease.
As for herbal treatments, they help relieve the painful symptoms of prostatitis and speed up healing. Here is the natural treatment from the experts at Dawasanté herbal medicine to cure prostatitis. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
In this context, an effective mutual or insurance allows benefiting from high reimbursements of the expenses of consultations of urologists, ultrasounds and biological analyzes as well as herbal remedies prescribed by the doctors.
PLANTS TO RELIEVE PROSTATITIS
Saw palmetto to relieve benign prostatic hyperplasia
The saw palmetto (Serenoa repens) is a shrub whose berries contain sterols, substances which have the property of relieving the symptoms of BPH. Several cross-analyzes of clinical trials of good methodological quality have confirmed the interest of saw palmetto extracts in the treatment of BPH.
Commission E and WHO recognize the use of saw palmetto in "the treatment of urinary difficulties associated with BPH".
The EMA grants the status of “well-established medical use in the symptomatic treatment of BPH” only to saw palmetto extracts obtained with hexane as an extraction solvent. In addition, it only grants the status of "traditional use to relieve symptoms of the lower urinary tract associated with BPH" to saw palmetto extracts obtained with ethanol as an extraction solvent.
In France, drugs based on saw palmetto extracts are available for this use, only one of which uses hexane to extract the active ingredients and none uses ethanol.
African plum to relieve benign prostatic hyperplasia
The African plum (Pygeum africanum) is a tree whose bark is used to produce standardized extracts containing sterols and docosanol. A cross-analysis of eighteen clinical trials points to some efficacy of African plum extracts in the treatment of BPH, but less than that of saw palmetto extracts.
The EMA grants “traditional use to relieve symptoms of the lower urinary tract associated with BPH” status only to African plum extracts obtained with chloroform as an extraction solvent.
In France, drugs based on saw palmetto extracts are available for this use, none of which uses chloroform for the extraction of the active ingredients.
Pumpkin seeds to relieve benign prostatic hyperplasia
Pumpkin seed extracts (Cucurbita pepo) are recognized by Commission E to “facilitate the emission of urine in men suffering from BPH”. These seeds contain many substances (phytosterols, essential fatty acids, etc.) whose action on the prostate is poorly understood. There are few studies of pumpkin seeds used on their own (they are often combined with other herbs offered in the treatment of BPH). Their use in this indication is based on tradition.
The root of stinging nettle to relieve prostate benign
The roots of stinging nettle (Urtica dioica) contain lignans, with properties similar to those of female hormones and which could explain their effects on the prostate. However, clinical trials evaluating the effects of nettle root on prostate adenoma are of poor methodological quality. They point to the effectiveness of nettle root without providing scientific proof.
Unlike other official sources (WHO, Commission E and ESCOP), the European Medicines Agency (EMA) considers that these studies are inconclusive and that BPH being a disease that must be treated medically, the root nettle can not be considered a traditional treatment for this pathology.
Against prostate cancer: coffee and tomatoes
No plant to date can accompany or cure prostate cancer. On the other hand, in prevention, a large study carried out on 48,000 people by the National Cancer Institute was able to establish that consumption of 6 cups of coffee per day reduced the risk of 60% of suffering from cancer of the prostate. Unfortunately, consuming so much coffee daily is not reasonable: in addition to a phenomenon of dependence, excess caffeine causes many side effects, such as nervousness, restlessness, anxiety, palpitations, insomnia, stomach irritation. , diarrhea ...
The good news, decaffeinated offers the same virtues. It is indeed the polyphenols in coffee, and not caffeine, which gives it these preventive properties. A similar study published by the same institute also showed that consuming cooked tomatoes two to three times a week reduces the risk of developing prostate cancer by a third (compared to occasional consumption). Finally, healthy living remains effective prevention: avoiding exposure to toxic products, including pesticides (farmworkers are more exposed to this cancer), being active and limiting the consumption of red meat, cold meats and cheeses. fatty, while favoring large rations of fruits, vegetables and fish.
Treatment of prostatitis: treatment of inflammation and contributions of phytotherapy in case of prostatic hypertrophy
Prostatitis requires drug therapy with antibiotics and anti-inflammatories. This cure lasts from 3 to 8 weeks depending on the germ causing the infection.
Besides antibiotic therapy, the patient may resort to herbal remedies to relieve the symptoms of an enlarged prostate such as:
- bearberry: anti-inflammatory and soothing pain in urination, this plant is prescribed in cases of acute prostatitis and cystitis. Also called bear grape, it is an antiseptic and powerful antibacterial against pathogenic bacteria of the urinary tract.
- giant sequoia: antidepressant and hormonal regulator, giant sequoia buds help to treat inflammation in cases of prostatic hypertrophy. They are also effective in stimulating appetite and reducing the fatigue that accompanies prostatitis.
- pumpkin seeds: they are used in herbal tea against urinary disorders associated with an enlarged prostate. These seeds are also effective in relieving pain, facilitating mixing, etc.
- serenoa repens: the berries of this saw palmetto are used to treat inflammation of the prostate and prevent a recurrence
Massages of the genitourinary area of the prostate with essential oils (Scots pine, cypress, peppermint, etc.) are also recommended to relieve symptoms and prevent prostatitis.
Oral antibiotic intake and herbal medicine find their limits in severe prostatitis. Hospitalization for 2 to 4 days is then required in order to put the patient on intravenous antibiotic therapy.
Prostatitis: symptoms, types and risk factors of prostatic hypertrophy
Prostatitis causes enlargement of the gland and compression of the urethra and bladder. The first clinical signs of this prostatic hypertrophy are pain and discomfort when urinating, which results in the accumulation of urine residues at the origin of the aggravation and complication of the urological disease.
Inflammation of the prostate can be either:
- acute prostatitis: usually of bacterial origin, it is characterized by high fever, severe pain in the lower abdomen and general fatigue. The patient also experiences frequent urges to urinate despite the small amounts of urination expelled
- chronic prostatitis: of bacterial or non-bacterial origin, it is the consequence of a poorly healed urinary tract infection. This recurring pathology manifests itself by twitching in the lower abdomen, aggravated by retention of urine
The enlarged prostate is favored by:
- the stress
- sexually transmitted infections
- urogenital malformation
- prolonged sitting (office, car, plane)
- the practice of certain sports such as horse riding or cycling
Prostatitis affects young men. It is often associated with psychological impacts and a deterioration in the quality of life due to painful symptoms, incontinence and difficulty in sexual relations.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.

OLIGO-ASTHENO-TERATOSPERMIE
OLIGO-ASTHENO-TERATOSPERMIA
You have been trying to have a baby for several months, but it is late. After tests, your doctor told you that your loved one has oligoasthenoteratospermia (OATS). What are OATS and what are the consequences?
However, the experts at Dawasanté provide you with a natural treatment to permanently cure oligo- asthenoteratospermia.
Click HERE or on the image below to discover this natural treatment
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
What is Oligoasthenoteratospermia or OATS?
OATS designates a set of abnormalities found during the spermogram during a male infertility assessment. The OATS groups together a low concentration of sperm (oligo) with therefore too few spermatozoa to naturally fertilize an oocyte, too low mobility of these spermatozoa (astheno) which does not allow them to join the oocyte and too large a proportion abnormal sperm (terato). However, OATS can present varying degrees. It can be severe, with very low mobility and concentration indices while the malformation index is very high. It can be moderate with indices closer to normal. Intermediate forms exist with indices of the same degree or which may be of different degrees: severe for one or two types of indices (eg: mobility and concentration) and moderate for the third.
What happens after diagnosis of the OATS?
Once the OATS is discovered, the doctor will look to determine if there are any causes for these abnormalities. Indeed, OATS can be reduced, at least in part, depending on its origin. He will look first for signs of infections, old or recent. Some infections, such as chlamydia, can cause a decrease in male fertility. Their treatment can help regain better fertility. Likewise, the treatment of a varicocele (varicose veins in one or both testicles) or stopping smoking may improve the results of a spermogram. Further research will be carried out to find out if there is a malformation in the testes or seminal tract. In all cases, a second spermogram will be done because it is possible that significant variations appear and allow to hope for other opportunities for natural fertilization.
What to do to have a child in the event of OATS?
If the diagnosis of OATS is confirmed, the possibility of natural fertilization is reduced. However, it does exist, especially if it is a moderate form. However, certain factors, such as the woman's age or the length of time contraception has been stopped must be taken into account and assisted reproduction (ART) may be considered. Depending on the case, it will be an in utero insemination (IUI) where the sperm is introduced directly into the uterus, and in vitro fertilization (IVF) where the sperm is brought into contact with one or more oocytes in the laboratory or an intracytoplasmic sperm injection (ICSI) where sperm is introduced directly into an oocyte in the laboratory. These different techniques will be offered depending on the degree of OATS. The success of IVF or ICSI is of the order of 25 to 30% which leaves hope to those who are concerned by this difficulty.
Asthenospermia is an abnormality of the sperm that is characterized by insufficient mobility while their number remains normal. Also called asthenozoospermia, this sperm fatigue is one of the possible causes of male fertility problems. What are the main causes? How is asthenospermia diagnosed? What treatment is there to promote procreation?
What is asthenospermia due to?
The main causes that can explain unsatisfactory sperm mobility are:
- a morphological anomaly of the male gametes,
- an infection,
- presence of anti-sperm antibodies
- medication,
- a varicocele,
- a dietary deficiency,
- a renal failure,
- liver failure
- chemotherapy,
- exposure to radiation,
- excessive alcohol consumption,
- a deficiency in calcium, vitamin D, or trace element ...
How is asthenospermia diagnosed?
A semen analysis, or spermogram, is used to assess the mobility of the sperm. It should be remembered that only mobile gametes can fertilize the egg. Many medical analysis laboratories rely on the classification decreed by the World Health Organization to classify spermatozoa:
- Level A (or I): progressive rapid sperm advance quickly and in a straight line,
- Level B (or II): the slow progressive spermatozoa advance slowly or in a curved line,
- Level C (or III): non-progressive spermatozoa move but do not progress,
- Level D (or IV): the sperm are immobile.
To be qualified as normal, the spermogram must show a minimum of 40% of motile spermatozoa and 32% of spermatozoa showing progressive mobility.
What solutions to have a child?
The management of asthenospermia varies mainly according to its origin. Thus, an infection will have to be treated according to its nature with appropriate antibiotic drugs while certain testicular abnormalities may, in some cases, be the subject of surgery. While there is no curative treatment for asthenospermia, certain drugs help improve the quality of sperm: vitamins, hormones, alternative medicine (herbal medicine, homeopathy, aromatherapy, etc.). When the treatments do not give satisfactory results, in vitro fertilization with donor sperm or an intracytoplasmic injection of sperm may be considered in the context of Medically Assisted Reproduction ( MAP).) when the couple wants a child.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
TERATOSPERMIA TREATMENT: Can it be cured?
The teratospermia (or teratozoospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. However, Dawasanté experts provide you with a natural plant-based treatment to improve the quality and quantity of your sperm.
Click HERE or on the image below to discover this treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Teratozoospermia can occur from birth, which is thought to be due to a genetic cause or be acquired over time through hormonal changes or trauma. Depending on the cause, it will be possible to apply personalized treatment to reverse this situation.
In congenital cases of teratozoospermia, it is very difficult to obtain a cure. The same is true when these changes are the result of cancer treatment. In severe cases of teratozoospermia, assisted reproduction will be necessary to become parents.
However, when the degree of teratospermia is lower, there are pharmacological or natural treatments that can help restore sperm quality.
Natural treatment
Since the exact cause of teratozoospermia is not known, it is difficult to apply a solution to problems with sperm morphology.
However, a healthy lifestyle can greatly influence the quality of sperm. For this reason, there may be variations in sperm values within a few months of each other.
Proper treatment should ensure that the process of sperm maturation during spermatogenesis proceeds properly. Therefore, we are going to discuss some recommendations for maintaining good habits that promote this correct formation of sperm.
1-1 Power supply
A healthy and balanced diet improves general health. In addition, the vitamins and antioxidants contained in certain foods also provide benefits to the quality of sperm.
These are some of the important components that a man should include in his diet to improve his fertility status:
- Selenium
- Vitamin C
- Zinc
- Omega-3 fatty acids
- this mineral is found in Brazil nuts, walnuts, tuna, beef, chicken, eggs and cheese. It should be taken in small amounts, otherwise it can be toxic.
- in spinach, tangerines, strawberries and tomatoes. Vitamin C is a powerful antioxidant and also helps in the absorption of iron.
- it is a mineral found in foods such as oysters, clams or red meat. Zinc is essential for the functioning of enzymes, which are responsible for producing energy in the body.
- in fatty fish and crustaceans. It is very important to include them in the diet because the human body is not able to synthesize them on its own. In addition, it brings multiple benefits to the cardiovascular system, the nervous system, the immune system, etc.
- Healthy and balanced diet to cure teratozoospermia

1-2 olive oil
Olive oil is essential in the Mediterranean diet and also has reproductive properties thanks to its oleic acid content.
Oleic acid acts as a lowering agent for bad cholesterol or LDL levels which can build up in the testes, making it difficult to produce sperm properly.
Olive oil also helps raise good cholesterol or HDL levels and prevent the risk of heart and brain complications.
In short, olive oil is an ally in the fight against male infertility and especially teratozoospermia.
PMA, like any medical treatment, requires that you trust the professionalism of the doctors and clinic you have chosen. Obviously, not all are the same. The Fertility Report selects the most advantageous clinics for you based on our rigorous quality criteria. In addition, the system performs a comparison of prices and conditions offered by different clinics to facilitate your decision making.
1-3 Avoid heat
High temperatures in the testes affect sperm production and can cause sperm abnormalities.
Therefore, men with infertility issues should consider the following recommendations:
- Do not use the laptop on your legs.
- Avoid saunas in general.
- Wear boxers and wide pants.
- Try not to cycle long distances.
Once the temperature decreases and the heat exposure decreases, the testes return to their normal function and the quality of sperm improves in a short time.
1-4 Eliminate toxins
Some compounds that we are exposed to on a daily basis can be very harmful to reproductive health without our being aware of it.
Tobacco, drugs, marijuana smoke, pesticides, chemicals, and excessive amounts of alcohol can cause sperm deformity.
It is therefore important to eliminate these bad habits from your environment.
2-Vitamin supplements
In some cases of teratozoospermia, it is common for the urologist to advise the administration of certain nutritional supplements that supplement the diet in order to obtain a better result.
The most common treatment is a vitamin and antioxidant supplementation.
Antioxidants are responsible for reducing the oxidative stress to which sperm are exposed, which causes cell damage and the fragmentation of their DNA.
Some recommended dietary supplements include vitamin E or essential amino acids like L-carnitine. Vitamin E treatment is also recommended for chemotherapy and radiation therapy, as it is a very powerful antioxidant.
On the other hand, Andean maca supplements are also very beneficial due to the multitude of properties of this Peruvian plant.
It should be noted that these compounds are not miraculous and that in no case will it be possible to regain total fertility if the seminal parameters are severely affected.
However, when there is mild teratozoospermia, they can help and give a little boost for men with vitamin deficiencies in the diet.
Peruvian Maca powder to treat teratozoospermia

3-Your frequently asked questions
3-1 Is there a cure for severe teratozoospermia?
If a man has less than 5% of sperm with normal morphology, it is very difficult to find a normal value with natural or pharmacological treatment. Improvement can be seen over time, especially if the man maintains a healthy lifestyle.
On the other hand, if the teratozoospermia appears associated with another pathology such as, for example, varicocele, it is possible that the spermogram improves its parameters during a surgical intervention to eliminate the varicocele.
3-2 Can acupuncture be of benefit in the treatment of teratozoospermia?
There are studies that say yes. In general, acupuncture has been successful in increasing pregnancy rates in idiopathic infertility, that is, when the origin is unknown. An improvement in seminal quality has also been observed in men with oligospermia, asthenospermia and teratospermia who practice acupuncture.
3-3 Does eating forest fruits improve seminal quality?
Yes, many forest fruits have antioxidant pigments and a great capacity for absorbing oxygen free radicals, so this food group is perfect if you want to improve or protect sperm quality.
Some research has uncovered the medicinal properties of pigmented polyphenols, such as flavonoids, anthocyanins, tannins and other phytochemicals present in the skin and seeds of these fruits.
Moreover, blueberries, blackberries, currants and strawberries are rich in vitamin C and other nutrients. Vitamin C is a powerful antioxidant that protects cells from cellular damage.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
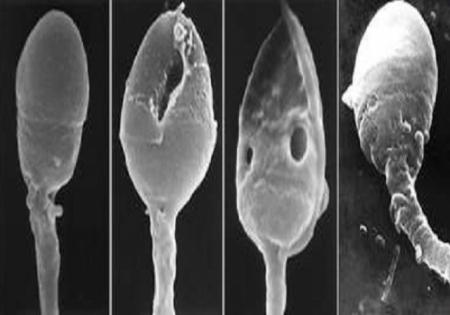
THE CAUSES OF TERATOSPERMIA: Natural treatment
The teratospermia (or teratozoospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. Dawasanté experts advise you to opt for a natural treatment without operation, against teratospermia.
Click HERE or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Teratozoospermia refers to the poor morphology of the sperm in a man's ejaculated semen.
These men have lower seminal quality and sometimes suffer from infertility and difficulty achieving pregnancy.
The causes of teratozoospermia are mostly unknown. However, we are going to address the possible alterations caused by these abnormal sperms in semen.
1-Defects in spermatogenesis
Most experts agree that the morphological changes in sperm occur during the last phase of their formation.
The spermatogenesis is the process by which sperm are formed in the testicles, which lasts about 3 months.
More precisely, spermiogenesis is the last phase of spermatogenesis, during which the spermatozoa, which already have their genetic content formed, undergo a process of maturation and acquire their characteristic morphology.
Once the sperm have their oval head and tail formed, they are released into the seminiferous tubules to follow their path.
Therefore, it is not surprising that any abnormality or alteration in spermiogenesis results in abnormalities in the head, neck or tail.
2-Reversible teratospermia
Teratozoospermia can be reversible or irreversible depending on the specific cause.
With reversible teratospermia, men can regain their seminal quality after a few months if they have received the appropriate treatment.
To check this, it is necessary to do another spermogram and compare it with the previous one.
We will now discuss the possible causes of reversible teratozoospermia:
2-1 Way of life
Although it may seem surprising, the lifestyle of men greatly affects the quality of their semen.
During times of stress and anxiety, sperm morphology may deteriorate, as many other parameters such as concentration and mobility.
The abuse of alcohol, tobacco, or other drugs are also factors linked to alterations in sperm.
Prolonged exposure to testicular heat affects spermatogenesis. Therefore, the bad habit of placing the computer on your legs, wearing tight clothes, or driving for a long time can cause teratozoospermia.
Testicular heat causes teratozoospermia

Finally, diet and sport also contribute to male fertility.
Men who are planning to become pregnant with their partner are recommended to maintain a good lifestyle, eat a balanced diet, exercise regularly and not consume substances that are harmful to the body.
2-2 Seminal infections
Semen infections refer to the invasion of microorganisms, bacteria, and viruses, into the male reproductive system.
Its presence is found in urine and semen, causing alterations in the sperm, as well as inflammation and obstruction of the seminal ducts.
The most common bacterial infections in the testes are chlamydia and gonorrhea. These infections can be fought with antibiotics and male fertility can be restored. If you would like more information on this, you can access the following article: Types of infections in seminal fluid.
The episodes of fever caused by flu or another disease may also occasionally affect sperm quality.
2-3 Pharmaceuticals
Sex hormones like testosterone, LH, FSH and inhibin have a very important role in the regulation of spermatogenesis.
Therefore, any drug that changes the appropriate levels of these hormones or affects their secretion by the brain has negative consequences for sperm production.
As we have already said, the alteration of the phase of spermiogenesis prevents the correct maturation of sperm and causes teratozoospermia.
Reversible causes of teratozoospermia
3-Irreversible teratospermia
If a man with teratozoospermia fails to improve his second spermogram after receiving treatment, one may begin to suspect that the teratozoospermia is irreversible.
In these cases, the couple will have to resort to assisted reproduction if they want to become a parent because it will naturally be very difficult to obtain a pregnancy.
In addition, there are other pathologies or situations that cause irreversible or prolonged teratozoospermia. The most relevant cases are examined below:
3-1 Cancer treatment
Chemotherapy and radiation therapy alters both sperm stem cells and sperm production, causing severe teratozoospermia and other more serious changes.
For these reasons, all men with cancer are advised to save a semen sample if they wish to have children in the future after they have overcome the disease.
3-2 Genetic diseases
It is one of the most difficult causes of diagnosis. Normally, when it has not been possible to determine the pathology that causes teratozoospermia, it is attributed to a genetic factor.
Defects in the genes or chromosomes of the sperm are a serious problem because they cannot be corrected.
3-3 Associated pathologies
Teratozoospermia can also result from other diseases that mainly affect the testes, for example:
- Trauma or blows to the testicles, especially in childhood
- Testicular varicocele
- Meningitis
- Diabetic sugar
In addition to all this, the age of males can also affect the morphology of the sperm. In particular, it has been observed that men over 45 have a higher rate of abnormal sperm in their semen.
Irreversible causes of teratozoospermia

4-Your frequently asked questions
4-1 Can live sperm have poor morphology?
By Zaira Salvador (embryologist).
Yes, teratozoospermia can be present in both living and dead sperm.
Dead sperm do not always have a bad morphology. Sometimes they are confused with immobile sperm and it is necessary to make a tincture to find out whether they are viable or not.
4-2 Can leukospermia cause teratospermia and male infertility?
By Zaira Salvador (embryologist).
Leukospermia, also known as leukocytospermia, is the appearance of leukocytes in semen, with a concentration level greater than 1 million per milliliter. The cause of this seminal pathology is an infection of the male reproductive tract which must be treated with antibiotics as it can affect spermatogenesis and cause oligospermia or teratozoospermia.
You can find the information in our article: Leukocytes in semen.
4-3 Are the causes of teratozoospermia and asthenozoospermia the same?
By Zaira Salvador (embryologist).
In most cases, asthenospermia and teratospermia have the same causes. The two seminal parameters are usually changed in the seminogram, known as astenoteratozoospermia. However, this is not always the case.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.













