regain their fertility
Blog / 83 results found
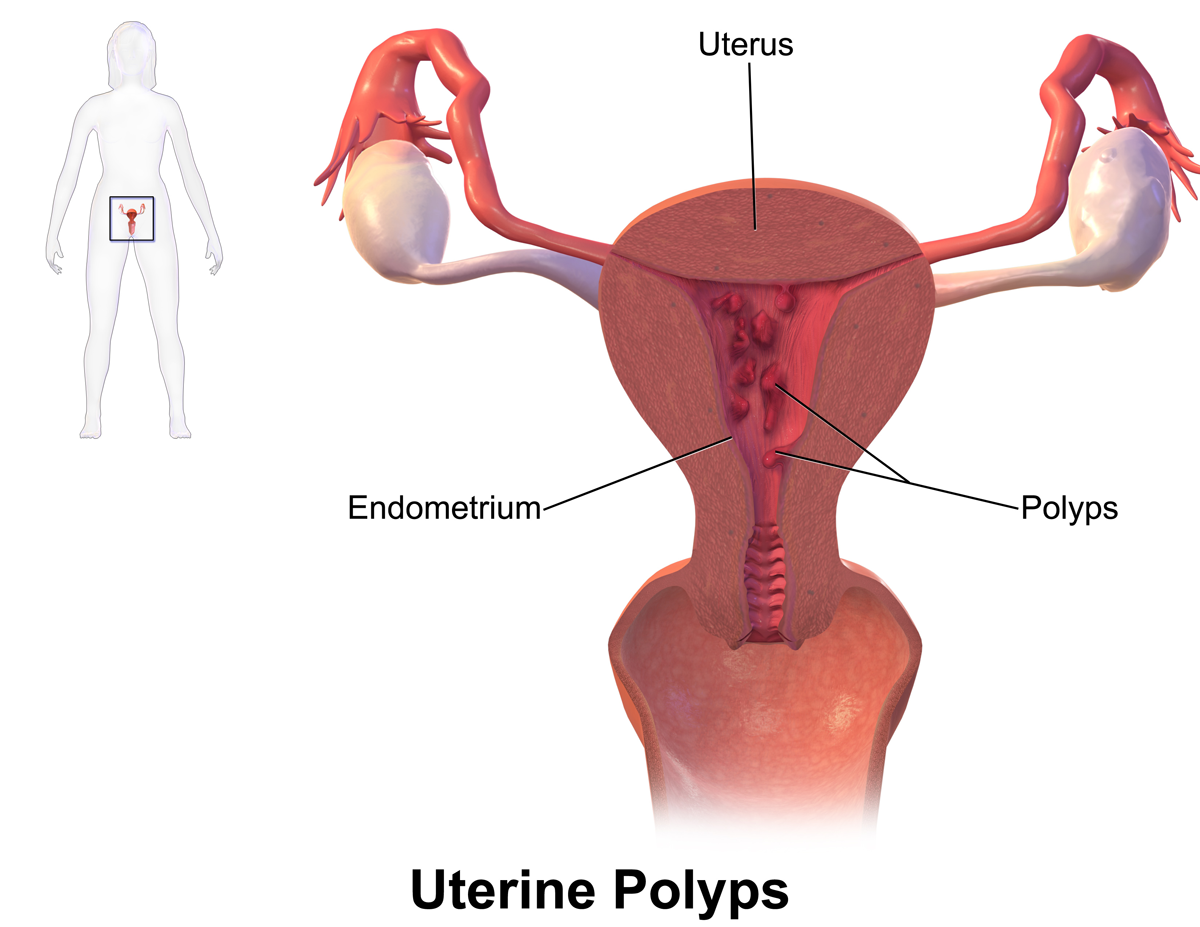
SYMPTOMS OF UTERINE POLYPs: Natural treatment
WHAT ARE THE SIGNS OF UTERINE POLYPS?

Uterine polyps are stressful news for any woman. They can cause a negative experience and discomfort. They are not cancerous, at least for the most part they are not. To what extent they still endanger health is a question whose exact answer can only be heard in the doctor's office.
Uterine polyps come in different sizes and are attached to the wall of the uterus. They are single or in a group of several. They are likely to occur at a young age but are more common in women before and during menopause.
Uterine growths are sensitive to estrogen and the most likely causes are hormonal changes. Among the risk factors for them are overweight, high blood pressure, and some drugs for breast cancer.
HERBAL TREATMENT FOR UTERINE POLYPS
The causes of this disease can be different, and tumors appear in young girls and older women. If the doctor put such a diagnosis - do not despair. There are ways not only with medication, you can still treat uterine polyps with an herbal remedy. Both methods are effective in killing polyps and preventing new ones. A woman can choose the most suitable treatment option for yourself, depending on the characteristics of her body.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: https://wa.me/22996374527
Symptoms of uterine polyps
The truth is that they are mostly found during random examinations by a gynecologist. This is not due to negligence or ignorance on the part of the ladies, but only because these polyps form asymptomatically. Doubt about their locality is caused mainly by:
- Irregular menstrual flows. They appear at no time and last indefinitely.
- Spots between periods. They are not exactly a monthly flow, but rather spots left by one.
- Prolonged menstruation. Significant lengthening of the menses for no apparent reason.
The most popular recipes against uterine polyps

Consider effective and easy-to-prepare folk remedies that will help treat uterine polyps without surgery and without significant obstruction to the body.
Herbal extract for regular intake
To prepare the soup, you will need 1 teaspoon black currant fruit, 3 teaspoons cinnamon wild rose fruit, 2 teaspoons of dioica nettle leaves.
Currants, rose hips, and nettle bloomery should be mixed and grind well.
Then take a tablespoon of the resulting mixture and pour two cups of boiling water.
Giving to run for an hour and filter through cheesecloth (during which time the infusion will gain almost room temperature).
If the taste is too bitter, you can add a little sugar - it does not affect the properties of the soup. It should be taken 4 times a day at any time by drinking half a glass. This recipe is a great help in treating cervical polyp.
Herbal decoction for douching
Endometrial surface polyps arise for various reasons, one of which is a violation of the natural hormonal balance against the background of nutrient deficiency. It is this situation that can be corrected by applying a decoction.
Should be used if there are vaginal cords.
To prepare the need: 2 tablespoons herb yarrow ordinary, 2 tablespoons rosemary leaves, 2 tablespoons sage leaves drug, 4 tablespoons plain oak bark.
All these components should be well ground and mixed in an enamel bowl. Then, pour boiling water volume of 2.5 liters and bring it to a boil.
Boil the broth need about half an hour, then cool - always at room temperature. When the broth itself reaches room temperature, it is necessary to filter through a fine sieve or gauze. Then it can be used for vaginal douching, the procedure is repeated twice a day. also the effective herbal treatment of uterine fibroids - Another annoying problem.
Effective folk remedy against uterine polyps
For the treatment of uterine polyps folk remedies it is possible as an operative or homeopathic way, and with the help of folk remedies, even if the symptoms are strong enough. Use this decoction should be in the presence of heavy and persistent vaginal cords.
To prepare the decoction, you will need to collect: 3 tablespoons of dioica nettle leaves, 5 tablespoons herb knotweed, 1 tablespoon chamomile, 1 tablespoon of ordinary oak bark.
You need to carefully grind and mix well all the ingredients. Then take two tablespoons of the resulting mixture, put in an enamel pan, and fill it with 1 liter of boiling water.
Decoction boil for 5 minutes on low heat, then leaves to cool to room temperature.
When the broth has cooled, strain it through a fine sieve or cheesecloth. The resulting mixture can be used for vaginal douching. For effective enough to use it at least twice a day.
Experience has shown that the use of this decoction can eliminate endometrial polyp without surgery.
Recipe based on celandine
Particularly effective since ancient times is considered the treatment of uterine polyps greater celandine. The more you can use it not only for sprintsevalnyh solutions but also for oral administration.
However, it should be remembered that before taking such funds it is necessary to consult with your doctor.
The same recipe is very simple.
We need to a quart a jar and fill it with fresh grass celandine.
Then you need to pour boiling water over the grass.
The bank is not broken, it is best to warm up before preparing the solution.
Cover the dish with a warm scarf and it will leave in a few hours.
Then, the mixture is ready, and it can be used for regular swallowing.
It should be taken three times a day. We must start with very small portions (about 1 teaspoon) and then gradually increase the dose by the end of the second week from one serving to 100 milliliters.
A two-week course can be effective enough to eliminate appearing polyp in the uterus.
Sometimes, of course, it is not enough, and you will have to repeat it. But before the infusion of celandine again, you need to rest for not less than two weeks.
It is also useful for uterine propolis, for example, candles for uterine fibroids from propolis are useful for healing.
As is the case with other folk remedies for the treatment of uterine polyps, be sure to remember that the infusion of celandine - is not a cure. And polyps, regardless of their origin, require medical supervision. However, to engage with homeopathy, and especially immediately agree to surgery should not be in any case - because your body must protect itself and carry out its treatment should be as painless as possible means.
To contact our experts please call or write to us on the following number, tel / WhatsApp
: https://wa.me/22996374527

WOMEN'S INFERTILITY: CAUSES, SYMPTOMS AND NATURAL TREATMENT
WOMEN 'S INFERTILITY : CAUSES, SYMPTOMS AND NATURAL TREATMENT
What is female infertility? What are its causes ?
The infertility is the inability for a couple to achieve pregnancy or to a woman, to lead his term gestation. It is estimated that infertility is established after two years of unprotected sex. Unlike infertility, female infertility is not permanent. It can result from various gynecological disorders or dysfunctions: endometriosis, ovarian dysfunction, uterine polyps, obstruction of the fallopian tubes, obesity, stress, excessive alcohol consumption. However, to remedy this problem, Dawasanté experts provide you with a natural treatment based on medicinal plants to permanently cure infertility.
HERBAL TEA AGAINST FEMALE INFERTILITY
Our natural remedies are the secret to cure any form of female infertility. We offer you a definite advantage: the absence of undesirable effects and contraindications. The natural approach is often the best approach to find a solution. Our natural remedies have allowed many women to have children. Being natural products based on plants and herbs, our natural remedies have no side effects, either on the body or on health. Our natural treatment is not dangerous. You can therefore cure female infertility without fear of the appearance of side effects.
CLICK ON THIS LINK TO GET THIS PRODUCT !!
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
What are the symptoms of female infertility?

The main symptom of female infertility is the absence of pregnancy. But beware, conceiving a child can naturally take time. So do not worry if the baby tests follow one another without the expected result. The process of fertilization is complex and can take time. However, it is advisable to consult a gynecologist if the absence of pregnancy is associated with menstrual cycle disorders ( amenorrhea , dysmenorrhea, etc.), abnormal vaginal discharge, or pelvic pain.
Who are the people at risk?
From the age of 30, female fertility tends to decrease. In addition, tobacco, alcohol and caffeine consumption also represent potential impediments to fertilization and can increase the risk of spontaneous abortion. Finally, physical condition is also an essential parameter. Thus, women who are overweight or, on the contrary, very thin may have difficulty in getting pregnant.
How is the diagnosis of female infertility made?
In the event of difficulty in obtaining a pregnancy, it is essential to consult a gynecologist, the only practitioner authorized to carry out an appropriate medical investigation. For this, the health professional has a battery of tests to confirm and detect the exact cause of infertility: blood tests, vaginal smear, pelvic ultrasound, hormonal assessment ... For the most difficult cases, he can also perform the Hühner test, a post-coital test that allows, among other things, to analyze the quality of cervical mucus.
What are the treatments for female infertility?
Indeed, the management of female infertility will depend on its origin. If it is menstrual disorders, hormonal treatments (ovulation stimulators, etc.) may be recommended. In addition, the surgical route will be preferred in the presence of ovarian cysts or obstruction of the fallopian tubes, while the use of medically assisted procreation techniques will be offered to certain couples.
Plants for hormonal detoxification
Due to the number of pollutants present in our daily environment, we are constantly exposed to many products that disrupt our hormones. (1,2,3) We call them, moreover, endocrine disruptors. These substances or compounds interfere with the proper functioning of our hormonal system and can increase the risk of suffering from infertility. Even by eating well, by not taking the car, by making your cosmetics and cleansers yourself, you risk coming into contact with certain endocrine disruptors, if only in the air you breathe. One interesting strategy for preserving your fertility is to help the body detoxify itself from endocrine disruptors. Here are some interesting herbs to help the liver with this task:
Dandelion (root)

Dandelion is one of the best liver plants. We know that it is the liver that takes care of breaking down the surplus hormones with a view to their elimination and the dandelion takes care of decongesting it while helping the intestinal elimination of hormones via the bile.
Milk thistle (flower)

Another beautiful liver plant! Milk thistle will help protect the body from toxic and fertility-damaging substances and help decrease excess estrogen in circulation.
Turmeric (rhizome)

Turmeric is one of the most antioxidant and anti-inflammatory plants. It helps stimulate the liver and the gallbladder and therefore promote the elimination of excess hormones. It also helps reduce inflammation and prevent the formation of free radicals, 2 factors that are highly harmful to reproductive health.
Plants to reduce stress
Stress is very damaging to reproductive health. Among other things, it can disrupt the normal production of hormones, lengthen the menstrual cycle, prevent ovulation and adversely affect the quality of the ovum and sperm. To calm daily stress, here are some interesting plants to take in herbal tea:
Lemon balm (leaf)

It is the plan of letting go! Have you been told that it is by letting go that you will get pregnant ? If you have difficulty, choose lemon balm. Plus, it will help your mood and digestion.
Oats (straw)

Oats are a great tonic for the nervous system. In addition, it contains several nutrients favorable to fertility and the cycle of women, including calcium. To be taken long term.
The motherwort (flower)
The motherwort is used for a range of problems including anxiety, depression, irritability, mood swings, etc. It is one of the best herbs to have on hand when the nervous system seems exhausted.
Plants that nourish the reproductive system
In addition, to get pregnant, it is important that the body has all the essential nutrients. The most important nutrients for male fertility are: copper, omega, zinc, selenium and vitamins B, C, D. For women: Omega 3, calcium, magnesium, iron, manganese, zinc and vitamins A (especially beta-carotenes), B, C, D, E. A good way to get the most vitamins and minerals possible, is to add nutritious plants to your daily life. Here are a few examples:
Nettle (leaf): Nettle is one of the richest nutritious plants! It contains a lot of iron, beta-carotene, B vitamins and vitamin C.
Raspberry (leaves): The raspberry, in addition to being the tonic par excellence of the reproductive system of women, contains a lot of iron, vitamin C and beta-carotenes. It also contains certain B vitamins, calcium, magnesium and potassium among others.
Although herbs are wonderful allies in improving your fertility, if you have a particular or long-standing infertility condition, consult a qualified naturopath or herbalist for more personalized recommendations. And more in-depth monitoring of your condition. Remember to consult a doctor for medical advice or if in doubt.
CLICK ON THIS LINK TO GET THIS PRODUCT !!
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.

ERECTION DISORDER: NATURAL TREATMENT
ERECTION DISORDER: NATURAL REMEDY
Called dysfunction erectile - or problems with erection or disorders of erection - the inability to achieve or maintain an erection sufficient for satisfactory sexual activity.
Indeed, erectile disorders have benefited from several campaigns aimed at the general public, especially since the advent of oral treatments which represented effective solutions more practical than those available until then. We thus tended to believe that sexual breakdowns were no longer so taboo in homes and the media ... Well, the results of our survey show the opposite: a majority of respondents (59%) believe that the media do not cover enough this theme.
Does this feeling translate into a lack of information? The causes of these intimate problems are relatively well known to the respondents: a psychological origin, age, physiological causes, medication, a lack of interest in sex ... Conversely, information on treatments suffers from a real lack. knowledge: nearly a third do not know that these problems can be cured! This is the reason why Dawasanté experts provide you with a natural treatment based on medicinal plants to definitively treat erectile disorders. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Among those who actively seek information, the Internet is the main source of information (52%), far ahead of the specialized press (21%), and television (18%). The mainstream press, radio and thematic channels remain far behind.
Erectile dysfunction: a real impact on the life of a couple
On a daily basis, the men concerned admit that these disorders affect their couple/family life (84% of respondents) and the image they have of themselves (78%). Beyond the sexual problem, several feelings are mingled: attack of their virility, feeling of bad aging, guilt, shame, depression ... So many negative feelings that can promote breakdowns, which will then feed this fear of failure: the terrible vicious circle specific to erectile dysfunction.
And this feeling is not for all that the prerogative of men since 73% of women believe that these intimate problems have a significant impact on their married life.
Erectile dysfunction: to be treated, it is still necessary to talk about it ...
In the event of erectile dysfunction, respondents would naturally turn to their general practitioner (49%), even ahead of their partner/friend (18.5%) and the sex therapist/sex therapist (17.3%). According to their statements, the choice to go to another doctor, an andrologist, or friends remains quite rare.
But among those who are affected by this problem (80.2%, including 26.5% from time to time, 22% quite regularly, 16.6% regularly, and 15.2% all the time), the reality is quite different: only 44% admit to having spoken about it with their doctor, but 16.5% spoke about it with another doctor, a sexologist or an andrologist. And 39% never talked about it!
Without talking about it, 45.5% of men do not benefit from medication and 11% have turned to alternative solutions. Only 43.5% received a drug (mainly Cialis ® 55% and Viagra ® 21%). Why not have taken a proven treatment? The two most common reasons are not daring to talk about it (22%) and fear of side effects (16%).
Just over half of the women who responded to our survey (55%) are in a relationship with a partner who has had or has erectile dysfunction. According to them, most of their partners do not take any treatment (68%); 13.5% a treatment prescribed by the doctor and 7.5% an alternative treatment. The difference between partners shows that men often hide the fact that they are taking treatment.
The ideal treatment must be effective and well-tolerated
Among the patients treated, 30.6% experienced side effects (including 77% often to very often, 23% rarely or very rarely): headache, redness in the face, blocked nose, digestive problems, problems with the vision, dizziness ...
But overall, are they satisfied with their treatment? There is a very slight predominance of dissatisfaction (53%), a feeling mainly linked to a lack of efficacy (38.4%) and the cost of the drug (21%). Then come the fact of having to take it for each report (14.5%) and the lack of spontaneity that this generates (13.8%)… Different sources of discontent among women (55% are satisfied with the treatment, 45 % no) who first cite the lack of spontaneity in intercourse and the lack of effectiveness on erection.
What would be the ideal treatment for you? The main characteristics sought by all respondents (men, women, all ages combined) are good efficacy (30%), good tolerance (18%), rapid action (15%) and ease of use ( 14%). The price and its reimbursement are not a priority, the costly aspect comes after the efficiency.
The different treatments available
Today, new solutions exist, whether oral or local treatment.
· Oral treatment is generally offered as a first-line treatment. We find sildenafil, vardenafil, tadalafil. Acting on the relaxation of the smooth muscles of the cavernous bodies, these three molecules increase the blood flow at the origin of the erection. To be effective, they must be combined with sexual stimulation such as foreplay, caresses ... Please note, these treatments may be subject to contraindications or interactions with other treatments, talk to your doctor or pharmacist.
· Hormonal treatment may be a solution if a biological workup shows a drop in testosterone associated with clinical signs such as fatigue and a significant increase in abdominal fat. Testosterone can help regain sexual desire and also increases muscle strength. This treatment is only temporary and should be monitored by testing for testosterone in the blood.
· A local treatment may be prescribed. It comes in the form of injections into the cavernous body of the penis. The method of administration is often scary, but the bite is not painful and the doctor accompanies his patient step by step and for as long as necessary. They are only issued on medical prescription and are reimbursed when erectile dysfunction is linked to serious and well-defined physical damage (following prostate cancer and prostatectomy, paraplegia or quadriplegia, multiple sclerosis by example…) This treatment allows a fast and good quality erection even without sexual stimulation.
· The fitting of a penile prosthesis may be considered as a last resort. It is intended for men for whom other treatments are ineffective or contraindicated for medical reasons. This choice must be made in a concerted manner between the patient, his / her partner, and a specialized medical team.
Having desire breakdowns impacts men's morale and can have consequences on married life. It is possible to cure erectile dysfunction in some cases with simple remedies from grandmother.
THE GOOD CHOICE
Erectile dysfunction: coffee has an influence on the risk of erectile dysfunction
According to a recent study conducted by the Health Science Center at the University of Texas, Houston, drinking two or three cups of coffee a day can reduce the likelihood of erectile dysfunction.
This study, published in the journal PLOS ONE, found that men who consumed 85 to 170 mg of caffeine per day had a 42% lower risk of erectile dysfunction (ED) than average. For those who consumed 171 to 303 mg, the risk reduction was 39%.
The researchers asked 3,700 male subjects to complete a questionnaire about the amount of caffeine they had consumed in the past 24 hours. While caffeine intake decreased the likelihood of erectile dysfunction in obese, overweight, or hypertensive people, the same was not true in diabetics.
"Caffeine does not compensate for the negative effects of diabetes on erectile dysfunction," says David Lopez, lead author of the study. "This is not very surprising, as diabetes is one of the biggest risk factors for this dysfunction. "
An estimated thirty million Americans suffer from erectile dysfunction - the inability to stay hard long enough. In general, the likelihood of dysfunction increases with age. Some 40% of the forties are affected, and 70% of septuagenarians, as the Huffington Post recently recalled.
Researchers believe that one of the effects of caffeine is to relax the helicine arteries in the penis, which improves blood flow and causes an erection.
Among the sources of caffeine studied, we can cite - in addition to tea and coffee - energy drinks and sodas, which are particularly harmful to health, as David Lopez points out.
“Remember that aside from caffeine, energy drinks and sodas contain other ingredients that we don't know much about,” he adds. "We are very familiar with sugar, which is clearly associated with diabetes and obesity. Other drinks are free from it, but some of their ingredients can cause cancer."
Given that this is an association study, David Lopez indicates that he cannot, for the moment, do
Say no to erectile dysfunction with ginger
Ginger has vasodilating virtues facilitating the flow of blood. It is an aphrodisiac food par excellence, our grandmothers already knew it and provide us with recipes against erectile dysfunction. Here is an example of infusion: grate 50 g of fresh ginger and let stand for at least 4 hours in a liter of water in the refrigerator. You must consume two glasses a day and wait 15 days to see the first results and improve libido.
Dry dates and nuts against erectile dysfunction
Another grandmother's remedy for erectile dysfunction is to mix and pound equal amounts of dry dates, pistachios, walnuts, almonds, and flaxseeds until you get a fine powder. Mix this powder in a glass of water and drink daily to achieve effective results against the troubles erection.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
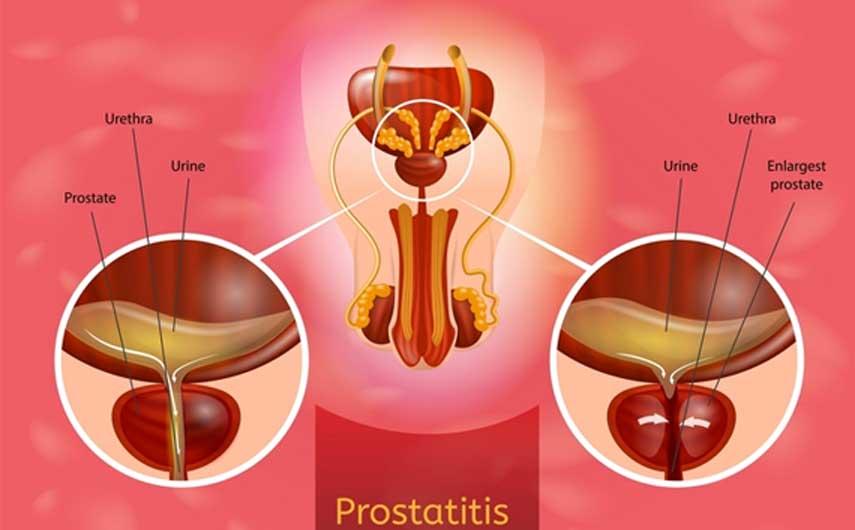
CHRONIC BACTERIAL PROSTATITIS: Natural treatment
Chronic Bacterial Prostatitis
What is chronic bacterial prostatitis?
Prostatitis chronic bacterial is a rare disorder that causes recurrent infection in the prostate and causes swelling, inflammation and infections frequent urinary tract. The prostate is a small gland located directly below the bladder in men.
Even with prolonged antibiotic treatment, bacteria can still survive in the prostate and symptoms often return. To remedy this pathology, Dawasanté experts provide you with a natural herbal treatment to cure prostatitis permanently. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Natural Treatment
If you suffer from prostate problems (inability to urinate, urination disorders, erectile dysfunction, premature ejaculation, lower back pain and penile pain, etc.), this is the miracle solution that will help you cure or prevent your prostatitis. The natural remedy to cure prostatitis permanently and quickly that we offer is composed of two elements: a herbal tea and an ointment. Generally, with the exception of the diagnosis too late, our natural treatment makes it possible to treat prostatitis quite easily and does not leave any sequelae. So trust us! This natural treatment is the secret to cure prostatitis without operation, without side effects thanks to plants.
Herbal tea is made from plants that have anti-inflammatory, astringent, antibacterial and calming properties. It works in particular by reducing the swelling of the prostate gland and providing immense relief. This natural remedy also contains several natural anti-inflammatory compounds that inhibit the inflammatory process that triggers inflammation and pain in the prostate gland. It also helps relieve urinary symptoms, including those caused by an excessively large prostate without having to have an operation. The natural remedy also helps in curing difficulty in urinating and it restores sexual balance. So this is the secret to cure prostatitis with plants.
First, the pain in your lower back and in your penis will gradually disappear. You will no longer have difficulty urinating and your erection will gradually return to normal. The use of herbal products to cure prostatitis gives excellent results. Our therapy to cure prostatitis that we offer is effective, fast, long-lasting. So; it will save you from having to go through an operation. Herbal tea to treat prostatitis has no side effects, either on the body or on health. Our natural treatment is secure. So this is the secret to cure prostatitis without operation and without side effects.
To discover our natural remedy to cure chronic bacterial prostatitis, click here
What are the symptoms of chronic bacterial prostatitis?
Bacterial infections in the prostate can be very painful. Symptoms start slowly and last for three months or more. See your doctor if you have any of the following symptoms:
- Blood in urine or semen
- Pain or burning sensation when urinating
- Pain on ejaculation
- Pain with stool
- Pain in the lower back, between the genitals and anus, above the pubic bone and in the testicles
- Foul-smelling urine
Serious complications can occur if an infection is not properly treated. Complications include:
- An inability to urinate
- Sepsis, which occurs when bacteria spread through the blood
- An abscess of the prostate, which is a collection of pus that causes inflammation
What are the causes of chronic bacterial prostatitis?
Prostatitis chronic bacterial is caused by a bacterial infection. Even when the main symptoms of infection have been treated, bacteria can continue to grow in the prostate.
Causes of infection include:
- Any bacteria that cause a urinary tract infection
- Sexually transmitted infections, such as chlamydia and gonorrhea
- Escherichia coli after infection of the testes, urethritis (inflammation of the urethra) or urinary tract infection
Certain factors put men at risk for developing this disease, such as:
- An enlarged prostate
- Infection in or around the testicles
- Narrowing of the urethra, or narrow urethra
How is chronic bacterial prostatitis diagnosed?
To make a diagnosis, your doctor will take your medical history and do a physical exam to look for swollen lymph nodes near the groin or for fluid discharge from the urethra.
Your doctor will also do a rectal exam to examine the prostate. During this test, your doctor will insert a lubricated, gloved finger into your rectum to look for signs of infection, such as a soft prostate or an enlarged prostate.
Your doctor may also perform the following tests:
- Test urethral fluid for bacteria
- Tests to rule out a sexually transmitted infection
- Urine test
Medical Treatment
Antibiotics are the main treatment for this condition. They are usually taken for four to six weeks. However, as the infection may come back, you may need to take antibiotics for 12 weeks or more. Your doctor will arrange for a follow-up after treatment to make sure the infection is completely gone.
It can take six months to a year for symptoms to go away completely. In the meantime, some home remedies may be able to ease your symptoms. Home remedies include:
- Hot baths
- Drink 64 to 128 ounces of water per day
- Use fabric softeners to avoid constipation
- Avoid alcohol, caffeine, citrus juices, and hot and spicy dishes
- Medicines to treat pain
Additional treatment may be necessary in the following rare cases:
- If you cannot pass urine, a health care provider will insert a tube called a catheter to empty your bladder.
- - If you have an abscess, your doctor will drain it.
- If you develop sepsis you will receive intensive antibiotic therapy and will need to stay in hospital.
- If you have stones or mineral deposits in your prostate, your doctor may need to remove your prostate. It's very rare.
Tips to follow if you have prostate cancer
When you are suffering from chronic bacterial prostatitis, certain lifestyle changes can be of great help. Here are the tips to follow:
–Drink plenty of water. Ideally, you should drink at least 1.5 liters of water per day. Fluid intake helps the metabolic process to function well.
-Avoid excessive consumption of alcohol and tobacco. They can irritate your bladder and especially make your symptoms worse.
-Eat healthily, especially avoid foods that are too sweet and fats. Eat lots of fruits and vegetables
-Avoid sitting in a sitting position for too long. But in the event that this is unavoidable, favor a comfortable seat
-Regular moments of relaxation and sufficient sleep are also essential.
-Avoid any other activity that generates pressure on the perineum that accentuates symptoms, for example, cycling.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
SOFT ERECTION NATURAL TREATMENT
ERECTION MOLLE NATURAL TREATMENT
When it comes to soft erection There are many causes that can lead to the inability of the penis to erect normally such as serious illnesses and psychological factors. All men with a weak erection problem show different causes and it is important to identify them correctly in order to apply the right treatment.
Therefore and in order to help you and completely eradicate these genes, the Health experts of Dawabio after much research offers you a very effective solution based on medicinal plants to treat a soft erection. Click on the image below to discover this natural treatment

We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
RECALL :
It is very important for men with impotence and other health problems to consult a doctor first to know the real state of your health and what will be the most appropriate treatments.
Usually, a flabby penis occurs in older men as they tend to have serious conditions like diabetes, kidney failure, high blood pressure, atherosclerosis, cardiovascular disease, and multiple sclerosis.
These diseases affect the nerves and also the circulation of blood to the penis. That is why, when you visit a doctor to discuss an impotence problem, he will ask you to examine your general health, as any of the slightly higher diseases can cause this sexual problem.
In the rest of our article we will outline some natural soft erection treatment.
1: Red vine, ginseng
If the erection gradually becomes poorer, without there necessarily being a drop in libido, and if the spontaneous erections in the morning or at night disappear, this often indicates a vascular cause. In this case, we can bet on circulatory plants such as sweet clover, red vine, witch hazel, horse chestnut ... We use them alone or in synergy (Quatuor Circulation, Super Diet; Nat & Form, etc.). 6 capsules per day or 5 ml of glycerine macerate (Phytostandard, Phytoprevent) morning and evening, for at least a month to treat sexual weakness or soft erection.
2: The "vegetable Viagra"
Tribulus Terrestris (also called " vegetable viagra ") and mucuna are two plants that act on the erection by promoting the production of testosterone. "This association is useful in the event of significant erectile problems associated with a decrease in libido", specifies the specialist.
Dosage: To be taken in the form of a glycerine macerate, 5 ml morning and evening as a minimum 3-month cure to see results.
3: Patchouli or pine essential oils
Essential oils with vasodilating virtues (pistachio lentisk, patchouli, palmarosa ...) can promote erection. Other oils with testosteronergic action can also help restart the machine if the problem is accompanied by a drop in libido: Scots pine, cumbawa, black spruce, Siam wood ... Aromatherapy can help. elsewhere be associated with herbal medicine to cure sexual weakness or soft erection.
4: A dietary supplement based on amino acids and vitamin B3
The combination of amino acids (l-arginine and l-carnitine) and vitamin B3 increases the production of nitrogen monoxide, thus promoting the vasodilation necessary for an erection. "The advantage is that you can take this dietary supplement continuously, to cure sexual weakness or soft erection. There is no need to plan the intake before sex, which helps keep sexual spontaneity This is interesting for those who experience a small decrease in libido which is accompanied by a decrease in erectile capacity but do not want or cannot take drugs such as Viagra, Cialis ... for medical reasons ", summarizes Annabelle Pongratz Muller-Vitu. It is in the form of sachets of powder to be diluted in water (Ezerex), in a cure of a one-month minimum.
5: An ylang-ylang massage
The psychic aspect of the erection is not to be neglected. "Tenderness, touch, caresses ... and the atmosphere of relationships are very important to restore dialogue and trust within the couple," recalls the sex therapist. To create favorable conditions, we can for example try to be massaged by (and massaged) his partner with a vegetable oil in which we dilute a few drops of essential oil, to be chosen for its fragrance, according to the smell that we feel. "talks" the most. Some ready-made massage oils (Light of Love massage oil, Essential Elements; Sensory Awakening massage oil, Puressentiel) contain essential oils known for their intoxicating and aphrodisiac fragrances: sandalwood, ylang-ylang, ... On the other hand, the essential oil will have no real therapeutic action by the cutaneous route.
6: A good workout
Sport is the number one ally of erection: it promotes good vascular health, improves self-esteem and endurance, lowers stress, helps fight against abdominal obesity which is very bad for the body. 'erection ", notes the specialist. No need to do much: 30 minutes 3 times a week already allow good maintenance at the cardiovascular level, which can only have a positive impact on the erection. help quickly find solutions to sexual weakness or your soft erection.
In general, a healthy lifestyle promotes a good erection and certain "enemies" should be avoided: alcohol, tobacco, cannabis.
Also to finish here are some foods that help treat erectile dysfunction :
· Dark chocolate: Yes, you read that right! Dark chocolate is an aphrodisiac and has many health benefits. It helps lower levels of the stress hormone cortisol and contains high levels of phenethylamine, a relaxing chemical that can also increase sexual pleasure. If all that wasn't enough, dark chocolate cocoa is rich in flavonoids; vasodilators that facilitate blood flow to the penis, and thus improve sexual weakness or soft erection.
· Bananas: Often embarrassing when eaten in public due to their resemblance to an erect penis! The fruit is very rich in potassium which is very beneficial for the heart and maintains good blood circulation, which is obviously essential for a strong erection. Potassium will also help maintain normal sodium levels and reduce the risk of high blood pressure. Bananas are also an excellent source of vitamin B and thus maintain your energy level and testosterone production, leading to higher libido.
· Chillies: Keep the heat with the chili in your sex life! Have you ever felt a rush of blood in your face and redness of the skin while eating chili peppers? This is because they work effectively to dilate blood vessels, and luckily not just on your face. When it comes to sex, they also do wonders by pumping more blood into the penis, and they work very quickly. However, it doesn't over-consume it, as it can irritate your stomach and intestines.
· Salmon: This is a fantastic food for weight loss because the fish generally do not contain carbohydrates and are perfect when combined with vegetables. Salmon is also good for the penis and thus may improve sexual weakness or flabby erection. Omega-3 fatty acids in oily fish help improve the functioning of your nervous system and promote healthy heart and blood circulation. towards the penis because of the enormous cardiovascular benefits they provide.
· Watermelon: This fruit has been shown to be a natural food similar to Viagra. The drug Viagra works by helping to relax and widen the blood vessels in the penis, allowing an easier erection when you are sexually aroused. Many experts claim that watermelon (or watermelon) works in a similar way due to the presence of "citrulline". Citrulline stimulates the production of arginine, an amino acid that helps relax and dilate blood vessels, thus improving blood circulation just like Viagra does.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
ALL ABOUT SPERMATOZOIDS: Bark, Roots, Herbal Teas, Plants
ALL ABOUT SPERMATOZOIDS: Bark, Roots, Herbal Teas, Plants
A spermatozoon is a mobile male reproductive cell (or gamete) involved in sexual reproduction. During fertilization, the sperm unites with an egg or an oocyte (female gamete) to form an egg cell, which will then develop into an embryo to give a new individual. This is how the Dawasanté experts provide you with a natural treatment to treat your problems with sperm abnormalities (oligospermia, necrospermia, asthenospermia, teratospermia, azoospermia, etc.).
Click on the image below to discover this natural treatment
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
The possible link between male infertility and chromosomal abnormalities in spermatozoa has been explored in several studies, since the advent of the technique of fluorescence in situ hybridization (FISH).
INTRODUCTION
Chromosomal abnormalities in humans may be responsible for infertility. In fact, the prevalence of abnormalities detected in the blood karyotype is ten times higher in infertile men than in the general population, ie around 5.3%, versus 0.6%. Numerical and structural abnormalities of the sex chromosomes are found with a high frequency, especially in men with severe azoospermia or oligo-astheno-teratospermia (OAT). The treatment of choice to remedy male infertility with OAT is Medically Assisted Reproduction (PMA) by Intra Cytoplasmic Sperm Injection (ICSI). However, it has been reported in recent years that the rate
of aneuploidy (abnormal number of chromosomes) of the sex chromosomes and de novo structural chromosomal abnormalities of paternal origin is higher in the offspring of these men. The risk of transmission of a chromosomal abnormality to offspring as the natural process of sperm selection is bypassed by the ICSI procedure should therefore be carefully considered and evaluated.
SPERMATOZOID CARYOTYPE AND FISH
Karyotypic analysis of spermatozoa makes it possible to determine in what proportion the gametes themselves are carriers of chromosomal abnormalities, in particular in infertile men.
In 1978, Rudak et al. described a technique for the karyotypic analysis of spermatozoa, based on the in vitro penetration of the latter into hamster oocytes. This technically heavy and delicate technique was only successfully practiced by a dozen laboratories around the world.
The technique of FISH (Fluorescence In Situ Hybridization) and its developments now make it possible to perform the chromosomal study of spermatozoa and analyze a large number of cells, using chromosome-specific probes that hybridize to particular regions of the DNA and can then be detected visually using a fluorescence microscope. For the FISH study, sperm from an ejaculate is spread on slides and undergo a chemical treatment resulting in the decondensation of their heads, while maintaining the structure that distinguishes them from other cells that may be in the ejaculate. Spermatozoa are also distinguished by the fact that they present signals corresponding to haploid and non-diploid cells. intact with clear hybridization signals are counted
MORPHOLOGICALLY NORMAL SPERMATOZOIDS
Morphology and motility are currently the parameters used to identify the sperm that will be microinjected as part of an ICSI procedure. Spermatozoa with an abnormal morphology are also more likely to present aneuploidy, but this risk has not been clearly quantified.
Ryu et al. studied the frequency of aneuploidy in sperm of normal morphology in infertile patients who are candidates for ICSI and all carriers of a normal blood karyotype compared to fertile patients. The morphology criterion used was that of Kruger. FISH analysis of chromosomes 18, X and Y were performed. In the group of infertile patients, and aneuploidy rate was found varying from 1.8% to 5.5% compared to 0% to 2.6% in the control patients. This result shows that the morphology of the spermatozoa is not an absolute criterion for the selection of a genetically normal spermatozoon.
Note that the different reported figures of sperm aneuploidy in men without fertility problems vary between 0 and 5% depending on the studies, differences which may be due to the use of probes with variable hybridization efficiency or to the visual interpretation of signals.
CHROMOSOMIC ANOMALIES, SPERMOGRAM AND LIFESTYLE
In a recent review, the sperm karyotypes of men without spermogram abnormalities were analyzed, with the aim of looking for possible correlations with age and lifestyle. The results of some fifty studies combining data from sperm analysis by FISH from 500 men (more than 5 million spermatozoa) were compiled. The results are an average reported rate of abnormality of 0.15% for each chromosome and 0.26% for sex chromosomes. The majority of chromosomes had an even distribution of abnormalities, with the exception of chromosomes 21, 22 and sex in which the frequencies of abnormalities were significantly higher. Trisomies 21 and 22 are also the most frequently found in the products of spontaneous miscarriages, showing the link between chromosomal abnormalities in spermatozoa and abnormalities found in the embryo. This work also demonstrated a slight increase in the frequency of disomies with paternal age, mainly for the sex chromosomes, but no effect of smoking, alcohol and caffeine consumption.
INFERTILITY AND KYOTYPES OF SPERMATOZOIDS
It is reported that 23% of men with azoospermia and 5-10% of men with OAT have an abnormal blood karyotype, resulting in a high likelihood of producing aneuploid gametes. It is known, for example, that the proportion of gametes with a chromosomal imbalance can be as high as 50% in men carrying a reciprocal translocation. However, a normal blood karyotype does not exclude the production of aneuploid gametes. An abnormal intra-testicular environment can affect spermatogenesis, in particular by disrupting the mechanisms controlling chromosome segregation during cell division.
A defect in spermatogenesis can have many origins such as systemic disease, malnutrition, endocrine disorders, obstructive pathologies and genetic defects. Indeed, a large number of severe OATs and azoospermia have genetic etiologies, including microdeletions at the level of the Y chromosome, abnormalities of meiosis, and mutations in the cystic fibrosis gene. However, “idiopathic” OAT remains the diagnosis most often retained in male infertility, despite extensive investigations to try to determine its origin. The main interest in identifying an etiology with OAT lies in the evaluation of the prognosis and the risk of producing embryos with chromosomal abnormalities.
A large study is now the source of much controversy over the relationship between spermogram abnormalities and potential risks of chromosomal abnormalities in ICSI. Fertilization and pregnancy rates obtained in relation to parameters of sperm number, mobility and morphology of infertile men were retrospectively analyzed in 966 cycles of ART with ICSI. The results showed comparable ICSI successes independent of the magnitude of OAT parameters. They concluded that in the extreme, only a living sperm in ejaculate can be sufficient for ICSI to be successful. While this study was therefore very reassuring, it does not
In order to study the etiology of “unlabelled” OATs, Calogero et al. used the FISH technique to explore the rate of aneuploidy in sperm chromosomes 8, 12, 18, X and Y in one group of patients with teratospermia, another with OAT and a control group. They observed similarly increased rates of aneuploidy in the first two groups, which suggested that teratospermia may be the critical endpoint associated with aneuploidy. The authors, therefore, recommended that a FISH analysis be performed in cases of teratospermia, before any attempt at ICSI. These same authors performed another study to try to relate the rate of sperm aneuploidy in eighteen men with OAT and the results of ICSI in affected couples. For these cases of OAT, and overall fertilization rate of 95% and a pregnancy of 39% was obtained. Very curiously, this pregnancy rate was significantly higher than reported by multiple centers practicing the ICSI technique (the generally accepted average rate is around 25%), which the authors of the article do not discuss. The rate of oocyte fertilization by ICSI was independent of the rate of aneuploidy. On the other hand, the patients who had not had a pregnancy (91%) had significantly higher aneuploidy rates than those of the controls.
Bernardini et al. also analyzed by FISH the rate of aneuploidy of the spermatozoa for chromosomes 1, 17, X, and Y, on a series of twenty-two cases of infertile men compared to fertile controls. A significantly higher rate of aneuploidy was found in men with OAT (18%) compared to controls (2.28%).
In the case of azoospermia patients, it is now sometimes possible to perform ICSI after a testicular biopsy in which sperm is found. The reported numbers of chromosomal abnormalities are impressive: indeed, one study estimated the proportion of chromosomal abnormalities at 19.6% in a group of patients with non-obstructive azoospermia and 8.2% in those with obstructive azoospermia. Here again, the link between gonadal insufficiency and the presence of chromosomal aneuploidies is well demonstrated.
It can be concluded from these data that a high rate of aneuploidy in spermatozoa is associated with a low rate of pregnancy and therefore less success through assisted reproduction by ICSI. However, the rate of fertilization of the oocytes does not seem to depend on the rate of aneuploidy, which means that the transferred embryos are more often carriers of aneuploidies and that on the other hand, their implantation would be disadvantaged. In this context, genetic counseling following a FISH analysis of the sperm would be highly desirable, before a couple begins a long and difficult procedure of assisted reproduction by ICSI.
SPERMATOZOID ANEUPLOIDS AND GENE FACTORS
A particularly important point of these studies is that they make it possible to explain certain male infertilities so far called “idiopathic”. In fact, disturbances of meiosis or premeiotic mitosis during spermatogenesis could predispose to the non-chromosomal disjunctions that are observed. The next step would consist in identifying which are the genetic factors at the origin of these disorders of meiosis and mitosis and to characterize them to have one more diagnostic means available in idiopathic male infertility. If gene abnormalities predisposing to non-disjunctions were detected, this diagnostic tool would be available and the possible transmission in the offspring of this pathology would be evaluable. And then supported by numerous studies. We now know that at least thirty genes are involved in the control of meiotic and mitotic divisions. For example, the role of HspA2, a “chaperone” protein with a specific testicular expression that is thought to be involved in the synaptonemal complex has recently been demonstrated. The role of genes of the MAD (Mitotic Arrest Deficiency) family involved in premeiotic mitotic control is also discussed.
There is a case, recently reported in the literature, where FISH analysis of spermatozoa made it possible to pose a contraindication to ART. In the study in question patients with different types of absolute teratospermia (100%) were studied. One of them had a sperm morphological abnormality consisting of macrocephaly and multiple flagella. In this patient, 90% of the sperm analyzed by FISH presented aneuploidy. This result was considered to be a contraindication to ICSI.
FEASIBILITY
In these various studies, between 3000 and 10,000 sperm per patient are analyzed. This represents a significant investment of time, considering that for FISH analysis on amniocytes, there are routinely between 50 and 100 cells. It is estimated that to detect significant levels of aneuploidy in sperm, an analysis of around 1000 cells may be sufficient. The method of collection is no different from that for a spermogram, and only a small fraction of ejaculate is used to smear onto slides for chemical treatment of the sample prior to FISH.
CONCLUSION
While the use of FISH on spermatozoa in male infertility appears undoubtedly valuable and contributory in the context of a pre-ART workup, or after repeated ART failures, the formal indications for this analysis have not yet been clearly established. established. One of the first uses of this approach could be to give couples undergoing a pre-ICSI procedure for OAT or azoospermia a more detailed indication of the chances of success and risks of miscarriages due to chromosomal abnormalities potentially present in the sperm. This information should then be communicated to patients within the framework of genetic counseling, taking into account the psychological repercussions of a possible poor prognosis of success.
Some authors also consider that this technique can be used in the event of miscarriages with repetitions of undetermined etiology beyond the framework of male infertility. Indeed, if 60% of the miscarriages of the first trimester are due to chromosomal abnormalities and a majority are of maternal origin, the FISH technique on the spermatozoa has shown a paternal origin in 8 to 12% of cases, corresponding to a greater incidence of chromosomal abnormalities in their gametes.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.

OLIGO-ASTHENO-TERATOSPERMIE
OLIGO-ASTHENO-TERATOSPERMIA
You have been trying to have a baby for several months, but it is late. After tests, your doctor told you that your loved one has oligoasthenoteratospermia (OATS). What are OATS and what are the consequences?
However, the experts at Dawasanté provide you with a natural treatment to permanently cure oligo- asthenoteratospermia.
Click HERE or on the image below to discover this natural treatment
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
What is Oligoasthenoteratospermia or OATS?
OATS designates a set of abnormalities found during the spermogram during a male infertility assessment. The OATS groups together a low concentration of sperm (oligo) with therefore too few spermatozoa to naturally fertilize an oocyte, too low mobility of these spermatozoa (astheno) which does not allow them to join the oocyte and too large a proportion abnormal sperm (terato). However, OATS can present varying degrees. It can be severe, with very low mobility and concentration indices while the malformation index is very high. It can be moderate with indices closer to normal. Intermediate forms exist with indices of the same degree or which may be of different degrees: severe for one or two types of indices (eg: mobility and concentration) and moderate for the third.
What happens after diagnosis of the OATS?
Once the OATS is discovered, the doctor will look to determine if there are any causes for these abnormalities. Indeed, OATS can be reduced, at least in part, depending on its origin. He will look first for signs of infections, old or recent. Some infections, such as chlamydia, can cause a decrease in male fertility. Their treatment can help regain better fertility. Likewise, the treatment of a varicocele (varicose veins in one or both testicles) or stopping smoking may improve the results of a spermogram. Further research will be carried out to find out if there is a malformation in the testes or seminal tract. In all cases, a second spermogram will be done because it is possible that significant variations appear and allow to hope for other opportunities for natural fertilization.
What to do to have a child in the event of OATS?
If the diagnosis of OATS is confirmed, the possibility of natural fertilization is reduced. However, it does exist, especially if it is a moderate form. However, certain factors, such as the woman's age or the length of time contraception has been stopped must be taken into account and assisted reproduction (ART) may be considered. Depending on the case, it will be an in utero insemination (IUI) where the sperm is introduced directly into the uterus, and in vitro fertilization (IVF) where the sperm is brought into contact with one or more oocytes in the laboratory or an intracytoplasmic sperm injection (ICSI) where sperm is introduced directly into an oocyte in the laboratory. These different techniques will be offered depending on the degree of OATS. The success of IVF or ICSI is of the order of 25 to 30% which leaves hope to those who are concerned by this difficulty.
Asthenospermia is an abnormality of the sperm that is characterized by insufficient mobility while their number remains normal. Also called asthenozoospermia, this sperm fatigue is one of the possible causes of male fertility problems. What are the main causes? How is asthenospermia diagnosed? What treatment is there to promote procreation?
What is asthenospermia due to?
The main causes that can explain unsatisfactory sperm mobility are:
- a morphological anomaly of the male gametes,
- an infection,
- presence of anti-sperm antibodies
- medication,
- a varicocele,
- a dietary deficiency,
- a renal failure,
- liver failure
- chemotherapy,
- exposure to radiation,
- excessive alcohol consumption,
- a deficiency in calcium, vitamin D, or trace element ...
How is asthenospermia diagnosed?
A semen analysis, or spermogram, is used to assess the mobility of the sperm. It should be remembered that only mobile gametes can fertilize the egg. Many medical analysis laboratories rely on the classification decreed by the World Health Organization to classify spermatozoa:
- Level A (or I): progressive rapid sperm advance quickly and in a straight line,
- Level B (or II): the slow progressive spermatozoa advance slowly or in a curved line,
- Level C (or III): non-progressive spermatozoa move but do not progress,
- Level D (or IV): the sperm are immobile.
To be qualified as normal, the spermogram must show a minimum of 40% of motile spermatozoa and 32% of spermatozoa showing progressive mobility.
What solutions to have a child?
The management of asthenospermia varies mainly according to its origin. Thus, an infection will have to be treated according to its nature with appropriate antibiotic drugs while certain testicular abnormalities may, in some cases, be the subject of surgery. While there is no curative treatment for asthenospermia, certain drugs help improve the quality of sperm: vitamins, hormones, alternative medicine (herbal medicine, homeopathy, aromatherapy, etc.). When the treatments do not give satisfactory results, in vitro fertilization with donor sperm or an intracytoplasmic injection of sperm may be considered in the context of Medically Assisted Reproduction ( MAP).) when the couple wants a child.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
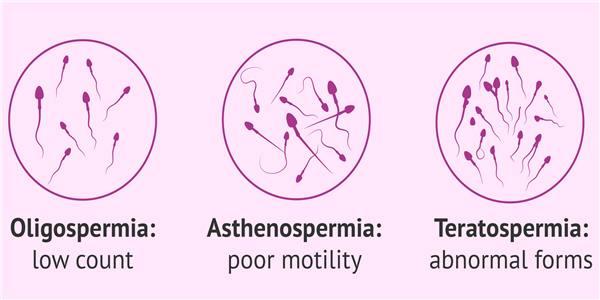
MALE INFERTILITY TERATOSPERMIA
The teratospermia (or teratospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. However, the experts at Dawasanté provide you with a natural treatment to permanently cure teratospermia and allow you to conceive quickly.
Click here or on the image below to find out what treatment
We deliver all over the world.
For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number.
Teratospermia is a sperm abnormality characterized by sperm with morphologic defects. These abnormalities can affect different parts of the sperm:
- the head, which contains the nucleus carrying the 23 paternal chromosomes;
- the acrosome, a small membrane at the front of the head that, at the time of fertilization, will release enzymes that will allow the sperm to cross the pellucid area of the oocyte;
- the flagellum, this "tail" which allows it to be mobile and therefore to move up from the vagina to the uterus and then the tubes, for a possible encounter with the oocyte;
- the intermediate part between the flagellum and the head.
Often, the anomalies are polymorphic: they can be multiple, in size or shape, affect both the head and the flagellum, vary from one sperm to another. It may be globozoospermia (absence of acrosome), double flagellum or double head, coiled flagellum, etc.
All these abnormalities have an impact on the fertilizing power of the sperm, and therefore on the fertility of the man. The impact will be more or less important depending on the percentage of normal sperm remaining. Teratospermia can decrease the chances of conception and even lead to male infertility if it is severe.
Often, teratospermia is associated with other spermatic abnormalities: oligospermia (insufficient number of spermatozoa-, asthenospermia (defect in sperm mobility. We then speak of oligo-asthenic-teratozoospermia (OATS).
Like all sperm abnormalities, the causes can be hormonal, infectious, toxic, drug-related. The morphology of spermatozoa is in fact the first parameter to be altered by an external factor (exposure to toxicants, infection, etc.). More and more specialists also consider that atmospheric and food pollution (via pesticides in particular) has a direct impact on the morphology of spermatozoa.
But sometimes, no cause is found.
The main symptom of teratospermia is difficulty conceiving. The fact that the shape of the sperm is abnormal does not affect the occurrence of malformations in the unborn child, but only the chances of pregnancy.
Teratospermia is diagnosed using a spermogram, one of the first examinations systematically performed in men during an infertility assessment. It allows a qualitative and quantitative study of sperm thanks to the analysis of different biological parameters:
- the volume of the ejaculate;
- pH;
- sperm concentration;
- the mobility of sperm;
- sperm morphology;
- the vitality of sperm.
The part about sperm morphology is the longest and most difficult part of the spermogram. In a test called a spermocytogram, 200 sperm are fixed and stained on smear slides. Then the biologist will study the different parts of the sperm under a microscope in order to assess the percentage of morphologically normal sperm.
The type of morphological abnormalities is also taken into account to estimate the impact of teratospermia on fertility. Several classifications exist:
- the David classification modified by Auger and Eustache, still used by certain French laboratories;
- the Kruger classification, the WHO international classification, is the most widely used in the world. Carried out using an automatic machine, this more “severe” classification classifies as atypical spermatozoa any spermatozoon which deviates, even very little, from the form considered as normal.
If the proportion of correctly formed sperm is less than 4% according to the WHO classification, or 15% according to the modified David classification, teratospermia is suspected. But as for any spermatic abnormality, a second or even a third spermogram will be carried out 3 months apart (the duration of a spermatogenesis cycle being 74 days) in order to make a firm diagnosis, especially as various factors can influence on sperm morphology (long abstinence time, regular cannabis intake, feverish episode, etc.).
A migration-survival test (TMS) usually completes the diagnosis. It makes it possible to have an evaluation of the number of spermatozoa able to end up in the uterus and able to fertilize the oocyte.
A sperm culture is often coupled with the spermogram in order to detect an infection which could alter spermatogenesis and lead to morphological defects of the sperm.
Teratospermia occurs when less than 4% of the sperm present in the male ejaculate is said to be “typical” or normal. The remaining 96% are carriers of abnormalities or have an alteration in their morphology. A normal sperm consists of an oval head, an intermediate body one and a half times longer than the head, and a long, thin tail (the flagellum) which promotes its mobility. The abnormalities detected can affect the head of the spermatozoon as well as its intermediate part or even its flagellum. There are also combined forms of anomalies.
Teratospermia is usually the cause of male infertility. Indeed, alterations in the morphology of spermatozoa can affect their mobility and prevent them from reaching the egg. There are different degrees of severity of teratospermia which can be classified as mild, moderate, or severe. The higher the degree of severity, the more difficult natural procreation will be.
Little is known about the causes of this anomaly. The origin can be infectious, medicinal, genetic, anatomical (varicocele or varicose veins of the testes), environmental or related to the hygiene of life. Finally, there are reversible forms of teratospermia. This is why the patient is generally asked to perform a second examination, 3 months apart from the first, in order to detect the persistence of the anomaly.
We deliver all over the world.
For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number.
UNDERSTANDING THE SPERMOGRAM: Natural treatment
UNDERSTANDING THE SPERMOGRAM
The semen is the result of the laboratory examination of the semen. Regardless of the poor quality and quantity of your sperm, Dawasanté experts provide you with a natural herbal treatment to improve the quality and quantity of your sperm. This will allow you to conceive quickly and be more fertile. Click on the image below to discover this natural treatment
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Topic: AKINETOSPERMIA, ASPERMIA, ASTHENOSPERMIA, AZOOSPERMIA, Cryptozoospermia, DYSKINESIA, FLAGELLAR, HYPERSPERMIA, HYPOSPERMIA, AGGREGATES, LEUCOSPERMIA, NECROSPERMIA, Oligo-Asthenoospermia, TOSPEROPERMIA, POLYPERSPATERMIA, TERATOSPERSPATERMIA, TOSPEROPERMIA
I - WHAT IS A SPERMOGRAM?
The spermogram is an analysis that will study the quantity and quality of sperm.
The spermogram is carried out after having collected the sperm in the laboratory and by masturbation.
The spermogram includes:
1 - An analysis of the volume of the ejaculate
2 - A determination of the pH
3 - The study of the mobility of the spermatozoa at the emission of the sperm and after 1 hour and 3 hours
4 - The calculation of the number of spermatozoa
5 - Their vitality
6 - Viscosity
7 - The percentage of abnormal forms observed under the microscope…
In addition, we also evaluate:
8 - The level of isolated flagella and / or lysed spermatozoa
9 - The level of white line cells
10 - The level of other cells (cells of the urogenital tract)
11 - The level of cell fragments
12 - The presence of red blood cells or blood residue
II - REFERENCE VALUES
1 - Quantity
2 to 6 ml
2 - Color
Normally viscous and opalescent white
3 - viscosity
On ejaculation, the sperm coagulates and liquefies in less than 30 minutes at 37 ° C
4 - Number
- From 40 million to 200 million per ml.
- Greater than 15 million per ml and must be greater than 39 million
for the entire ejaculate
5 - Mobility
This is the most important parameter
The mobility standard accepted after 30 minutes of the emission must not be below 80% of motile spermatozoa
- After 1 hour -
We must find more than 50% of motile spermatozoa
that is to say in progressive displacement
- After 3 hours -
We must find at least 30% of motile spermatozoa
Observation
The mobility of sperm is classified into four categories or grades (see below).
6 - Vitality
At ejaculation, the percentage of living spermatozoa must be
equal to or greater than 60% of all spermatozoa
7 - Leukocytes
The number of leukocytes must be less than 1 million / ml
8 - Abnormal forms
- According to the classification of Cohen Bacri
Abnormal forms should not exceed 15 to 20% of the total sperm
- According to the classification of “David”
Abnormal forms must not exceed 30%, of the total sperm
- According to the classification of “Kruger”
Abnormal forms must not exceed 4%, of the total spermatozoa
9 - The pH
It must be between 7.2 to 8
Good to know
The pH is a direct indicator of secretions from the annex glands (acid prostatic secretions and secretions from the seminal vesicles).
10 - Germ cells
Their percentage must not exceed 10%
Germ cells are the basic cells that evolve into the sperm after a complex transformation; a higher level may suggest a disorder in sperm production.
III - INTERPRETATION OF THE RESULTS
Male infertility can be caused:
1 - By poor quality sperm production
2 - By insufficient sperm production
3 - By an anomaly in the transport of these spermatozoa
Spermatozoon and its various abnormalities
IV - THE MAIN ANOMALIES
1 - HYPOSPERMIA
The total volume of the ejaculate less than 2 ml
The causes of hypospermia are varied:
- Technical problem in collecting sperm
- Abstinence
- Secretion deficit
- Retrograde ejaculation…
Good to know
The volume of semen gradually decreases with age without altering the other parameters.
2 - HYPERSPERMIA
The volume of the ejaculate much greater than normal
Hyperspermia and sometimes in connection with an inflammatory or infectious syndrome of the annex glands and more particularly the seminal vesicles.
Important
It can also be due to excessive sexual abstinence.
3 - OLIGOSPERMIA (OLIGOZOOSPERMIA)
It corresponds to an insufficient quantity of spermatozoa in the semen
Very important to know
1 - If the number of spermatozoa is less than 10 million / ml, there is infertility
2 - If the number of sperm is less than 5 million per ml, we speak of severe oligospermia.
4 - POLYSPERMIA
The concentration of spermatozoa greater than 200 million per ml
5 - AZOOSPERMIA
Absence of spermatozoa in the ejaculate
Two types of azoospermia are encountered:
1 - Secretory azoospermia -
Corresponds either to a primary, congenital or acquired testicular disease, or to an acquired congenital hypothalamic-pituitary insufficiency.
2 - Excretory azoospermia -
Corresponds to the presence of an obstacle in the excretory tract (epididymis, vas deferens, ejaculatory ducts).
These lesions can be acquired or congenital.
6 - ASTHENOSPERMIA Sperm
mobility defect
We speak of asthenospermia if at least 40% of the spermatozoa encountered are not mobile.
Sperm mobility is classified into four categories or classes -
1 - Class A -
Fast and progressive spermatozoa (speed> 25 µm / s)
2 - Class B -
Slow or weakly progressive spermatozoa (speed 5 - 25 µm / s)
3 - Class C -
Mobile spermatozoa but without any progressivity (mobility in place)
4 - Class D -
Immobile spermatozoa
 7 - NECROSPERMIA (NECROZOOSPERMIA)
7 - NECROSPERMIA (NECROZOOSPERMIA)
It is characterized by a very high percentage of dead spermatozoa
Necrospermia is often due to microbial infections.
There are two types of necrospermia:
1 - Partial necrospermia -
Corresponds to 42% of the spermatozoa found are dead
2 - Total necrospermia -
Corresponds to all the sperm found in the ejaculate are dead
8 - TERATOSPERMY OR TERATOZOOSPERMIA
It corresponds to an excessive quantity of abnormal spermatozoa
and can reach up to 30%
(see above, abnormal forms).
The main abnormal forms encountered are -
1 - Head abnormalities (less than 35%) -
Microcephaly, macrocephalic, elongated head, irregular head ...
2 - Anomalies of the intermediate part (less than 20%) -
The result from the presence of cytoplasmic remains
3 -Flagellum abnormalities (less than 20%) - Angulated, coiled flagellum ...
4 - Double forms (less than 10%) -
5 - The globozocephalic form -
Characterized by the absence of the acrosome.
The presence of this form is a sign that there is no possibility of fertilization.
9 - ASPERMIA
A total absence of ejaculate
10 - OAT
(Oligo-Astheno-Teratozoospermia)
It is the association of three pathologies and which are: Oligospermia, Astheno-spermia and Teratozoospermia.
11 - AGGLUTINATES
Agglutinates (or adjoining) correspond to a gathering of several spermatozoa living together.
The agglutinates are explained by the presence of living sperm and carriers of anti-sperm antibodies.
The presence of agglutinated spermatozoa should cause the presence of anti-sperm antibodies to be tested.
12 - AGGREGATES
They are to be distinguished from agglutinates because they correspond to the joining of several spermatozoa which have died together.
13 - FLAGELLAR DYSKINESIA
Abnormalities in the movements, speed and trajectory of spermatozoa
14 - LEUCOSPERMIA
Leukocytosis at more than 1 million / ml
This leukospermia suggests an infection
15 - AKINETOSPERMIA
All spermatozoa are immobile
16 - CRYPTOZOOSPERMY *
Absence of spermatozoa observed in a drop of sperm under the microscope
A thorough search in the whole of the sperm allows one to find some spermatozoa (less than 100,000 spermatozoa in the whole of the ejaculate).
There are two main cryptozoospermia -
1 - Severe cryptozoospermia
The number of spermatozoa found is less than 10,000
2 - Moderate cryptozoospermia,
The number of spermatozoa is greater than 10,000
* Important -
Cryptozoospermia is a new entity which has only gained interest since the appearance of the ICSI technique (Intra Cytoplasmic Sperm Injection) because with this technique, just a few spermatozoa ejaculated or taken from epididymis or testis, and regardless of sperm concentration and mobility, to achieve fertilization and pregnancy.
The appearance of the new technique of IMSI (Intra Cytoplasmic Morphologic Sperm Injection) which makes it possible to make a very thorough selection of the best spermatozoa in the ejaculate and to significantly increase the chances of obtaining fertilization and pregnancy from cryptozoospermic sperm.
17 - HEMOSPERMIA
It is the presence of blood in the sperm
V - APPENDIX
Seminal biochemistry -
It makes it possible to pose different types of pathology either having an origin of an obstacle being on the seminal tract, or of origin by malformation of the ways of excretion of the spermatozoa and more particularly at the level of the epididymis, duct vas deferens, seminal vesicles, prostate.
The main substances of dosed are carnitine, alpha-glucosidase, citrate, acid phosphatases, zinc, fructose, etc.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
TERATOSPERMIA AND PREGNANCY: Natural treatment
The teratospermia (or teratozoospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. However, Dawasanté experts provide you with a natural plant-based treatment to treat your teratospermia and allow you to conceive quickly.
Click HERE or on the image below to discover this natural treatment.

We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Obtaining a natural pregnancy with teratozoospermia can be complicated, and in the most severe cases it is virtually impossible for fertilization to take place and the embryo to develop afterward.
Men who are infertile with teratozoospermia will need to use assisted reproduction techniques to become parents.
The appropriate treatment for PMA will depend on many factors, not just the degree of sperm abnormalities. The rest of the seminal parameters, as well as the age and state of health of the woman, are also limiting when it comes to achieving pregnancy.
Below you will find an index with all the points that we will cover in this article.
1-Natural pregnancy
Amorphous sperm can make pregnancy difficult for any of the following reasons:
- They have more difficulty moving due to their abnormal shape, which prevents them from reaching the egg in the fallopian tube .
- Abnormalities in the head can prevent sperm from entering the egg so it can be fertilized.
- When the cause of teratozoospermia is genetic, the resulting embryo may have DNA alterations that prevent its correct development.
Infertility due to teratospermia
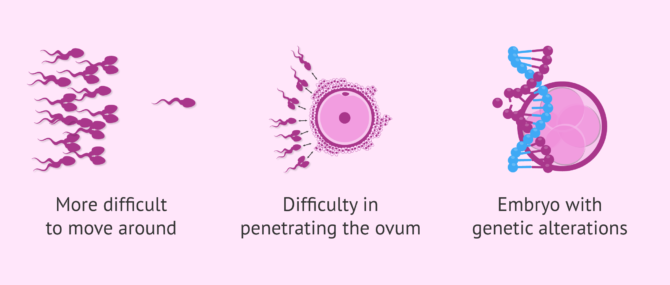
All these reasons make natural pregnancy not possible or its arrival is delayed.
When the degree of teratozoospermia is low, the normal sperm that exists in the semen could lead to a viable pregnancy. Depending on the parameters of sperm concentration and mobility, the probability of natural pregnancy with teratozoospermia will be higher or lower.
On the other hand, when teratozoospermia is moderate, severe or associated with another disorder ( oligozoospermia or asthenozoospermia ), the couple will most likely need ART treatment to have a child.
2-Medically assisted procreation treatments
Once the diagnosis of teratospermia has been obtained, depending on its severity and other values of the spermogram, the specialist will recommend the treatment that offers the best guarantees of success in the couple.
It should be noted that the reproductive status of women also plays an important role in this decision. When the male factor is the problem, there are several assisted reproduction techniques that can be performed depending on the characteristics of each patient.
2-1 Artificial insemination (AI)
The artificial insemination is the introduction of sperm directly into the uterus of a woman to get pregnant. Beforehand, it will be necessary to perform the capacitation of the sperm sample and to perform ovarian stimulation in the woman.
This assisted reproduction treatment can give good results in cases of mild teratozoospermia (3-4% of sperm are normal), provided that the number and mobility of sperm are affected.
To perform artificial insemination, a man must obtain a total of 2-3 million progressively motile sperm in the REM spermogram.
In addition, the woman must be under 35 - 36 years old, have leaky fallopian tubes and have no other serious infertility problem. If you want more information about this treatment, we recommend that you consult the following article: What is artificial insemination?
2-2 In vitro fertilization (IVF)
IVF is one of the most important treatments for assisted human reproduction. It consists of taking several mature eggs from the woman after ovarian stimulation and follicular puncture, then putting them in direct contact with male sperm and carrying out fertilization.
This method offers good results in cases of moderate teratozoospermia (1-2% of normal sperm) or mild teratozoospermia when the woman is over 35 years old. It would also be the treatment to try if, after several artificial inseminations, no pregnancy is obtained.
There is a variant of IVF in which fertilization is forced by the direct introduction of the sperm into the egg. This is called an intracytoplasmic sperm injection ( ICSI ).
ICSI is mainly used in cases of severe teratozoospermia (total normal sperm is less than 1%) or if the above techniques have not worked.
However, most IVF treatments today use ICSI as a technique for creating the embryos, as it offers a higher success rate than conventional IVF.
We recommend that you read the following article for more detailed information on this technique: What is ICSI and how much does it cost?
PMA, like any medical treatment, requires that you trust the professionalism of the doctors and clinic you have chosen. Obviously, not all are the same. The Fertility Report selects the most advantageous clinics for you based on our rigorous quality criteria. In addition, the system performs a comparison of prices and conditions offered by different clinics to facilitate your decision making.
2-3 IMSI
The IMSI is a variant of the ICSI technique that was discussed in the previous section. It is based on a more rigorous selection of the spermatozoa to be micro-injected according to their morphology.
To do this, we use an electron microscope with a superlens that offers a magnification of over 6,000 times.
This technique offers many advantages in the case of teratozoospermia because it allows us to visualize in detail the morphology of the spermatozoa and to choose the best ones.
Another benefit of IMSI is that it reduces the likelihood of miscarriage with its use.
The IMSI technique

If you want to know more about it, you can read the following article: What is IMSI?
3-Your frequently asked questions
3-1 Which assisted reproduction treatment is most appropriate for a pregnancy when the man has teratozoospermia?
By Zaira Salvador (embryologist).
The fertility treatment indicated for a couple with teratospermia will depend on various factors, such as the degree of teratozoospermia, the age of the woman, the time of infertility, etc.
The most appropriate, in general, would be to undergo in vitro fertilization (IVF) treatment with intracytoplasmic sperm injection (ICSI).
Read more
3-2 Can abnormal sperm cause miscarriages?
By Zaira Salvador (embryologist).
Having teratozoospermia does not imply that there is a greater risk of miscarriage when the pregnancy has already been achieved. However, if the cause of teratozoospermia is genetic and the sperm carry DNA mutations, a miscarriage or the birth of a sick child could occur.
3-3 Can teratozoospermia lead to pregnancy with Down syndrome?
By Zaira Salvador (embryologist).
Teratozoospermia is not directly related to trisomy 21, which is the chromosomal alteration that causes Down syndrome. However, sperm with abnormal morphology may have genetic abnormalities that cause fertilization failures, a greater likelihood of miscarriages, or other pathologies.
3-4 What is the appropriate treatment for a couple with teratozoospermia and PCOS?
By Zaira Salvador (embryologist).
Treatment will depend on the degree of teratozoospermia and the age of the woman. If the teratozoospermia is mild and the woman is under 35, it is possible to try artificial insemination. If the above requirements do not work or are not met, in vitro fertilization would be necessary.
It is estimated that 30 to 40% of fertility disorders are due to abnormalities in the fertility of the male partner. In men, infertility is related to the quality and number of sperm in semen.
Male fertility abnormalities
There are four types of sperm abnormalities, which can be associated in the same person.
What is azoospermia?
We speak of azoospermia when the semen does not contain sperm. This fertility disorder may be due to:
- absence or abnormality in the production of sperm (for example, in a man who has undergone cancer treatment with radiotherapy to the pelvis or chemotherapy, and whose cells that make sperm have been damaged by this treatment) ;
- blockage of the pathways used by sperm from the testes to the organs where sperm is stored (the seminal vesicles). Sometimes the transport channels are blocked and the sperm cannot travel to the seminal vesicles. These obstacles may be congenital or due to an ill-treated sexually transmitted infection.
What is oligospermia
We speak of oligospermia when the sperm contains too low a number of sperm. The causes of oligospermia are similar to those of azoospermia.
What is teratospermia?
The teratospermia is the presence of sperm "abnormal" in large numbers in semen. It is due to a manufacturing defect in the testicles. Malformed sperm have difficulty moving or fail to enter the oocyte.
What are the risk factors for male fertility disorders?
Some risk factors for infertility have been identified in humans:
- age (over 40);
- smoking or alcoholism ;
- factors that expose the testes to too high a temperature (too frequent hot tubs and baths, saunas and steam rooms, too much time spent driving, etc.): the production of sperm requires a temperature of the testes lower than that of the body (i.e. is for this reason that they are outside). Sometimes, the venous circulation is bad at the level of the testicles (it is the “varicocele”) and their temperature increases with a higher risk of infertility.
- toxic products used in certain professions;
- a medical history (especially cancer treatment or mumps).
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
TERATOSPERMIA TREATMENT: Can it be cured?
The teratospermia (or teratozoospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. However, Dawasanté experts provide you with a natural plant-based treatment to improve the quality and quantity of your sperm.
Click HERE or on the image below to discover this treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Teratozoospermia can occur from birth, which is thought to be due to a genetic cause or be acquired over time through hormonal changes or trauma. Depending on the cause, it will be possible to apply personalized treatment to reverse this situation.
In congenital cases of teratozoospermia, it is very difficult to obtain a cure. The same is true when these changes are the result of cancer treatment. In severe cases of teratozoospermia, assisted reproduction will be necessary to become parents.
However, when the degree of teratospermia is lower, there are pharmacological or natural treatments that can help restore sperm quality.
Natural treatment
Since the exact cause of teratozoospermia is not known, it is difficult to apply a solution to problems with sperm morphology.
However, a healthy lifestyle can greatly influence the quality of sperm. For this reason, there may be variations in sperm values within a few months of each other.
Proper treatment should ensure that the process of sperm maturation during spermatogenesis proceeds properly. Therefore, we are going to discuss some recommendations for maintaining good habits that promote this correct formation of sperm.
1-1 Power supply
A healthy and balanced diet improves general health. In addition, the vitamins and antioxidants contained in certain foods also provide benefits to the quality of sperm.
These are some of the important components that a man should include in his diet to improve his fertility status:
- Selenium
- Vitamin C
- Zinc
- Omega-3 fatty acids
- this mineral is found in Brazil nuts, walnuts, tuna, beef, chicken, eggs and cheese. It should be taken in small amounts, otherwise it can be toxic.
- in spinach, tangerines, strawberries and tomatoes. Vitamin C is a powerful antioxidant and also helps in the absorption of iron.
- it is a mineral found in foods such as oysters, clams or red meat. Zinc is essential for the functioning of enzymes, which are responsible for producing energy in the body.
- in fatty fish and crustaceans. It is very important to include them in the diet because the human body is not able to synthesize them on its own. In addition, it brings multiple benefits to the cardiovascular system, the nervous system, the immune system, etc.
- Healthy and balanced diet to cure teratozoospermia

1-2 olive oil
Olive oil is essential in the Mediterranean diet and also has reproductive properties thanks to its oleic acid content.
Oleic acid acts as a lowering agent for bad cholesterol or LDL levels which can build up in the testes, making it difficult to produce sperm properly.
Olive oil also helps raise good cholesterol or HDL levels and prevent the risk of heart and brain complications.
In short, olive oil is an ally in the fight against male infertility and especially teratozoospermia.
PMA, like any medical treatment, requires that you trust the professionalism of the doctors and clinic you have chosen. Obviously, not all are the same. The Fertility Report selects the most advantageous clinics for you based on our rigorous quality criteria. In addition, the system performs a comparison of prices and conditions offered by different clinics to facilitate your decision making.
1-3 Avoid heat
High temperatures in the testes affect sperm production and can cause sperm abnormalities.
Therefore, men with infertility issues should consider the following recommendations:
- Do not use the laptop on your legs.
- Avoid saunas in general.
- Wear boxers and wide pants.
- Try not to cycle long distances.
Once the temperature decreases and the heat exposure decreases, the testes return to their normal function and the quality of sperm improves in a short time.
1-4 Eliminate toxins
Some compounds that we are exposed to on a daily basis can be very harmful to reproductive health without our being aware of it.
Tobacco, drugs, marijuana smoke, pesticides, chemicals, and excessive amounts of alcohol can cause sperm deformity.
It is therefore important to eliminate these bad habits from your environment.
2-Vitamin supplements
In some cases of teratozoospermia, it is common for the urologist to advise the administration of certain nutritional supplements that supplement the diet in order to obtain a better result.
The most common treatment is a vitamin and antioxidant supplementation.
Antioxidants are responsible for reducing the oxidative stress to which sperm are exposed, which causes cell damage and the fragmentation of their DNA.
Some recommended dietary supplements include vitamin E or essential amino acids like L-carnitine. Vitamin E treatment is also recommended for chemotherapy and radiation therapy, as it is a very powerful antioxidant.
On the other hand, Andean maca supplements are also very beneficial due to the multitude of properties of this Peruvian plant.
It should be noted that these compounds are not miraculous and that in no case will it be possible to regain total fertility if the seminal parameters are severely affected.
However, when there is mild teratozoospermia, they can help and give a little boost for men with vitamin deficiencies in the diet.
Peruvian Maca powder to treat teratozoospermia

3-Your frequently asked questions
3-1 Is there a cure for severe teratozoospermia?
If a man has less than 5% of sperm with normal morphology, it is very difficult to find a normal value with natural or pharmacological treatment. Improvement can be seen over time, especially if the man maintains a healthy lifestyle.
On the other hand, if the teratozoospermia appears associated with another pathology such as, for example, varicocele, it is possible that the spermogram improves its parameters during a surgical intervention to eliminate the varicocele.
3-2 Can acupuncture be of benefit in the treatment of teratozoospermia?
There are studies that say yes. In general, acupuncture has been successful in increasing pregnancy rates in idiopathic infertility, that is, when the origin is unknown. An improvement in seminal quality has also been observed in men with oligospermia, asthenospermia and teratospermia who practice acupuncture.
3-3 Does eating forest fruits improve seminal quality?
Yes, many forest fruits have antioxidant pigments and a great capacity for absorbing oxygen free radicals, so this food group is perfect if you want to improve or protect sperm quality.
Some research has uncovered the medicinal properties of pigmented polyphenols, such as flavonoids, anthocyanins, tannins and other phytochemicals present in the skin and seeds of these fruits.
Moreover, blueberries, blackberries, currants and strawberries are rich in vitamin C and other nutrients. Vitamin C is a powerful antioxidant that protects cells from cellular damage.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
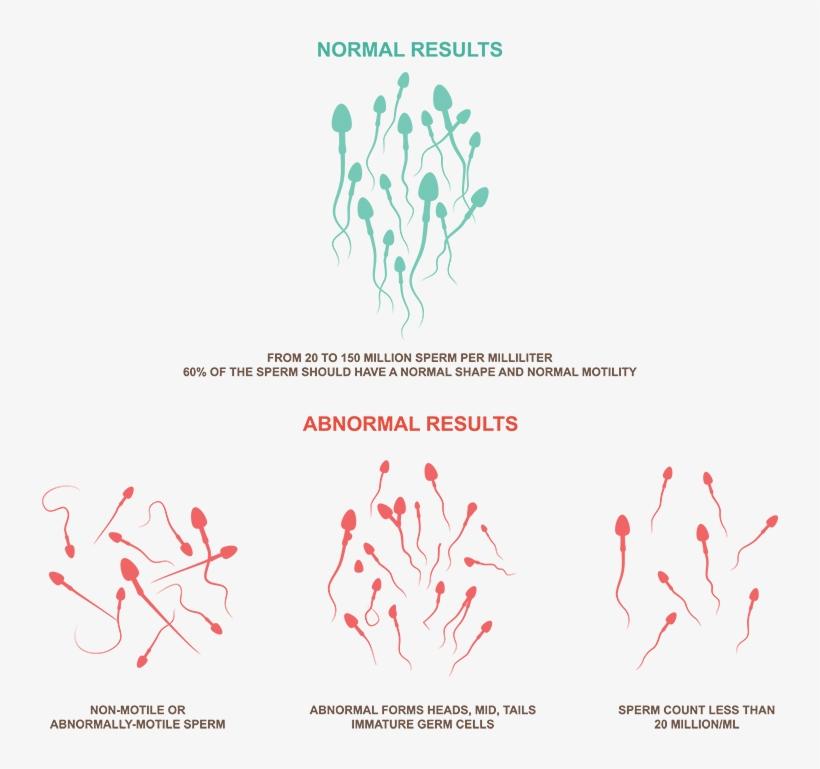
TYPES OF TERATOSPERMIA: mild, moderate, and severe
The teratospermia (or teratozoospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. This is how the Dawasanté experts provide you with a natural treatment to treat all your fertility problems related to the quality and quantity of your sperm.
Click HERE or on the image below to discover this natural treatment
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Teratozoospermia or teratospermia is a seminal alteration that involves a high percentage of abnormally shaped sperm.
It is a cause of male infertility, the severity of which will depend on the greater or lesser number of amorphous sperm cells in the semen.
According to the different criteria used to assess the degree of teratozoospermia, we can distinguish 3 types: mild, moderate, or severe.
1-Classification of teratozoospermia
When a man performs a spermogram to assess the quality of his sperm, in the results report, he will obtain the values of all seminal parameters, including sperm morphology.
A man is considered to have teratozoospermia when the percentage of sperm with normal morphology in his seminogram is less than 4%, according to criteria established by the World Health Organization (WHO) in 2010.
On the other hand, some labs also use Kruger's strict criteria to diagnose teratozoospermia. According to Kruger, a man suffers from teratozoospermia when less than 15% of his sperm has a normal form.
Percentage of normal sperm
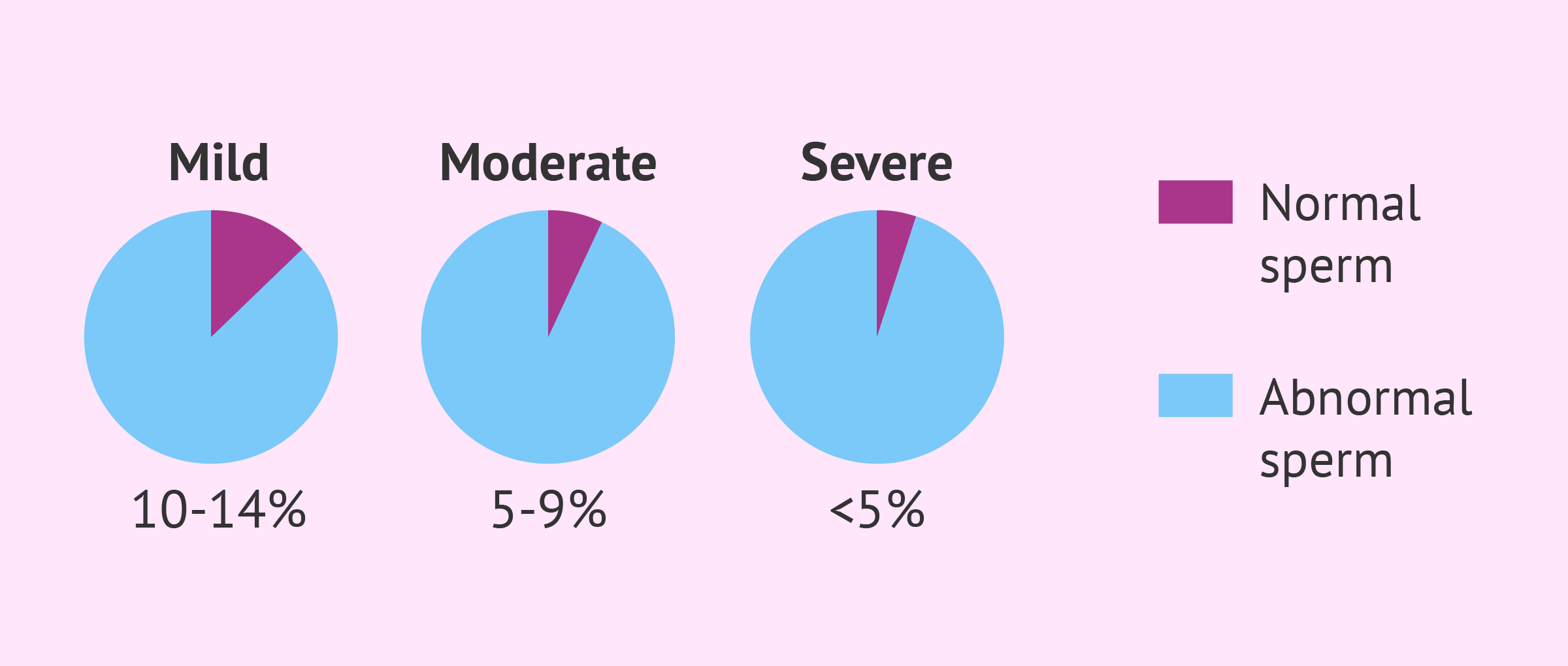
Since the WHO benchmark is so low, there is no point in talking about types of teratozoospermia based on the number of normal sperm. Therefore, for the classification of spermatozoa in this sense, it is better to use Kruger's criterion, which is stricter than the previous one.
1-1 Mild teratozoospermia
A man suffers from mild teratozoospermia when the number of normal sperm in his spermogram ranges from 14% to 10%.
The rest of the sperm will have an abnormality in their head, neck or tail. Despite this, men with mild teratospermia do not have a bad prognosis for having children.
If assisted reproduction techniques are necessary to achieve pregnancy, artificial insemination (AI) and in vitro fertilization ( IVF ) may be performed, depending on the concentration and mobility of the sperm.
The shape of the sperm is important for the fertilization of the egg. However, men with mild teratozoospermia can achieve a natural pregnancy.
In addition, there are various dietary supplements that contain vitamins and antioxidants that help in the maturation of sperm and can improve their morphology.
If you are interested in this topic, you can read the following article: Treatment of teratozoospermia.
1-2 Moderate teratozoospermia
Moderate or severe teratozoospermia is diagnosed when sperm results show that only 9-5% of sperm have a normal shape.
With this diagnosis, it is quite complicated to have children naturally. To achieve a pregnancy with moderate teratozoospermia, an in vitro fertilization technique such as ICSI will most likely be necessary.
The ICSI (Intracytoplasmic Sperm Injection) is based on the selection of spermatozoa under a microscope and their direct injection into each egg and fertilization.
PMA, like any medical treatment, requires that you trust the professionalism of the doctors and clinic you have chosen. Obviously, not all are the same. The Fertility Report selects the most advantageous clinics for you based on our rigorous quality criteria. In addition, the system performs a comparison of prices and conditions offered by different clinics to facilitate your decision making.
1-3 Severe teratozoospermia
When the spermogram morphology test shows a normal sperm value of less than 5%, the man has severe or severe teratozoospermia.
Sperm with good morphology is therefore very few in number and, therefore, the possibility of achieving natural pregnancy is very low.
Spermatozoa with alterations in their morphology have problems progressing gradually, they have more difficulty reaching the egg, penetrating its thick pellucid layer and also fusing its male nucleus with the female one. The consequence of all this is that they can lead to fertilization failures.
Teratozoospermia and fertilization failure

The most suitable assisted reproduction technique for extreme teratozoospermia is ICSI or its improved variant: IMSI.
The IMSI is the same as intracytoplasmic sperm injection, but with the use of a microscope magnification of 6300, so it is possible to get very close to the sperm morphology and make a better selection.
2-Your frequently asked questions
2-1 Can we cure severe teratozoospermia?
If a man has less than 5% of sperm with normal morphology, it is very difficult to regain a normal value with natural or pharmacological treatment. Improvement can be seen over time, especially if the man maintains a healthy lifestyle.
On the other hand, if the teratozoospermia appears associated with another pathology such as, for example, varicocele, it is possible that the spermogram improves its parameters during a surgical intervention to eliminate the varicocele.
2-2 What is isolated teratozoospermia?
Discrete teratozoospermia means that the affected parameter, in this case, the morphology of the sperm, does not have a value much lower than the reference value. Therefore, it would be a mild teratozoospermia.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
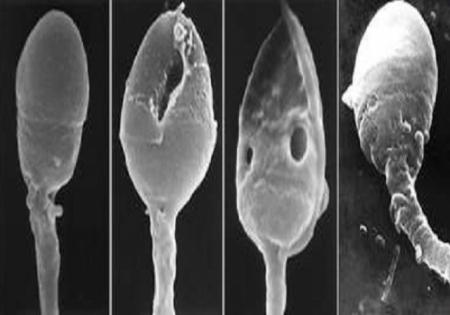
THE CAUSES OF TERATOSPERMIA: Natural treatment
The teratospermia (or teratozoospermia ) is a sperm abnormality characterized by sperm having morphologies defects. Due to these deformities, the fertilizing power of sperm is impaired, and the couple may have difficulty conceiving. Dawasanté experts advise you to opt for a natural treatment without operation, against teratospermia.
Click HERE or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Teratozoospermia refers to the poor morphology of the sperm in a man's ejaculated semen.
These men have lower seminal quality and sometimes suffer from infertility and difficulty achieving pregnancy.
The causes of teratozoospermia are mostly unknown. However, we are going to address the possible alterations caused by these abnormal sperms in semen.
1-Defects in spermatogenesis
Most experts agree that the morphological changes in sperm occur during the last phase of their formation.
The spermatogenesis is the process by which sperm are formed in the testicles, which lasts about 3 months.
More precisely, spermiogenesis is the last phase of spermatogenesis, during which the spermatozoa, which already have their genetic content formed, undergo a process of maturation and acquire their characteristic morphology.
Once the sperm have their oval head and tail formed, they are released into the seminiferous tubules to follow their path.
Therefore, it is not surprising that any abnormality or alteration in spermiogenesis results in abnormalities in the head, neck or tail.
2-Reversible teratospermia
Teratozoospermia can be reversible or irreversible depending on the specific cause.
With reversible teratospermia, men can regain their seminal quality after a few months if they have received the appropriate treatment.
To check this, it is necessary to do another spermogram and compare it with the previous one.
We will now discuss the possible causes of reversible teratozoospermia:
2-1 Way of life
Although it may seem surprising, the lifestyle of men greatly affects the quality of their semen.
During times of stress and anxiety, sperm morphology may deteriorate, as many other parameters such as concentration and mobility.
The abuse of alcohol, tobacco, or other drugs are also factors linked to alterations in sperm.
Prolonged exposure to testicular heat affects spermatogenesis. Therefore, the bad habit of placing the computer on your legs, wearing tight clothes, or driving for a long time can cause teratozoospermia.
Testicular heat causes teratozoospermia

Finally, diet and sport also contribute to male fertility.
Men who are planning to become pregnant with their partner are recommended to maintain a good lifestyle, eat a balanced diet, exercise regularly and not consume substances that are harmful to the body.
2-2 Seminal infections
Semen infections refer to the invasion of microorganisms, bacteria, and viruses, into the male reproductive system.
Its presence is found in urine and semen, causing alterations in the sperm, as well as inflammation and obstruction of the seminal ducts.
The most common bacterial infections in the testes are chlamydia and gonorrhea. These infections can be fought with antibiotics and male fertility can be restored. If you would like more information on this, you can access the following article: Types of infections in seminal fluid.
The episodes of fever caused by flu or another disease may also occasionally affect sperm quality.
2-3 Pharmaceuticals
Sex hormones like testosterone, LH, FSH and inhibin have a very important role in the regulation of spermatogenesis.
Therefore, any drug that changes the appropriate levels of these hormones or affects their secretion by the brain has negative consequences for sperm production.
As we have already said, the alteration of the phase of spermiogenesis prevents the correct maturation of sperm and causes teratozoospermia.
Reversible causes of teratozoospermia
3-Irreversible teratospermia
If a man with teratozoospermia fails to improve his second spermogram after receiving treatment, one may begin to suspect that the teratozoospermia is irreversible.
In these cases, the couple will have to resort to assisted reproduction if they want to become a parent because it will naturally be very difficult to obtain a pregnancy.
In addition, there are other pathologies or situations that cause irreversible or prolonged teratozoospermia. The most relevant cases are examined below:
3-1 Cancer treatment
Chemotherapy and radiation therapy alters both sperm stem cells and sperm production, causing severe teratozoospermia and other more serious changes.
For these reasons, all men with cancer are advised to save a semen sample if they wish to have children in the future after they have overcome the disease.
3-2 Genetic diseases
It is one of the most difficult causes of diagnosis. Normally, when it has not been possible to determine the pathology that causes teratozoospermia, it is attributed to a genetic factor.
Defects in the genes or chromosomes of the sperm are a serious problem because they cannot be corrected.
3-3 Associated pathologies
Teratozoospermia can also result from other diseases that mainly affect the testes, for example:
- Trauma or blows to the testicles, especially in childhood
- Testicular varicocele
- Meningitis
- Diabetic sugar
In addition to all this, the age of males can also affect the morphology of the sperm. In particular, it has been observed that men over 45 have a higher rate of abnormal sperm in their semen.
Irreversible causes of teratozoospermia

4-Your frequently asked questions
4-1 Can live sperm have poor morphology?
By Zaira Salvador (embryologist).
Yes, teratozoospermia can be present in both living and dead sperm.
Dead sperm do not always have a bad morphology. Sometimes they are confused with immobile sperm and it is necessary to make a tincture to find out whether they are viable or not.
4-2 Can leukospermia cause teratospermia and male infertility?
By Zaira Salvador (embryologist).
Leukospermia, also known as leukocytospermia, is the appearance of leukocytes in semen, with a concentration level greater than 1 million per milliliter. The cause of this seminal pathology is an infection of the male reproductive tract which must be treated with antibiotics as it can affect spermatogenesis and cause oligospermia or teratozoospermia.
You can find the information in our article: Leukocytes in semen.
4-3 Are the causes of teratozoospermia and asthenozoospermia the same?
By Zaira Salvador (embryologist).
In most cases, asthenospermia and teratospermia have the same causes. The two seminal parameters are usually changed in the seminogram, known as astenoteratozoospermia. However, this is not always the case.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
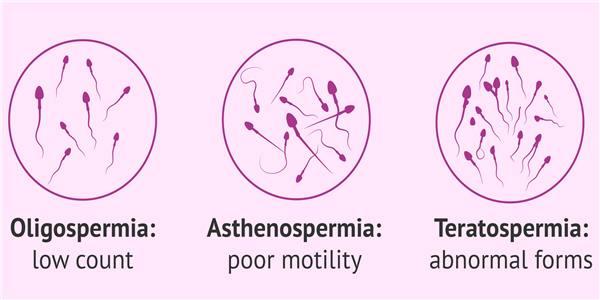
TERATOSPERMIA OR TERATOZOOSPERMIA: definition and treatment
Teratozoospermia or teratospermia is an alteration that occurs in men when more than 95% of their sperm have an abnormal morphology.
Therefore, teratospermia is considered a cause of male infertility due to a sperm factor, and its origin is varied and sometimes unrecognized. This is why the Dawasanté experts provide you with a natural treatment to improve the quality and quantity of your sperm; which will allow you to quickly conceive.
Click HERE or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number
There are several treatments to be able to conceive a child with sperm affected by teratospermia depending on whether the man's sperm has other spermatic disorders, such as, for example, sperm concentration or mobility.
1-Teratozoospermia: what is it?
Poor morphology of the spermatozoa, indeed the latter can present defects in the head, middle part or neck, or the tail.
The WHO estimates that a man with 4% sperm with a normal form (at least) does not have fertility problems. In lower quantity, we are talking about male infertility by teratospermia. This baseline changed in 2010, previously it was 14%, so it is possible that on other sites you will find that teratospermia is considered to be more than 85% abnormal.
According to the strict Kruger criterion, values equal to or greater than 15% of sperm with normal morphology are considered normal. This criterion is always stricter than that of the WHO, but the WHO is the one that is taken as a global reference.
The count of sperm of good or bad morphology is carried out through a medical examination called a spermogram, where the structure of the sperm is analyzed under a microscope.
There are several laboratories which in addition to the Kruger criteria, add those of the WHO.
If the medical report does not specify the details of the analysis to the laboratory, the parameters dictated by the WHO in 2010 are the reference values used.
Diagnosis of teratozoospermia

2-Causes
Teratozoospermia involves male infertility because the sperm that reach the oocyte are unable to fertilize it due to their poor morphology.
The causes that cause the existence of amorphous sperm in human semen are manifold and difficult to diagnose. Here they are:
- Genetic disorders
- Chemotherapy and radiotherapy
- Seminal infections and orchitis
- Varicocele and other testicular disorders
- Febrile period
- Diabetes or meningitis
- Tobacco, alcohol and drug abuse
- Poor lifestyle: poor diet, exposure to toxic substances, clothes that are too tight
Some of these factors can cause reversible teratozoospermia, which goes away with fever, infection, or periods of stress. In the same way, it is possible to recover a good spermatic morphology by improving one's lifestyle, diet, quitting smoking, etc.
3-Types
Sperm morphology defects are classified according to their position on the head, at the neck or at the tail. However, to diagnose teratospermia, all defects are taken into account.
Sperm is considered normal when it has a head with an oval shape and an acrosome inside. The neck or middle piece is slightly larger than the tail, and the tail is elongated and straight.
After analyzing the morphology of the sperm during the spermogram, it is possible to determine the degree of teratozoospermia depending on the seminal quality. For this, the laboratories use the Kruger criteria. Here is their classification:
- Mild teratozoospermia
- 10% to 14% of spermatozoa have normal morphology.
- Moderate teratozoospemia
- the percentage of normal sperm varies between 5% and 9%.
- Severe teratozoospemia
- less than 5% of sperm have normal morphology.
As we have commented before, it is the WHO criteria that are used to diagnose teratospermia, and therefore, this classification is obsolete. However, it is still possible to find it on some spermograms.

3-1 Teratozoospermia index
This seminal parameter is used to know the number of defects that each sperm has. It is possible that sperm has only one malformation, or several distributed over several parts.
In order to calculate the rate of teratospermia (TZI), we use the following formula: TZI = (c + p + q) / x , where each variable means:
- c = head malformations
- p = malformations of the middle part of neck
- q = tail malformations
- x = total number of abnormal sperm
The interpretation of these results is carried out as follows:
- TZI close to 1
- sperm with abnormalities in one area
- TZI close to 2
- spermatozoa with abnormalities in two areas
- TZI nearly 3
- sperm with defects on the head, neck and tail
It is important to note that the same seminal sample can present sperm of three types: one malformation, two, or three. The rate of teratospermia will indicate which type is most present.
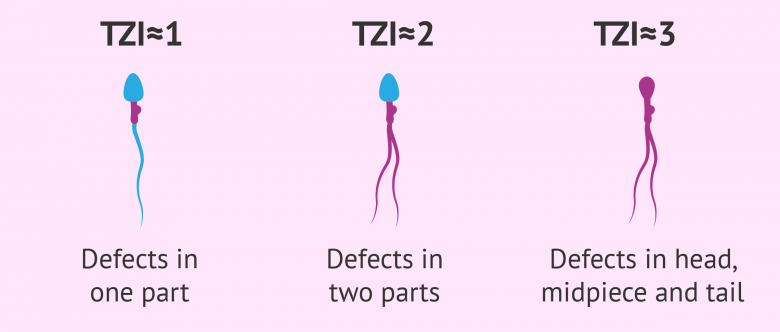
4-Teratospermia and pregnancy
A man with teratospermia could have a natural pregnancy without problems if the rest of the seminal parameters such as concentration or mobility are not affected.
However, in cases where the pregnancy is delayed, it is possible to follow the doctor's recommendations to recover the correct sperm morphology.
On the other hand, if teratospermia has a genetic cause or is congenital, it is more difficult to find an effective treatment to cure it.
4-1 Natural treatments
First of all, men who suffer from teratospermia need to change their lifestyle and put aside bad habits like tobacco or alcohol.
A healthy and balanced diet always helps to recover some of the fertility. In concrete terms, foods rich in antioxidants and essential acids such as L-carnitine help improve sperm quality.
Oily fish is another product rich in omega 3 acids which bring great benefits to human reproductive health.
These nutritional contributions can also be taken by food supplements such as Andean maca or vitamin E supplements, a powerful antioxidant.
4-2 Assisted reproduction (ART)
In the case of fertility treatment to be able to achieve pregnancy and mild teratozoospermia, it is possible to perform artificial insemination (AI), if the concentration and mobility of the sperm allow it.
This is the first option to consider if the woman has no problems with fertility and the only cause of the lack of a pregnancy is teratozoospermia.
Faced with cases of moderate or severe teratospermia, it is necessary to do IVF - ICSI. It is an in vitro fertilization technique that uses the intracytoplasmic injection of sperm for the fertilization of oocytes.
If this topic interests you, you will find information here: IVF.
If you need to undergo IVF treatment to become a mother, we recommend that you use the Fertility Report. In 3 simple steps, which will allow you to know the clinics abroad that meet our rigorous quality criteria. In addition, you will receive a report with useful tips before you make clinic visits.
Finally, there is a new technique which is a variation of the previous one. It is known as IMSI and consists of amplifying the image before the micro-injection to be able to observe the sperm morphology in more detail.
The microscope used by IMSI to select the sperm has an objective that amplifies the image to such an extent that morphological abnormalities are detected.
5-Your frequently asked questions
5-1 What is the cause of teratozoospermia?
Teratozoospermia is an alteration that affects male semen and involves most of the sperm having an abnormal shape.
Due to their poor morphology, sperm cannot fertilize the oocyte and cause sterility.
The causes of teratozoospermia are as follows:
- Genetic alterations
- Chemotherapy and radiotherapy
- Semen infections and orchitis
- Testicular trauma
- Varicocele
- Fever
- Diabetes and meningitis
- Tobacco, alcohol, drugs
Bad eating habits, clothes that are too close to the body ...
Certain causes can be resolved (fever, quitting smoking, healthy habits ...), which implies that in some cases, the pathology is reversible.
5-2 Does teratozoospermia cause miscarriages?
In principle, the poor morphology of the sperm does not cause any miscarriage once the fertilization of the oocyte has taken place and the embryo has implanted. If, on the other hand, the sperm also have genetic disorders, this may be a cause of miscarriage.
5-3 How to improve the amorphous sperm of semen?
If the pathology of teratospermia is not specific, the man should follow some indications to modify his lifestyle, which could negatively influence his reproductive state. Some men who stop smoking or alcohol consumption and change their diet may see an improvement in their sperm quality after 3 months.
5-4 Can leukospermia cause teratospermia and male infertility
Leukospermia, also known as leukocytospermia, is the appearance of leukocytes in semen, with a concentration level greater than 1 million per milliliter. The cause of this seminal pathology is an infection of the male reproductive tract which must be treated with antibiotics as it can affect spermatogenesis and cause oligospermia or teratozoospermia.
You can find the information in our article: Leukocytes in semen.
We deliver all over the world.
For more information, you can contact our experts at +229 51374202 direct line or by WhatsApp at the same number
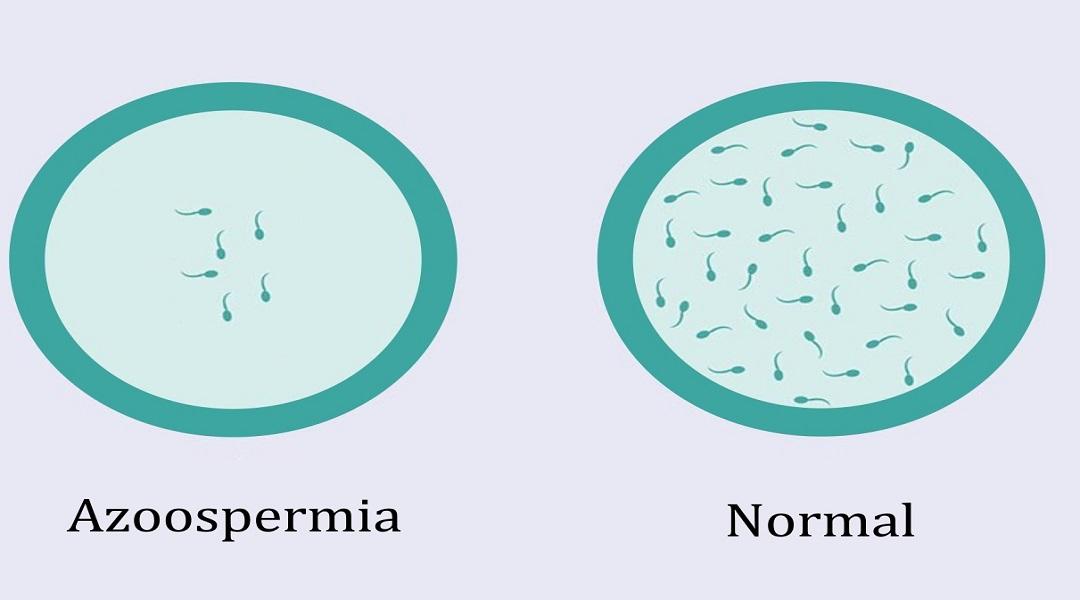
AZOOSPERMIA CAUSES: natural treatment
What is Azoospermia?
The azoospermia is a sperm abnormality characterized by the total absence of sperm in the ejaculate. It obviously leads to infertility in men, because in the absence of sperm there can be no fertilization. However, Dawasanté experts provide you with a natural herbal treatment to improve the quality and quantity of your sperm. Click here or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.

Azoospermia affects less than 1% of men in the general population or 5 to 15% of infertile men (1).
The causes
Depending on the cause, there are two types of azoospermia:
Secretory azoospermia (or NOA, for non-obstructive azoospermia)
Spermatogenesis is impaired or absent and the testes do not produce sperm. The cause of this spermatogenesis defect can be:
- hormonal, with hypogonadism (absence or abnormality in the secretion of sex hormones) which may be congenital (Kallmann-Morsier syndrome for example) or acquired, due in particular to pituitary tumors which alter the functioning of the hypothalamic-pituitary axis or after a treatment (eg chemotherapy);
- genetics: Klinefelter syndrome (presence of an extra X chromosome), which affects 1 in 1,200 men (2), structural abnormality of chromosomes, (microdeletion, i.e. loss of a fragment, of the Y chromosome in particular), translocation (one segment of the chromosome detaches and attaches to another). These chromosomal abnormalities are the cause of 5.8% of male infertility problems (3);
- bilateral cryptorchidism: the two testes have not descended into the bursa, which impairs the process of spermatogenesis;
- infection: prostatitis, orchitis.
Obstructive or excretory azoospermia (OA, obstructive azoospermia)
The testes do indeed produce sperm but they cannot be exteriorized due to a blockage of the ducts (epididymis, vas deferens or ejaculatory ducts). The cause may be of origin:
- congenital: the seminal tract has been altered from embryogenesis, resulting in an absence of the vas deferens. In men with cystic fibrosis, a mutation in the CFTR gene can cause the absence of vas deferens;
- infectious: the passages have been blocked following an infection (epididymitis, prostato-vesiculitis, prostatic utricle).
1-Pre-testicular causes
In this case, the origin of azoospermia is due to alterations at the endocrine level, that is, it is manifested by irregularities in the levels of the hormones responsible for regulating sperm production or spermatogenesis. . These are therefore cases of secretory azoospermia.
Among the main endocrine disorders that can cause azoospermia, we can find:
- Hypogonadotropic hypogonadism: this is a deficiency of the hormones released by the pituitary gland and responsible for stimulating the production of sperm in the testes. The main hormones are FSH (follicular stimulation) and LH (luteinizing). This problem can be due to genetic alterations such as Kallmann syndrome, tumors, trauma, pharmacological treatments, consumption of anabolic agents, etc.
- Hyperprolactinemia: it is the excessive increase in the hormone prolactin release. It blocks the hormone GnRH (a hormone that releases gonadotropins), whose function is to regulate the release of FSH and LH. This can be due to the consumption of antihypertensive drugs, stress, tumors, antidepressants, etc.
- Androgen insensitivity syndrome: this is mainly due to genetic mutations that cause resistance to androgens so that full virilization of the patient does not take place. Depending on the degree of severity, testosterone levels can be low, which prevents or hinders spermatogenesis, among other related consequences.
Patients who suffer from azoospermia due to this syndrome will have slightly decreased testicular volume, they will not produce sperm in the testes, and their FSH levels will generally below, except in cases of androgen resistance. In this case, the LH is elevated but the FSH and testosterone concentrations are usually normal or slightly elevated.
Testicular causes
The absence of sperm is due to problems in the testis which hamper spermatogenesis and therefore lead to errors or even blockage of sperm production.
The most common testicular pathologies are:
- Varicocele: dilation of the spermatic veins.
- Cryptorchidism: no descent of the testis from the inguinal canal to the scrotal pocket.
- Orchitis: Inflammation of the testicle, usually due to infection, as is often the case with mumps.
- Genetic alterations
- Testicular torsion
- Trauma
- Continuous increase in testicular temperature
The type of azoospermia from which these patients suffer is also secretory, but the clinical picture is different from the previous one: they have a lower testicular volume (due to non-production of sperm) but the FSH levels are high.
FSH, which is responsible for stimulating the testes to produce sperm, increases. This is why the testes do not respond to their stimulus, the body sends more FSH for the testes to function.
Post-testicular causes
When the cause of azoospermia is post-testicular, it is obstructive azoospermia. In this case, the testes are able to produce sperm properly, but there is a problem in the seminal ducts (vas deferens, epididymis or urethra) responsible for transporting sperm in an ejaculation.
Among these problems, we can highlight:
- Absence of vas deferens: this is a congenital pathology which, if it affects bilaterally, prevents sperm from coming out during ejaculate. This happens, for example, in some cases of cystic fibrosis.
- Obstruction of the vas deferens, the epididymis, or the urethra: it may be involuntary (trauma, surgery or disease) or voluntary. This is called a vasectomy.
Patients have a normal testicular size and FSH hormone levels are also average. Obstructive azoospermia is the least serious compared to fertility. It allows the man to obtain a pregnancy, either naturally, by a medical intervention which makes it possible to unblock the channels, or by obtaining sperm directly from the testicle and the subsequent application of a medically assisted procreation technique.
Your frequently asked questions
Is varicocele a cause of infertility in men?
By Victoria Moliner (embryologist).
Yes, varicocele can be a cause of male infertility. This pathology can manifest itself in different degrees of affection, so its harmful effect on male fertility (which mainly causes seminal and hormonal changes) can also be from mild to severe.
Is hormonal azoospermia always secretory?
By Andrea Rodrigo (embryologist).
Yes, when the lack of sperm is caused by hormonal problems, it is secretory azoospermia because of the lack of regulation by hormones prevents or complicates spermatogenesis.
Can cycling be the cause of my testicular factor azoospermia?
By Andrea Rodrigo (embryologist).
Continued use of the bicycle does not necessarily cause azoospermia, provided that the correct position is taken on the bicycle and, in some cases, certain testicular protection systems are used.
Routine improper use of the bicycle can increase the temperature of the scrotal region and thus prevent the proper production of sperm, which can reduce the quality of sperm.
As an added note, it is important to note that excessive exercise can affect sperm production in addition to other bodily functions.
Is azoospermia reversible?
By Andrea Rodrigo (embryologist).
It is possible that azoospermia is transient or punctual and, therefore, we can speak of reversible azoospermia. This means that, although it is unusual, a man may have a certain period of azoospermia, for example, due to stress or some other situation, and after this period recover the production of sperm and, with it, the presence of these in the ejaculate.
Read more
Why is there an absence of sperm in the spermogram?
By Zaira Salvador (embryologist).
When a man gets zero sperm as a result of his semen analysis, he may have azoospermia. First of all, this diagnosis should always be confirmed by a second spermogram, in case an error may have occurred while handling the first sample.
If azoospermia is confirmed, there are several causes of this seminal alteration, from blockage of the seminal ducts to problems with sperm production. More human testing should be done to find a more complete diagnosis.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
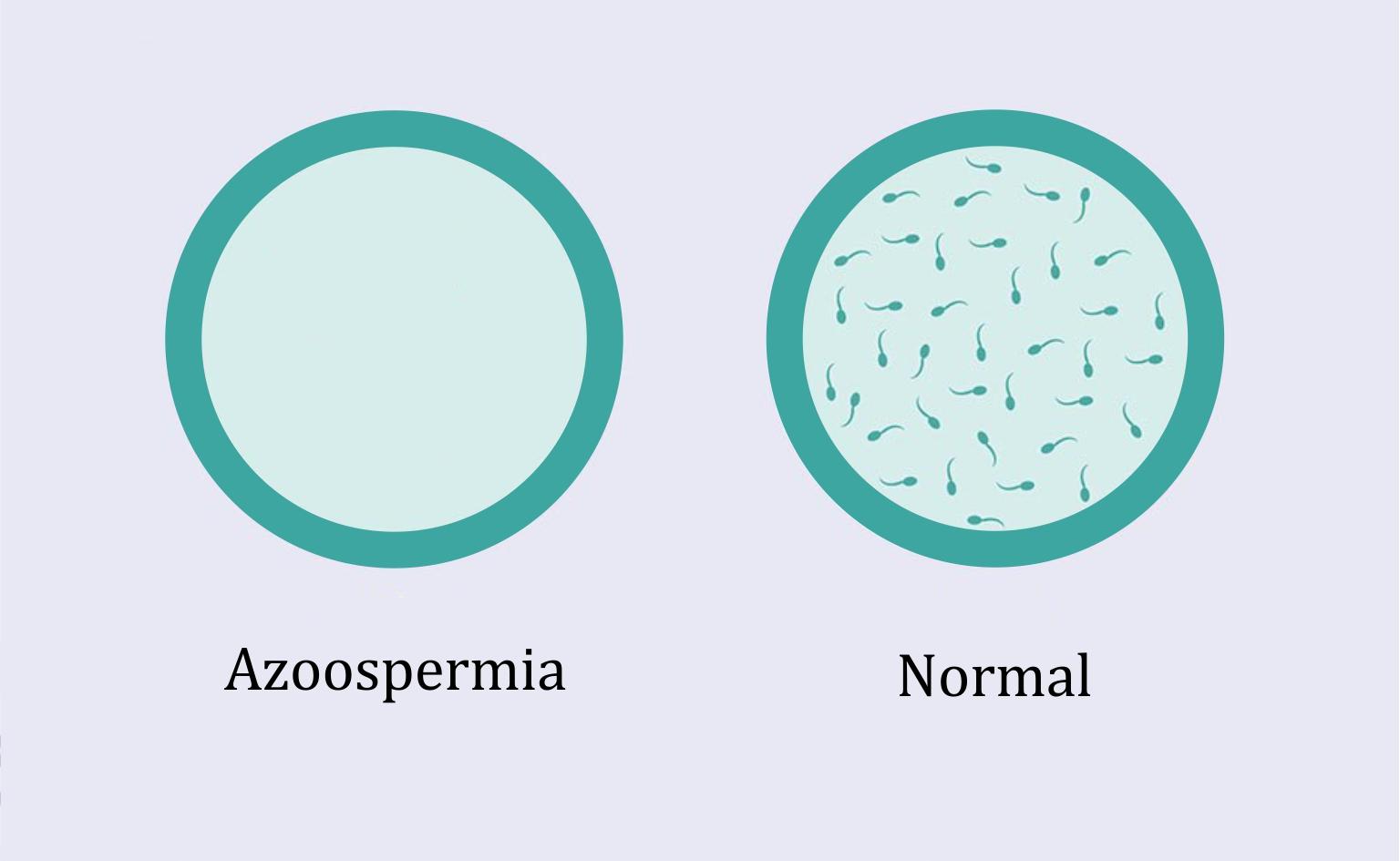
AZOOSPERMIA AND PREGNANCY: Natural treatment
Natural pregnancy in a woman whose partner has secretory or obstructive azoospermia is not possible. However, when the treatments applied do not solve the problem, Dawasanté experts offer you a natural herbal treatment to cure your azoospermia and allow your partner to quickly get pregnant.
Click here or on the image below to discover this natural treatment .
To discover our natural solution to treat azoospermia click here!
Contact our experts, tel / WhatsApp: +22990312738
1: Aspiration of sperm
In men with obstructive azoospermia , no sperm is seen in the ejaculate, but sperm is produced in the testis.
One option is to extract the sperm directly from the testis or epididymis. In this way, it is possible to obtain sperm, but in low quantity and of poor quality in relation to mobility and morphology.
For this reason, in the event of obtaining sperm by aspiration, it will be necessary to resort to the technique of ICSI (intracytoplasmic sperm micro-injection). ICSI is the ideal in vitro fertilization technique because only one sperm is needed for each egg to be fertilized. In addition, in this process, it is the specialist himself who introduces the sperm into the egg.
There are several procedures for extracting sperm, and their names come from the acronyms in English:
1.1: MESA
Corresponds to the term: microsurgical epididymal sperm aspiration , i.e., microsurgical aspiration of epididymal sperm. It is used in patients with obstruction of the genital tract. This involves making a small incision in the epididymis and extracting the sperm from inside the epididymis.
It is a complicated operation and the costs are high. For this reason, although it allows to collect more sperm than with a PESA, it is not the most chosen technique.
1.1.1: PESA
It is the percutaneous aspiration of epididymal sperm ( percutaneous epididymal sperm aspiration ). This is a simpler and less invasive procedure than the previous one and does not require as many skills on the part of the doctor. It is performed under sedation, so that the patient does not feel any pain.
A needle is inserted through the skin of the scrotum to reach the epididymis. The downside is that the needle is inserted blind, and although this is unusual, it is possible that no sperm will be aspirated.
1.1.2: TESA
Its English name is: testicular sperm aspiration , and it is referred to as the aspiration of sperm from the testis. It is also performed percutaneously, just like PESA. The difference is that the aspiration is done from the testes and not from the epididymis.
This type of aspiration is usually performed when the other options (MESA and PESA) are not applicable due to changes such as absence or obstruction of the epididymis.
2: Testicular biopsy
Also known as TESE ( testicular sperm extraction ). It is performed under local anesthesia and consists of the following elements:
- The specialist opens the different testicular layers using a scalpel or a laser until it reaches the testicle, from which he will extract small pieces. About 2-3 cm of testicular layers are opened. They will then be closed with one or two stitches.
- After the biopsy is performed or at the same time as the biopsy, the tissues are analyzed under a microscope for sperm, which will then be used in the ICSI technique in the hope of pregnancy.
- Although it is indicated in patients with obstructive azoospermia , it is also applied in certain situations of secretory azoospermia. In many of these cases, although no sperm is produced in the testes, foci of spermatogenesis can be found, that is, if you search exhaustively, it is possible to find a sperm.
- In any case, the possibility of achieving pregnancy by applying ICSI with the few sperm found after testicular biopsy of patients with secretory azoospermia is low.
3: Sperm donation
The above procedures may be effective for obstructive azoospermia , but they are not usually applied to secretory azoospermia. In patients with this alteration, where no treatment is able to reverse spermatogenesis, it is recommended to resort to sperm donation .
This is artificial insemination or in vitro fertilization with sperm donated by a healthy young man . This donor is subjected to a series of physical and psychological examinations to verify his good state of health and to confirm the safety of the use of his sperm.
The choice of one or the other reproductive technique will depend on certain qualities of the woman such as her age, the patency of the fallopian tubes, etc.
This is an alternative with a high probability of success . However, it has a major drawback: humans give up transmitting their genetic heritage. This means that the children born will not be the biological children of their father, since they will inherit the traits of the donor who gave the sperm.
4: Your frequently asked questions
If my husband has total azoospermia, should we consider donating sperm as the only option so that I can get pregnant?
If as total azoospermia you hear irreparable secretory azoospermia, yes, sperm donation is the best option for you to achieve pregnancy.
In severe cases of secretory azoospermia, it is very difficult to obtain viable sperm with fertilizing ability, so it is necessary to resort to sperm donation.
After 11 years of vasectomy, will I be able to have children if I have a testicular biopsy?
A testicular biopsy is used to obtain sperm directly from the testis, which is the place of production. However, after so long a time of voluntary obstruction, that is, after preventing the produced sperm from coming out, it is possible that the organism itself has reduced production. However, since only one sperm per egg is needed for ICSI treatment, you may be able to achieve pregnancy in your partner from the sperm found during the biopsy.
In any case, you should be aware that it is quite possible that no viable sperm will be found after the biopsy.
Pregnancy was detected by measuring serum HCG on two independent occasions, at least 15 days after the embryo replacement. Clinical pregnancy was determined by observing a gestational sac with a fetal heartbeat on a transvaginal ultrasound at 6–7 weeks gestation. The clinical embryo implantation rate was defined as the number of gestational sacs seen during ultrasound screening at 6-7 weeks gestation divided by the number of embryos transferred.
To discover our natural solution to treat azoospermia click here!
Contact our experts, tel / WhatsApp: +22990312738
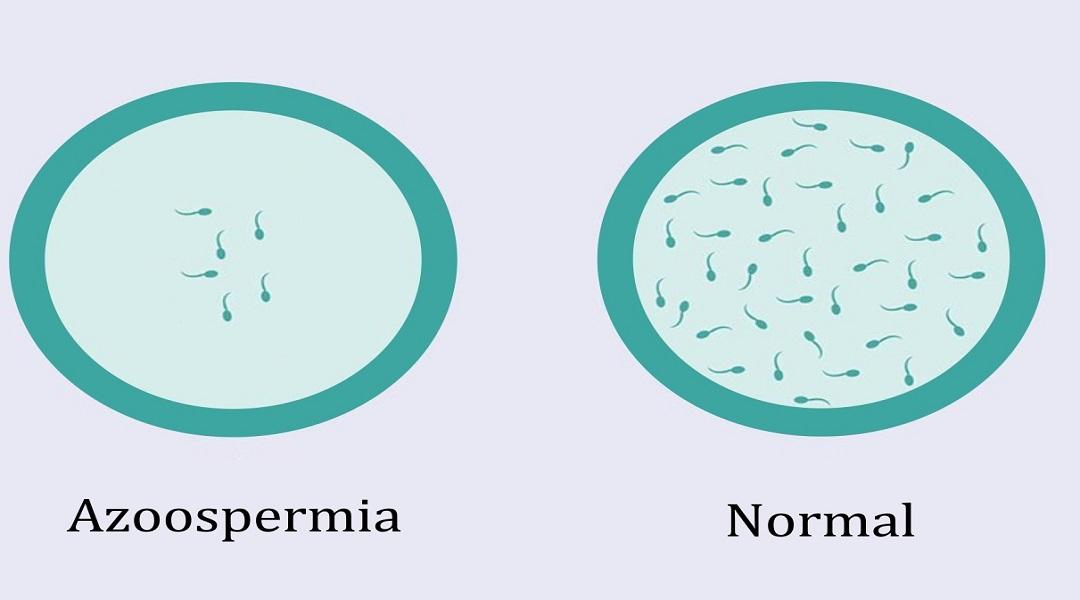
NONOBSTRUCTIVE AZOOSPERMIA: Natural treatment
Azoospermia is a total absence of sperm in the ejaculate. Depending on the cause, we distinguish two forms of azoospermia: obstructive and secretory. The prognosis for achieving pregnancy is different in each case. However, Dawasanté experts provide you with a natural treatment to boost your fertility by improving your sperm, allowing you to conceive quickly. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
1: Azoospermia: definition and diagnosis
In order to study male fertility, the most common test is a spermogram. It consists of collecting a sample of ejaculate and examining it in the laboratory to check, among other things, the concentration and mobility of sperm.
Once the result is obtained, we compare the reference rates of the World Health Organization (WHO) to carry out the diagnosis:
zero sperm in the ejaculate.
less than 100,000 sperm / ml.
less than 15 million / ml.
- Normozoospermia
no seminal parameters are altered.
Therefore, azoospermia can be defined as the absence of sperm in the ejaculate. It is considered to be responsible for between 3 and 10% of cases of male infertility.
Azoospermia is imperceptible to humans, so it is necessary to take a spermogram to diagnose it.
It is also helpful to determine FSH hormone levels. This is produced by the brain and is responsible for spermatogenesis (formation of sperm) in the testes. If the FSH levels are high, it can be inferred that the mother cells of the sperm are reduced or even absent.
You can also analyze the concentration of testosterone and fructose to get a more accurate diagnosis.
Causes
The absence of sperm in the ejaculate is mainly due to two causes:
- Secretory or non-obstructive azoospermia
the testes are not able to produce sperm.
- Azoospermia obstructive
sperm are produced, but cannot be expelled during ejaculate due to obstruction of the vas deferens.
To determine the type of azoospermia, it is necessary to perform a testicular biopsy, which consists of obtaining a small fragment of each testicle and analyzing the presence or absence of sperm. In this way, it will be easy to distinguish an obstructive azoospermia from a secretory.
Through hormonal analysis, the type of azoospermia can be determined, because if there are disturbances in the levels of hormones involved in spermatogenesis , it is secretory azoospermia. However, this method is not as reliable as a biopsy to find out if there are sperm available for ART treatment.
1: Secretory azoospermia
The azoospermia secretory or non-obstructive is the most severe and frequent and assumes 70% of cases of azoospemie. It can be congenital (from birth) or acquired (by disease or toxic treatment). Its most common causes are:
- Abnormalities of testicular descent.
- Exposure to toxic substances: drugs, radiotherapy and chemotherapy.
- Genetics: Gene disorders related to spermatogeneses, such as mutations or deletions.
- Hormonal disorders, such as hypogonadotropic hypogonadism (deficiency of hormones released by the pituitary gland and responsible for stimulating sperm production in the testes).
- Testicular problems: mumps, trauma, inflammation and sever varicocele.
The recovery of sperm from secretory azoospermia is complex, as spermatogenesis is strongly affected. Despite this, pregnancy is possible.
Some patients with this pathology have presented slight foci of spermatogenesis in the testes. To do this, doctors do multiple small testicular biopsies to find sperm.
If sperm are indeed found, the sample is frozen and is then used in an intracytoplasmatic sperm injection (ICSI).
Depending on the cause of the azoospermia, in some cases, it is possible to restore spermatogenesis by hormonal treatments and thus achieve pregnancy.
In cases where it is not possible to collect sperm, it is necessary to use donor sperm to become parents.
2 :Azoospermie obstructive
Obstructive azoospermia is caused by a problem with the ducts that carry sperm from the testes to the urethra, where ejaculate occurs. Here are the most common causes:
- Absence of vas deferens (either from birth or after surgery).
- Inflammation or trauma to the testis, epiydima, vas deferens or prostate.
In patients with this type of disorder, it is easier to obtain sperm. In some cases, this azoospermia can be reversible and thanks to several techniques of micro-surgery, the obstruction can sometimes be resolved or the ducts united so that the sperm can reach the spermatic fluid.
Otherwise, the sperm are obtained directly from the testes by testicular biopsy and are used in assisted reproduction therapy (ICSI). A single biopsy is normally sufficient, as spermatogenesis is produced normally.
Azoospermia and varicocele
The relationship between azoospermia and varicocele is relatively common: 5% of varicocele cases turn into azoospermia. However, for this to happen, the varicocele must be severe.
Varicocele is a dilation of the veins that form the spermatic cord and directly affects spermatogenesis, which is the production of sperm.
In secretory azoosperm patients who have corrected their varicocele by surgery (surgical treatment of varicocele ), approximately 50% of the testicular tissue and 55% of the sperm mobility will be recovered.
Azoospermia following vasectomy
Vasectomy is a method of male sterilization that results in the absence of sperm in the ejaculate. The goal is to intentionally induce obstructive azoospermia by severing the vas deferens, thus preventing the passage of sperm from the testis to the urethra.
As the vas deferens are blocked, the sperm will be stored in the epididymis and, over time, will be reabsorbed by the body itself.
Vasectomy does not affect sperm production, although it is true that over time the body can decrease sperm production or it can be altered slightly.
Your frequently asked questions
No. Azoospermia is the absence of sperm in the ejaculate, but the man has no problems ejaculating. In the case of aspermia, the problem is the lack of ejaculation, it does not refer to the sperm.
What are the symptoms of azoospermia?
By Andrea Rodrigo (embryologist).
Azoospermia does not lead to symptoms that are visible in everyday life such as pain, discomfort, swelling, etc. Therefore, the safe way to diagnose it is not based on the symptoms, but only on the result of the spermogram.
Secretory azoospermia is more serious. It prevents the production of sperm and, therefore, it is not possible to have biological children even by applying assisted reproduction techniques. As we mentioned, the only option for getting pregnant if you are suffering from this type of azoospermia is sperm donation.
Can I use artificial insemination in the case of azoospermia?
No. To achieve pregnancy by artificial insemination , it is necessary to have a good sperm concentration and that patients suffering from azoospermia do not have any sperm in the ejaculate.
Can you be naturally pregnant with secretory azoospermia?
The only way to achieve a natural pregnancy with secretory azoospermia is through hormonal treatment, as it restores spermatogenesis. However, in many cases it is difficult for this to happen, as it all depends on the cause of azoospermia.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
AZOOSPERMIA NATURAL TREATMENT: the experts at Dawasanté
What is azoospermia?
The azoospermia is a lack of sperm in the semen. If, after a year of unprotected sex, no pregnancy has occurred, it means that the man, woman, or both may have a fertility problem. In 40% of infertile couples, the man has a fertility problem. However, Dawasanté experts provide you with a natural herbal treatment to improve the quality of your sperm and allow you to conceive quickly.
Click here or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
How common is azoospermia?
About 1% of all men and 10% to 15% of infertile men have azoospermia.
Treatment
Here we are going to offer you a mixture of African plants, roots and bark that will help you heal your azoospermia. Our blend of plants and roots has already enabled many men around the world to heal from infertility and experience the joy of being a father. What allows us to have excellent results is that we produce all these plants and roots ourselves and that we select only the best plants so that they retain all their therapeutic and medicinal virtues. They are the best roots and plants against azoospermia.
Here are five plants and roots that will help you cure azoospermia:
1. Saw palmetto

Saw palmetto helps boost libido by stopping the breakdown of testosterone in the body. In men, sperm production is guided by testosterone. Too little testosterone results in a low sperm count. Likewise, too little testosterone reduces a woman's egg production. Saw palmetto can therefore increase male and female fertility by altering the balance of free testosterone in the body.
2. Ashwagandha

Ashwagandha is traditionally used to improve sexual health. It supports the endocrine system and promotes its better functioning. It also strengthens the hormonal balance in the body. It stimulates libido and improves sperm count in men. It improves stamina and also improves sexual performance.
3. Saw Palmetto

Saw Palmetto nourishes the entire endocrine system, which can help improve overall reproductive function in humans. Men with high stress, poor immune function, poor lifestyle and eating habits are found to respond well to this plant. This plant is classified as an adaptogen and is antiandrogenic, anti-inflammatory, softening, urinary antiseptic and immuno-amphoteric. Saw Palmetto is also a reproductive amphoteric. What does this mean though? It just means that it normalizes reproductive function.
Saw Palmetto nourishes the body deeply when taken regularly for many months. Constant use of this herb is beneficial in improving the quality and quantity of sperm.
4. Ginseng

Ginseng is often referred to as the king of all herbs and is proven to be the panacea for improving overall well-being. Ginseng is also an aphrodisiac and is used to treat sexual dysfunction and to improve sexual behavior in traditional Chinese medical practices. Data from animal studies have shown a positive correlation between ginseng's performance, libido and copulation, and these effects have been confirmed in case-control studies in humans. In addition, ginseng improves the quality of sperm and their number. We highly recommend it.
5. Maca

Maca has the ability to improve female fertility, which is why it is getting a lot of attention. It balances female hormones to improve fertility. However, this herb also has the ability to boost male fertility. This plant effectively improves the quality of sperm (poor sperm quality is a cause of male infertility). According to a study, men who consume maca regularly have more mobile sperm, more sperm and more semen per ejaculation.
The natural treatment that we offer to cure azoospermia consists mainly of natural herbal teas. The herbal tea is composed of plants and roots whose active ingredients are able to restore the male hormonal balance, by increasing the level of testosterone, the number and the mobility of your sperm. It is the miracle solution to cure azoospermia.
To find out about our natural remedy to cure azoospermia, click here
Cause of azoospermia
Depending on the cause, there are two types of azoospermia:
Secretory azoospermia (or NOA, for non-obstructive azoospermia)
Spermatogenesis is impaired or absent and the testes do not produce sperm. The cause of this spermatogenesis defect can be:
- Hormonal, with hypogonadism (absence or abnormality in the secretion of sex hormones) which may be congenital (Kallmann-Morsier syndrome for example) or acquired, due in particular to pituitary tumors which impair the functioning of the hypothalamic-pituitary axis or after a treatment (eg chemotherapy);
- Genetics: Klinefelter syndrome (presence of an additional X chromosome), which affects 1 in 1,200 men, structural abnormality of the chromosomes (microdeletion, i.e. loss of a fragment, of the Y chromosome in particular), translocation (one segment of the chromosome detaches and attaches to another). These chromosomal abnormalities are the cause of 5.8% of male infertility problems;
- Bilateral cryptorchidism: the two testes have not descended into the bursae, which impairs the process of spermatogenesis;
- An infection: prostatitis, orchitis.
Obstructive or excretory azoospermia (OA, obstructive azoospermia)
The testes do indeed produce spermatozoa but they cannot be exteriorized due to a blockage of the ducts (epididymis, vas deferens or ejaculatory ducts). The cause may be of origin:
- congenital: the seminal tract has been altered from embryogenesis, resulting in an absence of the vas deferens. In men with cystic fibrosis, a mutation in the CFTR gene can cause the absence of vas deferens;
- infectious: the passages have been blocked following an infection (epididymitis, prostato-vesiculitis, prostatic utricle).
Symptoms
The main symptom of azoospermia is infertility.
Diagnostic
The diagnosis of azoospermia is made during an infertility consultation, which in men systematically includes a spermogram. This examination consists of analyzing the content of the ejaculate (semen), evaluating various parameters and comparing the results with the standards established by the WHO.
In the event of azoospermia, no sperm is found after centrifugation of the entire ejaculate. To make the diagnosis, however, it is necessary to carry out one or even two other spermograms, each 3 months apart, because spermatogenesis (cycle of sperm production) lasts about 72 days. In the absence of sperm production over 2 to 3 consecutive cycles, the diagnosis of azoospermia will be made.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
VARICOCEL AND FERTILITY: Natural treatment
VARICOCEL AND FERTILITY
Many men have dilated veins in the scrotum, which is the pouch containing the testicles. Doctors call these veins varicoceles. Many men with varicocel have no symptoms, but some may have fertility problems. Varicoceles are common and affect 10 to 15% of men. Doctors continue to debate the role of varicoceles in infertility. However, Dawasanté experts provide you with a natural herbal treatment to cure varicocele and treat your infertility. Click on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Some research suggests that treating a varicocele may improve fertility outcomes. However, a systematic review indicates that the available evidence is weak and that doctors need to do more research.
In this article, find out if a varicocele affects fertility.
What is a varicocele?
A varicocele occurs when a bulge results from dilated veins inside the scrotum. The swelling usually looks like a magnification above the testis, without discoloration. A pampiniform plexus is a group of veins inside the scrotum. These veins help cool the blood before it goes to the testicular artery, which supplies the testes with blood.
If the testicles are too hot, they cannot produce healthy semen. The health of sperm affects fertility. It is therefore essential that the veins can cool the blood. Most people with a varicocele don't have symptoms, but some may have fertility problems. When a person has a varicocele, they may also experience swelling and tenderness in the scrotum.
Treatment
First, varicocele is not inevitable, the only way out is an operation. The use of natural plants makes it possible to cure varicocele permanently by avoiding surgical operation. The natural remedy for curing varicocele that we offer is completely herbal. It contains two elements namely: an herbal tea and an ointment. Trust us! Because it is the secret to cure varicocele without operation thanks to the plants.
Herbal tea to cure testicular varicose veins is vasculoprotective and venotonic. It is a natural remedy that cures varicocele successfully by strengthening the valves or valves located in the veins of the spermatic cords. So the veins become tonic and tenacious to facilitate the dynamic rise of blood along the veins. This to join the most important veins like the left renal vein and the inferior vena cava. The operation for varicocele is very expensive and is of little benefit. As for our remedy, it has proven its effectiveness with dozens of resolved cases. So, this is one of the best natural herbal remedies to cure varicocele and prevent operation.
Using herbal teas to cure varicocele usually gives excellent results as it helps prevent the operation. So our natural remedy is the best herbal therapy for Varicocele. The solution to curing varicocele is in plants. Being natural products based on plants and herbs, our herbal teas to treat varicocele do not cause any side effects, whether on the body or on health. Our natural remedy is the miracle solution to cure varicocele without operations or side effects. So it is the best natural remedy to cure varicocele.
To discover our natural remedy for varicocele click here
Do Varicoceles Cause Infertility?
Most men with varicoceles do not have fertility problems. Infertility rates in people with varicoceles, however, are higher than in those without. This difference may be due to the fact that varicoceles interfere with the body's ability to make and store semen.
A 2014 study found that varicoceles are sometimes, but not always, a factor in infertility.
Research on whether treating varicoceles can improve fertility is mixed.
A 2012 meta-analysis of previous studies found that treating a varicocele could improve fertility, especially if the cause of a couple's infertility is unknown. However, the researchers stress that the evidence is weak and therefore more research is needed.
The main concern with varicoceles is that the bulging of the veins can damage the sperm and reduce their number. In individuals with an average sperm count, a varicocele is unlikely to cause infertility.
When a couple cannot conceive, it is essential to do a variety of tests, including a sperm count, and not to assume that varicocele is necessarily the only cause.
Causes and risk factors
A varicocele occurs when the veins in the scrotum grow larger. Each vein has a valve that prevents blood from flowing back, but sometimes the valve fails. This causes blood to flow back, damaging the vein and causing swelling. Doctors do not fully understand what causes valve failure and varicocele. They are common and usually do not mean that a person has an underlying health problem.
Studies have proven that smoking can be a risk factor for varicocele because it damages a person's blood vessels. The same study found no link between alcohol or occupation and varicoceles.
Rarely, growth in the stomach can put pressure on the veins, causing a varicocele. This problem is more common in men over 45.
In many people, a varicocele has no apparent cause.
Diagnostic
Most men with varicoceles don't notice anything unusual, although some people report an occasional thrill or throbbing in the scrotum. Many affected people only find out that they have a varicocele after having had problems with infertility. A doctor can often diagnose a varicocele during a physical exam by examining the scrotum and looking for any unusual lumps and blood vessels.
If a doctor suspects a varicocele, they may order an ultrasound. This is a painless imaging test that allows the doctor to see the veins inside the scrotum.
If the person has fertility problems, the doctor may also order a semen analysis to check the quality of the semen.
Medical treatment
Varicoceles that do not cause symptoms do not require treatment. A varicocele may need treatment when:
- · A man has varicocele and low sperm count or other semen problems.
- · Varicocele causes pain or swelling.
- · A couple has unexplained infertility and the male has a varicocele.
When people choose to undergo treatment, they have two different options:
Embolization
Embolization is a surgical procedure that temporarily cuts off the blood supply. A doctor can perform this procedure in their office under local anesthesia, which means that a person will not feel any pain in the area.
During embolization, a doctor inserts a needle into a vein usually through the groin. Sometimes they can insert a needle through the neck. The needle helps the doctor access the veins in the scrotum and block the varicocele. A person may experience pain and tenderness after the procedure, but the recovery time is short and the person can immediately resume normal activities.
Surgery
A doctor can surgically remove a varicocele by blocking blood flow to the damaged vein. This operation is called a varicocelectomy.
A person will undergo general anesthesia before the varicocelectomy in order to be asleep and unable to feel any pain during the procedure. A person may experience pain and tenderness for several days.
Surgery is more effective is embolization with a failure rate of less than 5%. Laparoscopic surgery uses a smaller incision than open surgery and requires less recovery time but also requires a very skilled surgeon. Open surgery uses a wider cut in the scrotum.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
ASTHENOSPERMIA: NATURAL TREATMENT
What is asthenospermia?
The asthenospermia or asthenozoospermia is a sperm abnormality characterized by insufficient mobility of spermatozoa. It can alter a man's fertility and reduce the couple's chances of pregnancy because if they are not sufficiently mobile, the sperm cannot migrate from the vagina to the tube to fertilize the oocyte. However, Dawasanté experts provide you with a natural plant-based treatment to permanently cure asthenospermia.
Click here or on the image below to discover this natural treatment.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.
Asthenospermia can be isolated or associated with other sperm abnormalities. In the case of OATS, or oligo-astheno-teratozoospermia, it is associated with oligospermia (sperm concentration below normal values) and teratozoospermia (too high a proportion of abnormally shaped sperm). The impact on human fertility will be even greater.
Treatment
Here we are going to offer you a mixture of African plants, roots and barks that will help you heal your asthenospermia. Our blend of plants and roots has already enabled many men around the world to recover from their asthenospermia and experience the joy of being a father. What allows us to have excellent results is that we produce all these plants and roots ourselves and that we select only the best plants so that they retain all their therapeutic and medicinal virtues. They are the best roots and plants against asthenospermia.
Here are five plants and roots that will help you cure asthenospermia:
1. ROOTS MALE INFERTILITY
The effects of herbal remedies for treating asthenospermia problems have been proven by studies and hundreds of years of use. Here we are going to offer you a mixture of African plants, roots and bark that will help you heal your infertility. Our blend of plants and roots has already enabled many men around the world to heal from infertility and experience the joy of being a father. What allows us to have excellent results is that we produce all these plants and roots ourselves and that we select only the best plants so that they retain all their therapeutic and medicinal virtues.
2.The fruit of the Tribulus (Tribulus Terrestris)

Tribulus is expected to be very effective in improving sperm count, motility, and morphology when combined with changes in diet and exercise.
The main part of Tribulus that contributes to fertility in men is a constituent called protodioscin. This constituent improves the levels of DHEA in the male body. In men with erectile dysfunction, their DHEA levels have been found to below. Some studies have shown that protodioscin, extracted from Tribulus, increases the natural levels of DHEA necessary for a proper erection. Protodioscin is also the main constituent responsible for the aphrodisiac qualities of Tribulus. The increase in sexual desire while using this herb has been reported by both men and women.
A study by dawabio experts showed a 61% increase in conception in couples with anti-sperm antibodies (the immune system attacking sperm) taking Tribulus. The average duration of conception for a couple after treatment was 5 months. Tribulus is one of the best herbs for improving male fertility. Tribulus supports the production of LH and testosterone in men.
It also helps increase sperm count, motility, and health. It reduces the effects of anti-sperm antibodies.
3. Ginseng
Ginseng is often referred to as the king of all herbs and is proven to be the panacea for improving overall well-being. Ginseng is also an aphrodisiac and is used to treat sexual dysfunction and to improve sexual behavior in traditional Chinese medical practices. Data from animal studies have shown a positive correlation between ginseng's performance, libido and copulation, and these effects have been confirmed in case-control studies in humans. In addition, ginseng improves the quality of sperm and their number. We highly recommend it.
4. Maca

Maca has the ability to improve female fertility, which is why it is getting a lot of attention. It balances female hormones to improve fertility. However, this herb also has the ability to boost male fertility. This plant effectively improves the quality of sperm (the poor quality of sperm is a cause of male infertility). According to a study, men who consume maca regularly have more mobile sperm, more semen and more semen per ejaculation.
5. Ashwagandha

Ashwagandha is traditionally used to improve sexual health. It supports the endocrine system and promotes its better functioning. It also strengthens the hormonal balance in the body. It stimulates libido and improves sperm count in men. It improves stamina and also improves sexual performance.
The natural treatment that we offer to cure asthenospermia consists essentially of natural herbal teas. The herbal tea is composed of plants and roots whose active ingredients can restore the male hormonal balance, by increasing the level of testosterone, the number and the mobility of your sperm. It is the miracle solution to cure asthenospermia.
To discover our natural remedy to cure asthenospermia, click here
Causes of asthenospermia
As with all semen abnormalities, the causes of asthenospermia can be numerous:
- a morphological anomaly of the male gametes,
- an infection,
- presence of anti-sperm antibodies
- medication,
- a varicocele,
- a dietary deficiency,
- a renal failure,
- liver failure
- chemotherapy,
- exposure to radiation,
- excessive alcohol consumption,
- a deficiency in calcium, vitamin D or trace element ...
Symptoms
Asthenospermia does not show any symptoms other than difficulty conceiving.
Diagnostic
A semen analysis, or spermogram, is used to assess the mobility of the sperm. It should be remembered that only mobile gametes can fertilize the egg. Many medical analysis laboratories rely on the classification issued by the World Health Organization to classify spermatozoa:
- Level A (or I): progressive rapid sperm advance quickly and in a straight line,
- Level B (or II): the slow progressive spermatozoa advance slowly or in a curved line,
- Level C (or III): non-progressive spermatozoa move but do not progress,
- Level D (or IV): the sperm are immobile.
To be qualified as normal, the spermogram must show a minimum of 40% of motile sperm and 32% of sperm showing progressive mobility.
We deliver all over the world.
For more information, you can contact our experts on +229 51374202 direct line or by WhatsApp at the same number.








